Search
Search
Changing lives through innovation
It started like any other day. Paul Garrett could never have imagined that by the end of the day, he would be paralyzed from the waist down.
On May 25, 2019, Paul was making coffee before another day’s work as an appliance installer when he noticed a slight tingling in the toes of his right foot. Being fairly fit and in his early sixties, he didn’t think much of it – until the numbness got worse, moving up to the base of his spine and down the other leg. Within 30 minutes of the initial sensation, he lost all feeling and function in his legs.
Paul was rushed to the nearest emergency department. For some reason, he knew his life had changed forever. He assumed he was suffering from a stroke.
“Before the ambulance arrived, it was terrifying and emotional. I had this feeling I would never walk again.”
"... Nothing was working when I got to Parkwood Institute."
It wasn’t a stroke but Paul was right about the life-altering ramifications. After days of testing, he was diagnosed with acute onset transverse myelitis, a rare neuroimmune disorder where inflammation damages the insulating material (myelin) covering the nerves along the spine. Without this protective coating, signals from the brain to the spine and back cannot occur.
Paul came to St. Joseph’s Health Care London’s Spinal Cord Injury (SCI) Rehabilitation Program at Parkwood Institute, where his care team partnered with him and wife Brenda to develop a recovery plan.
“They started from scratch with me, nothing was working when I got to Parkwood Institute,” says Paul.
When occupational therapist Charlie Giurleo asked Paul and Brenda what their initial goals for rehabilitation were, they were quick to answer. Paul wanted to get to his son’s wedding, just a month away. The team, and
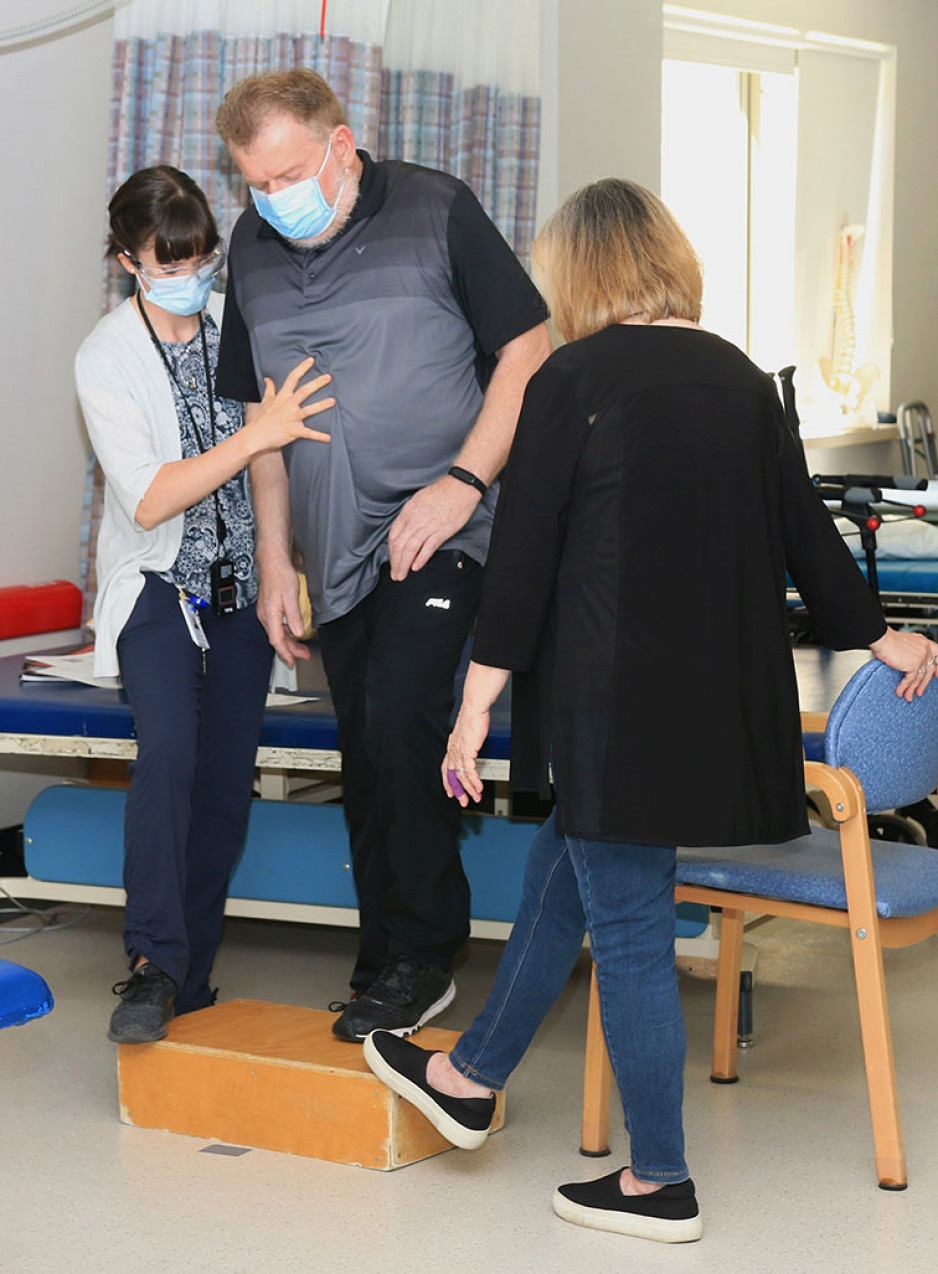
Paul, got to work, focusing treatments and exercises on learning how to get out of bed, transfer from the wheelchair to the car, and stand independently.
"... We were able to move on and adapt, thanks to the team..."
“I made it to the wedding, and I was even able to stand for a few pictures with my family. It was amazing.”
Then it was time to set longer term goals for his recovery and Paul knew exactly what he wanted, “I wanted to walk out of the building on my own.”
While the physical recovery was a significant hurdle for the Garretts, so was the emotional recovery.
“The SCI Rehabilitation Program team gave us wonderful support and information on how to live with a spinal cord injury,” says Brenda. “There was a lot of grief in the beginning for a life that was profoundly changed and would never be the same again, but we were able to move on and adapt thanks to the team at Parkwood Institute who were so positive and empowering.”
Emboldened by his care team, Paul was able to remain upbeat. Each time he met a new health care provider, he would tell them, ‘You’re on Team Paul now,’ as he held up his hand for a fist bump.”
Getting stronger
With the support of Team Paul, including his wife, a determined Paul worked on his walking one day at a time. “The team said to me, to go quicker is to go slower… to remain focused every day and get a little bit stronger.”
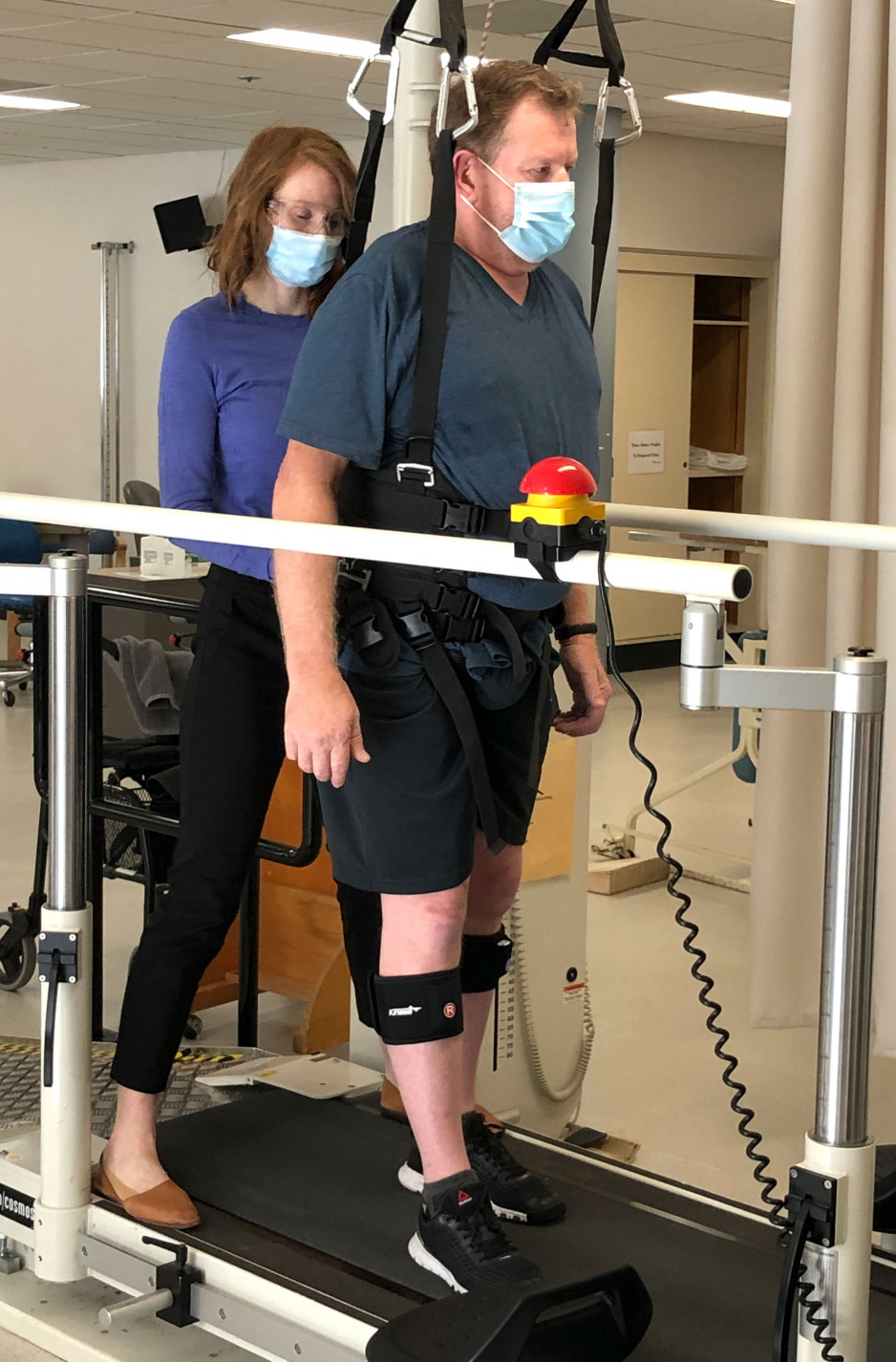
Paul was fortunate to have access to specialized rehabilitation equipment and expertise of members of St. Joseph’s Gray Centre for Mobility and Activity as part of his treatment.
“The equipment and the expertise in The Gray Centre were instrumental in Paul’s recovery.”
The Gray Centre is focused on expanding and advancing mobility and rehabilitation treatment and prevention solutions through research and collaborations between scientists and health care providers using the latest technology and innovations.
“Current patients of St. Joseph’s rehabilitation programs are already benefiting from The Gray Centre,” says physiotherapist Stephanie Cornell. Stephanie was a big part of Team Paul, supporting his rehabilitation plan and treatment.
“The equipment and the expertise in The Gray Centre were instrumental in Paul’s recovery,” says Stephanie. “Utilizing technology such as the body weight support treadmill, we were able to help Paul relearn a walking pattern and get back to being more active in his community.”
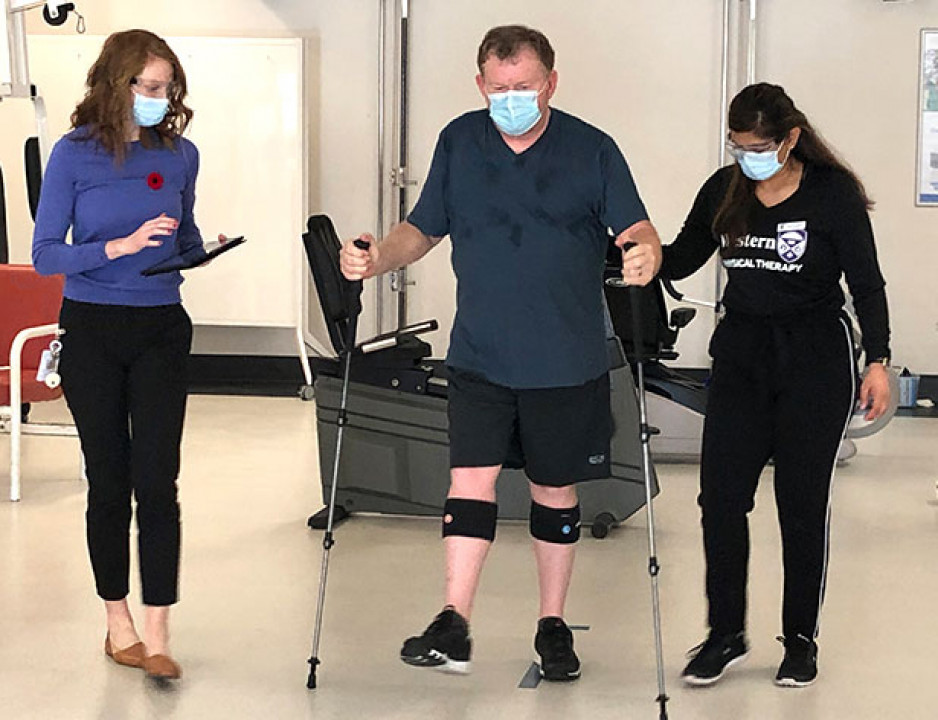
All of Paul’s hard work paid off. After his last rehabilitations session he met his goal and walked out of the building on his own. Members of Team Paul lined his pathway out to cheer him on and mark the momentous occasion.
Recipients of the Gray Centre 2022 Catalyst Grant Competition
The Gray Centre for Mobility and Activity recently completed the 2022 Catalyst Grant Competition. Catalyst grants are intended to provide seed funding to develop innovative research and clinical ideas and better position these projects to secure subsequent larger grants from external agencies. The Catalyst Grant Evaluation Committee reviewed several very strong proposals and selected four studies for funding:
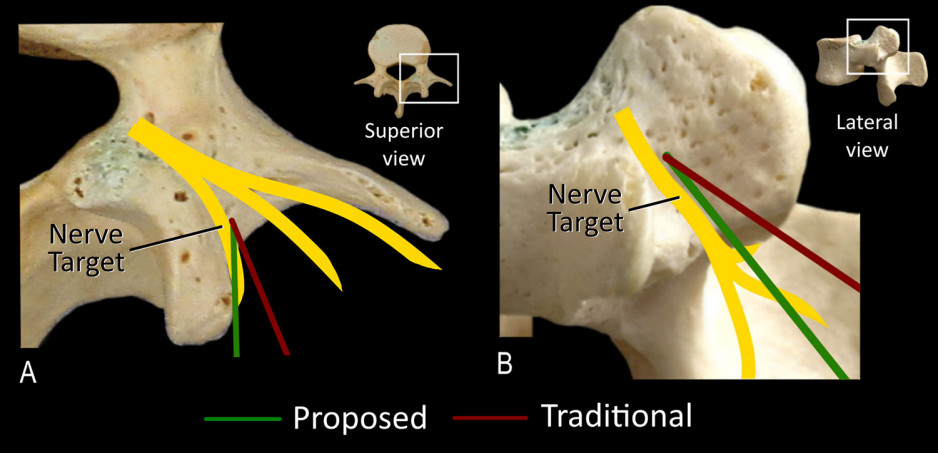
Evaluation of a novel technique for lumbar medial branch denervation to treat chronic mechanical low spinal pain originating from the facet joint:
Lead Investigator: Dr. Eldon Loh
A common treatment for chronic mechanical low back pain is to guide a small radiofrequency electrode towards specific joints in the spine and destroy the surrounding sensory nerves that are signaling pain to the brain. When successful there is substantial pain relief for the patient but the results are inconsistent, likely due to inaccurate site targeting of the electrode. In this work, Dr. Eldon Loh and his colleagues will first test in cadavers the safety and efficacy of a potentially more accurate method of guiding the electrode to these spinal joints. If successful, this method will then be used clinically in a small cohort of consenting patients to determine whether a larger randomized control trial testing this novel method should be conducted.
Pilot of an online, integrated behaviour change and physical activity program for those with neurological conditions:
Lead Co-Investigators: Swati Mehta PhD, Dalton Wolfe PhD
There is significant disparity in access to physical activity programs for people with mobility impairments, which greatly impacts mobility, function and long-term wellbeing. Swati Mehta, PhD, Dalton Wolfe, PhD, and their colleagues will test an online, group-based intervention consisting of exercise and behaviour activation strategies targeting these and other outcomes. Importantly, this programming will be applied to patient groups across several clinical programs at Parkwood Institute.
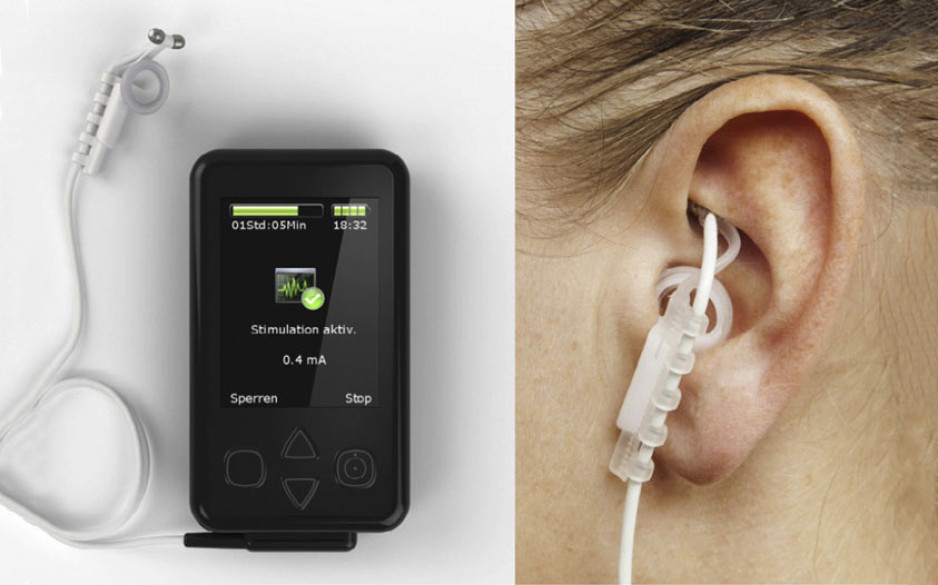
Study into the effect of transcutaneous vagus nerve stimulation on upper limb function in individuals with paralysis caused by spinal cord injury
Lead Co-Investigators: Drs. Keith Sequeira, Eldon Loh, and David Allison, PhD
The vagus nerve normally plays an important role in many of the body’s functions. Unfortunately, following spinal cord injury the activity of the vagus nerve is commonly reduced. Artificially stimulating the vagus nerve through a process known as vagus nerve stimulation (VNS) can help to increase the activity of this nerve and new evidence from animal models has shown that this treatment can improve physical recovery after spinal cord injury. For this study, Drs. Keith Sequeira, Eldon Loh, and David Allison, PhD, will test whether VNS in addition to traditional rehabilitation services lead to better mobility outcomes for patients with spinal cord injury compared to traditional rehabilitation services alone.
Evaluation of the perspectives of individuals with chronic neurological conditions regarding existing activity programs at Parkwood Institute:
Lead Investigator: Janelle Unger, PhD
One of the main goals of the Gray Centre is to expand the mobility and activity programming that Parkwood Institute offers to community members living with chronic conditions. A critical component to this expansion is evaluating existing programs to identify their strengths and challenges. In this work, Janelle Unger, PhD, and her colleagues will conduct a large series of interviews to explore the lived experiences of individuals participating in Parkwood Institute’s existing activity programs. The research team will then develop recommendations for how to best modify these current programs and optimally develop future program and service provisions.
The Gray Centre is excited to support these innovative projects. Congratulations to all the 2022 catalyst grant recipients.
Rehabilitation following lower limb loss
The fastest growing age group in Canada are those over 80 years old. This age demographic is most likely to have chronic medical conditions such as vascular disease and diabetes, which are also two of the primary causes for why individuals undergo lower limb amputation. Unfortunately, very little research focuses on the rehabilitation and long-term health outcomes of this oldest age cohort following this life changing procedure.
The Gray Centre’s Mobility Experts, Drs. Michael Payne, Ricardo Viana and Susan Hunter (PhD), along with their collaborators, Drs. Courtney Frengopoulos and Katherine Fuller, recently published an article in Prosthetics and Orthotics International, which synthesized all the existing scientific knowledge regarding prosthetic rehabilitation for those over 80 years old after lower limb amputation. Although much more research is needed, the research group found that this oldest age cohort can often perform normal activities of daily living and be discharged to home following a rehabilitation program but may need support from a caregiver or family member. Dr. Frengopoulos explains the full scope of their findings in the video below.
Ali Bateman
Ali Bateman, MD
Assistant Professor, Schulich School of Medicine and Dentistry
Acquired and Traumatic Brain Injury; Spinal Cord Injury
Dr. Ali Bateman is a physiatrist at Parkwood Institute and an Assistant Professor in the Department of Physical Medicine and Rehabilitation Schulich School of Medicine & Dentistry at Western University. She is also an Associate Scientist at Lawson Health Research Institute, and the Quality Improvement Lead in the Department of Physical Medicine & Rehabilitation.
Dr. Bateman completed her medical degree and residency training at Western University, and is currently completing a master’s degree in Quality Improvement and Patient Safety through the Institute of Health Policy, Management, and Evaluation at the University of Toronto. She is also certified by the Canadian Society of Clinical Neurophysiologists and holds the designation of CSCN Diplomate (EMG). As a consultant physiatrist, Dr. Bateman provides care in acquired brain injury and spinal cord injury rehabilitation programs and the electrodiagnostic laboratory at Parkwood Institute.
Her research interests centre on quality improvement, patient safety, and knowledge translation with the aim of achieving best practices so that all persons with spinal cord and/or brain injury receive the best quality care.

Caitlin Cassidy
Caitlin Cassidy, MD
Assistant Professor, Schulich School of Medicine and Dentistry
Childhood Onset Conditions; Implementation Science and Education
Dr. Caitlin Cassidy is a physiatrist at Parkwood Institute and an Associate Professor in the Department of Physical Medicine and Rehabilitation, and is also cross appointed to the Department of Paediatrics. Her primary clinical and research roles revolve around the Transitional and Lifelong Care (TLC) program at Parkwood Institute. The TLC program provides longitudinal rehabilitative care to adolescents and adults living with a physical disability of childhood onset, many of whom experience mobility challenges and may struggle to find accessible opportunities to increase their fitness and activity levels.
Dr. Cassidy’s research interests include the natural history and long-term outcomes of people with these conditions, and collaborates closely with Dr. Laura Brunton from the School of Physical Therapy at Western University to determine the impacts that access to activity and wellness programming have on pain, fatigue and other outcomes for people with cerebral palsy and spina bifida. Dr. Cassidy also acts as the discipline lead for Musculoskeletal Medicine in undergraduate medical education at Schulich School of Medicine & Dentistry at Western University.

Dalton L. Wolfe
Dalton L. Wolfe, PhD
Lawson Scientist, Parkwood Institute Research
Implementation Science and Education; Spinal Cord Injury
Dalton Wolfe is a Scientist at Lawson Health Research Institute, an Assistant Professor in the Faculty of Health Science and leads the Research 2 Practice (R2P) team, which is a unique research program within Parkwood Institute that focuses on strategies for generating evidence and implementing best practice within rehabilitation. Professor Wolfe’s primary research interest is in the area of knowledge mobilization and best practice implementation with a focus on physical activity and activity-based therapies in spinal cord injury and brain injury rehabilitation.
Professor Wolf also co-leads the Ontario SCI Implementation, Evaluation and Quality Care Consortium, which focuses on implementation of quality indicators towards the enhancement of care across the 5 academic health centres involved in SCI rehabilitation in Ontario. As part of the Parkwood Rehabilitation Innovations in Mobility Enhancement initiative (PRIME), Professor Wolfe is focused on enhancing clinical decision-making to improve locomotor and other movement-related outcomes with activity-based therapies such as robotic, manual and FES-assisted therapies. As with many of the R2P initiatives this involves implementation science and participatory research methods to put in place practice-based research infrastructure that enables iterative knowledge generation as well as implementation. Trainees work alongside clinicians, administrators and persons with lived experience to tackle clinically relevant questions.

Eldon Loh
Eldon Loh , MD
Associate Professor, Schulich School of Medicine and Dentistry
Chronic Pain
Dr. Eldon Loh is a Physiatrist at Parkwood Institute and an Associate Professor in the Department of Physical Medicine and Rehabilitation at the Schulich School of Medicine and Dentistry at Western University. He completed residency training in Physical Medicine and Rehabilitation at the University of Alberta in 2010 and a clinical fellowship in interventional pain management in 2011. His research interests include improving the management of chronic neuropathic pain after spinal cord injury, and the development of novel and improved techniques for interventional pain management of axial spine pain.
He is Chair of the panel that developed and updates the Canadian Best Practice Guidelines for Neuropathic Pain after spinal cord injury and works with international partners to improve point-of-care tools for implementing the guidelines. His interventional pain research focuses heavily on a bench to bedside approach, utilizing anatomical findings to inform clinical practice. He has also examined the impact of Ontario’s healthcare utilization of different interventional procedures such as radiofrequency ablation and paravertebral nerve blocks.

Heather MacKenzie
Heather MacKenzie, MD; MSc
Assistant Professor, Schulich School of Medicine and Dentistry
Acquired and Traumatic Brain Injury
Dr. Heather MacKenzie is a physiatrist at Parkwood Institute and an Assistant Professor in the Department of Physical Medicine and Rehabilitation in the Schulich School of Medicine and Dentistry at Western University. She completed her residency training in Physical Medicine and Rehabilitation at Western University and subsequently earned a Master’s of Science degree in Epidemiology at the Harvard T. H. Chan School of Public Health.
Her research program focuses on predicting outcomes after concussion/mild traumatic brain injury (mTBI). Although concussions/mTBIs are common and the majority of symptoms resolve within three months, a significant proportion of individuals remain symptomatic beyond one year. These persistent symptoms result in mobility challenges and reduced participation in instrumental activities of daily living as well as vocational and leisure activities. Dr. MacKenzie’s current research focuses on identifying patients that are at high-risk for developing persistent symptoms from concussion/mTBI so that interventions can be prioritized and rehabilitation services can be quickly mobilized. Early intervention for those expected to have a prolonged recovery has the potential to alter their trajectory and optimize their potential for a positive outcome and may also reduce the occurrence of persistent symptoms and decrease secondary disability related to their injury.

Jamie Fleet
Jamie Fleet, MD
Assistant Professor, Schulich School of Medicine and Dentistry
Stroke
Dr. Jamie Fleet is a physiatrist at Parkwood Institute and an Assistant Professor in the Department of Physical Medicine and Rehabilitation at the Schulich School of Medicine and Dentistry at Western University. Dr. Fleet completed medical school as well as residency training in Physical Medicine and Rehabilitation at McMaster University. She is currently enrolled in a Master’s program in Clinical Epidemiology through the Health Research Methodology program at McMaster University with a focus on fracture treatment and prevention in older patients after stroke. Her primary clinical area of focus is in stroke rehabilitation.
Though still early in her career, Dr. Fleet has developed a strong research background, primarily focusing on drug safety studies in older adults using large data through ICES. Her other research interests include exercise and health promotion/prevention strategies in patients after stroke, as well as fall prevention strategies and pain management. "

Janelle Unger
Janelle Unger, PT; PhD
Assistant Professor, Faculty of Health Science
Stroke, Spinal Cord Injury
Janelle Unger is an Assistant Professor in the School of Physical Therapy at Western University and a registered physiotherapist. Professor Unger's research focus is on optimizing recovery following neurological injury. She investigates the effectiveness of novel interventions to improve gait and balance with kinetic, kinematic, and clinical outcomes. Professor Unger is also interested in evaluating service delivery and community programs for individuals with chronic injuries as well as understanding the lived experiences of people with neurological conditions using qualitative data. Her goal is to create a program that will focus on enhancing lifelong mobility and participation in physical activity for people with chronic neurological conditions.

Jaspreet Bhangu
Jaspreet Bhangu, MD, PhD
Assistant Professor, Schulich School of Medicine and Dentistry
Balance, Gait and Falls
Dr. Jaspreet Bhangu, is a geriatrician at Parkwood Institute and an Assistant Professor within the Division of Geriatric Medicine in the Schulich School of Medicine and Dentistry at Western University. He graduated from the Royal College of Surgeons, Ireland in 2004. He completed his specialist training in Internal and Geriatric Medicine in Ireland in 2016. He completed a PhD in Medical Gerontology with Trinity College Dublin in 2017 studying falls and syncope in older adults and then completed a clinical fellowship with the University of Toronto. He also holds a Master’s degree in Bioethics and Health. He has extensive experience in human intervention research and his research interests include cardiac causes of falls, orthostatic hypotension and autonomic dysfunction, vascular contributions to cognitive decline and digital medicine.

Jenny Thain
Jenny Thain, MD
Assistant Professor, Schulich School of Medicine and Dentistry
Balance, Gait and Falls; Implementation Science and Education
Dr. Jenny Thain is a geriatrician at Parkwood Institute and an Assistant Professor within the Division of Geriatric Medicine at the Schulich School of Medicine and Dentistry at Western University. Dr. Thain completed a Master’s degree in Health Professions Education through the University of Maastricht and completed her medical training at the University of Nottingham, sub-specializing in orthogeriatric medicine.
Her areas of clinical interest include osteoporosis and bone health, with a particular interest in orthogeriatric care. She is the Chair of the Canadian Geriatrics Society Osteoporosis and Bone Health Special Interest Group, a member of the Osteoporosis Canada Scientific Advisory Council and Fragility Fracture Network Scientific Committee and the Geriatric clinical lead of the Hip Fracture Unit at Victoria Hospital, London.

Keith Sequeira
Keith Sequeira, MD
Associate Professor, Schulich School of Medicine and Dentistry
Implementation Science and Education
Dr. Keith Sequeira is a physiatrist at St. Joseph's Health Care London and London Health Sciences Centre and an associate professor in the Department of Physical Medicine and Rehabilitation in the Schulich School of Medicine and Dentistry at Western University. Dr. Sequeira completed his medical degree at the University of Toronto in 1994, residency training in Physical Medicine and Rehabilitation at Albany Medical Center in 1998, followed by a fellowship in Electrodiagnostic and Sports Medicine at Michigan State University.
Dr. Sequeira is the Medical Director of the Acquired Brain Injury Rehabilitation Program at Parkwood Institute and runs spasticity, EMG, brain and spinal cord injury clinics. Dr. Sequeira is the past Residency Program Director of Physical Medicine & Rehabilitation at Western, a program that he designed and initiated in 2005 and functions. He is the WSIB Champion, working on the integration of WSIB education into the medical school curriculum at Western, past director of the undergraduate the musculoskeletal curriculum within the medical school at Western, the recipient of the Dean’s Award of Excellence for Undergraduate Medical Education, and has authored numerous publications, including a 2020 article in the New England Journal of Medicine on lumbar radiculopathy.

Laura Brunton
Laura Brunton, PT, PhD
Assistant Professor, School of Physical Therapy
Childhood Onset Conditions
Laura Brunton is an Assistant Professor in the School of Physical Therapy at Western University and is a registered Physiotherapist. Professor Brunton's current research focus is exploring and understanding fatigue and pain experienced by individuals with cerebral palsy and the possible relationships with physical activity, sleep, pain and mental health. Professor Brunton has an interest in developing novel approaches to increase and support the self-management skills for youth and adults with childhood-onset conditions. A secondary interest of Professor Brunton’s is the development and validation of clinical measures to support comprehensive assessment of clients in clinical practice.

Laura Graham
Laura Graham, PT, PhD
Assistant Professor, School of Physical Therapy
Neurological injury, mild traumatic brain injury
Laura Graham is an Assistant Professor and Graduate Chair of Western University’s Master of Physical Therapy Program, and an Associate Scientist with Lawson Health Research Institute. Professor Graham’s teaching focus is neurological injury/illness rehabilitation and her research interests revolve around the development of interventions for adults with persistent symptoms following concussion or other mild traumatic brain injuries (mTBI).
Professor Graham has worked as a physiotherapist at Parkwood Institute since 2011, primarily in adult brain injury rehabilitation. She has consulted with Ontario Brain Institute and WSIB Ontario on mTBI Program of Care revision, presented education of the treatment of mTBI both locally and internationally, and has taught physiotherapist instructors across Canada about concussion/mTBI rehabilitation for the National Orthopaedic Division of the Canadian Physiotherapy Association.
Professor Graham is currently helping to develop and evaluate two interventions for adults with mTBI. The first is BrainEx90, which is a circuit training-style therapy that covers self-management exercises, vision rehabilitation, vestibular rehabilitation, balance and core stability, cardiovascular training, and cognitive rehabilitation. nd the second is MyBrainPacer™ App, which is a symptom self-management tool to support people with mTBI through planning and pacing activities.

Manuel Montero-Odasso
Manuel Montero-Odasso, MD; PhD
Professor, Schulich School of Medicine and Dentistry
Mobility, Cognitive and Brain Health
Dr. Manuel Montero-Odasso is a geriatrician at Parkwood Institute and Professor and Faculty Scholar in the Schulich School of Medicine and Dentistry at Western University. He is also the Director of the Gait & Brain Lab at Parkwood Institute, a clinician-scientist at the Lawson Health Research Institute and serves as team leader at the Canadian Consortium on Neurodegeneration in Aging and the Ontario Neurodegenerative Research Initiative.
Dr. Montero-Odasso leads the Gait and Brain Health Program goal of understanding mechanisms and treatments of mobility and cognitive decline in aging by focusing on the interaction between gait performance and cognition and how this increases the risk of falls. Through this work Dr. Montero-Odasso has established the use of “motor biomarkers”, like slowing of gait speed and dual-task effects on gait to predict frailty, falls, and dementia. He is also a co-PI of the Canadian Therapeutic Platform for Multidomain Interventions to Prevent Dementia, which focuses on multi-domain lifestyle interventions that include physical exercises, cognitive training, diet, self-management of cardiovascular factors and sleep, in order to reduce the risk or delay the onset of dementia in older adults.
Dr. Montero-Odasso has received more than $6 million of competitive peer-reviewed research funding, has published over 150 scientific articles, 14 books and book chapters, and has received several accolades, including the American Geriatrics Society New Investigator Award, the Schulich Clinician Scientist Award, the Premier of Ontario Excellence Research Award, and the CIHR New Investigator Award. In 2019, he was inducted as one of the Top 10 Hispanic Canadian for his contribution in Medicine and Science. He has been invited to give more than 100 international presentations as a guest speaker. He serves as associate editor for the Journal of Gerontology Medical Sciences, Geriatrics, and Journal of Alzheimer’s Disease, among others. He also serves as executive member and Vice-President of the Canadian Geriatrics Society.

Michael Payne
Michael Payne, MD
Assistant Professor, Schulich School of Medicine and Dentistry
Amputation
Dr. Michael Payne is a physiatrist at Parkwood Institute and an Associate Professor in the Department of Physical Medicine and Rehabilitation at the Schulich School of Medicine & Dentistry at Western University. He completed his undergraduate degree in Mechanical Engineering at Queens University followed by a Master’s degree in Sports Medicine and a medical degree at Western University, residency training in Physiatry at the University of Ottawa, and then a clinical fellowship in Australia.
Dr. Payne’s clinical practice has always focused on addressing mobility limitations across a wide range of physical impairments and has been the medical director of the Regional Amputee Rehabilitation program at St. Joseph’s Health Care London since 2009. Dr. Payne collaborates extensively with Dr. Susan Hunter from the School of Physical Therapy from Western University to address research questions centred around improving meaningful outcomes for people with limb loss or deficiencies. Specific interests include mobility outcome measurements, dysvascular amputation associated cognitive impairment, biomechanics, quality of life, gait abnormalities and falls.

Ricardo Viana
Ricardo Viana, MD, OT
Associate Professor, Schulich School of Medicine and Dentistry
Amputation; Stroke
Dr. Ricardo Viana is a physiatrist at Parkwood Institute and an Associate Professor in the Schulich School of Medicine and Dentistry at Western University. Prior to studying medicine, Dr. Viana was an cccupational therapist. Dr. Viana completed his medical training in 2008 and his Physical Medicine and Rehabilitation residency training in 2013. Dr. Viana’s clinical focus is on Stroke and Amputee rehabilitation as well as neuromuscular and pain medicine.
Dr. Viana has two primary research interests. First, is understanding the impact of dual-task performance on mobility, balance and falls for those with amputation. And second, is systematic reviews in support of the Evidence Based Review Stroke Rehabilitation. Dr. Viana also has a growing interest in education, both medical education and knowledge translation in the clinical setting.

Robert Teasell
Robert Teasell, MD
Professor, Schulich School of Medicine and Dentistry
Stroke
Dr. Robert Teasell is a physiatrist at Parkwood Institute, a Professor in the Schulich School of Medicine and Dentistry at Western University, former Chair-Chief and current Research Director of the Department of Physical Medicine and Rehabilitation. He is a Clinical Researcher with Lawson Health Research Institute, Parkwood Institute Research and Director of the CORRE Research Group. Dr. Teasell has authored over 800 publications including over 350 peer-reviewed articles and has been involved with $24 million of research funding. He has won over 50 awards including Lawson Scientist of the Year, and Post-Acute Stroke Excellence Award, both in 2018, American Congress of Rehabilitation Medicine and National Stroke Association in the United States.
Dr. Teasell has supervised many graduate students and since 2014, three research team members have won the Lawson Leadership Impact Award (best graduate student at Lawson Institute) and three have become Vanier Scholars. Research interests include the Clinical Application of Best Evidence in Neurorehabilitation. Projects include: Stroke Rehabilitation Evidence-Based Review, Acquired Brain Injury Evidence-Based Review and Spinal Cord Injury Evidence-Based. The details of all projects within the CORRE Research Group can be found on the lab website.

Siobhan Schabrun
Siobhan Schabrun, PhD
Professor, School of Physical Therapy
Chronic Pain
Siobhan Schabrun is the incoming William and Lynne Gray Endowed Research Chair in Mobility and Activity and Professor in the School of Physical Therapy. Her research program is focused on understanding, treating and preventing persistent pain – a major cause of reduced mobility and activity amongst otherwise healthy individuals and those living with musculoskeletal and neurological conditions. In addition, Professor Schabrun explores the use of non-invasive brain stimulation technologies to boost neuroplasticity and improve outcomes following traditional forms of rehabilitation such as exercise, functional electrical stimulation and virtual reality training. Professor Schabrun is passionate about improving the translation of research evidence into practice and about promoting the participation of women and girls in science.