Search
Search
Revealing the culprit behind Parkinson’s disease
An estimated 55,000 Canadians are living with Parkinson’s disease. While researchers are advancing therapies to treat symptoms, such as tremors, there is currently no method to stop progression.
To begin addressing this problem, a team of scientists at Lawson Health Research Institute is developing an imaging tracer.
“There’s a protein in the brain called alpha-synuclein (α-syn) that scientists believe is a culprit in causing Parkinson’s disease. The protein forms in ‘clumps’ called Lewy bodies that kill brain cells and potentially lead to disease,” explains Dr. Justin Hicks, Lawson Imaging Scientist. “Unfortunately, we have no way to study it in human brains and this has limited our ability to test therapies against it.”
Efforts have been made to study the elusive protein through modern imaging techniques like positron-emitting tomography (PET). Scientists have attempted to develop a PET probe – a radioactive molecule that targets the specific protein in order to produce highly specific images or scans – but they have been unsuccessful.

Above: Dr. Justin Hicks working in the Nordal Cyclotron & PET Radiochemistry Facility
“Unfortunately, the Lewy bodies caused by α-syn are hard to distinguish from protein clumps found in Alzheimer’s disease and other dementias. This makes it very difficult to know whether a PET probe has found clumps associated with Parkinson’s disease.”
Through a new study, Dr. Hicks and his team are working to find a solution. To do so, they will examine a different but related protein.
“There’s another protein called fatty acid binding protein 3 (FABP3) and one of its roles is to ‘chaperone’ the α-syn protein in human cells. Past studies have shown that levels FABP3 are higher in patients with Parkinson’s disease when compared to healthy controls,” explains Dr. Hicks. “This suggests that high concentrations of FABP3 can be used as an alternate measure of α-syn.”
They hope to measure levels of the FABP3 protein in place of the α-syn protein, and gain a better understanding of the role that both proteins play in the development and progression of Parkinson’s disease. To image Lewy bodies associated with Parkinson’s disease, the researchers are working to produce a PET probe that targets FABP3.
To accomplish this, they will be working in their lab to find a chemical that targets FABP3. Once found, they will attach a radioactive isotope to the chemical and produce a finished tracer. The tracer will then be tested in preclinical models.
Once injected, the PET probe will find and stick to FABP3. The PET isotope will emit a small amount of radioactivity and these emissions will show up as PET images.
“The ultimate goal is to develop a PET probe that can be used to distinguish Parkinson’s disease from other neurodegenerative diseases. The probe could also be used to assess new therapies that reduce levels of the α-syn protein,” says Dr. Hicks. “If successful, we hope this research will lead to a better understanding of the progression of Parkinson’s disease and ways to prevent it.”
Dr. Hicks and his team are being funded for this project through Lawson’s Internal Research Fund (IRF) competition. “Lawson’s IRF is extremely important for early career researchers. It allows us to generate data and publications to then apply for larger external funding. It also permits an added level of risk to pursue projects that may not reach their end goal but often spur new lines of research.”
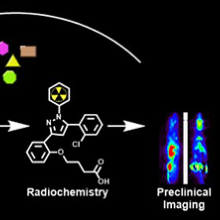
Above: A graphic depiction of this research project and its goals.
Revealing the secrets of dementia
The immune system is one of our greatest defenses against disease and injury. But what happens when it betrays us?
With conditions like rheumatoid arthritis the immune system is manipulated to attack the human body. Inflammation, normally a protective immune response, can be employed to cause symptoms like pain.
Surprisingly, research suggests our immune system may be similarly affected in patients with neurodegenerative dementias.
“We know there are increased numbers of inflammatory cells in the brains of patients with dementia but we don’t know what role they’re playing,” says Dr. Elizabeth Finger, a scientist at Lawson Health Research Institute and neurologist at St. Joseph’s Health Care London’s Parkwood Institute. “Are they doing their proper job of cleaning up damaged cells or is their presence more sinister?”
Dr. Finger’s research group aims to identify and understand changes in the brain that lead to symptoms of dementia, find novel treatments to improve patient quality of life and hopefully prevent the disease altogether. Critical to this work is Dr. Finger’s collaboration with Lawson Imaging scientists Drs. Keith St. Lawrence, Udunna Anazodo, and Justin Hicks.
The researchers utilize Canada’s first hybrid positron emission tomography and magnetic resonance imaging (PET/MRI) machine located at St. Joseph’s Hospital. This high-powered imaging allows them to assess changes to both structure and function in the brains of patients with neurodegenerative dementias like Alzheimer’s disease, frontotemporal dementia and Lewy body dementia.
In one of their many studies they are examining whether there is inflammation in the brains of patients with frontotemporal dementia and, if so, whether this inflammation is present in areas of the brain not yet damaged by the disease.
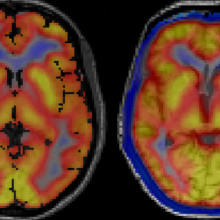
Images captured using a hybrid PET/MRI machine show activated immune cells in the frontal brain regions in a patient with frontotemporal dementia (right) compared to a healthy volunteer (left).
“A presence in those parts of the brain would suggest that inflammation is not playing its normal role of cleaning up damaged cells,” explains Dr. Finger. “It would suggest the brain’s immune response is overactive and that we should consider clinical trials for medications that modulate this response.”
Dr. Finger is an active investigator for novel therapies. In 2019, her group will participate in at least two clinical trials for medications that target genetic mutations that can cause frontotemporal dementia. The studies are phase I trials, which means they are the first time the medications are being tested in humans.
Dr. Finger is also leading a North American multi-centre trial called FOXY. The study will examine the therapeutic potential of a hormone called oxytocin to improve the loss of emotion and empathy that frequently occurs in patients with frontotemporal dementia.
“In the past there were very few treatments for frontotemporal dementia,” explains Dr. Finger. “We are glad to say that Lawson and St. Joseph’s will offer the opportunity to take part in these advances. Words cannot adequately express the appreciation we have for our patients, caregivers and healthy volunteers who participate in research. The time and effort they selflessly donate with the goal of helping future patients is truly inspiring and motivating.”

This story originally appeared in an annual publication from the Alzheimer Society London and Middlesex.
Scientists studying carbon monoxide as a possible treatment for sepsis
Sepsis is the leading cause of death worldwide with limited treatment options
MEDIA RELEASE
For immediate release
LONDON, ON – Sepsis is a life-threatening condition that occurs when the body’s response to an infection triggers excessive inflammation. The inflammatory response can cause damage to organs such as the heart, liver, lungs and brain. While there are currently limited treatments for sepsis, researchers at Lawson Health Research Institute are working to change that by examining the use of carbon monoxide-releasing molecules to treat patients. “This is an unusual approach that is looking at using carbon monoxide which is the infamous gas molecule,” says Dr. Gediminas Cepinskas, Scientist and Director of the Centre for Critical Illness Research at Lawson. “If administered and used in small non-toxic concentrations, carbon monoxide can offer very potent protective and anti-inflammatory effects.”
In studies on the subject, including the most recent one published in the journal of Experimental Biology and Medicine, the research team was able to demonstrate efficacy in using carbon monoxide-releasing molecules to protect individual cells in the liver and lungs of sepsis induced inflammation in preclinical models. “We have been working on isolated organs and organ specific cells to test carbon monoxide-releasing molecules to narrow down which specific cells are more sensitive to treatment and which biochemical pathways are involved,” Says Dr. Cepinskas. “We are making great progress in our work and have had success in addressing the efficacy of carbon monoxide-releasing molecules in preclinical models.”
Dr. Cepinskas is one of just a few scientists worldwide studying carbon monoxide-releasing molecules to treat inflammatory conditions such as sepsis. While carbon monoxide is commonly known as dangerous, using it in a controlled manner does not pose a danger and may have therapeutic potential. “Our immune system is usually our defense system, but with sepsis it becomes so activated it starts to attack our own cell tissues, resulting in injury and dysfunction of the affected organs,” explains Dr. Cepinskas. “Almost each and every cell in our body naturally produces carbon monoxide which is used in defense against harmful and injured stimuli. We are taking advantage of this knowledge and currently we are the only lab in Canada working on this potential carbon monoxide-based therapy.”
Dr. Cepinskas is also collaborating with clinicians at London Health Sciences Centre (LHSC) to study the use of carbon monoxide-releasing molecules to treat limb compartment syndrome and to improve organ transplantation.
The research team, which has patents in the area of carbon monoxide-releasing molecules, is now working with the pharmaceutical industry to move this potential therapy into human clinical trials in the future.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Sharing the gift of hope through research
Community members and those in the field of health research attended a special open house and interactive tour by research groups at Lawson Health Research Institute – celebrating the holiday spirit and the gift of hope that is made possible through hospital-based research.
A part of St. Joseph’s Health Care London, Parkwood Institute represents the next era in care, recovery and rehabilitation. Across the site, clinical and research teams in different disciplines and specialties are collaborating in new ways.
The teams that make up Parkwood Institute Research, a Lawson program, are conducting clinical studies with the goal of understanding disease and improving care for a wide range of patients.
“Many people in the community know the high-quality and compassionate care that is supported by the various clinical teams at Parkwood Institute,” says Dr. Cheryl Forchuk, Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, and Assistant Scientific Director at Lawson. “What most don’t know is that we have research teams working across these sites, with each other and research patients.
Researchers tackle the most important challenges and provide access to highly innovative and meaningful solutions that improve the lives of patients and their families, added Dr. Forchuk.

At the open house on November 30, there were 11 interactive displays in the areas of cognitive vitality and brain health, mobility and activity and mental health. This included the Gait and Brain Laboratory, the Operational Stress Injury Clinic, wound care, the Mental Health Nursing Research Alliance and more:
- The Mental Health INcubator for Disruptive Solutions (MINDS) of London Middlesex is a social innovation lab focused on developing, testing, implementing and evaluating disruptive solutions that promote the mental and emotional wellbeing of Transition-Aged Youth in our London-Middlesex community.
- The Canadian Consortium on Neurodegeneration in Aging (CCNA), supported by CIHR and many partners, is the premier research hub for all aspects of research involving neurodegenerative diseases that affect cognition in aging – including Alzheimer's disease.
- A dynamic lab with the top neurorehabilitation evidence-based reviews in stroke, brain injury, spinal cord injury and multiple sclerosis, or insight into clinical trials of stroke rehabilitation using exoskeletons, exercise paradigms, pharmaceuticals, and clinical studies of psychosocial factors that influence chronic pain in brain injury and spinal cord injury populations.
The open house had a festive theme and each of the exhibits involved a problem solving element to encourage learning and foster teamwork.

Peggy Sattler, Member of Provincial Parliament for London West, and Terence Kernaghan, Member of Provincial Parliament for London North Centre, were among the over 300 people in attendance.
“This special open house opportunity is meant to be a fun experience where you were also learning about research,” explains Dr. Forchuk. “During this holiday season, we wanted to share our own gift of hope in the form of collaborative research that is making a real difference.”
See photos from the open house on Facebook.
Small box holds big promise in cardiac care
London, Ontario – For a non-descript box it wields a mighty name and even more impressive possibilities for people with heart disease. Called the AngioDefender, the machine – no bigger than a shoebox - holds much promise in the ability to personalize cardiac care, say researchers at Lawson Health Research Institute, the research arm of St. Joseph’s Health Care London.
St. Joseph’s Hospital in London is the only Canadian cardiac rehabilitation centre testing the AngioDefender, a non-invasive tool that can assess the health of blood vessels by using a simple blood pressure cuff. At the recent Canadian Cardiovascular Congress in Toronto, Lawson researchers presented findings of their study, which assessed the feasibility and reliability of the AngioDefender in patients undergoing cardiac rehabilitation.
“Right now everyone basically gets similar treatment in terms of maximizing therapy based on risk factor profiles,” says Dr. Neville Suskin, Lawson scientist and medical director of St. Joseph’s Cardiac Rehabilitation and Secondary Prevention Program. “With this machine, if it does what we hope it will do, it gives us insight into a person’s vascular health so that we can know if the treatment is working and adjust and individualize their care.”
Also key, says Dr. Suskin, is the machine can be used by any medical professional in any doctor’s office.
The AngioDefender system, manufactured by Everist Health, measures the health of the endothelium — the interior lining of blood vessels. Using a blood pressure cuff, the device runs through a series of inflations and deflations to analyze the endothelium’s response to changes in blood flow. When the blood pressure cuff is inflated, blood flow decreases and stops. When the blood pressure cuff deflates, blood flow increases and the main artery in the arm responds by getting bigger (dilating). How well it dilates is a sign of endothelial (vascular) health.
Using a specially designed data analysis algorithm, the AngioDefender system produces each patient’s “flow-mediated dilation” score. When the information is combined with the patient’s other risk factors, it calculates the patient’s vascular age. The whole process takes 15 to 20 minutes.
“The ability for a health professional to obtain a measure of vascular health in such a straightforward manner is very novel” says Dr. Suskin, whose team has found that the machine is feasible to use in a busy cardiac rehabilitation practice setting. “It doesn’t take long, patients tolerate it, and they are also very keen to know their vascular health as determined by this machine.”
If successful, the device may become part of the standard screening to assess early-stage cardiovascular disease and atherosclerosis, and an innovative way to monitor the effectiveness of treatment.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Renowned for compassionate care, St. Joseph’s Health Care London is a leading academic health care centre in Canada dedicated to helping people live to their fullest by minimizing the effects of injury, disease and disability through excellence in care, teaching and research. Through partnership with Lawson Health Research Institute and our collaborative engagement with other health care and academic partners, St. Joseph’s has become an international leader in the areas of: chronic disease management; medical imaging; specialized mental health care; rehabilitation and specialized geriatrics; and surgery. St. Joseph’s operates through a wide range of hospital, clinic and long-term and community-based settings, including: St. Joseph’s Hospital; Parkwood Institute; Mount Hope Centre for Long Term Care; and the Southwest Centre for Forensic Mental Health Care. www.sjhc.london.on.ca
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Smart Homes for community living
A first-of-its-kind research study by Lawson Health Research Institute is moving into the community and evaluating the use of smart technologies in the home for people with severe mental illness.
After prototyping this approach within a hospital setting through St. Joseph’s Health Care London, the research team will be outfitting eight affordable housing units at Canadian Mental Health Association Middlesex and London and Middlesex Community Housing with smart home technology.

In-hospital prototype for using smart technologies in the home
The Smart Home Community Model
“This solution is for people who are having difficulty managing their everyday life and need a high level of care to maintain community living,” says Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson and project lead for the Smart Home Community Model. “Technology and applications are being embedded in the lived environment and then tested to ensure they are safe, secure and appropriate for use in health care.”

Dr. Cheryl Forchuk announcing this phase of the project, from within one of the apartment buildings.
Study participants will select from a wide range of tools that will best meet their individual needs. Devices such as smartphones and touch-screen monitors connect with applications to provide video-conferencing, questionnaires, and prompts and reminders based on the person’s care plan.
As an example, participants have regular access to mood scales with questions about how they are feeling. These are used extensively in mental health care settings to help address issues and start conversations with clients. The care team receives notification of the answers, giving regular insight into how the person is doing and if they need additional follow-up.

Depending on their needs, participants have access to automated medication dispensers and smart health monitoring devices, such as weigh scales, blood pressure monitors, glucometers, and tracking monitors for heart rate, activity and sleep.
This patient population often faces health challenges on multiple fronts, with higher rates of diabetes and cardiac issues. They can struggle keeping balance when it comes to activity, weight and sleep. Fluctuations in any of these can be early indicators that a crisis is looming.
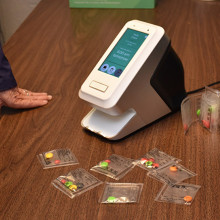
“By integrating and testing these smart tools for health care, we are not simply looking at the technology but how it can be used as a tool for communication,” says Dr. Forchuk. “We see smart technology supporting more seamless communication between health care providers and the client – all from their own homes. This helps them better manage their care and overall wellbeing, flag issues earlier on and avoid trips to the clinic when appropriate.”
Paula's Perspective
Paula Rawlinson is chair of the family council and sits on the patient council for St. Joseph’s Parkwood Institute Mental Health Care. She personally has lived experience with mental health and as also acted as a caregiver for a family member.
“Both myself and my family member could have benefitted from these tools, very much so,” says Paula. “When I was really suffering, I isolated myself from people a lot. Even when I lived in a group home because I needed a higher level of care. Having some sort of helpful device right there, encouraging me to keep up with things and connecting me to someone I trusted, would have made a huge difference. Especially after the first discharge.”

She adds that for someone who is really struggling, this could be a life-saving strategy that makes a vital difference.
For her family member, Paula sees many uses for these tools and knows that they would actually use them. “I’ve been able to see the tools and they are even simpler than using email. It makes them accessible to a lot of people in the community who would make good use of them to improve their situation.”
Results and Impact
Some of the tools as part of this project have previously been tested formally as part of a research study and shown positive results.
The health team has access to the data to more easily stay in touch with the person. They can work together to track trends and pinpoint triggers, creating more personalized and effective strategies. With less focus on the daily aspects of care, providers reported that in-person meetings offered more meaningful and important discussions.
“All of the data is also viewable by the client who continues to work with a health care provider,” explains Dr. Forchuk. Clients can reach out sooner and get support more quickly. Potential issues and crisis are addressed earlier on, and in previous studies they reduced psychiatric readmissions, emergency room visits and arrests. Clients reported more satisfaction with their care and feeling better overall.

“When we have more people successfully achieving community living and managing their care with fewer outpatient visits and other service utilization, we can open up capacity in the system and deliver quality care at a lower cost.”
The team anticipates that participants will experience greater levels of independence and autonomy in maintaining housing and self-care for mental health and chronic illnesses.
Paul points out that one of the key outcomes is to avoid re-admission. “One of the main, recurring struggles is loneliness. With tools to keep people in more regular contact with their care team and assistance with their everyday life, they can shift more to having a fun life. You can build up those crucial relationships with family and friends – and those people feel less burnout as caregivers. It adds a lot of support and resiliency.”

Dr. Forchuk adds that “our approach is to care for the whole person – mind, body and soul. It goes beyond managing the mental illness and is about supporting people in managing their life.”
The team already has four people enrolled in the study. In addition to people living alone, they will have participants with roommates and families to test the strategy under various real-life situations. The initial study will take place over one year.
This phase of project has received generous funding from the Canada Mortgage and Housing Corporation. The Canadian Institutes for Health Research contributed to the initial pilot phase.
Smart technology in the home effective for supporting mental health care, study finds
A research team from Lawson Health Research Institute has announced promising results from a one-of-a-kind demonstration study that evaluated the use of smart technologies in the home for people with severe mental illness.
“Our Smart Homes solution is for people who are having difficulty managing their everyday life and need a high level of care to maintain community living,” says Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson and project lead for Smart Home Community Model Phase.
“We have strong initial evidence showing that technology and applications embedded in the lived environment are safe, secure and appropriate for use in health care.”
After prototyping this approach within a hospital setting through St. Joseph’s Health Care London, the research team outfitted affordable housing units at Canadian Mental Health Association (CMHA) Elgin-Middlesex and London and Middlesex Community Housing (LMCH) with smart home technology.
The team presented the full study results during a virtual event.
There were 13 participants as part of this project phase who had different living situations such as individual apartments, group homes or family homes. Anxiety, mood and psychotic disorders were the most common mental health diagnoses, with many also suffering from chronic pain that make the activities of daily life difficult.

Each study participant selected from a wide range of tools that would best meet their individual needs, with all but one participant selecting more than one tool. Devices such as smartphones and touch-screen monitors connect with applications to provide video-conferencing, questionnaires, and prompts and reminders based on the person’s care plan. They also had access to automated medication dispensers and smart health monitoring devices for tracking heart rate, activity and sleep.
“All of the data is viewable by both the client and health care provider, allowing for more seamless care and identification of issues earlier on,” adds Dr. Forchuk.
The study found that visits to a health or social service provider and the emergency department decreased, as did home visits from a provider. Telephone appointments increased and communication between the client and provider were enhanced. Almost 80 per cent of the participants felt that the technologies improved their health care overall.
Higher levels of community integration and a greater sense of independence were also reported, including a better ability to remain connected with friends and family during the pandemic. When medication dispensers were used, no medication doses were missed. Participants felt they were better able to track their own health and more motivated to lead healthier lives.
“The compliment of smart technology in our Supportive Independent Living Program has proven to improve the quality of life of participants by reducing use of emergency services and fostering learning opportunities for independent living skills to create a good quality of life,” says Nedrita Shemshedini, Manager of Supportive Independent Living at CMHA Elgin-Middlesex. “In a large-scale rollout, this model could improve wellbeing and empower persons to better manage their care.”
The research team hopes this work will help inform the integration of smart technology more fully into mental health care delivery. Laura Pearson, Executive Director at Ontario Peer Development Initiative, urges that “there is a need for key policies to be addressed and changed in order to support funding and access for technology at a system level for the purpose of mental health care.”
The community model phase of the Smart Homes project was generously funded by the Canada Mortgage and Housing Corporation (CMHC).
Smart technology in the home effective for supporting mental health care, study finds
LONDON, ON – A research team from Lawson Health Research Institute has announced promising results from a one-of-a-kind demonstration study that evaluated the use of smart technologies in the home for people with severe mental illness.
“Our Smart Homes solution is for people who are having difficulty managing their everyday life and need a high level of care to maintain community living,” says Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson and project lead for Smart Home Community Model Phase. “We have strong initial evidence showing that technology and applications embedded in the lived environment are safe, secure and appropriate for use in health care.”
After prototyping this approach within a hospital setting through St. Joseph’s Health Care London, the research team outfitted affordable housing units at Canadian Mental Health Association (CMHA) Elgin-Middlesex and London and Middlesex Community Housing (LMCH) with smart home technology.
There were 13 participants as part of this project phase who had different living situations such as individual apartments, group homes or family homes. Anxiety, mood and psychotic disorders were the most common mental health diagnoses, with many also suffering from chronic pain that make the activities of daily life difficult.
“More and more, smart technologies like phone applications or virtual care are being used for mental health care. A smart home solution like the one we have tested could be considered a higher dose of technology, offered to clients with higher needs. The right dose for one may not work for another – the technological solutions used should vary depending on the individual,” explains Dr. Forchuk.
Each study participant selected from a wide range of tools that would best meet their individual needs, with all but one participant selecting more than one tool. Devices such as smartphones and touch-screen monitors connect with applications to provide video-conferencing, questionnaires, and prompts and reminders based on the person’s care plan. They also had access to automated medication dispensers and smart health monitoring devices for tracking heart rate, activity and sleep.
“All of the data is viewable by both the client and health care provider, allowing for more seamless care and identification of issues earlier on,” adds Dr. Forchuk.
The study found that visits to a health or social service provider and the emergency department decreased, as did home visits from a provider. Telephone appointments increased and communication between the client and provider were enhanced. Almost 80 per cent of the participants felt that the technologies improved their health care overall.
Higher levels of community integration and a greater sense of independence were also reported, including a better ability to remain connected with friends and family during the pandemic. When medication dispensers were used, no medication doses were missed. Participants felt they were better able to track their own health and more motivated to lead healthier lives.
“The compliment of smart technology in our Supportive Independent Living Program has proven to improve the quality of life of participants by reducing use of emergency services and fostering learning opportunities for independent living skills to create a good quality of life,” says Nedrita Shemshedini, Manager of Supportive Independent Living at CMHA Elgin-Middlesex. “In a large-scale rollout, this model could improve wellbeing and empower persons to better manage their care.”
The research team hopes this work will help inform the integration of smart technology more fully into mental health care delivery. Laura Pearson, Executive Director at Ontario Peer Development Initiative, urges that “there is a need for key policies to be addressed and changed in order to support funding and access for technology at a system level for the purpose of mental health care.”
The community model phase of the Smart Homes project was generously funded by the Canada Mortgage and Housing Corporation (CMHC).
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
St. Joseph’s launches Health Crisis Fund to support local COVID-19 research
LONDON, ON – St. Joseph’s Health Care London and Lawson Health Research Institute have announced plans to move forward with clinical trials testing a drug that could potentially be used to prevent and treat COVID-19. St. Joseph’s Health Care Foundation will accelerate the creation of the studies by providing seed funding to get the research started through donor support. Based on the immediate need, The St. Joseph’s Health Crisis Fund has been created by St. Joseph’s Health Care Foundation to enable these and other research studies currently in development through Lawson, the research arm of St. Joseph’s.
While supporting urgent COVID-19 clinical trials will be an immediate focus, The St. Joseph’s Health Crisis Fund will also support critical patient care equipment and care and comfort items for healthcare staff and volunteers working on the frontlines of the pandemic across St. Joseph’s.
The initial clinical trials aim to study the use of hydroxychloroquine as a preventative medication and treatment for COVID-19. Led locally by Dr. Michael Silverman, Medical Director of St. Joseph’s Infectious Diseases Care Program, one trial will assess the safety and efficacy of using the drug to prevent COVID-19 in health care workers recently exposed to the virus. This trial will also assess the drug as a treatment for non-hospitalized patients with mild cases of the illness. St. Joseph’s will be one of many participating sites in the trial, which is being led by the Research Institute of the McGill University Health Centre.
“There is much debate surrounding the drug hydroxychloroquine. We do not yet know whether it’s safe or effective, and it should not be routinely recommended until we do,” says Dr. Silverman, also a Lawson Associate Scientist and city-wide Chair/Chief of Infectious Diseases. “We plan to carefully study the drug through a randomized controlled trial and assess whether it can help combat COVID-19.”
Dr. Silverman is also partnering with Dr. Michael Borrie, Geriatrician at St. Joseph’s and Lawson Scientist, on a prevention trial to test the safety and efficacy of the drug for patients and residents at Parkwood Institute who have been exposed to COVID-19. They are at a higher risk of infection, as well as serious complications and potential admission to acute care.
“Lawson researchers like Drs. Silverman and Borrie excel in rapid response research,” says Dr. David Hill, Lawson Scientific Director. “Hospital-based research is uniquely positioned to handle these types of studies, as close proximity to patients and sample collection is essential.”
St. Joseph’s Infectious Diseases Program is the only program of its kind in the region. Dr. Silverman, head of St. Joseph’s Infectious Disease program, has worked with communities in crisis in Zambia, Zimbabwe, Uganda and the rainforests of Guyana. He is working closely with other health care partners in the London and surrounding area to coordinate the region’s response to the COVID-19 pandemic.
“The Sisters of St. Joseph, who founded our organization, faced contagious diseases and other pandemics at different times in our 150+ year history,” says Michelle Campbell. “Today, it’s a different time, and a new disease. Now, more than ever, we ask our community to help us address the crisis facing us all.”
Those interested in donating to St. Joseph’s Health Crisis Fund are asked to visit St. Joseph’s Health Care Foundation’s website to learn more at sjhcfoundation.org. Donations can be made online, through direct mail submissions or by calling the Foundation directly at 519-646-6085.
-30-
Renowned for compassionate care, St. Joseph’s Health Care London is a leading academic health care centre in Canada dedicated to helping people live to their fullest by minimizing the effects of injury, disease and disability through excellence in care, teaching and research. Through partnership with Lawson Health Research Institute and our collaborative engagement with other health care and academic partners, St. Joseph’s has become an international leader in the areas of: chronic disease management; medical imaging; specialized mental health care; rehabilitation and specialized geriatrics; and surgery. St. Joseph’s operates through a wide range of hospital, clinic and long-term and community-based settings, including: St. Joseph’s Hospital; Parkwood Institute; Mount Hope Centre for Long Term Care; and the Southwest Centre for Forensic Mental Health Care. www.sjhc.london.on.ca
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
St. Joseph’s Health Care Foundation gathers, grows and grants philanthropic funds to enable St. Joseph’s Health Care London to pursue excellence in care, teaching and research. Through donor support, the foundation contributes to advances in the delivery of patient care, specialized equipment, research initiatives and capital funds at St. Joseph’s Hospital, Parkwood Hospital, Mount Hope Centre for Long Term Care, Regional Mental Health Care London and Southwest Centre for Forensic Mental Health Care and Lawson Health Research Institute. As one of the largest charitable organizations in Southwestern Ontario, St. Joseph’s Health Care Foundation is an accredited member of Imagine Canada’s Ethical Trustmark Program, which recognizes the foundation’s commitment to ethical fundraising and donor accountability. www.sjhcfoundation.org
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca