Search
Search
Over $10 million in funding announced from CIHR
Health researchers from across London were awarded more than $10 million from Canadian Institutes of Health Research (CIHR), with $2.8 million through Lawson Health Research Institute and $7.3 million through Schulich Medicine & Dentistry. A total of 15 projects were funded.
CIHR’s Project Grant program is designed to capture ideas with the greatest potential for important advances resulting in the creation of new knowledge and its translation into improved health and health care for Canadians.
Congratulations to all of the successful applicants!
Projects through Lawson Health Research Institute:
Karen Bosma, and Laurent Brochard: “Proportional Assist Ventilation for Minimizing the Duration of Mechanical Ventilation: The PROMIZING Study.”
Critically ill patients frequently require the life-sustaining technology of mechanical ventilation, but prolonged use can place patients at risk for long-term functional impairment and increased mortality, and is also costly to the health care system.
The PROMIZING Study is an international, multi-centre randomized clinical trial that will identify ways to reduce the duration of mechanical ventilation for patients at greatest risk and to determine whether a novel mode of ventilation developed in Canada could replace the standard of care.
“It is vital that Canada continue to invest in high impact, hospital-based research such as the PROMIZING study which enable researchers to develop and test treatments, technologies, and procedures that will improve clinically relevant, patient-important outcomes while also improving the efficiency of our healthcare system.” – Dr. Karen Bosma
Diane Bryant, and Alan Getgood: “Anterior Cruciate Ligament Reconstruction using Bone Patellar Bone or Quad Tendon Autograft with or without Lateral Extra Articular Tenodesis in Individuals who are at High Risk of Graft Failure (STABILITY II)”
Anterior cruciate ligament reconstruction (ACLR) is complicated by high failure rates in young active individuals, which is associated with worse outcomes and higher rates of osteoarthritis.
Currently, there are different types of grafts being used to rebuild a torn ACL. There is a need to evaluate whether one method is better at reducing failure, minimizing complications and creating better outcomes in terms of functional performance. This study will determine the best graft choice for young patients at risk of ACLR failure which will ultimately lead to positive effects on activity and quality of life.
Patrick Luke and Rabindra Bhattacharjee: “Therapeutic potential of bloodless oxygenated perfusion of donor kidneys for prolonged storage and protection for transplantation.”
Kidney failure among Canadians has tripled over the last 20 years. Transplantation improves the quality of life and survival of patients at a much lower cost than dialysis. However, only 40 per cent of patients receive functional kidneys due to lack of living organ donors.
To increase the number of kidneys available for transplantation, surgeons are accepting orgrans from deceased donors. Currently, during storage, the organs can suffer injuries from a lack of oxygen as well as cold temperatures and the conditions are not conducive to use drugs that can prevent damage.
The study is looking at the effects of a bloodless oxygen carrying perfusion liquid that will allow the storage of human donor kidneys for long periods of time at room temperature, and will also evaluate if certain drugs can maximize the preservation of these organs.
“Hospital-based research institutes are uniquely positioned to conduct patient-centred research. Investment through CIHR supports the physicians and researchers who are committed to improving treatments for patients at the front line of care.” – Dr. Patrick Luke
Emil Schemitsch: “The DECIPHER Study: DEterminants of Function and Clinically Important outcomes in Proximal Humerus Fractures in the Elder Population: A National CohoRt.”
Shoulder fractures are becoming increasingly common for older adults and cause considerable limitations and impacts for their daily life. While different approaches are taken to treat shoulder fractures, there is a lack of knowledge and evidence to show which of those methods are the most effective and for which patients.
The DECIPHER study will seek to answer important questions about which treatment and rehabilitation strategies are best for different patients, strengthening the clinical strategy for managing these difficult and prevalent injuries. It will also provide an economic analysis to understand the impact for healthcare system costs.
“Such an analysis has the potential to significantly affect patient care and Canadian practice patterns, as well as inform the development of future pivotal clinical trials. DECIPHER will have an important impact on patient care, health system costs and future research directions locally, nationally and internationally.” - Dr. Emil Schemitsch.
Projects through Schulich Medicine & Dentistry:
Subrata Chakrabarti, with collaborators Bekim Sadikovic, Krishna Singh, and Stephanie Frisbee: “Novel mechanisms in diabetic cardiomyopathy.”
Peter Chidiac and Jeffrey Dixon: “Allosteric regulation of GPCR signaling by extracellular nucleotides.”
Bryan Heit: “Role of ELKS1 and Rab17 in Differential Antigen Sorting and MHC II Trafficking Following Efferocytosis and Phagocytosis.”
Marlys Koschinsky and Michael Boffa: “B Apo(a):apoB100 interactions as key determinants of Lp(a) biosynthesis.”
Shawn Li: “Novel anticancer immunotherapy targeting the molecular mechanisms of T cell suppression by immune checkpoints.”
Julio Martinez‐Trujillo and Michael Poulter: “Reverse engineering working memory circuits in the primate brain: Implications for the study of memory deficits.”
Maria Mathews and Jennifer Shea with collaborators, Ivy Bourgeault, Emily Marshall, Amy Bombay, Nicole Doria, Julia Lukewich, and Amanda Myers: “Increasing Indigenous Participation in the Physician Workforce.”
Charles McKenzie, and Timothy Regnault: “Hyperpolarised 13C MRI of Placental Metabolism in Intrauterine Growth Restriction.”
Marco Prado: “A Regulation of chaperone‐mediated proteostasis by STI1.”
Lloy Wylie and Lana Ray with collaborators Christopher Mushquash, Victoria Smye, Nadine Wathen, Cheryl Forchuk, and Brock Pitawanakwat: “Educating for Equity: Building Culturally Safe Care through Indigenous Narratives.”
Xiufen Zheng: “The role of circular RNA in heart transplantation”
Over $2 million in federal funding to advance discoveries in health research
Last week, the Honourable Kirsty Duncan, Minister of Science and Sport, announced an unprecedented investment of more than $588 million through the Natural Sciences and Engineering Research Council of Canada’s (NSERC) Discovery Grants program.
The successful applications in London include 12 projects funded for Lawson Health Research Institute scientists, through Western University. In total, they will receive $2.3 million in funding over five years.
“The funding demonstrates our strong and enduring commitment to science and researchers. Since taking office, our government has worked hard to bring science and research back to their rightful place and this historic investment in the discoveries of tomorrow is just one example of how we are achieving this goal,” says The Honourable Kirsty Duncan, Minister of Science and Sport.
Across Canada, this funding will go to more than 4,850 researchers and students as they pursue their world-leading discovery work. It also includes support for nearly 500 early-career researchers who will bring a diversity of new voices and new insights to their fields.
Local research highlights
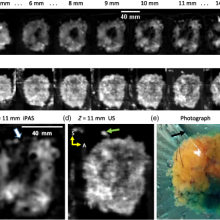
Dr. Jeffrey Carson is exploring the role of photoacoustic imaging as a method for detecting breast cancer. Currently, during the procedure the breast must be submerged in a tank of water to enhance the transmission of photoacoustic waves from the breast to the sensors.
“The water tank is cumbersome and impractical,” notes Dr. Carson. “Our goal is to eliminate the need for the water tank by detecting the photoacoustic waves through the air without making contact with the breast.” Their hope is that the project leads to the development of a non-contact photoacoustic scanner offering women the opportunity to sit or stand comfortably during breast imaging. “This simple improvement could greatly accelerate the adoption of photoacoustic imaging for breast cancer screening.”
Dr. Carson adds that funding like this provides graduate student trainees opportunities to develop knowledge and skills in engineering, mathematics, and biophysics. “They bring innovative new ideas to the Canadian medical device industry through employment and entrepreneurship.”
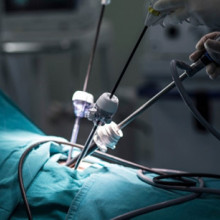
Dr. Rajnikant Patel is developing advanced robotic and intelligent systems for the next generation of systems and devices for minimally invasive surgery and therapy. These reduce trauma and costs while enhancing efficiency and reliability.
“For us, this funding opportunity is unique because it supports a program of research rather than a project,” says Dr. Patel. “We can explore new areas and directions that will lead to research projects and medical applications. A program that investigates novel robotic and AI technologies fits well with NSERC’s mandate.”
Dr. Gregor Reid is leading a revolutionary project that could save the world’s honeys bees, insects that are vital to human survival.
The intent is to develop an understanding of how lactobacilli strains can counter the most widely used pesticides that are wiping out nature's critically important pollinators. The lactobacilli appear to potentially degrade some of these toxic chemicals and improve the ability of honey bees to fight off early death.
“NSERC funding gives ideas like this a chance and even though the funding amount is relatively small, it allows graduate students to apply for their own awards and work on the project,” explains Dr. Reid. Students Brendan Daisley and Johnny Chmiel have been awarded NSERC scholarships to work on this important research.

Dr. Xiugen Zheng’s project is investigating the role of circular RNA AEBP in the development and function of dendritic cells which are very important immune cells in the immune system. This will provide insights into new molecular and gene regulators, and their impact on the immune system and overall health.
“NSERC research funding greatly supports us to study the basic scientific questions that are critical for better understanding health problems and developing treatment for diseases,” says Dr. Zheng.
Dr. Rudolf Veldhuizen’s laboratory aims to understand how surfactant performs its function at a molecular and biophysical level. Pulmonary surfactant is a material in the lung that allows people and other mammals to breath with minimal effort. You can see this in babies who are born prematurely and have trouble breathing due to the lack of surfactant.
“Previous work has established a generalized model of how surfactant improves lung function under standardized conditions. This, however, does not explain how surfactant functions in extreme conditions,” says Dr. Veldhuizen. “By exploring conditions in comparative, mechanistic studies we will be able to establish a more universal understanding of surfactant function.”
This funded work provides a foundation for clinically relevant studies to further explore the role of alterations to surfactant in lung injuries and the opportunities for therapeutic interventions.

Dr. Shou Li is developing state-of-the-art machine learning system able to analyze huge amounts of clinical data and provide human level intelligent analysis. This work will enable the prediction of disease onset, progression and prognosis. “It is added value that will lead to more effective and efficient health care,” explains Dr. Li.
He adds that this funding is supporting a multi-disciplinary research program that combines the strength of multiple teams. “We will look at both the fundamental side of machine learning systems and clinical applications. In this way, we connect basic science with clinical science.”

Congratulations to all the Lawson scientists who received funding:
- Dr. Dean Betts for Metabolic reprogramming to enhance the generation of canine induced pluripotent stem cells (Physiology and Pharmacology)
- Dr. Jeffrey Carson for Development of non-contact photoacoustic tomography (Medical Biophysics)
- Dr. Louis Ferreira for Multi-Directional Mechanical Testing of Bone using CTCompatible Loading Mechanisms (Mechanical and Materials Engineering)
- Dr. Shuo Li for Innovative Machine Learning for Medical Data Analytics (Medical Imaging)
- Dr. Penny MacDonald for Investigating cognitive functions mediated by ventral and dorsal striatum (Clinical Neurological Sciences)
- Dr. Charles McKenzie for Fetoplacental Molecular and Metabolic Magnetic Resonance Imaging; instalment (Medical Biophysics)
- Dr. Rajnikant Patel for Design and Control of Robotic Systems and Devices for Medical Applications (Electrical and Computer Engineering)
- Dr. Gregor Reid for Detoxification functionality of lactic acid bacteria (Microbiology and Immunology)
- Dr. Rudolf Veldhuizen for Mechanisms of surface tension reduction by pulmonary surfactant (Physiology and Pharmacology)
- Dr. Aaron Ward for Machine learning-based quantitative image, tissue, and clinical data analysis for lesion detection and characterization on prostate cancer imaging (Medical Biophysics)
- Dr. Eugene Wong for Optimization of spatiotemporal-modulated electric fields and fabrication of organs-on-chips for applications in Medical Physics (Physics and Astronomy)
- Dr. Xiufen Zheng for The role of circular RNA AEBP2 in dendritic cells (Pathology)
Parkwood Institute Research Open House 2019
Parkwood Institute Research, a program of Lawson Health Research Institute, is hosting its third annual Open House and interactive tour showcasing research that is making an impact for patients and their families.
A part of St. Joseph’s Health Care London, Parkwood Institute represents the next era in care, recovery and rehabilitation. Across the site, clinical and research teams from across disciplines and specialties work together to bring tested solutions to the people who need them the most.
The special open house with interactive tour gives guests the opportunity to meet researchers and their teams to learn more about their work in the areas of Cognitive Vitality and Brain Health, Mobility and Activity, and Mental Health.
This free event is open to the public including members of London’s vibrant health care and research community.

Event Details
Date: Thursday, November 28, 2019
Time: 2:00 – 5:00 p.m.
Locations: Parkwood Institute Main Building Auditorium (Room B2-109)
*PLUS selected locations throughout the building. Directions to be provided.
Click here for directions to Parkwood Institute and parking maps.
The lot rate is $5.00 when you enter. $1 and $2 coins and credit card accepted (press the start button then insert payment)
Refreshments and snacks will be available along your tour.
If you have any questions, please contact @email
Download the event poster.
Parkwood Institute Research Open House 2020 – VIRTUAL EVENT
Parkwood Institute Research, a program of Lawson Health Research Institute, is hosting its fourth annual Open House showcasing research that is making an impact for patients and their families.
The special open house this year will move to a VIRTUAL platform making it even easier to connect to the researchers and their teams who work in the areas of Cognitive Vitality and Brain Health, Mobility and Activity, and Mental Health.
Why you should attend:
- See videos, demonstrations and project summaries presented by the different research teams.
- Participate in interactive activities so you can learn more about PIR and why their work matters.
- Ask questions to the research teams LIVE during the online event.
- Learn about ways to get involved with research.
- Have fun with live polls, games, match-making and more!
A part of St. Joseph’s Health Care London, Parkwood Institute represents the next era in care, recovery and rehabilitation. Across the site, clinical and research teams from across disciplines and specialties work together to bring tested solutions to the people who need them the most.
This free virtual event is open to anyone interested in learning more about hospital-based research happening in this region and getting to know members of London’s vibrant health care and research community.
Event Details
Date: Thursday, November 26, 2020
Time: 2:00 – 4:00 p.m.
Location: This is a VIRTUAL event being held on the Whova event and conference app. It can be accessed through a web browser or by downloading the Whova app on your preferred device.
If you have any questions, please contact PIR_Info@sjhc.london.on.ca.
Event poster
Partnership with Siemens Healthineers will create a centre of excellence in advanced diagnostic imaging and therapeutics
Continuing to build on the established excellence in medical imaging, London’s academic teaching hospitals, London Health Sciences Centre (LHSC), and St. Joseph’s Health Care London, and Western University’s Schulich School of Medicine & Dentistry announced a partnership with Siemens Healthineers in magnetic resonance imaging (MRI), interventional angiography, cardiology and cardiac surgery that will create a centre of excellence in advanced diagnostic imaging and therapeutics in southwestern Ontario.
This new partnership includes the creation of an education, training and scientific research support fund in the area of advanced diagnostic imaging and therapeutics. Siemens will provide in excess of $1 million in support funding for research, advanced clinical applications, teaching and outcomes analysis.
“This partnership represents another important building block in the incredible foundation of imaging excellence that we have in London,” says Dr. Narinder Paul, Chair/Chief of the Department of Medical Imaging at LHSC, St. Joseph’s, and Schulich Medicine & Dentistry.
“Not only will we become leaders in state-of-the-art imaging and intervention through the centre of excellence, but thanks to the research contribution from Siemens Healthineers, we will also have dedicated funds for critical research in cardiovascular and neurological diseases that will translate to improved services and outcomes for patients in London and the region.”
The research fund will support collaborations between research teams in diagnostic and interventional radiology, cardiology, and cardiac surgery, with imaging scientists at Lawson Health Research Institute, the research institute of LHSC and St. Joseph’s, and Schulich Medicine & Dentistry’s Robarts Research Institute, as well as research teams from across Western. These teams will partner with scientists from Siemens Healthineers to focus on improving both the patient experience and the outcomes in important cardiovascular and neurological diseases. The research funds will be leveraged against provincial and federal research grants to increase the funds available to the research teams.
“Collectively, Western and our partner institutions in London are becoming a global powerhouse, recognized for our expertise and facilities in imaging that drives discovery and innovation across a broad range of disciplines,” says Alan Shepard, President & Vice-Chancellor of Western University. “This partnership with Siemens Healthineers builds on our strengths, increases capacity to enhance patient care, and expands opportunities to integrate education, training and research for the benefit of learners and faculty. It’s a huge win for London and southwestern Ontario.”
“Imaging scientists and clinicians, working on campus and within hospital walls, have positioned London as a leader in non-invasive biomedical imaging, conducting groundbreaking research that impacts health care here and around the world,” adds Dr. David Hill, Lawson Scientific Director and Integrated Vice President, Research for London’s hospitals.
“With strong industry partnerships and working seamlessly with our hospitals and academic partners, we can build on this success. The advancements made here can be quickly translated into care within the very units where the testing is being done, which ultimately improves care for the patients and families that we serve.”
The centre of excellence will provide hands-on training in MRI, diagnostic, and interventional catheter procedures through development of advanced simulation and phantom models. Medical learners and radiologists, cardiologists, cardiac surgeons, neurologists, neurosurgeons, and technologists in London and from across Canada will be able to access this centre to improve their diagnostic and therapeutic skills, which will in-turn improve patient access to skilled clinicians.
As well, LHSC and St. Joseph’s are acquiring six clinical MRIs and six angiogram suites to be used for patient care, which will include the introduction of the first 3T MRI in the region. University Hospital will acquire a 3T/1.5T pair of MRIs, and two biplane angiogram suites. Victoria Hospital will acquire a 3T/1.5T pair of MRIs, a biplane and two single plane angiogram suites. St. Joseph’s will acquire a 3T/1.5T pair of MRIs, and a single plane angiogram suite.
“Investments in capital equipment, such as these new MRI machines and angiogram suites, are incredibly important as they will immediately translate into safer, higher quality care for the patients we serve – in this case it’s by offering the highest resolution images available, in less time, and with improved comfort for patients,” says Dr. Paul Woods, President and CEO, London Health Sciences Centre.
“London has an illustrious history of innovation that has been groundbreaking in shaping the scope and possibilities of medical imaging within the health-care system,” says Dr. Gillian Kernaghan, President and CEO, St. Joseph’s Health Care London. “This exciting partnership ensures our ongoing leadership and expertise in the introduction of leading-edge medical imaging technologies and is a critical step toward new approaches in imaging research and patient care.”
MRI is used to provide critical diagnostic information about the physical structure and the biological processes of the body. MRI scanners differ from other imaging technologies as they use strong magnetic fields, magnetic field gradients, and radio waves, instead of X-rays, to generate images of the organs in the body. MRI is widely used in hospitals to facilitate medical diagnosis and/or the staging of disease without exposing patients to radiation.