Search
Search
‘Brain training’ may be an effective treatment for post-traumatic stress disorder, clinical trial finds
LONDON, ON - Neurofeedback, also called ‘brain training,’ consists of exercises where individuals regulate their own brain activity. In a new study from Lawson Health Research Institute and Western University, researchers have found that neurofeedback may be an effective treatment for individuals with post-traumatic stress disorder (PTSD). Published in NeuroImage: Clinical, the clinical trial found that neurofeedback was effective in reducing symptoms of PTSD.
“Brain connectivity involves different parts of the brain communicating with each other and helps to regulate states of consciousness, thought, mood and emotion,” explains Dr. Ruth Lanius, scientist at Lawson, professor at Western’s Schulich School of Medicine & Dentistry and psychiatrist at London Health Sciences Centre. “Individuals with PTSD tend to have disrupted patterns of brain connectivity, but our research suggests they can exercise their brains to restore patterns to a healthy balance.”
Neurofeedback uses a system called a neurofeedback loop in which a person’s brain activity is measured through sensors placed on the scalp and displayed back to them using a computer interface. This allows the individual to complete exercises and visually see the results.
The trial tested neurofeedback with a total of 72 participants, including 36 participants with PTSD and 36 healthy control participants. Of those with PTSD, 18 were randomized to participate in neurofeedback treatment while the other 18 acted as a comparison group.
The study found that the severity of PTSD symptoms decreased in participants randomized to receive neurofeedback treatment. After treatment, 61.1 per cent of participants no longer met the definition for PTSD. This remission rate is comparable to gold standard therapies like trauma-focused psychotherapy.
The research team also used functional magnetic resonance imaging (fMRI) at St. Joseph’s Health Care London to capture brain scans of participants both before and after participation in the trial. They found that individuals with PTSD experienced positive changes in brain connectivity in the salience network and the default mode network following neurofeedback treatment.
“The salience network is involved in detecting threat as part of the ‘fight or flight’ response. It is normally hyperactive in individuals with PTSD. Meanwhile, the default mode network is activated during rest and is involved in autobiographical memory. We often see that this network is less active during rest and functionally disrupted among individuals with PTSD,” says Dr. Andrew Nicholson, affiliated scientist at Lawson. “Neurofeedback helped restore the functional connectivity of both networks to healthier levels.” Dr. Nicholson is an assistant professor at McMaster University and was formerly a post-doctoral fellow at Schulich Medicine & Dentistry.
The study involved weekly sessions of neurofeedback over 20 weeks. Participants were asked to reduce the intensity of the brain’s dominant brain wave – the alpha rhythm. Brain activity was visualized as either a still cartoon or a distorted picture. If the alpha rhythm was successfully reduced, the cartoon started playing or the picture started becoming clearer.
“Participants were not instructed on how to reduce the alpha rhythm. Rather, each individual figured out their own way to do so,” notes Dr. Lanius. “For example, individuals reported letting their mind wander, thinking about positive things or concentrating their attention.”
The team notes the treatment could have a number of clinical implications following further validation.
“Neurofeedback could offer an accessible and effective treatment option for individuals with PTSD,” says Dr. Lanius. “The treatment is easily scalable for implementation in rural areas and even at home.”
-30-
Downloadable Media

Dr. Ruth Lanius, scientist at Lawson, professor at Western’s Schulich School of Medicine & Dentistry and psychiatrist at London Health Sciences Centre
Click for larger image.

Dr. Andrew Nicholson, affiliated scientist at Lawson and assistant professor at McMaster University.
Click for larger image.
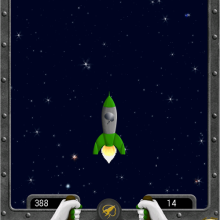
The study tested use of a neurofeedback loop in which a person's brain activity is measured through sensors placed on the scalp and displayed back to them using a computer interface. Brain activity was visualized as either a still cartoon or a distorted picture that would move or become clearer when the alpha rhythm was successfully reduced.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Western delivers an academic experience second to none. Since 1878, The Western Experience has combined academic excellence with life-long opportunities for intellectual, social and cultural growth in order to better serve our communities. Our research excellence expands knowledge and drives discovery with real-world application. Western attracts individuals with a broad worldview, seeking to study, influence and lead in the international community.
The Schulich School of Medicine & Dentistry at Western University is one of Canada’s preeminent medical and dental schools. Established in 1881, it was one of the founding schools of Western University and is known for being the birthplace of family medicine in Canada. For more than 130 years, the School has demonstrated a commitment to academic excellence and a passion for scientific discovery.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
$65.75M grant positions Lawson as Canadian leader in workplace-injury research
Massive research investment by the Workplace Safety and Insurance Board (WSIB) to St. Joseph’s Health Care London will transform occupational illness and injury
LONDON, Ont. – A “game-changer” investment of $65.75 million to Lawson Research Institute (Lawson) of St. Joseph’s Health Care London, (St. Joseph’s) will transform the prevention, diagnosis and treatment of workplace injuries and illness for Ontarians.
The visionary 10-year commitment is the WSIB's largest-ever research injection; the largest non-government research investment in London history; and the biggest single grant stewarded through St. Joseph’s Health Care Foundation.
The landmark investment will bring people, technology and science-backed innovation together to launch the first-in-Canada Occupational Injury Prevention and Treatment Network. Its focus on novel solutions in workplace health will serve Ontario’s workforce, and its innovations will have worldwide impact.
Landmark work, global leadership
“This is a game-changer, something that will transform how we work together to get ahead of work-related injury, pain and mental illness,” says Lisa Porter, PhD, Vice-President Research at St. Joseph’s and Scientific Director at Lawson, the research arm of St. Joseph's. “This investment will propel us to global leadership in finding solutions to some of the most pervasive issues affecting workplaces today.”
Occupational injuries and illnesses – including chronic pain, physical disability and mental health conditions – have a significant impact on many people, families and businesses in Ontario. Every year, they account for almost 250,000 claims registered through the WSIB, with benefit payments of approximately $2.5 billion.
“Too many Ontario families experience the human cost of workplace injury,” says Jeffery Lang, President and CEO of the WSIB. “We want fewer injuries to happen, and if they do, to be able to help people with a safe and faster recovery. This research is going to help us get there – and with their established expertise, St. Joseph’s Health Care London’s Lawson team is a natural partner for this important work.”
Investment and innovation
The network will innovate long-term solutions to prevent mental and physical injuries, accelerate recovery and ensure sustainable health for the workforce.
It will feature state-of-the-art infrastructure and expertise including:
- A first-in-Canada positron emission tomography/magnetic resonance imagery (PET/MRI) scanner enabling research into rapid and accurate diagnosis of mental health conditions including post-traumatic stress and depression
- A cutting-edge Computer-Assisted Rehabilitation Environment (CAREN), a unique, virtual-reality environment that will test and solve workplace injury, rehabilitation and chronic pain in new ways
- Three new endowed research Chairs and teams of scientists solving the most critical research questions plaguing people injured at work, an investment that will ensure long-term consistency and sustainability of the work
- Deploying technology in data science, artificial intelligence (AI) and virtual reality, making the network accessible by centres and workplaces across Canada
- Rapid-access research area to design and test assistive devices such as splints and mobility technology
- Leading research initiatives specific to health-care practitioners in employee wellness, resilience and mental health solutions for occupational trauma
St. Joseph’s President and CEO Roy Butler says, “We know that discovery-driven, patient-focused research improves lives – that is the focus of our hospital-based research at Lawson, and we’re humbled that the WSIB has entrusted us to expand this vital work to minimize the effects of workplace injury, disease and disability. This significant investment will drive innovation opportunities that will translate into novel new treatments and tools that can be used to battle workplace injury and illness.”
He adds, “This investment will enable us to leverage the deep expertise St. Joseph’s already has in mental health, chronic pain and rehabilitation, and creates the opportunity to expand our knowledge to support workplace wellness, including for frontline health-care workers.”
Foundation President and CEO Michelle Campbell says, “Donors to the foundation invest in research because they know that innovation leads to healthier people and healthier communities. It’s a partnership of promise, a confident stride towards better outcomes for patients. The WSIB’s research grant is a whole new level of leadership, and we’re proud to be integral to this transformation in workplace health.”
As the network hub, St. Joseph's will use its vast community and research partnerships throughout London and across Canada, in multiple collaborations across a wide range of health disciplines.
- 30 –
Media package is available, with downloadable B-roll, headshots, photos and fact sheet
For interviews or more information, contact:
Debora (Flaherty) Van Brenk
Communication Consultant, St. Joseph’s Health Care London
C: 226-577-1429 or 519-318-0657
@email
OR
Christine Arnott,
Public Affairs Manager, WSIB
@email
About Lawson Research Institute: Lawson Research Institute, the health innovation arm of St. Joseph's Health Care London, is committed to making and sharing discoveries that improve lives locally and internationally. Every day, Lawson researchers work to transform imagination to innovation to patient impact. Lawson leads health-care research. Find us online at sjhc.london.on.ca/research and on social media @stjosephslondon.
$7.55 million grant to take LHSC-developed technology global
On average it takes five to seven years to diagnose a rare disease. But, for growing numbers of rare diseases, that is all about to change with new artificial intelligence-led technology developed by researchers at London Health Sciences Centre (LHSC) and Lawson Health Research Institute that will be going global.
With funding of $7,551,693 that includes a Genome Canada Genomic Applications Partnership Program (GAPP) grant and support from Illumina Inc., a leading developer of tools for analysis of genetic variation, research led by Dr. Bekim Sadikovic will change what has been years of trial and error in the search for a diagnosis into a simple blood test that could ultimately be available in any lab around the world.
“Despite advances in genome sequencing, it is estimated that nearly 70 per cent of people with a rare genetic disease are not diagnosed,” says Dr. Sadikovic, Research Chair in Clinical Genomics and Epigenomics with the Archie and Irene Verspeeten Clinical Genome Centre at LHSC, and Scientist at Lawson.
“To receive specialized care, you need a specific genetic diagnosis. Without one, you can’t access therapy and, unlike other types of diseases, genetic diseases don't only affect the patient, they affect whole family because they can be inherited,” he says.
Using machine learning, Dr. Sadikovic has developed EpiSign™, the first technology that uses a patient’s epigenome to diagnose genetic disorders. At its most basic level this means that artificial intelligence is used to detect the pattern of chemical signals, called epigenetics, that turn genes within a person’s DNA on or off. The position of this on-off switch for any specific gene could mean someone has blue eyes versus brown eyes, or it could mean they have a rare genetic disease.

Over the last ten years, Dr. Sadikovic has been researching epigenetics and has created a database that contains the epigenetics of hundreds of genetic diseases, and diseases caused by toxic environmental exposures, the largest database of its kind in the world.
This decade of research has culminated in an ongoing national trial of this diagnostic technology called EpiSign-CAN. Funded by Genome Canada, the trial involves testing of thousands of patients across 14 Canadian academic hospitals.
“It is these episignatures that allow us to diagnose patients that otherwise cannot be diagnosed with standard genetic techniques,” Dr. Sadikovic explains. “So, we can now interpret this genetic data that we couldn’t understand before, and provide critical answers for patients and families affected by hundreds of rare diseases.”

This $7.44 million grant funding from the Government of Canada through Genome Canada will enable the next phase of the project in which EpiSign™ technology will be implemented in labs at academic institutions in 15 countries around the world.
“This research is a great example of LHSC’s commitment to supporting the world-leading advances in diagnosis of patients with rare diseases,” says Brad Campbell, Corporate Hospital Administrative Executive at LHSC.
Along with Dr. Sadikovic’s laboratory at LHSC, two industry partners will be involved in this project. Illumina Inc. will be developing custom microchip hardware to facilitate streamlined sample collection, and EpiSign Inc., a Canadian startup biotechnology company which is a partnered venture between LHSC and Dr. Sadikovic, will develop end-user software for automated data analysis in labs around the world.
“The support provided by Genome Canada and Illumina will enable adoption of EpiSign technology and place it at the forefront of patient care globally,” Campbell says.
Dr. Sadikovic’s work has also been supported with funding through LHSC’s Academic Realignment Initiative Awards and generous donor support through London Health Sciences Foundation, including through the Archie and Irene Verspeeten Clinical Genome Centre.
Media contact:
Roxanne Beaubien
Senior Media Relations Consultant
London Health Sciences Centre
Cell: 226-577-1511
@email
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
London Health Sciences Centre has been at the forefront of medicine in Canada for 145 years and offers the broadest range of specialized clinical services in Ontario. Building on the traditions of its founding hospitals to provide compassionate care in an academic teaching setting, London Health Sciences Centre is home to Children’s Hospital, University Hospital, Victoria Hospital, the Kidney Care Centre, two family medical centres, and two research institutes – Children’s Health Research Institute and Lawson Health Research Institute. As a leader in medical discovery and health research, London Health Sciences Centre has a history of over 70 international and national firsts and attracts top clinicians and researchers from around the world. As a regional referral centre, London Health Sciences Centre cares for the most medically complex patients including critically injured adults and children in southwestern Ontario and beyond. The hospital’s nearly 15,000 staff, physicians, students and volunteers provide care for more than one million patient visits a year. For more information, visit www.lhsc.on.ca.
A “safety net of relationships” to bridge the gap between hospital and community at discharge
LONDON, ON – A beneficial and cost-effective approach to mental health care that supports people as they go from hospital and back into the community is outlined in a new resource and has been recognized internationally by the World Health Organization (WHO).
“The immediate period after discharge from hospital, usually the first month, can be one of the most vulnerable times in the life of someone experiencing a mental illness. It can be when they are most at risk of committing suicide,” explains Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson Health Research Institute. “However, what we’ve seen is that there’s often a gap between when someone says ‘goodbye’ to the hospital inpatient unit and ‘hello’ to the community care provider.”
Today during a virtual book launch, a research team from Lawson and several community organizations discussed details of a new publication from Routledge, From Therapeutic Relationships to Transitional Care: A Theoretical and Practical Roadmap, edited by Dr. Forchuk. The book combines theory, research and best practices into a “roadmap” for organizations and others worldwide coordinating services or studying mental health care systems. It includes a practical toolkit for implementing the Transitional Discharge Model (TDM), developed and tested in communities across Ontario.
TDM was born from a participatory action project with consumers of mental health services. They identified two factors that were most important to them when they were going from hospital to the community: consistency in therapeutic relationships and a supportive peer friendship. They described it as a “safety net of relationships” that would bridge the gap between hospital and community services.
“As a person-centred, evidence-based model, transitional discharge supports a smooth adjustment from hospital to community,” says Dr. Forchuk. “The inpatient staff continue to care for discharged clients until therapeutic relationships are established with community care providers. At the same time, we have a friendship model of peer support. These are trained people with lived experience of mental illness who have made the same journey.”
Lance Dingman was a TDM client during the early phases of the project. “It makes a big difference when you’re able to get back to living in the community and in your own dwelling. You get to make more of your own decisions and learn about what you want to do. You grow with your experience and the guidance of others who are there to support you.”
Later becoming a peer support coach, Dingman feels implementing TDM for mental health care is important because people can learn from each other and get healthier in the process. “As a peer support worker, I sit with people and they tell me their story. It takes me back and I know what they are going through – I was where they are. I can share my own story and tell them what I did to get better.”
Dr. Forchuk’s team analyzed the cost of TDM after being tested in nine hospitals across Ontario, including London Health Sciences Centre and St. Joseph’s Health Care London. On average, the length of stay in hospital was reduced by almost 10 (9.8) days per admission and each site saved approximately $3.3 million per year. “People can return home sooner because a higher level of care and support is in place when they leave hospital. If all hospitals in Ontario with mental health services were able to implement our transitional discharge model, we would save $60 million per year in hospital stay costs alone while providing enhanced mental health care.”
The TDM approach is now considered a “good practice” by WHO and was recently the only Canadian example included in its Guidance on community mental health services: Promoting person-centered and rights-based approaches. This set of publications provides information and support to all stakeholders who wish to develop or transform their mental health system and services to align with international human rights standards including the UN Convention on the Rights of Persons with Disabilities.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Benchmarking the evaluation process for living kidney donation to improve outcomes
LONDON, ONTARIO - Living kidney donation rates have remained stagnant over the last decade, and many potential living donors find the evaluation process to be lengthy and difficult to navigate. Researchers from Lawson Health Research Institute and Western University have published results identifying indicators to monitor and improve the performance of transplant centres in how efficiently they evaluate individuals interested in becoming living kidney donors. The findings appear in the current issue of CJASN.
In 2019, there were 219 living donor kidney transplants in Ontario. There are several advantages to kidney transplantation from a living donor compared to deceased. However, many living donor candidates drop out of the evaluation process for a variety of reasons.
“From speaking with living donors, we know that some people find the evaluation process frustrating and cumbersome,” says Dr. Amit Garg, Professor at Western’s Schulich School of Medicine & Dentistry and Scientist at Lawson. “To ensure living donation is safe for both the donor and the recipient, a thorough evaluation is needed looking at medical, physical and psychosocial considerations.” Dr. Garg is also Director of the Living Kidney Donor Program at London Health Sciences Centre (LHSC).
Marian Reich started the journey of living kidney donation 11 years ago, giving the gift of life to her sister-in-law, Susan. “The evaluation process took one full year to complete, and in that time Susan lost the option of a pre-emptive transplant and started dialysis. I wasn’t fully aware that I had to be the driver of the process, and how to do that.”
Reich believes living donor evaluation should be consistent across the country, with a clearer process outlined for potential living donors and recipients. “Research studies like this one bring forth best practice and evidence-based information that includes the perspective of those with lived experiences.”
The research team, which included Patient Partners such as Reich who co-authored the paper, surveyed 77 participants who were kidney transplant recipients and recipient candidates, living kidney donors and donor candidates, or health care providers and administrators.
Out-of-pocket cost incurred by donors is one of the most significant barriers to donation. Another challenge is the lack of reliable information about the expectations and requirements of the donation process. For example, the time commitment, nature of the testing and reasons for the tests performed.
The evaluation process takes on average 10 months to complete, requiring multiple visits to the transplant centre. The intended recipient’s health may deteriorate during this wait to the point they may no longer receive a transplant. “By improving the efficiency of the process, more living donor candidates could complete the evaluation and more transplants performed,” adds Dr. Garg.
The study found a diverse set of quality indicators to measure the evaluation process, focusing on efficiency and safety to improve patient outcomes. They also identified a single measure tracking the costs of living donor evaluation from a health system perspective to assist with planning and budgeting.
“This is an important first step towards system monitoring, benchmarking and accountability in living kidney donor evaluation,” explains Dr. Steven Habbous, co-lead investigator and PhD graduate with Lawson and Western’s Schulich School of Medicine & Dentistry. “In other areas of the health care system, there are reported metrics that hospitals and funders use to compare performance between similar hospitals and track changes over time. We need to measure what we value, and value what we measure.”
The team will present the data to the Canadian National Living Kidney Donation Advisory Committee to help develop national guidelines. Potential improvement strategies are to evaluate multiple living donor candidates concurrently for the same recipient or offer some aspects of the evaluation virtually.
The study was funded by the Can-SOLVE CKD Network, a Canada-wide initiative to enhance kidney disease research and care in partnership with patients. The Ontario-based team led by Dr. Garg is one of 18 Can-SOLVE CKD research groups across the country investigating issues such as earlier diagnosis, better treatments, and innovative care – all based on priorities identified by patients.
-30-
Downloadable Media
Click image for larger version

Dr. Amit Garg, study co-lead investigator, Professor at Western’s Schulich School of Medicine & Dentistry, and Scientist at Lawson. Dr. Garg is also Director of the Living Kidney Donor Program at LHSC.

Dr. Steven Habbous, study co-lead investigator and PhD graduate with Lawson and Western’s Schulich School of Medicine & Dentistry

Marian Reich, study co-author, Patient Partner and living kidney donor
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
The Schulich School of Medicine & Dentistry at Western University is one of Canada’s preeminent medical and dental schools. Established in 1881, it was one of the founding schools of Western University and is known for being the birthplace of family medicine in Canada. For more than 130 years, the School has demonstrated a commitment to academic excellence and a passion for scientific discovery.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Canadian team first in world to treat COVID-19 with specialized dialysis
LONDON, ON - As part of a randomized controlled trial, a team from Lawson Health Research Institute is the first in the world to treat a patient with COVID-19 using a modified dialysis device. The device gently removes a patient’s blood, modifies white blood cells and returns them to fight hyperinflammation. It is being tested with critically ill patients at London Health Sciences Centre (LHSC).
Evidence suggests that COVID-19 causes a heightened immune response, termed a ‘cytokine storm,’ in the most severely ill patients. Treatment options to address this hyperinflammatory state are currently limited and there are concerns about global drug shortages.
“Working in the intensive care unit (ICU), I was aware that more treatment options were needed in the fight against COVID-19,” says Dr. Chris McIntyre, lead researcher, Lawson Scientist and LHSC Nephrologist. “This led to the idea of treating a patient’s blood outside of the body. We could reprogram white blood cells associated with inflammation to alter the immune response.”
The research uses a modified version of a standard dialyzer called an extracorporeal leukocyte modifying device. It gently removes blood in a much slower circuit than standard dialysis. Through a process using specific levels of biochemical components, it targets and transforms white blood cells associated with inflammation before releasing them back into circulation. The hope is that these ‘reprogrammed’ cells will now fight hyperinflammation - rather than promoting it - in affected organs like the lungs.
The clinical trial will include up to 40 critically ill patients with COVID-19 at LHSC’s Victoria Hospital and University Hospital. Research participants will be randomized to receive either standard supportive care or standard supportive care in combination with this novel treatment. The research team will compare patient outcomes to determine if the treatment is effective.
“The ultimate goal is to improve patient survival and lessen their dependency on oxygen and ventilation,” explains Dr. McIntyre. “If effective, it’s possible that this treatment could be combined with other therapies. For example, this could be used to modulate inflammatory consequences while an antiviral drug is used to reduce the viral load.”
Led by Lawson’s Kidney Clinical Research Unit, this new trial was accelerated from initial conception to treatment of the first patient in only 40 days. It represents an important research collaboration with a multidisciplinary team. The trial is leveraging insights gained from another local study led by Dr. Douglas Fraser which is analyzing blood samples from COVID-19 patients at LHSC to better understand the cytokine storm.
“We’re identifying which cytokines or biomarkers are important to the hyperinflammatory response seen in COVID-19 patients,” says Dr. Fraser, Scientist at Lawson and Paediatric Critical Care Physician at LHSC. “With the knowledge we’re gaining, we can study a patient’s blood to determine whether this extracorporeal treatment is making a difference.”
If successful, the treatment also has potential to be used with other conditions like sepsis.
-30-
DOWNLOADABLE MEDIA


This modified dialysis device gently removes a patient’s blood, 'reprograms' white blood cells and returns them to fight hyperinflammation.


Dr. Chris McIntyre, Scientist at Lawson Health Research Institute, is the first in the world to treat a patient with COVID-19 using a modified dialysis device.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Clinical use of EpiSign proven for diagnosing rare heritable disorders
LONDON, ON – A study led by researchers at Lawson Health Research Institute (Lawson) provides clinical validation of EpiSign, a molecular genomics test that diagnoses rare, heritable neurodevelopmental conditions.
Invented at Lawson by Dr. Bekim Sadikovic, the diagnostic test uses machine learning to analyze the EpiSign Knowledge Database. This database compiles information on rare genetic diseases using laboratory analyses of the epigenome from patients with suspected genetic abnormalities. The epigenome is a process that can change the expression of a gene without changing the gene sequence.
“Using 211 blood samples, we measured test performance and diagnostic yield in 207 subjects from two different cohorts,” explains Dr. Sadikovic, lead researcher at Lawson and Scientific and Clinical Director of the Verspeeten Clinical Genome Centre at London Health Sciences Centre (LHSC). The targeted cohort were subjects with previous genetic findings that were ambiguous or inconclusive. The screening cohort were those with clinical findings consistent with hereditary neurodevelopment syndromes but with no previous genetic findings.
“Of the 207 subjects tested, 57 were positive for a diagnostic episignature including 48 in the targeted cohort, and 8 in the screening cohort. Only four remained inconclusive after EpiSign analysis,” says Dr. Sadikovic. “This gives us strong evidence for the clinical use of EpiSign, as well as the ability to provide conclusive findings in the majority of subjects tested.”
While currently there are limited treatment options associated with many of these conditions,
providing a diagnosis can help physicians better predict the course of the disease, and allows for better planning and support for the patient. EpiSign is the only test in the world that has been clinically validated for testing these kinds of genetic disorders.
“Patients with rare diseases often wait years and undergo numerous exams and tests before receiving a correct diagnosis, if one is found at all,” says Matthew Tedder, PhD, staff scientist at the Greenwood Genetic Center, one of the EpiSign clinical testing laboratories. “EpiSign provides an additional high-yield diagnostic tool for clinicians to include in their evaluation of patients with undiagnosed diseases, providing better medical management for patients and hope for their families.”
The study, “Clinical epigenomics: genome-wide DNA methylation analysis for the diagnosis of Mendelian disorders", is published in February’s Genetics in Medicine and was completed in collaboration with the Greenwood Genetic Center and the University of Amsterdam.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
COVID-19 shown to leave unique lung fingerprint
LONDON, ON – Researchers at Lawson Health Research Institute (Lawson) developed and tested an artificial neural network for diagnosing COVID-19. The AI system was trained to learn and recognize patterns in ultrasound lung scans of patients with confirmed COVID-19 infection at London Health Sciences Centre (LHSC) and compared them to ultrasound scans of patients with other types of lung diseases and infections.
“The AI tool that we developed can detect patterns that humans cannot. Lung ultrasound scans of patients with COVID-19, as well as other lung diseases, produce a highly abnormal imaging pattern, but it is almost impossible for a physician to tell apart different types of infections by looking at these images. There are details, however, that distinguish COVID-19 at the pixel level that cannot be perceived by the human eye,” explains Dr. Robert Arntfield, Lawson Researcher and Medical Director of the Critical Care Trauma Centre at LHSC.
“The neural network was able to identify the unique characteristics among different scans, and exceed human-level diagnostic specificity. Our study of over 100,000 ultrasound images showed that while trained physicians could – as expected - not distinguish between different causes of lung disease, the AI had nearly perfect accuracy in making the diagnosis. It’s almost like the AI sees a QR code that we cannot see, unique to the disease.”
LHSC is a global leader in the use of point-of-care ultrasound. It has become an important tool for the diagnosis and care of critically ill patients experiencing acute respiratory failure. The convenience, portability and low cost of using these machines makes them ideally suited for pandemic conditions.
This study is part of a collaborative effort by a small group of local clinicians driven to innovate and create technology that solves complicated problems with AI. “There are a lot of brilliant minds in our city, and I’m very proud that we were able to rapidly pull together a local team to design, develop and test a complex idea,” says Dr. Arntfield. “We are already expanding on these findings with more research.” Lawson has recently approved Dr. Arntfield’s “Project Deep Breathe” which aims to go beyond COVID-19 and explore multiple conditions where lung ultrasound and AI can be paired together.
The study, “Development of a convolutional neural network to differentiate among the etiology of similar appearing pathological B lines on lung ultrasound: a deep learning study”, is published in BMJ Open.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Detecting prostate cancer with a drop of blood and Gulf War technology
London, Ontario - Gulf War technology is making it possible for researchers to detect prostate cancer with a single drop of blood.
Hon Leong, PhD, assistant professor at Western University’s Schulich School of Medicine and Dentistry and scientist at Lawson Health Research Institute, and his team have repurposed a machine once used to detect airborne pathogens in the second Gulf War. The machine is now used for fluid biopsies – a non-invasive way to detect prostate microparticles in the blood in a matter of minutes. Microparticles are essentially garbage released by prostate cells that circulate throughout the bloodstream.
Most men who are more than 40 years old, regardless of their health, have detectable levels of prostate microparticles in their bloodstream. Leong’s research is the first clinical cancer research project to correlate the number of microparticles in the blood to the risk of having prostate cancer – the more microparticles, the higher the risk.
Used in the Gulf War, and more commonly to test water purity, the machine uses flow cytometry to detect microparticles. Flow cytometry measures the specific characteristics of a fluid, such as blood, as it passes through a laser.
Leong’s research provides a more accurate and less invasive testing method for patients suspected of having prostate cancer, and helps to identify patients who are at a higher risk of dying from prostate cancer.
Current methods of detecting prostate cancer, such as the prostate-specific antigen (PSA) test and biopsies, have limitations. PSA tests are based on measuring a specific protein released by the prostate gland, but do not provide a definitive diagnosis. A physical exam and biopsy are needed if PSA levels are elevated. However, even the painful biopsy procedure has a 15 per cent error rate. During biopsies, a painful and invasive procedure, 12 needles are inserted into the rectum, with the hope of extracting material from an area with a tumour.
“Our findings point to a new direction in how we can better identify patients who actually have prostate cancer,” said Leong. “With this test, we can improve the clinical outcomes for patients, reducing costs for unnecessary procedures and reducing errors in diagnosis.”
- 30 -
See all Lawson Media Releases
Western delivers an academic experience second to none. Since 1878, The Western Experience has combined academic excellence with life-long opportunities for intellectual, social and cultural growth in order to better serve our communities. Our research excellence expands knowledge and drives discovery with real-world application. Western attracts individuals with a broad worldview, seeking to study, influence and lead in the international community.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Diagnosing COVID-19 using artificial intelligence
LONDON, ON – A team of researchers at Lawson Health Research Institute is investigating whether an artificial neural network could be used to diagnose COVID-19. The AI system is being trained to learn and recognize patterns in ultrasound lung scans of patients with confirmed COVID-19 at London Health Sciences Centre (LHSC) by comparing them to ultrasound scans of patients with other types of lung infections.
“Machines are able to find patterns that humans cannot see or even imagine. Lung ultrasound scans of patients with COVID-19 pneumonia produce a highly abnormal imaging pattern. This pattern isn’t unique to COVID-19, and can be seen in other causes of pneumonia. It is plausible, however, that there are details that distinguish COVID-19 at the pixel level that cannot be perceived by the human eye,” explains Dr. Robert Arntfield, Lawson Researcher and Medical Director of the Critical Care Trauma Centre at LHSC. “If we can train a neural network to learn and identify these unique characteristics among different scans, we can apply this AI to enhance the diagnostic power of portable ultrasound.”
Point-of-care ultrasound has become increasingly important for the care of critically ill patients and LHSC is a global leader in the use of this technology at the bedside. Lung ultrasound has proven to be effective in diagnosing different types of lung infections and illnesses, such as pneumonia, with a high degree of accuracy. The convenience, portability and low cost of using these machines has helped them become a standard bedside tool in emergency departments and intensive care units worldwide.
This research project is part of a grassroots effort by a small group of local clinicians to innovate and create technology to solve sophisticated problems with AI. With many of Dr. Arntfield’s team having a background in computer programming, they were able to code the neural network being tested. Minimal funding was required, with the project being driven largely by the urgency of COVID-19 coinciding with the recent creation of this clinical AI working group.
“Our research team has used AI to help improve diagnostics related to other parts of the body. This project is a great example of the unique ability we have here in London to be agile: that is, to identify a gap and move quickly towards finding a solution,” says Dr. Arntfield. “I am thrilled that we were able to move through the approval process quickly, and get our ideas working in such a short amount of time.”
-30-
Downloadable Media
Dr. Robert Arntfield
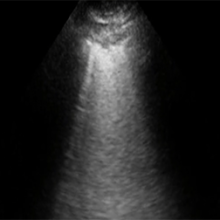
COVID-19 pneumonia ultrasound
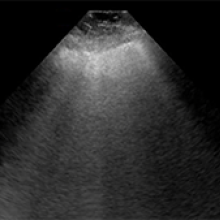
NON COVID-19 pneumonia ultrasound
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Differences in walking patterns could predict type of cognitive decline in older adults
LONDON, ON - Canadian researchers are the first to study how different patterns in the way older adults walk could more accurately diagnose different types of dementia and identify Alzheimer’s disease.
A new study by a Canadian research team, led by London researchers from Lawson Health Research Institute and Western University, evaluated the walking patterns and brain function of 500 participants currently enrolled in clinical trials. Their findings are published today in Alzheimer's & Dementia: The Journal of the Alzheimer's Association.
“We have longstanding evidence showing that cognitive problems, such as poor memory and executive dysfunction, can be predictors of dementia. Now, we’re seeing that motor performance, specifically the way you walk, can help diagnose different types of neurodegenerative conditions,” says Dr. Manuel Montero-Odasso, Scientist at Lawson and Professor at Western’s Schulich School of Medicine & Dentistry.
Dr. Montero-Odasso is world renowned for his research on the relationship between mobility and cognitive decline in aging. Leading the Mobility, Exercise and Cognition (MEC) team in London, he is pioneering novel diagnostic approaches and treatments to prevent and combat early dementia.
This study compared gait impairments across the cognitive spectrum, including people with Subjective Cognitive Impairment, Parkinson’s Disease, Mild Cognitive Impairment, Alzheimer’s disease, Lewy body dementia and Frontotemporal dementia, as well as cognitively healthy controls.
Four independent gait patterns were identified: rhythm, pace, variability and postural control. Only high gait variability was associated with lower cognitive performance and it identified Alzheimer’s disease with 70 per cent accuracy. Gait variability means the stride-to-stride fluctuations in distance and timing that happen when we walk.
“This is the first strong evidence showing that gait variability is an important marker for processes happening in areas of the brain that are linked to both cognitive impairment and motor control,” notes Dr. Frederico Perruccini-Faria, Research Assistant at Lawson and Postdoctoral Associate at Western’s Schulich School of Medicine & Dentistry, who is first author on the paper. “We’ve shown that high gait variability as a marker of this cognitive-cortical dysfunction can reliably identify Alzheimer’s disease compared to other neurodegenerative disorders.”
When cognitive-cortical dysfunction is happening, the person’s ability to perform multiple tasks at the same time is impacted, such as talking while walking or chopping vegetables while chatting with family.
Having gait variability as a motor marker for cognitive decline and different types of conditions could allow for gait assessment to be used as a clinical test, for example having patients use wearable technology. “We see gait variability being similar to an arrhythmia. Health care providers could measure it with patients in the clinic, similar to how we assess heart rhythm with electrocardiograms,” adds Dr. Montero-Odasso.
This study was primarily funded by the Canadian Consortium on Neurodegeneration in Aging (CCNA), a collaborative research program tackling the challenge of dementia and other neurodegenerative illnesses. The CCNA was supported by a grant from the Canadian Institutes of Health Research
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Western delivers an academic experience second to none. Since 1878, The Western Experience has combined academic excellence with life-long opportunities for intellectual, social and cultural growth in order to better serve our communities. Our research excellence expands knowledge and drives discovery with real-world application. Western attracts individuals with a broad worldview, seeking to study, influence and lead in the international community.
The Schulich School of Medicine & Dentistry at Western University is one of Canada’s preeminent medical and dental schools. Established in 1881, it was one of the founding schools of Western University and is known for being the birthplace of family medicine in Canada. For more than 130 years, the School has demonstrated a commitment to academic excellence and a passion for scientific discovery.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Evaluating virtual symptom tracking for COVID-19 positive patients, new study
LONDON, ONTARIO - A research study from the Cardiac Arrythmia Network of Canada (CANet) and Lawson Health Research Institute is testing the use of a new online patient care platform designed to help track symptoms for COVID-19 positive patients.
Patients are now being enrolled in the study from the Urgent COVID-19 Care Clinic at London Health Sciences Centre. This virtual clinic helps identify, triage, monitor and manage potential complications for people recovering from COVID-19 at home. Patients can self-monitor their health with ongoing access to virtual physician support.
The COVID-19 Virtual Care at Home research study is testing the use of VIRTUES (Virtual Integrated Reliable Transformative User-Driven E-health System), a virtual, patient-centred platform created by CANet to help guide COVID-19 positive patients in managing their illness. They will have remote access to a team of health care providers including those specialized in the fields of cardiology, emergency medicine, internal medicine, infectious disease, neurology and respirology.
“Using VIRTUES, the care team can monitor a range of symptoms remotely that tells us a lot about how the patient is doing. In addition to tracking their temperature, we are using a home-based pulse oximeter to measure pulse rate and oxygen saturation,” says project co-lead Dr. Marko Mrkobrada, LHSC physician and Lawson Associate Scientist.
As symptoms are logged and tracked, there are alerts for communication between the patient and members of the care team. They can react quickly if additional care is needed such as a visit to the doctor’s office or hospital.
“The COVID-19 pandemic has highlighted the need for effective virtual health care,” says Dr. Anthony Tang, CANet CEO and Scientific Director. “Technology solutions support this care by giving both patients and health care providers fast and accurate access to critical information about symptom progression.”
As a made-in-Canada solution, CANet partnered with Clearbridge Mobile, an application development company in Toronto, to adapt an existing virtual care platform. “We responded quickly to provide a way for health care providers to remotely monitor, triage and manage care for patients with COVID-19, and help identify early on those who are at higher risk of complications,” adds Dr. Tang. Before the pandemic, VIRTUES was used for remote monitoring and care for patients with implantable cardiac defibrillators and pacemakers.
“We want to learn more about making health care technology user-friendly. Patients will have more information about their care and hopefully will experience reduced anxiety,” explains project co-lead Dr. Erin Spicer, LHSC physician and Lawson Associate Scientist. “While the majority of COVID-19 cases don’t require hospitalization, this system allows us to more closely monitor a patient’s progress and make informed decisions if their symptoms worsen.”
This research project highlights the importance of collaborative effort. Most importantly, with patient partners' active participation in helping design the VIRTUES platform and this research project. Along with CANet’s investment to adapt the VIRTUES platform for this project, the Department of Medicine at Western University’s Schulich School of Medicine & Dentistry has provided active support with many sub-specialists and investments from the Centre of Quality, Innovation and Safety (CQuinS) program.
“I am proud to be associated with this vital initiative. This research project will be comforting for patients contracted with COVID-19, providing reassurance that they are cared for by experts and monitored with technology advancement.” Dr. James Calvin, citywide Chair/Chief of Medicine.
The research team explains that these types of remote care systems may be able to play an important role in stemming the spread of the virus, while providing high-quality, accessible care using fewer resources. It also provides a means of rapid and accurate tracking of case recovery.
“We want to keep people safe. Following evaluation of VIRTUES here in London, we hope to see it implemented across the province and beyond. Patients have access to enhanced care while being able to hopefully stay in their homes during their recovery, helping to decrease exposure of COVID-19 in the community and for frontline health care workers,” adds Dr. Tang.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
CANet is a Pan-Canadian multidisciplinary and multi-sectoral research and development network of investigators, well-positioned industry partners, patients, caregivers, and healthcare providers focused on arrhythmia research, technology development and commercialization, and digital transformation activities. CANet is funded in part by the federal government's Networks of Centres of Excellence (NCE), Canada's flagship science and technology program.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Genetic testing could personalize care for patients with Crohn’s disease, particularly women
LONDON, ON - In a study involving 542 Crohn’s disease patients, researchers at Lawson Health Research Institute examined whether a patient’s DNA can be used to identify their risk of severe disease. They found that patients with a genetic variant in a gene called FXR (farnesoid X-receptor) are much more likely to need surgery and to need it earlier in their care journey. Surprisingly, they found that women with the genetic variant are at an even higher risk than men.
Crohn’s disease is an often debilitating condition that affects one in every 150 Canadians. The condition is characterized by intestinal inflammation caused by unnecessary attacks from the body’s immune system. It’s a disease that can behave and progress differently from one person to the next, with some requiring surgery to remove affected parts of the intestine.
“While medications are prescribed to manage Crohn’s disease, physicians have to balance the risk of side effects with the risk of undertreating severe cases of the disease,” explains Dr. Aze Wilson, Associate Scientist at Lawson Health Research Institute and Gastroenterologist at London Health Sciences Centre (LHSC). “In order to personalize treatment, it would be great to have a tool for identifying which patients will have the most severe cases of illness.”
Dr. Wilson and her colleagues became interested in the FXR gene because of its role in intestinal health. The FXR gene is a part of human DNA that controls how we process drugs and has also been linked to how well our intestines work. The research team suspected that variation in the gene could lead to poorer outcomes in Crohn’s disease patients.
“Given the importance of FXR to intestinal health, we wanted to see whether it plays a role in disease severity and we discovered that it does,” says Dr. Wilson. “Our findings suggest that genetic testing could be used to identify patients at a high risk of poor outcomes. This would allow physicians to tailor treatments to give patients the best chance at success.”
The team also discovered that women who carried the genetic variant were at the highest risk of needing surgery and the highest risk of early surgery, even when compared to men with the genetic variant. Struck by this finding, they conducted further testing using laboratory-based cell models. They found that estrogen (a female sex hormone) in combination with the genetic variant reduced the function of FXR even further.
“Differences between men and women with Crohn’s disease are not often considered in research or clinical practice. We apply treatments in the same way to both sexes, which may not be the best approach,” explains Dr. Wilson. “We identified a group of women who may benefit from a different approach to care. The study highlights the need for evaluating the effect of biological sex on disease and the interaction it may have with our DNA.”
Looking forward, the team hopes to further explore the effect of this genetic variant on intestinal health using laboratory-based cell models. They also hope to assess the value of genetic testing as a tool for informing treatment decisions made by patients and their physicians.
“One of our larger goals as a research group is to develop a personalized care plan for patients with Crohn’s disease and ulcerative colitis – one that integrates genetic information and other biomarkers to improve how care is delivered to these patient populations,” notes Dr. Wilson.
The study, “Genetic variation in the farnesoid X-receptor predicts Crohn’s disease severity in female patients,” is published in Nature’s Scientific Reports.
-30-
DOWNLOADABLE MEDIA

Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
ICU patients with non-brain-related injuries may suffer undetected cognitive dysfunction
LONDON, ON - A new study led by Western University and Lawson Health Research Institute has found that most patients entering hospital intensive care units (ICU) for non-brain-related injuries or ailments also suffer from some level of related cognitive dysfunction that currently goes undetected in most cases.
The findings were published today in the influential scientific journal, PLOS One.
Many patients spend time in the ICU for reasons that have nothing to do with a known brain injury, and most health care providers and caregivers don’t have any evidence to believe there is an issue with the brain. For example, a patient may have had a traumatic injury that does not involve the brain, yet still requires breathing support to enable surgeons to fix damaged organs, they may have issues with their heart or lungs, they may contract a serious infection, or they may simply be recovering from a surgical procedure like an organ transplant that has nothing directly to do with their brain.
For the study, Western researchers from the Schulich School of Medicine & Dentistry and the Brain and Mind Institute and researchers from Lawson assessed 20 such patients as they left the ICU and every single patient had detectible cognitive deficits in two or more cognitive areas of investigation, including memory, attention, decision-making and reasoning. Again, this is in spite of the fact that, on the face of it, they had no clear brain injury.
The discovery was made using online tests, developed by renowned Western neuroscientist Adrian Owen and his teams at the Brain and Mind Institute and BrainsCAN, which were originally designed to examine cognitive ability in patients following brain injuries but for this purpose, are being used to detect cognitive deficits in people who have spent time in an intensive care unit without a diagnosed brain injury.
“Many people spend time in an intensive care unit following a brain injury and, of course, they often experience deficits in memory, attention, decision-making and other cognitive functions as a result,” explains Owen, a professor at Schulich Medicine & Dentistry. “In this study, we were interested to see how patients without a specific brain injury fair after leaving the ICU. The results were astonishing.”
Why cognitive ability declines even in non-brain related visits to the ICU likely varies from patient to patient, but Dr. Kimia Honarmand from Schulich Medicine & Dentistry says the lesson to be learned is that many conditions affect brain function, even though they might not directly involve the brain.
“If you are having trouble breathing, your brain may be starved of oxygen. If you have a serious infection, the inflammation that occurs as a result of infection may affect brain function. If you are undergoing major surgery, you might be given drugs and have procedures that may affect your breathing, which in turn may affect the flow of oxygen to the brain,” explains Dr. Honarmand. “What we have shown here is that all or any of these events can lead to deficits in brain function that manifest as impairments in cognition. And healthy cognition is a vital determinant of functional recovery.”
Dr. Marat Slessarev, Lawson Scientist, says these findings can shift how the medical community treats incoming patients and more importantly, outpatients following ICU visits.
“Historically, the clinical focus has been on just survival. But now we can begin to focus on good survival,” says Dr. Slessarev, also an associate member at the Brain and Mind Institute and an assistant professor at Schulich Medicine & Dentistry. “These sensitive tests will enable doctors to both detect cognitive impairment and track cognitive performance over time, which is the first step in developing processes for optimizing brain recovery.”
-30-
Western delivers an academic experience second to none. Since 1878, The Western Experience has combined academic excellence with life-long opportunities for intellectual, social and cultural growth in order to better serve our communities. Our research excellence expands knowledge and drives discovery with real-world application. Western attracts individuals with a broad worldview, seeking to study, influence and lead in the international community.
The Schulich School of Medicine & Dentistry at Western University is one of Canada’s preeminent medical and dental schools. Established in 1881, it was one of the founding schools of Western University and is known for being the birthplace of family medicine in Canada. For more than 130 years, the School has demonstrated a commitment to academic excellence and a passion for scientific discovery.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Local researchers using artificial intelligence to lead the way in bedside lung imaging
LONDON, ON- A team at Lawson Health Research Institute are testing a new form of artificial intelligence (AI), paired with portable ultrasound machines, to image and identify lung concerns in real time, right at the beside of critically ill patients.
Approximately 100 critical care patients at London Health Sciences Centre (LHSC) will be part of this study which will test whether an AI model can automatically determine the presence of abnormal lung signals. Past studies have suggested that the AI model is very accurate in reading stored images, but this study will evaluate if it retains accuracy when asked to interpret live images being generated at the beside.
The study is made possible through the use of novel hardware created in Waterloo, Ontario by startup tech company, Wavebase.
“The (WaveBase) device attaches to the ultrasound machine and mirrors the ultrasound image in a second screen,” explains Dr. Robert Arntfield, Lawson researcher and Medical Director of the Critical Care Trauma Centre at LHSC. “The AI model searches the images for patterns in real time and predicts whether it is ‘seeing’ normal or abnormal lung tissue.”
Although bedside lung ultrasounds are commonly used in critical care to detect concerns such as infections, pneumonia or a collapsed lung, the pairing with real time diagnostic AI is a research milestone. It could expand the usage of bedside ultrasounds by enabling those with little or no ultrasound training to use the device.
“Bedside lung ultrasounds in critical care can often have a large impact in identifying life-threatening conditions within minutes,” says Dr. Chintan Dave, Critical Care Medicine Fellow at LHSC and Western University. “We would like to see members of the healthcare team, like critical care nurses or respiratory therapists, be able to use AI to accurately determine the health of the lungs rapidly at the bedside. Employing AI into the clinical workflow, could improve access to immediate diagnoses and treatments.”
In order to be certain that the AI’s predictions are accurate, the phase one study will compare its interpretations to a gold standard experts’ interpretation of the same lung ultrasound scans. Once this accuracy is assured, the team will proceed with a second phase to assess the device with non-expert users and customized settings for more in-depth diagnostics.
“We see a bright future for lung ultrasound imaging with AI within the critical care environment,” adds Dr. Arntfield. “We are trying to write the first chapter of this meaningful AI story here at LHSC and Lawson.”
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Local scientists creates novel test that could easily diagnose repetitive blast injury
LONDON, ON- In a world first, researchers at Lawson Health Research Institute, together with scientists from Defence Research and Development Canada, have developed a breath test that could be used to diagnose repetitive blast injury – a mild traumatic brain injury resulting from pressure changes that occur during explosions. The device will soon go through clinical trials to validate its efficacy.
“A pressure wave is sent through the head and brain after an explosion, resulting in effects similar to a concussion,” says Dr. Douglas Fraser, Scientist at Lawson and Professor at Western University’s Schulich School of Medicine and Dentistry. “Examples of individuals who are most at risk of this condition include military personnel, police, individuals in the mining industry and tragically the public, who are currently experiencing this first hand through the war in Ukraine.”
The test leverages findings from a new peer-reviewed study in the Journal, Frontiers in Neurology. The research team examined blood biomarkers in members of the Canadian Armed Forces who have experienced repetitive blasts.
“When we looked at these service personnel there were certain metabolites in their blood that had changed quite dramatically compared to those who had not been exposed to blast injury,” explains Dr. Fraser, who is also a Paediatric Critical Care Physician at London Health Sciences Centre. “What was remarkable about these metabolites is that some of them are expelled in a person’s breath.”
Currently there is no accurate way to diagnose repetitive blast injury other than relying on a patient’s history and symptoms. Using their findings, the research team has identified a combination of metabolites that can be measured in breath as a diagnostic test.
“The individual would blow into what looks like a straw and the breath would go into a device which would measure the metabolites of interest,” adds Dr. Fraser. “The device would then determine if the person is in the danger zone, or if they have been exposed to too many blasts.”
Dr. Vivian McAllister, Director of the Office of Military Academic Medicine at Schulich Medicine & Dentistry says this discovery could be a game changer when it comes to this condition.
“The symptoms of blast injury overlap with other neurological conditions, especially depression, so accurate diagnosis is essential,” says Dr. McAllister. “Early diagnosis allows for interventions that we know to be successful in reducing the symptoms and consequences of mild traumatic brain injury.”
The test has been developed and patented with WORLDiscoveries, the technology transfer and business development office for Lawson and Western, and licensed to Neuroltixs Inc. for development. The next steps will be to confirm the efficacy of the test through upcoming clinical trials.
“We hope to validate the breath aspect of the test, which could then be used as a health surveillance tool,” says Dr. Fraser. “Once validated through clinical trials, this portable device could be easily developed and it will allow us to determine who has been over exposed to blast injuries and how we can protect them in the future.”
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Locally developed test found to increase diagnosis of rare hereditary disorders
LONDON, ON – A clinical trial named “EpiSign-CAN,” led by researchers at Lawson Health Research Institute (Lawson) has been awarded $4.8 million to measure the clinical impact of a new molecular genomics test for diagnosing genetic neurodevelopmental conditions.
Developed at Lawson, the diagnostic test, called EpiSign, uses machine learning to analyze the EpiSign Knowledge Database. This database compiles information on rare genetic diseases using laboratory analyses of the entire genome, referred to as the epigenome, from patients with suspected genetic abnormalities.
A recent paper describes the newly discovered biomarkers for over 50 neurodevelopmental conditions. Dr. Bekim Sadikovic, Lawson Scientist and Head of the Molecular Diagnostics Division at London Health Sciences Centre (LHSC) explains, “before this study, many such conditions required targeted, and often labour intensive and costly assays for a diagnosis, which in many cases provided no conclusive answers. Now, using our EpiSign Knowledge Database which includes the epigenomic information of thousands of patients and controls, we are able to diagnose over 50 conditions with a single test, including in patients where targeted genetic testing was inconclusive.”
The upcoming clinical trial hopes to validate the use of this test in the first-line of diagnosing rare genetic disorders across Canada. “Patients and families typically wait years, and undergo multiple exams and lab tests in search of a definitive diagnosis. With EpiSign, we estimate that we will be able to increase the number of people who receive a diagnoses by five per cent, or more in the future as the database develops” explains Dr. Sadikovic. “Though individual genetic conditions are rare, there are over 4,000 recognized genetic disorders which affect thousands of patients in Canada.”
EpiSign-CAN will study 4,000 patients, who will either receive EpiSign testing as part of the initial diagnostic workup or after classical genetic testing approaches have been exhausted. The goal is to assess the impact of using EpiSign in the first stage of diagnosis vs. after other tests have failed to provide answers in this patient population.
Timely diagnosis will prevent the so called “diagnostic odyssey,” and by doing so has the potential to improve healthcare outcomes for these patients and decrease cost to the health system.
As the EpiSign Knowledge Database continues to grow, researchers are finding correlations between specific episignatures, or molecular DNA markers, and related physiological features across a syndrome.
This research is co-funded through the collaboration of three partners; LHSC, Illumina, and Genome Canada. This is the first time researchers at Lawson have been awarded a Genome Canada Genomic Applications Partnership Program (GAPP) grant. “Genome Canada focuses its resources on new innovation that has a strong likelihood of translating directly to patient care. Their support of our work is extremely meaningful,” says Dr. Sadikovic.
The study describing the most recent advancements in EpiSign technology, “Evaluation of DNA methylation episignatures for diagnosis and phenotype correlations in 42 Mendelian neurodevelopmental disorders,” is published in The American Journal of Human Genetics.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
London expands approach to prevent discharge from hospital to homelessness
LONDON, ON - During a virtual event for Londoners hosted by Lawson Health Research Institute and the City of London, a multi-sectoral research team announced two projects representing a collaborative approach to preventing homelessness from within hospital walls.
Built on the unique and successful No Fixed Address (NFA) strategy, these projects are being tested as a potential best practice for preventing hospital discharge to homelessness. NFA seeks to stop the cycle between hospital admissions and homelessness by providing timely and accessible supports to patients who would otherwise be discharged into homelessness. It brings housing and financial supports into the health-care system, starting as soon as upon admission, to assist in finding appropriate housing and supports or avoiding a potential eviction.
“Canada lacks a validated and coordinated service model to address the issue of hospital stay to no fixed address, which can often be the beginning of an individual’s experience with homelessness,” explains Dr. Cheryl Forchuk, Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, and Assistant Scientific Director at Lawson. “There are multiple factors that cause people to be discharged into homelessness - systemic, organizational and personal. We need a collaborative and coordinated approach that honours housing as a basic human right.”
Several departments at London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London collaborate with staff from the City of London, Canadian Mental Health Association (CMHA) Elgin-Middlesex, Youth Opportunities Unlimited (YOU), Salvation Army’s Housing Stability Bank and Ontario Works in the City of London to provide direct, on-site (or virtual) support for patients at risk of homelessness.
“Implementing a coordinated approach to addressing homelessness allows our staff to actively work alongside our partners in health care to prevent and divert individuals and families from an experience of homelessness by assessing their needs and connecting them to the housing supports.,” says John D’Oria, Coordinated Access Manager, City of London. “Whether it’s financial, social service or mental health support, this partnership and approach allows for a holistic approach to client care at the right time.”
Patients discharged from hospital to homelessness in Canada face many challenges that make recovery more difficult. They often experience higher readmission rates and emergency department visits. This is particularly concerning for youth, who have been found to be the fastest growing segment of the homeless population.
NFA was initially tested with strong success for mental health patients across the city and the second version of the project was extended to medical units at LHSC’s University and Victoria Hospitals.
PROJECT 1: Collaboration to Address Homelessness - Health, Housing and Income (H2I)
This research study will evaluate the City of London’s Coordinated Access Outreach program at hospital sites. A Coordinated Access Outreach worker will support individuals at risk of homelessness to maintain or obtain housing. Ontario Works will assist with the provision of income and employment supports and the Salvation Army Housing Stability Bank may be accessed for needed financial resources to secure or maintain housing.
Over two years, 106 participants will be interviewed in hospital and again six months post-discharge. Focus groups with participants, health care providers and community partners will provide further insight into the effectiveness of NFA. This project is funded by the Canada Mortgage and Housing Corporation (CMHC)’s National Housing Strategy.
PROJECT 2: Preventing discharge to No Fixed Address – Youth (NFA-Y)
This research study will customize, implement and evaluate the NFA strategy for vulnerable youth ages 16-24. The unique health and housing needs of youth at-risk will be explored by streamlining housing and financial support into a coordinated system of care, with additional support provided by Youth Opportunities Unlimited and Children’s Aid Society London and Middlesex.
Over 3-4 years, data to be collected from 93 youth at three time points. Focus groups with youth participants, health care providers, and community agency partners will help enhance the NFA strategy to meet the unique needs of youth. This project is funded by the National Centres of Excellence (NCE) Making the Shift (MtS) Youth Social Innovation Lab.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
London ranks in top ten of Canada’s research hospitals
MEDIA RELEASE
For immediate release
January 18th, 2022
LONDON, ON – Lawson Health Research Institute has ranked eighth in the country for the 2021 edition of Canada’s Top 40 Research Hospitals List by Re$earch Infosource. This is the eighth consecutive year that Lawson has maintained this strong national position, which puts the institute within the top five in Ontario.
Lawson, the research institute of London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London, has also maintained the top ranking for research intensity among the large tier institutions with a little more than $600,000 of research spending per researcher.
“This is a validation of the extensive support from LHSC and St. Joseph’s, our hospital foundations, Western University and our staff and physicians,” says Lawson’s Scientific Director Dr. David Hill. “These strong partnerships make the hospital environment in London a nationally recognized centre of discovery and knowledge translation.”
Hospital-based researchers belong to a health system at the forefront of the ongoing COVID-19 pandemic. With close proximity to patients and access to samples, they have mobilized to address COVID-19 in many different ways, and are making a difference around the world when it comes to advances and discoveries.
“The Province of Ontario designated health research as an essential service early in the pandemic,” explains Dr. Hill. “They understood that only science can get us through this, be it through vaccine development, surveillance and testing, evaluating new drugs to help patients in ICU survive, or studying the long-term health impacts. We have made substantial contributions of new knowledge through Lawson.”
The top 40 list analyzes hospital-based research institutes from across the country on several metrics, including total research income from the previous fiscal year. According to the report, Lawson received $121,888 million in research income in 2021.The ranking looks at funds received from all sources, including both internal and external, to support research at LHSC and St. Joseph’s.
Quick summary of Lawson’s ranking
- Rank in Top 40 Research Hospitals 2021: 8 (same as 2020)
- FY2020 research spending: $121,888 million
- Percentage change 2019-2020: 2.6%
- Research intensity: $618,700 thousand per researcher
- Research intensity - percentage of total hospital spending: 7.0%
-30-
About Lawson Health Research Institute: Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
For more information, please contact:
Celine Zadorsky
Communications & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. 75664
C: 519-619-3872
@email
www.lawsonresearch.ca/news-events
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
London researchers discover novel method to diagnose long COVID
Study found unique blood biomarkers in patients with post-COVID-19 condition
LONDON, ON – Published this week in Molecular Medicine, researchers at Lawson Health Research Institute have found that patients with post-COVID-19 condition (long COVID) have unique biomarkers in their blood. The team is now working on developing a first of its kind blood test that could be used to diagnose long COVID. The discovery could also lead to new therapeutics for this condition.
Long COVID occurs when someone experiences symptoms like fatigue, cognitive issues, shortness of breath and gastrointestinal issues after an initial COVID-19 diagnosis. It can sometimes take up to 12 months for the condition to occur.
“It’s estimated that 30 to 40 per cent of patients with COVID-19 will develop long COVID,” says Dr. Douglas Fraser, Lawson Scientist and Critical Care Physician at London Health Sciences Centre (LHSC). “Physicians currently rely on symptoms alone to diagnose the condition, but our research offers a unique profile of blood biomarkers that could be used in a clinical test.”
The researchers studied 140 blood samples from participants at LHSC and St. Joseph’s Health Care London, including St. Joseph’s Post-Acute COVID-19 Program. Participants were those with presumed long COVID, hospital inpatients with acute COVID-19 infection and healthy control subjects.
“We chose to study blood vessels that link all the body systems together to look for changes after an acute infection,” explains Dr. Fraser, who is also a Professor at Western University’s Schulich School of Medicine & Dentistry.
The team found that blood vessels of those with presumed long COVID were changing rapidly after a confirmed COVID-19 infection. They also found that patients with long COVID had 14 elevated blood biomarkers associate with blood vessels. With the help of machine learning, they discovered that two biomarkers called ANG-1 and P-SEL could be used to classify long COVID with 96 per cent accuracy.
“Long COVID is a relatively new condition and we have much to learn about it,” says Dr. Michael Nicholson, Associate Scientist at Lawson, Respirologist at St. Joseph’s and Associate Professor at Schulich Medicine & Dentistry. “This research advances our understanding of long COVID with the potential to improve diagnosis and patient care.”
The advantage of biomarkers is that they not only help diagnose a disease but also provide insight into potential treatments. The team is now focused on using their findings to create a clinical diagnostic test with a goal of also exploring therapeutics.
“With a point-of-care diagnostic test, we could confidently diagnose long COVID and eventually develop targeted therapeutics against these blood vessel changes that we have discovered,” says Dr. Fraser. “The ultimate goal is to improve patient outcomes following a long COVID diagnosis.”
This research was supported by funding from London Health Sciences Foundation, London Community Foundation and the AMOSO Innovation Fund. It builds on a growing body of COVID-19 research from scientists at Lawson Health Research Institute.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
