Search
Search
‘Brain training’ may be an effective treatment for post-traumatic stress disorder, clinical trial finds
Neurofeedback, also called ‘brain training,’ consists of exercises where individuals regulate their own brain activity. In a new study from Lawson Health Research Institute and Western University, researchers have found that neurofeedback may be an effective treatment for individuals with post-traumatic stress disorder (PTSD). Published in NeuroImage: Clinical, the clinical trial found that neurofeedback was effective in reducing symptoms of PTSD.

Neurofeedback uses a system called a neurofeedback loop in which a person’s brain activity is measured through sensors placed on the scalp and displayed back to them using a computer interface. This allows the individual to complete exercises and visually see the results.
The trial tested neurofeedback with a total of 72 participants, including 36 participants with PTSD and 36 healthy control participants. Of those with PTSD, 18 were randomized to participate in neurofeedback treatment while the other 18 acted as a comparison group.
The study found that the severity of PTSD symptoms decreased in participants randomized to receive neurofeedback treatment. After treatment, 61.1 per cent of participants no longer met the definition for PTSD. This remission rate is comparable to gold standard therapies like trauma-focused psychotherapy.
The research team also used functional magnetic resonance imaging (fMRI) at St. Joseph’s Health Care London to capture brain scans of participants both before and after participation in the trial. They found that individuals with PTSD experienced positive changes in brain connectivity in the salience network and the default mode network following neurofeedback treatment.

The study involved weekly sessions of neurofeedback over 20 weeks. Participants were asked to reduce the intensity of the brain’s dominant brain wave – the alpha rhythm. Brain activity was visualized as either a still cartoon or a distorted picture. If the alpha rhythm was successfully reduced, the cartoon started moving or the picture started becoming clearer.
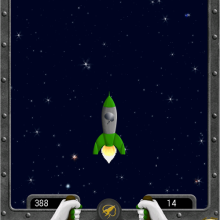
“Participants were not instructed on how to reduce the alpha rhythm. Rather, each individual figured out their own way to do so,” notes Dr. Lanius. “For example, individuals reported letting their mind wander, thinking about positive things or concentrating their attention.”
The team notes the treatment could have a number of clinical implications following further validation.
“Neurofeedback could offer an accessible and effective treatment option for individuals with PTSD,” says Dr. Lanius. “The treatment is easily scalable for implementation in rural areas and even at home.”
Read more about neurofeedback and the team's research:
$65.75M grant positions Lawson as Canadian leader in workplace-injury research
Massive investment by the Workplace Safety and Insurance Board (WSIB) to St. Joseph’s Health Care London is largest-ever grant to transform occupational illness and injury
A “game-changer” investment of $65.75 million to Lawson Research Institute of St. Joseph’s Health Care London will transform the prevention, diagnosis and treatment of workplace injuries and illness for Ontarians.
The Workplace Safety and Insurance Board’s visionary 10-year commitment is the WSIB's largest-ever research injection; the largest non-government health research funding in London history; and the biggest single grant received and stewarded by St. Joseph’s Health Care Foundation.
The investment will launch the Occupational Injury Prevention and Treatment Research Network – a first-in-Canada hub where people, technology and science-backed innovation will help solve the human and health costs of occupational injury and illness across Ontario and around the world.
Landmark work, global leadership
“This is a game-changer, something that will transform how we work together to get ahead of work-related injury, pain and mental illness,” says Lisa Porter, PhD, Vice-President Research at St. Joseph’s and Scientific director of Lawson, the research arm of St. Joseph's.
“This investment will propel us to global leadership in finding solutions to some of the most pervasive issues affecting people in workplaces today,” Porter says.
Occupational injuries and illnesses – including chronic pain, physical disability and mental health conditions – accounted for more than 93,000 claims registered through the WSIB last year, with an average lost work time of 63.2 days.
Occupational injuries and illnesses – including chronic pain, physical disability and mental health conditions – have a significant impact on many people, families and businesses in Ontario. Every year they account for almost 250,000 claims registered through the WSIB, with benefit payments of approx. $2.5 billion.
“Too many Ontario families experience the human cost of workplace injury,” says Jeffery Lang, President and CEO of the WSIB. “We want fewer injuries to happen, and if they do, to be able to help people with a safe and faster recovery. This research is going to help get us there and with their established expertise, the St. Joseph’s Health Care and Lawson Research Institute team are a natural partner for this important work.”
Investment and innovation
The network will innovate long-term solutions to prevent mental and physical injuries, accelerate recovery and ensure sustainable health for Ontario workers.
It will feature state-of-the-art infrastructure and expertise including:
- A first-in-Canada positron emission tomography/magnetic resonance imagery (PET/MRI) scanner dedicated to research into rapid and accurate diagnosis of mental health conditions including post-traumatic stress and depression
- A cutting-edge Computer-Assisted Rehabilitation Environment (CAREN), a unique, virtual-reality environment that will test and solve workplace injury, rehabilitation and chronic pain in new ways
- Three new endowed research Chairs and teams of scientists solving the most critical research questions plaguing people injured at work, an investment that will ensure long-term consistency and sustainability of the work
- Deploying technology in data science, artificial intelligence (AI) and virtual reality, making the network accessible by centres and workplaces across Canada
Rapid-access research area to design and test assistive devices such as splints and mobility technology
St. Joseph’s President and CEO Roy Butler says, “We know that discovery-driven, patient-focused research improves lives – that is the focus of our hospital-based research at Lawson, and we’re humbled that the WSIB has entrusted us to expand this vital work to minimize the effects of workplace injury, disease and disability. This significant investment will drive innovation opportunities that will translate into novel new treatments and tools that can be used to battle workplace injury and illness”
“This investment will enable us to leverage the deep expertise St. Joseph’s already has in mental health, chronic pain and rehabilitation, and creates the opportunity to expand our knowledge to support workplace wellness, including for frontline health-care workers,” Butler says.
Butler adds that the network will strengthen existing partnerships and create new collaborations – within St. Joseph’s as well as among a wide range of health professionals, researchers, post-secondary institutions and industry locally, across the province and nationally.
Butler notes St. Joseph’s already excels in research and treatment for related injuries and illnesses.
That includes: preventing and treating chronic pain through the hospital’s Pain Management Program and the Gray Centre for Mobility and Activity hand and upper limb care and injury prevention through the Roth | McFarlane Hand and Upper Limb Centre; advanced imaging expertise; and mental health solutions for veterans and first responders at the MacDonald-Franklin OSI Research Centre. All are specialty research areas of St. Joseph’s with deep roots in addressing occupational injury and illness.
A partnership of promise
Many groundbreaking research initiatives at St. Joseph’s have been made possible by generous supporters of St. Joseph’s, says Michelle Campbell, President and CEO of St. Joseph’s Health Care Foundation.
Medical research in Canada, including the research done in our hospitals, relies heavily on private funding. Donors to our foundation, invest in research because they know that innovation leads to better frontline care, and healthier communities,” Campbell says.
“It’s a partnership of promise, a confident stride toward better outcomes for patients. The WSIB’s gift through St. Joseph’s Health Care Foundation is a whole new level of leadership, and we’re proud to be integral to this transformation in workplace health,” says Campbell.
Earlier this year, the WSIB announced a $20-million gift to Fanshawe College to create a Centre of Excellence in Immersive Technology for Workplace Safety, primarily to help first responders and responders-in-training learn to prevent and treat occupation-related mental health issues such as PTSD, anxiety and depression.
The Network at St. Joseph’s broadens that work to bring research-specific innovation aimed at benefiting the physical and mental wellbeing and safety of workers in all occupations.
The new hub at St. Joseph's will make use of the institution’s vast community and research partnerships throughout London and across Canada, in multiple collaborations across a wide range of health disciplines.
2017 SRF Spotlight: Drs. Muriel Brackstone & Gregor Reid
Announced at the 2017 Lawson Impact Awards, Drs. Muriel Brackstone and Gregor Reid were recipients of Lawson’s annual Strategic Research Fund (SRF) competition. Their project, “Re-setting the breast microbiome to lower inflammation and risk of cancer,” will examine whether taking an oral probiotic can reduce inflammation and lower the risk of breast cancer.
One in nine Canadian women will develop breast cancer during her lifetime (Canadian Breast Cancer Foundation). Many cancers are considered to be the result of inflammatory processes. While inflammation has been a focus of research in breast cancer, the role of bacteria has not.
Recently, Drs. Reid and Brackstone were collaborators on a study that was the first to describe the breast microbiome, proving the existence of bacteria in human breast tissue. Led by Dr. Reid and his former PhD student, Dr. Camilla Urbaniak, further research demonstrated that the types of bacteria found in women with breast cancer differ significantly from those found in healthy tissue.
One bacterial species from the cancerous tissue, Escherichia coli (E. coli), is capable of producing low amounts of substances known to cause cancer and induce inflammation, while the bacteria found in healthy tissue, like Lactobacillus, are known to interfere with cancer processes.
“The question is whether we can manipulate this to essentially get rid of more harmful bacteria and replace them with beneficial ones like Lactobacillus,” says Dr. Reid, a Lawson scientist and Director of the Canadian Centre for Human Microbiome and Probiotic Research.
In this new study, Dr. Brackstone and Dr. Reid will join forces to test their theory that taking an oral probiotic lactobacilli will lead to these organisms reaching the breast tissue, displacing harmful bacteria and reducing inflammation.
Drs. Brackstone and Reid will compare bacteria from the breast tissues of women at risk for breast cancer who are taking the probiotic against those at risk who are taking a placebo. They will also compare to the breast tissue of healthy women who are not at risk. The research participants will provide nipple and needle aspirates for their bacteria to be analyzed both at the beginning of the study and after three months of either taking the probiotic or a placebo. The samples will also be tested for inflammatory compounds, levels of heavy metals and pesticides that may influence cancer risk.
“I think this study will shed light into what actually occurs in the milk ducts where most breast cancers originate,” says Dr. Brackstone, a Lawson scientist, surgical oncologist and medical director for the London Breast Care Clinic. “If successful, this project could lead to larger studies and contribute to a new way of approaching breast cancer management.”
Now in its third year, Lawson’s Strategic Research Fund (SRF) supports research projects that will advance science in alignment with Lawson’s strategic research goals, as outlined in Lawson’s 2014-2018 Strategic Plan. This year’s competition once again focused on “inflammation”. Chosen projects received $50,000 over a two-year period.
Learn more about this research project:
2018 Staff Award of Excellence: Sarah Best
Sarah Best, research manager at Lawson Health Research Institute, was a recipient of this year’s Staff Award of Excellence, presented at the 2018 Lawson Impact Awards. The award was created to honour the contributions of dynamic, hardworking staff members who help advance science at Lawson.
Best is a part of the Cognitive Clinical Research Group at St. Joseph’s Heath Care London’s Parkwood Institute. In addition to managing the research group’s staff and trainees, she has a wide range of responsibilities, including developing strategies for recruitment and retention of clinical trial participants, budgeting, assisting with grant applications, and ensuring the team has the appropriate space, hardware and training to complete their research.
“Sarah has grown a team of skilled, well-trained staff and her leadership has ultimately resulted in an increase in the volume and complexity of trials we can offer for patients with mild cognitive impairment and Alzheimer’s disease,” says Dr. Michael Borrie, Lawson researcher and medical director of the Cognitive Clinical Research Group.
Best is also the budget officer for the Consortium of Canadian Centres for Clinical Cognitive Research and a member of the platform implementation team for the Canadian Consortium on Neurodegeneration and Aging (CCNA). The CCNA was formed by more than 350 clinicians and researchers throughout Canada to accelerate progress in age-related neurodegenerative disease research.
The Comprehensive Assessment of Neurodegeneration and Dementia (COMPASS-ND) Study is a CCNA study collecting clinical, neuropsychological, and MRI imaging data as well as blood, saliva, and urine samples from participants to learn about who is at risk of developing dementia, to determine how early dementia can be detected and to find out what tests are most effective at detecting dementia. Best has helped facilitate the study start-up and patient recruitment for the more than 30 sites involved in COMPASS-ND, including Parkwood Institute.
“Working in the field of neurodegeneration is really important right now as we see the numbers of individuals that have cognitive impairment growing exponentially. Currently, we only have symptomatic treatments so we’re really looking to find that breakthrough that will lead to a disease-modifying treatment to better serve patients and actually change the course of their disease,” says Best.
She adds, “I’m really honoured to receive this award, especially knowing the previous recipients and the impact that they've had on the London research community.”
A “safety net of relationships” to bridge the gap between hospital and community at discharge
A beneficial and cost-effective approach to mental health care that supports people as they go from hospital and back into the community is outlined in a new resource and has been recognized internationally by the World Health Organization (WHO).
"The immediate period after discharge from hospital, usually the first month, can be one of the most vulnerable times in the life of someone experiencing a mental illness. It can be when they are most at risk of committing suicide,” explains Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson Health Research Institute. “However, what we’ve seen is that there’s often a gap between when someone says ‘goodbye’ to the hospital inpatient unit and ‘hello’ to the community care provider.”
During a virtual book launch, a research team from Lawson and several community organizations discussed details of a new publication from Routledge, From Therapeutic Relationships to Transitional Care: A Theoretical and Practical Roadmap, edited by Dr. Forchuk. The book combines theory, research and best practices into a “roadmap” for organizations and others worldwide coordinating services or studying mental health care systems. It includes a practical toolkit for implementing the Transitional Discharge Model (TDM), developed and tested in communities across Ontario.
Purchase your copy of the book HERE and enter promo code SMAO3 at checkout for a 20% discount.

How Transitional Discharge works
TDM was born from a participatory action project with consumers of mental health services. They identified two factors that were most important to them when they were going from hospital to the community: consistency in therapeutic relationships and a supportive peer friendship.
It became known as a “safety net of relationships” that would bridge the gap between hospital and community services.
As a person-centred, evidence-based model, transitional discharge supports a smooth adjustment from hospital to community in two main ways:
- The inpatient staff continue to care for discharged clients until therapeutic relationships are established with community care providers.
- A friendship model of support with trained peer support workers who have lived experience of mental illness as they have made the same journey.

Perspective of a TDM client and peer support coach
Lance Dingman was a TDM client during the early phases of the project. “It makes a big difference when you’re able to get back to living in the community and in your own dwelling. You get to make more of your own decisions and learn about what you want to do. You grow with your experience and the guidance of others who are there to support you.”
Later becoming a peer support coach, Dingman feels implementing TDM for mental health care is important because people can learn from each other and get healthier in the process. “As a peer support worker, I sit with people and they tell me their story. It takes me back and I know what they are going through – I was where they are. I can share my own story and tell them what I did to get better.”
Cost-analysis and savings for the system
Dr. Forchuk’s team analyzed the cost of TDM after being tested in nine hospitals across Ontario, including London Health Sciences Centre and St. Joseph’s Health Care London.
- On average, the length of stay in hospital was reduced by almost 10 (9.8) days per admission.
- Each site saved approximately $3.3 million per year.
“People can return home sooner because a higher level of care and support is in place when they leave hospital. If all hospitals in Ontario with mental health services were able to implement our transitional discharge model, we would save $60 million per year in hospital stay costs alone while providing enhanced mental health care.”
International implementation
In Scotland, the parliament has already declared TDM as a best practice after demonstrating a significant reduction in readmission rates.
The TDM approach is now considered a “good practice” by WHO and was recently the only Canadian example included in its Guidance on community mental health services: Promoting person-centered and rights-based approaches. This set of publications provides information and support to all stakeholders who wish to develop or transform their mental health system and services to align with international human rights standards including the UN Convention on the Rights of Persons with Disabilities.
A golden age in microbiome research
According to Dr. Jeremy Burton, we’re in a golden age of microbiome and probiotics research.
“Thanks to advancements in next-generation sequencing, we’re learning more and more every day about the impacts of the microbiome on the human body,” states Dr. Burton.
Effective September 1, 2020, Dr. Burton has been appointed as Research Chair in Human Microbiome and Probiotics at Lawson Health Research Institute for a five-year term. As part of the Chair’s responsibilities, Dr. Burton will also assume the title of Director for the Canadian Centre for Human Microbiome and Probiotics Research, which is located at Lawson.
Funded by an endowment through St. Joseph’s Health Care Foundation, the position is responsible for leading Lawson’s Human Microbiome and Probiotics research program. The specialized research chair was established at St. Joseph’s in 2007 as a result of a significant investment by Danone International, in recognition of groundbreaking microbiome research by Dr. Gregor Reid, the inaugural holder of the Chair.
With extensive experience in both academia and industry, Dr. Burton is a world-renowned scientist specializing in urinary microbiome research. He points to the diversity of microbiome research at Lawson as a strength to be leveraged.
“Our program is conducting a diverse array of microbiota-related research from probiotic studies to fecal transplants to the investigation of drug-microbiome interactions,” explains Dr. Burton. “There’s a lot of interest in conducting microbiome research as it’s become clear how it affects so many human systems. We are also working with a number of other groups across the city – both clinical and basic sciences – to meet their microbiota-related research needs.”
There are two pillars to Dr. Burton’s vision for microbiome and probiotics research at Lawson. The first is advancing translational research that leads to improved patient outcomes, such as new microbial therapies. The second is improving our understanding of the microbiome by studying its function in real-time.
“In most studies, we collect patient samples, put them in the freezer and then analyze them later. We now want to follow people in real-time to get a better understanding of how the microbiome functions inside the human body,” notes Dr. Burton. “We hope to accomplish this by harnessing technologies already available at Lawson. For example, we’ve been collaborating with the Lawson Imaging program to look at bacteria in real-time using the Institute’s imaging technology.”

Above: Dr. Jeremy Burton (right) in the lab with Dr. Kait Al (left), Postdoctoral Fellow
Dr. Burton is known for forging strong interdisciplinary relationships to enhance knowledge translation, especially within the Division of Urology.
“Dr. Burton has established a robust academic laboratory and strategic partnerships that are advancing the Institute’s scientific mandate. He is a natural leader,” says Dr. David Hill, Lawson Scientific Director. “As Research Chair in Human Microbiome and Probiotics, Dr. Burton will further Lawson’s reputation in the field.”
Dr. Burton will build on a 30-year legacy of microbiome research.
“There’s a long history of microbiome research at Lawson and St. Joseph’s,” he says. “We were lucky to have visionaries like Dr. Gregor Reid – my predecessor in this position – who have helped revolutionize the field.”
For Dr. Burton, this is the next step in an illustrious career with Lawson. He first joined the Institute and Western University’s Schulich School of Medicine & Dentistry as a Postdoctoral Fellow in 2001 after completing his BSc, MSc and PhD at the University of Otago in New Zealand.
“I had a very productive time as a Fellow, publishing something like 15 manuscripts in two years. It was an amazing experience and a time that I really relished.”
He was then recruited to industry in 2003 where he developed a strong background in clinical trials and global business development.
“Working in industry helped shape me into the principal investigator that I am today. But there were so many questions about the microbiome that I wanted to answer and I ultimately found myself back in academia.”
Dr. Burton rejoined Lawson as a Scientist in 2011. Prior to his appointment as Lawson Research Chair in Human Microbiome and Probiotics, he held the title of Deputy Director of the Canadian Centre for Human Microbiome and Probiotics Research since 2011 and Miriam Burnett Chair in Urological Sciences since 2013. He is also an Associate Professor in the Departments of Surgery and Microbiology and Immunology at Schulich Medicine & Dentistry.
“What brought me back to London is the people and the collaborative environment. Researchers cross departmental and divisional borders with ease. As a scientist, I can walk from my lab to a clinic, and clinician-researchers can do the same in reverse. Everyone has a ‘can do’ attitude and they are willing to test big ideas with one another.”
Learn about recent microbiome and probiotics research at Lawson:
- Gut microbiome may influence how cancer patients respond to oral therapies, study suggests
- New urinary microbiome study could be first step in providing personalized care to patients with ureteral stents
- Fecal transplants show promise as treatment for non-alcoholic fatty liver disease
- Café Scientifique: The invisible world inside us
- Using probiotics to protect honey bees against fatal disease
- Could microorganisms in poop help treat the deadliest form of skin cancer?
- Researchers find gut microbiome plays an important role in atherosclerosis
- Probiotics for respiratory tract infections could save Canada nearly $100 million a year
A year in review: Lawson research highlights from 2018
New clinical protocol after general surgery cuts opioid prescribing in half
Recognizing the role that opioid prescribing plays in the national opioid crisis, a team of researchers at Lawson and Western University have developed a new clinical protocol called STOP Narcotics. The protocol includes a combination of patient and health care provider education and an emphasis on non-opioid pain control. The study found that they were able to reduce the overall amount of opioids being prescribed after general surgery by 50 per cent while still adequately treating a patient’s post-operative pain. Read more.
Probiotics for respiratory tract infections could save Canada nearly $100 million a year
A recent study suggests the use of probiotics to prevent respiratory tract infections in Canada could result in nearly $100 million per year in savings. There is growing evidence that probiotics can reduce the risk of respiratory tract infections and lower their frequency, as well as reduce the duration of an infection, antibiotic use and absences from work. Replicating a research model used in France, researchers examined the potential clinical and economic impacts in Canada. Read more.

Blood test can predict optimal treatment for advanced prostate cancer, study finds
An international collaborative study between Lawson, Memorial Sloan Kettering Cancer Center, the Royal Marsden and Epic Sciences is one of the first to demonstrate that a blood test can predict how patients with advanced prostate cancer will respond to specific treatments, leading to improved survival. The study used a liquid biopsy test that examines circulating tumour cells (CTCs) in blood samples from patients with advanced prostate cancer who are deciding whether to switch from hormone-targeting therapy to chemotherapy. Read more.

Machine learning could predict medication response in patients with complex mood disorders
Mood disorders like major depressive disorder (MDD) and bipolar disorder are often complex and hard to diagnose, especially among youth when the illness is just evolving. This can make decisions about medication difficult. In a collaborative study by Lawson, The Mind Research Network and Brainnetome Center, researchers have developed an artificial intelligence (AI) algorithm that analyzes brain scans to better classify illness in patients with a complex mood disorder and help predict their response to medication. Read more.
Lawson researchers receive $4.4 million to study personalized medicine at LHSC
Personalized medicine is the analysis of a patient’s DNA to predict how they will respond to medications. Led by Dr. Richard Kim, scientist at Lawson and clinical pharmacologist at London Health Sciences Centre (LHSC), researchers at Lawson have received $4.4 million to study an expanded personalized medicine program at LHSC that involves full integration of research into patient care. Read more.

Drinking more water does not slow decline of kidney function for patients with kidney disease clinical trial shows
A study published in JAMA (Journal of the American Medical Association) by researchers at Lawson and Western University found that coaching patients with Chronic Kidney Disease to drink more water does not slow down the decline of their kidney function. Read more.

Funding for unique strategy to prevent homelessness after hospital discharge
On September 10, the Ministry of Families, Children and Social Development, announced that Lawson will receive $223,572 from the Homelessness Partnering Strategy’s Innovative Solutions to Homelessness funding stream to support the project “No Fixed Address Version 2 Expansion” research project. This research will further refine the No Fixed Address strategy for reaching and supporting patients during the crucial transitional period when they are being discharged from the hospital and re-integrated into the community. Read more.

Synthetic surfactant could ease breathing for patients with lung disease and injury
Human lungs are coated with a substance called surfactant which allows us to breathe easily. When lung surfactant is missing or depleted, which can happen with premature birth or lung injury, breathing becomes difficult. In a collaborative study between Lawson and Stanford University, scientists have developed and tested a new synthetic surfactant that could lead to improved treatments for lung disease and injury. Read more.

Research team develops clinically-validated 3D printed stethoscope
A team of researchers have developed an open-source, clinically validated template for a 3D printed stethoscope for use in areas of the world with limited access to medical supplies – places where a stethoscope could mean the difference between life and death. Read more.

Family environment influences emotional well-being of children with epilepsy
Children with epilepsy have a higher risk of developing emotional and behavioural disorders, including depression, anxiety and poor self-esteem, yet it has been difficult for researchers to pinpoint why this occurs. Researchers at Children’s Health Research Institute, a Lawson program, have found that family environment influences the relationship between clinical characteristics of epilepsy at diagnosis and children’s emotional well-being two years later. Read more.

How the brain is folded provides researchers with an accurate marker to predict psychosis in high-risk patients
By using images of the brain to look at how its outer surface is folded on itself, researchers can predict which high-risk patients will develop psychosis with more than 80 per cent accuracy. Before now, there has been no way to examine young people before they become ill to reliably identify who will develop acute psychosis and who will not. Read more.

High-dose radiation can improve survival in cancer patients once thought incurable
Cancer that spreads from an original tumour to other parts of the body is generally considered incurable. In an international study led by Lawson, researchers challenged this idea by showing that high-dose radiation can improve survival in patients with cancer that has spread to five or less sites. The study called SABR-COMET was the first randomized phase II clinical trial of its kind. Read more.
Advancing research during the COVID-19 pandemic
From the moment the COVID-19 pandemic was declared in March 2020, our teams at Lawson Health Research Institute have been at the forefront. Researchers at London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London immediately began to work towards understanding the new virus in an effort to discover lifesaving health-care solutions.
To date, dozens of research projects have been advanced through Lawson with some receiving international attention as ‘world firsts’. As we mark the three-year anniversary of COVID-19 being declared a global pandemic by the World Health Organization (WHO), we share with you COVID-19 research highlighted over the past year.
Study finds acute kidney injury associated with severe COVID-19 leads to high mortality rates
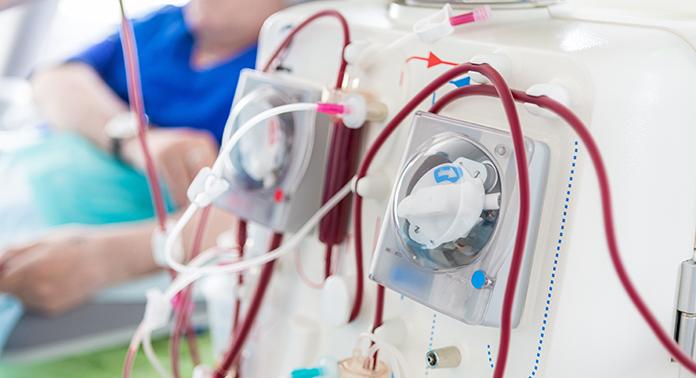
Severe cases of a COVID-19 infection can cause a host of serious complications, including acute kidney injury. In a published study, scientists at Lawson found that acute kidney injury in patients with a severe COVID-19 infection leads to a high mortality rate.
By accessing data collected through the Ontario Renal Network (ORN), Dr. Peter Blake, Lawson Researcher and Provincial Medical Director at the Ontario Renal Network, and his colleagues examined 271 people at 27 renal programs across the province, including patients at LHSC, who received dialysis for acute kidney injury due to a COVID-19 infection. Read more.
Study shows a decline in Veterans’ mental health throughout the pandemic

In published findings from Lawson, more than half of Canadian Veterans reported a decline in their mental health over the course of the COVID-19 pandemic.
When it comes to mental health conditions, Veterans are an at-risk population, often having higher rates of depression and post-traumatic stress disorder (PTSD). When the COVID-19 pandemic hit, scientists at Lawson wanted to understand its effects on this already at-risk population.
To examine the potential impacts the research team launched a longitudinal study recruiting Canadian Veterans and spouses of Canadian Veterans. Participants complete online questionnaires every three months, with questions focused on mental health and virtual health care services. Read more.
Virtual care associated with significant environmental and patient cost savings

A study published in JAMA Network Open by researchers at ICES, Lawson and Western University found that virtual care during the COVID-19 pandemic led to a significant reduction in carbon dioxide emissions and patient travel-related expenses, such as gasoline, parking or public transit costs.
Findings show that for more than 10 million patients with at least one appointment during the study period (63 million visits in total), virtual care was associated with estimated savings of:
• 3.2 billion kilometers of patient travel;
• 545 to 658 million kilograms of carbon dioxide (CO2) emissions; and
• $569 to $733 million (Canadian [US $465-$599 million]) in expenses for gasoline, parking, or public transit. Read more.
London researchers discover novel method to diagnose long COVID

Published in Molecular Medicine, researchers at Lawson found that patients with post-COVID-19 condition (long COVID) have unique biomarkers in their blood. The team is now working on developing a first of its kind blood test that could be used to diagnose long COVID. The discovery could also lead to new therapeutics for this condition.
The researchers studied 140 blood samples from participants at LHSC and St. Joseph’s Health Care London, including St. Joseph’s Post-Acute COVID-19 Program. Participants were those with presumed long COVID, hospital inpatients with acute COVID-19 infection and healthy control subjects. Read more.
Researchers are combining new technologies to examine blood proteins in COVID-19 patients

Published in the Journal of Cellular and Molecular Medicine, a team at Lawson discovered unique patterns of blood plasma proteins in critically ill patients that may help develop a more personalized approach to treating severe COVID-19.
Called the plasma proteome, the proteins studied are released by cells that often play an important role in the body’s immune response to viruses. The research team studied how they adapt and change to a COVID-19 infection. Read more.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Advancing research on haemochromatosis
Thanks to decades of work by dedicated researchers like London, Ont.-based Dr. Paul Adams, haemochromatosis has become much easier to diagnose, though many people are still unaware of the genetic condition. And while treatment options are effective, they are limited, according to a new review published in The Lancet.
In Canada and the United States, one in 227 people have haemochromatosis, making it more common than cystic fibrosis. However, the U.K. Biobank Project, a large-scale biomedical database and research resource, found that only 12 per cent of people who have the condition actually know they have it.
Dr. Adams, a Scientist at Lawson Health Research Institute and Professor at Western University’s Schulich School of Medicine & Dentistry, explains, “The most common genetic test done in Canada and the U.S. is the best way to make the diagnosis, but you have to think of the condition and the doctor has to know that there is a genetic test available. So those two steps are some of our stumbling blocks.”
In Ontario, testing and diagnosis often comes only after some other issue arises, “One day someone stumbles on the fact that there's a liver abnormality, or the patient is complaining of fatigue and the doctor orders blood tests, thinking blood iron is going to be low,” Dr. Adams explains. “And then it turns out to be very high.”
Most common in people of Northern European ancestry, haemochromatosis results in excess iron in the body and includes symptoms such as fatigue and arthritis pain, and can lead to serious complications like cirrhosis of the liver, liver cancer and death.

Starting in January 2000, Dr. Adams conducted a multi-year study involving 20,000 London, Ont. residents that helped change how haemochromatosis is diagnosed – moving from testing iron levels to genetic testing. With iron levels affected by alcohol consumption, obesity, inflammation and some types of cancer, the previous measure led to many false positive tests.
But knowing when genetic testing should be done remains a challenge. The underdiagnosis and lack of awareness also remain an issue when it comes to more serious complications.
“If this is diagnosed early, like as a young adult, then this can be treated and those complications won’t develop,” Dr. Adams says. “If you donate blood, treatment is very similar to that procedure and it's tolerated extremely well in most. People who have a lot of excess iron will have this blood taken once a week until their iron levels come down.”
He hopes this new publication will lead to better diagnosis and treatment, and sees a future in emerging biological therapies.
Dr. Adams continues to be involved in global research, including work with the U.K. Biobank Project on genomic testing, and is investigating partnerships to develop future gene editing treatment.
People looking for more information about haemochromatosis can reach learn more on the Canadian Haemochromatosis Society’s website.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
An image of the future: Innovations in imaging research
Lawson Health Research Institute (Lawson) has long been a leader in biomedical imaging. The first Canadian magnetic resonance imaging (MRI) of a human occurred at St. Joseph’s Health Care London (St. Joseph’s). The country’s first positron emission tomography/computed tomography (PET/CT) and positron emission tomography/magnetic resonance imaging (PET/MRI) scanners were also installed at St. Joseph’s. New developments in imaging research continue to enhance the diagnosis, prevention and treatment of a wide range of diseases, from cancer to post-traumatic stress disorder.
On May 23, Lawson hosted a Café Scientifique event where a panel of Lawson Imaging scientists discussed their cutting-edge work. Guests had the opportunity to ask questions as part of an open-forum discussion to gain insights from the speakers, and from one another.
In celebration of Canada’s 150th anniversary as a nation, this event is the first of a two-part series focusing on the future vision for health care in Canada and the legacy that research at Lawson will leave.
Imaging of the heart: Seeing the cause of chest pain more clearly
By Dr. Ting-Yim Lee, Lawson scientist, Medical Physicist at St. Joseph’s, professor at Western University’s Schulich School of Medicine & Dentistry, and scientist at Robarts Research Institute
When patients with chest pain arrive in the emergency department, they are given an electrocardiogram (ECG) and blood test. These diagnostic tests determine if the pain has a non-cardiac cause (such as heart burn), if it is caused by a heart attack, or if the patient has angina (plaque formation in the coronary arteries that either reduces or temporarily cuts off blood flow to the heart) but did not have a heart attack.
If a patient has angina, they are then given additional diagnostic testing to see whether a blood clot has formed and where it is located. This is determined by two different imaging techniques: x-ray imaging (angiogram) and nuclear imaging. This process is invasive and means that patients must be scheduled for two different exam days. Using two techniques also means that there can be image misalignment, and the images often provide poor detail.
Dr. Ting-Yim Lee’s lab has pioneered a Computed Tomography (CT) method for imaging blood flow to the heart muscle (CT Perfusion), which can help patients avoid unnecessary tests and treatment, as well as reduce health care costs.
“CT imaging is a non-invasive imaging technique that uses x-rays to create high-detail cross-sectional images of the body. Using this method, we can evaluate the degree of blockage in coronary arteries – with one diagnostic test instead of two,” says Dr. Lee.
Using light and sound to improve breast surgery
By Dr. Jeffrey Carson, Lawson scientist and associate professor at Western University’s Schulich School of Medicine & Dentistry
“Most women diagnosed with breast cancer undergo surgery, and months of chemotherapy and radiotherapy. They must deal with the discomfort, side-effects, emotional stress and financial burden of treatment. Almost one in four surgeries for breast cancer must be repeated, meaning many women have to go through this all over again,” says Dr. Jeffrey Carson.
In breast conserving surgery, there is a high chance of repeat surgery as the surgeon must see and remove 100 per cent of the tumour in order for it to be successful. They are not able to determine whether the entire tumour was removed until after the surgery has been completed.
Dr. Carson and his team at St. Joseph’s have developed a technology called Intraoperative Photoacoustic Tomography (iPAT), which has the potential to reduce the chance of repeat surgery for breast cancer. The technology is able to image surgery specimens in the operating room during surgery, allowing surgeons to determine whether the whole tumour has been removed before the surgery is complete.
How imaging can improve the management of epilepsy
By Dr. Udunna Anazodo, postdoctoral fellow at Lawson
Most patients with epilepsy are effectively treated with antiepileptic drugs. However, 36 per cent will not respond to the drugs. For these patients, surgery on the area of the brain that is causing seizures is the standard of care – if patients are good surgical candidates.
“If patients with epilepsy are to undergo surgery there must be a good indication of where the seizure focus is and it must be possible to determine that removing this portion of the brain will not affect brain function,” says Dr. Udunna Anazodo.
To see whether they are good candidates for surgery, patients must undergo an invasive procedure called intracranial monitoring, where electrodes are placed on the brain.
Dr. Anazodo has been studying how PET/MRI can be used to map seizures with the goal of minimizing the need for invasive intracranial monitoring. This technique makes it possible to locate areas in the brain that cause seizures and to see if the seizures affect brain functions.
See photos from the event on Lawson’s Facebook page.

Above: Café Scientifique presenters (from left to right): Drs. Jeffrey Carson, Frank Prato (moderator), Ting-Yim Lee and Udunna Anazodo.
An innovative year: Top 12 research stories of 2023
It’s been another year of transformational research at Lawson Health Research Institute. Our teams have published groundbreaking findings and launched new studies that will have a profound impact on patient care.
The following are 12 highlights of research and innovation from across London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London (St. Joseph’s). From trialing new cancer treatments to advancing understanding of mental health, our research teams have achieved a number of important milestones.

1. New study suggests blood plasma proteins hold answers to better understanding long COVID
Lawson researchers continued to advance understanding of COVID-19 this past year. In one study, researchers found that unique patterns in blood plasma proteins of patients with suspected long COVID could act as a drug target to improve patient outcomes. Read more.

2. New study finds exercise, cognitive training combo boosts mental sharpness in seniors
A study from Lawson and Western University found that a combination of computerized cognitive training and aerobic-resistance exercises can improve functions like memory, attention, recognition and orientation in older adults with mild cognitive impairment. The results suggest a new way to address declining mental sharpness in older adults. Read more.

3. $7.55 million in funding to take LHSC-developed technology global
Technology to diagnose rare genetic disorders developed by researchers at Lawson and LHSC will be going global thanks to $7.55 million in funding from Genome Canada grant and Illumina Inc. The new artificial intelligence-led technology could allow rare diseases to be diagnosed with a simple blood test. Read more.

4. Fecal transplants show promise in improving melanoma treatment
Fecal microbiota transplants (FMT) from healthy donors are safe and could improve response to immunotherapy in patients with advanced melanoma, according to results from a world-first multi-centre clinical trial led by Lawson researchers. Read more.

5. New study shows technology could play an important role in mental health support
A team of Lawson researchers found that the use of ‘smart home’ technology like touch screen devices, activity trackers, weigh scales and medication dispensers may lead to better outcomes for those living with both mental health and physical disorders. The study found that participants using the technology started logging more exercise, making healthier food choices and not missing medication doses. Read more.

6. Canadian children’s hospital visits for suicidal thoughts, self-poisoning and self-harm up during pandemic, study finds
A national study with Lawson researchers found that during the first two years of the COVID-19 pandemic, adolescent emergency department (ED) visits and hospitalizations for suicidal thoughts, self-harm and self-poisoning increased across Canada, with the greatest increase occurring among adolescent girls. Read more.
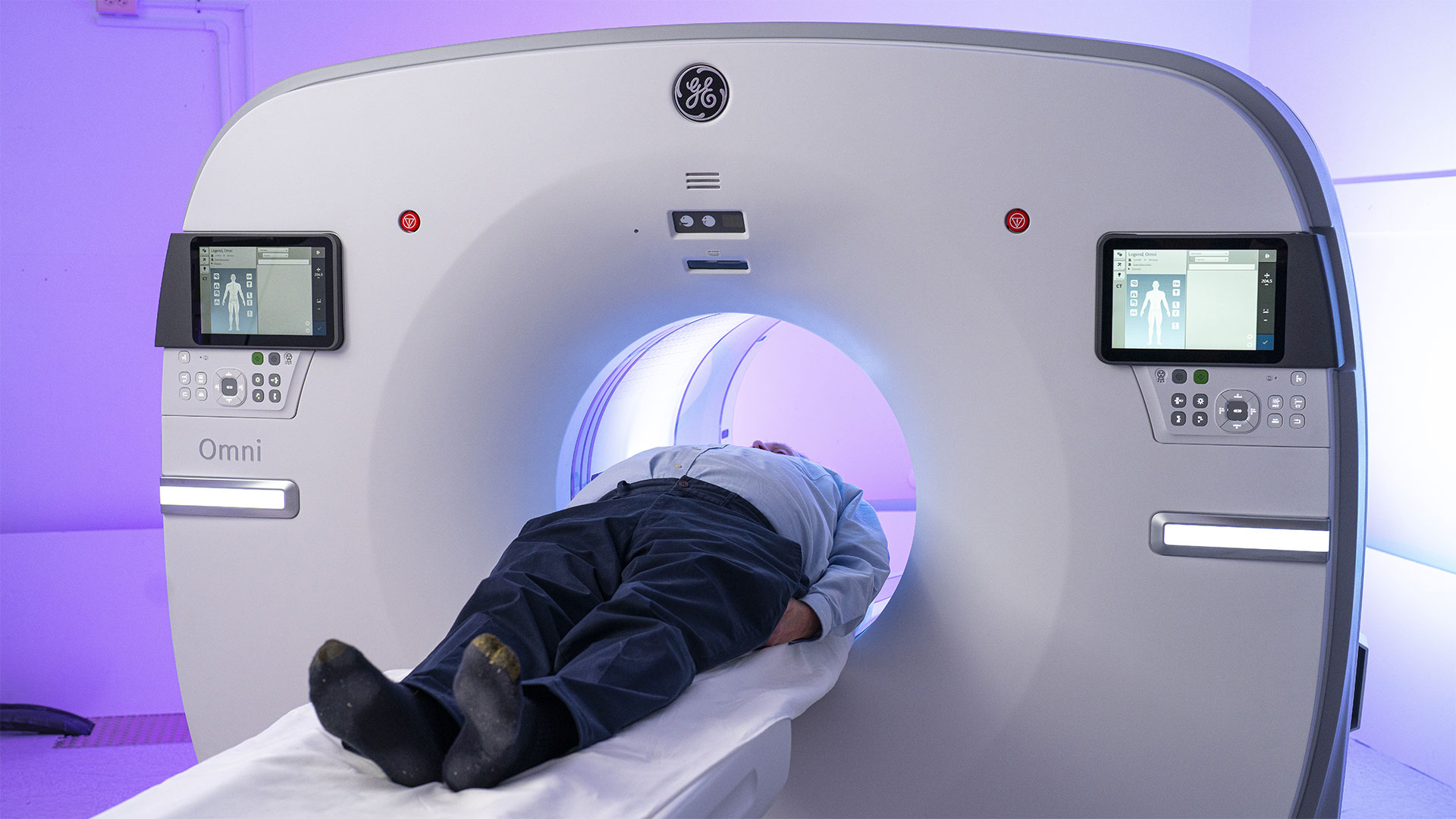
7. St. Joseph’s to become Canada’s first centre of excellence in molecular imaging and theranostics
A partnership between Lawson, St. Joseph’s Health Care London and GE HealthCare will create Canada’s first centre of excellence in molecular imaging and theranostics at St. Joseph’s. The centre will focus on using precision diagnostic imaging and targeted therapy to advance personalized treatment of cancer and other diseases. Read more.
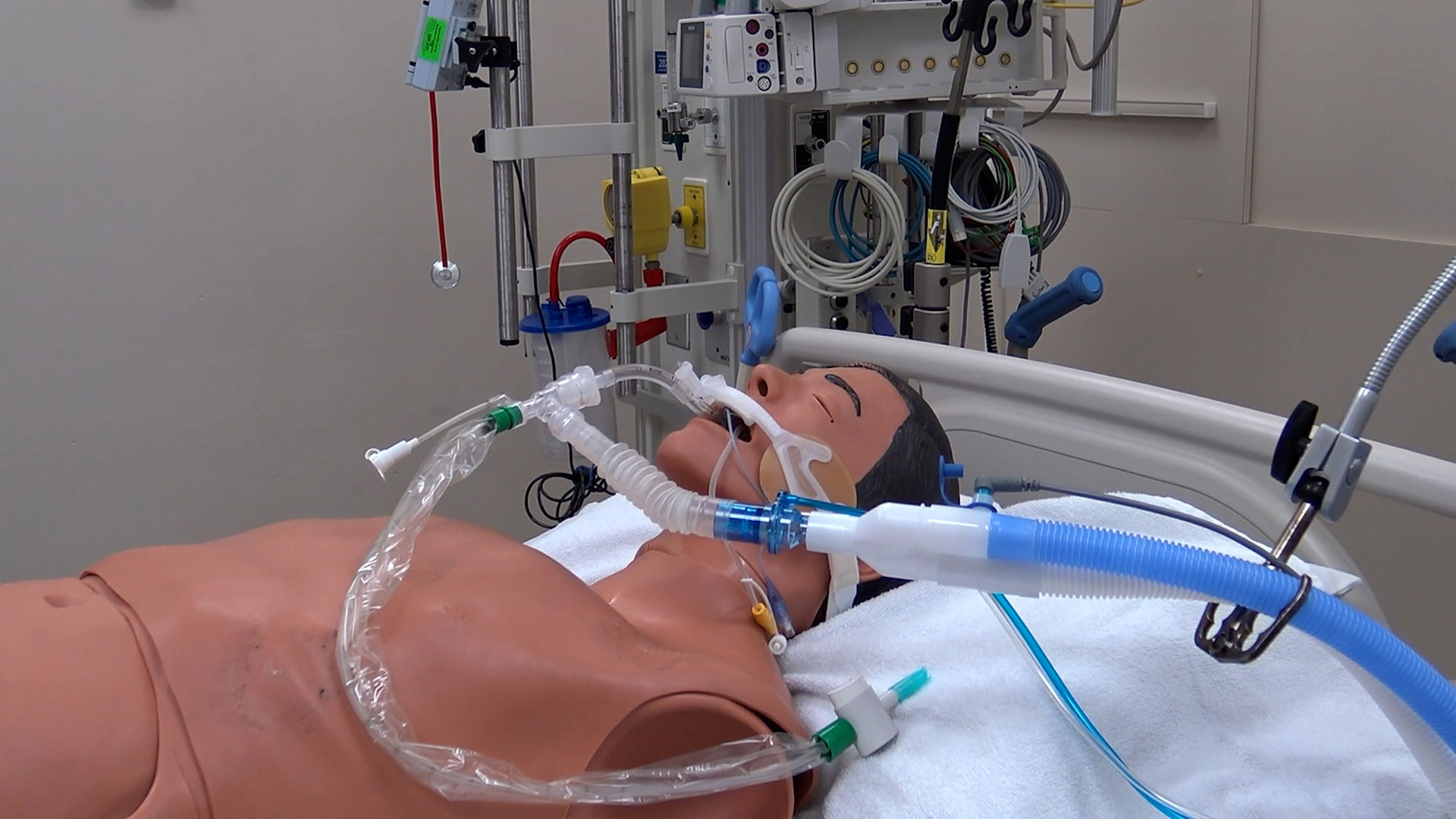
8. Researchers investigate a new method of sedation for paediatric patients
Intravenous sedatives are normally used to sedate critically ill children. However, they can contribute to a complication called delirium, which includes symptoms of confusion, disorientation, agitation, excessive drowsiness and poor attention. To improve outcomes, scientists at Children’s Health Research Institute (a program of Lawson), Sunnybrook Research Institute and The Hospital for Sick Children (SickKids) are collaborating on a pilot study to understand whether inhaled sedation could be a better alternative to keep critically ill children sedated and comfortable. Read more.
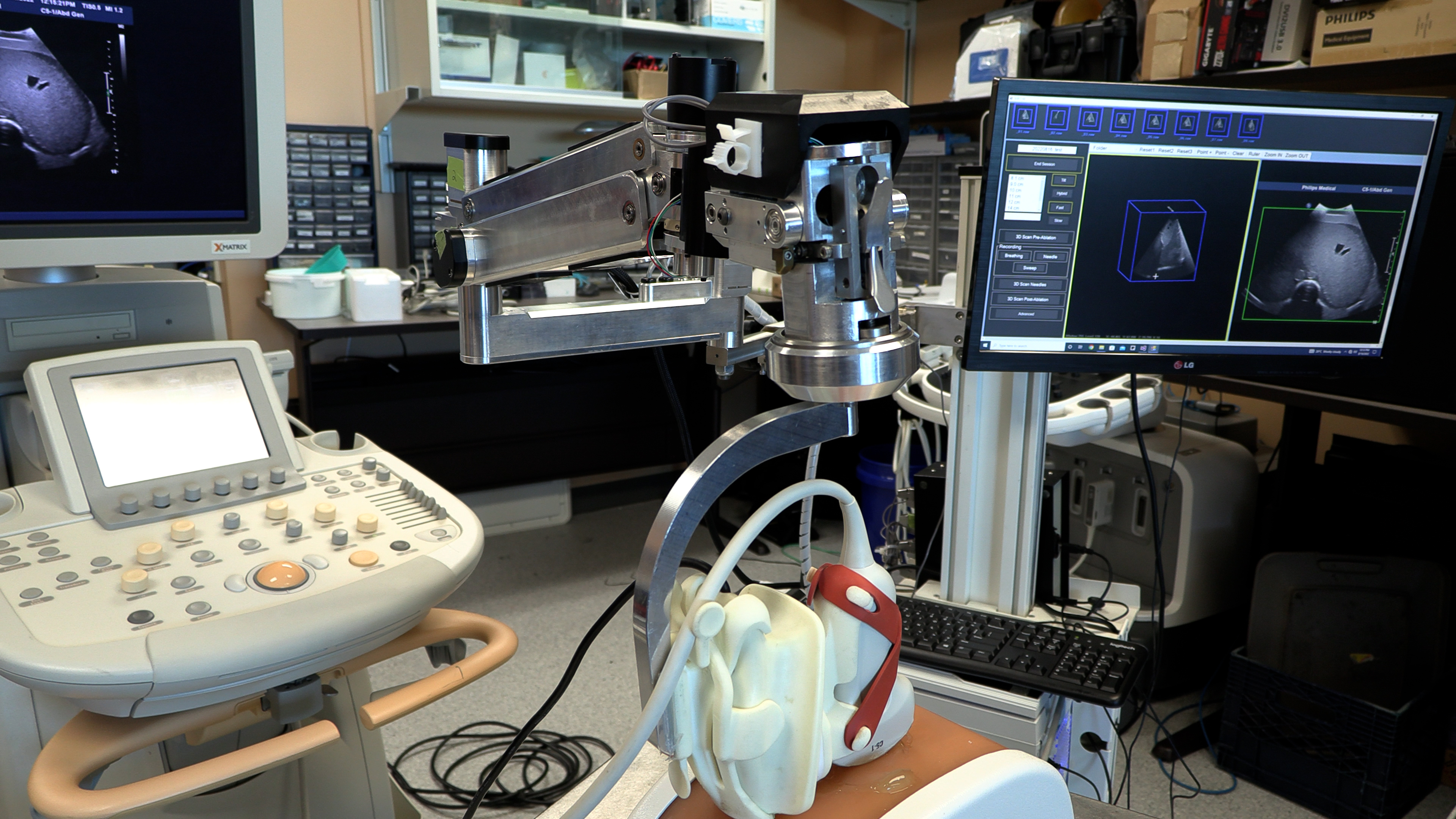
9. New robotic 3D ultrasound may improve accuracy of liver cancer ablation therapy
A technique that turns a normal ultrasound into a 3D image is showing promise in making thermal ablation for liver cancer treatment more accurate in a study from Lawson and Western University. Thermal ablation – using heat to destroy a cancerous tumour – can have fewer complications and a shorter recovery time than surgery. Read more.

10. Assessing neurofeedback in stroke survivors
Functional near-infrared spectroscopy (fNIRS) is used to detect changes in brain oxygen levels using light, but more recently it has also been used to develop brain-computer interfaces – allowing patients with brain injuries to control a device with their thoughts. Researchers at Lawson launched a new study to assess whether fNIRS can be used to improve patient outcomes during stroke rehabilitation. Read more.

11. Specific type of inflammation may be linked to risk of colorectal cancer
A preclinical study found that a specific type of inflammation may be linked to an increased risk of colorectal cancer. Previously, the degree of inflammation caused by illnesses like colitis, Crohn’s disease and other forms of inflammatory bowel disease were shown to be an important indicator of the development of colorectal cancer. However, this new study found the type of inflammation, rather than the severity and duration, may be more important in determining cancer risk. Read more.
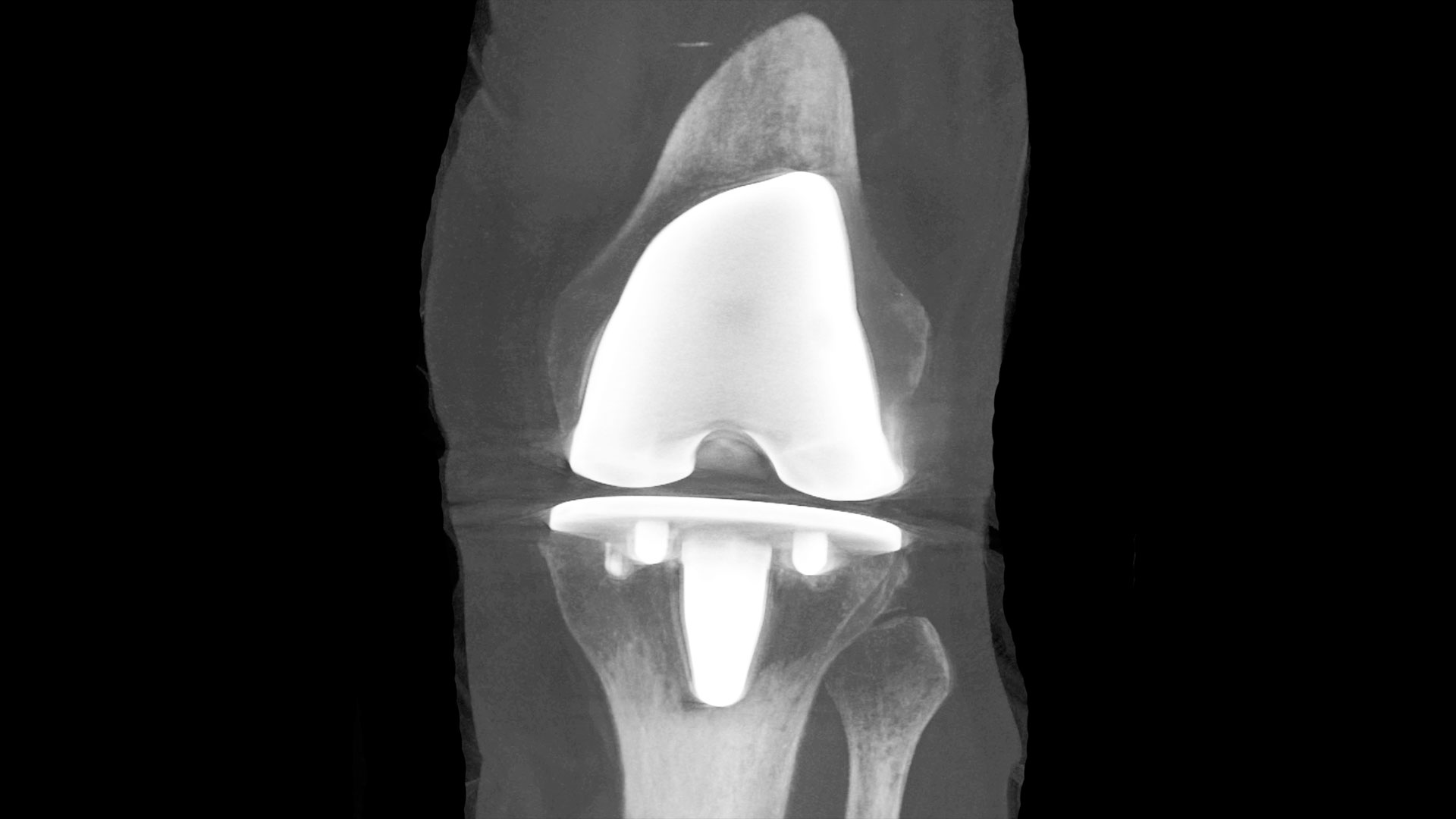
12. New study examining if probiotics can improve outcomes in knee replacement surgeries
Lawson researchers launched a study to assess whether daily probiotics can improve outcomes in patients undergoing a total knee replacement surgery. Of the more than 70,000 knee replacement surgeries in Canada each year, nearly 10 per cent of patients experience complications. With patients who are considered healthy likely to have better outcomes, the research team is interested in improving the gut microbiome as a way to support patients’ overall health. Read more.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Assessing neurofeedback in stroke survivors
A new study aims to assess the use of functional near-infrared spectroscopy (fNIRS), a type of imaging, to provide neurofeedback during stroke rehabilitation with a goal of eventually improving patient outcomes.
fNIRS is used to detect changes in brain oxygen levels using light. More recently it has also been used to develop brain-computer interfaces (BCIs), which allow patients with brain injuries to control devices like robotic arms with their thoughts.
Dr. Sue Peters, a Scientist at Lawson Health Research Institute and Director of the Neurorehabilitation Physiology Lab at St. Joseph Health Care London’s Parkwood Institute, was one of the recipients of the Spring 2022 Lawson Internal Research Fund (IRF) Awards.
The funds will go towards a new study to assess whether fNIRS can be used to direct neurofeedback in stroke survivors – helping them with rehabilitation.
“Currently, there's no real measure of brain activity that is used in stroke rehabilitation to help make clinical decisions,” says Dr. Peters, who is also a Professor at Western University.

Over 400,000 Canadians live with the effects of a stroke, according to the Heart and Stroke Foundation, and there’s hope that fNIRS could make a big difference by eventually improving movement and independence.
“We're going to use the device in some common tasks that people might do with their arm and determine whether we can use this device reliably and accurately in a stroke-related context,” Dr. Peters explains.
Participants in the study will imagine moving while remaining still. This activates very similar parts of the brain to when people actually move. If done correctly, patients will see a visual cue generated through measurement using fNIRS.
“We know from MRI studies that when I move my right hand, the left side of my brain is activated,” notes Dr. Peters. “We think we can use this concept in stroke rehab.”
Dr. Peters is recruiting 40 people from the community who are at least six months post stroke and 40 healthy adults of all ages. They will first participate in motor assessment with a physiotherapist and then wear an fNIRS cap while thinking about moving their wrist to measure brain activity.
Previously, there were a lack of methods to image the brain during real-life movement.
“The hope is to eventually conduct a clinical trial where we're testing motor interventions to see whether some things are more effective than others at activating the regions of the brain that were impacted by the stroke.”
Dr. Peters believes the study has the potential to have a big impact on the future of rehabilitation for stroke patients, leading to lasting changes in quality of life.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Bridging the gap from discovery to patient care
The following column was provided to Hospital News by Dr. David Hill, scientific director, Lawson Health Research Institute.
Dedicated health researchers across the country are working every day to make discoveries that improve patient outcomes and support a higher quality of life. Our research hospitals have a mandate to develop and test new treatments, technologies and procedures that address our most pressing health challenges.
There is a cycle of health innovation that is supposed to happen – scientific discoveries are made, they transition to clinical trials and then are adopted as an improved standard of care. This is followed by evaluations of the new method and moving along to the next cycle of refinements and improvements. But the reality in Canada is that gaps, in some cases chasms, disrupt the creation and adoption of evidence-based health innovations.
This starts with discovery. The research funding climate in Canada continues to be extremely difficult. Despite the Federal Government outlining substantial new investments in discovery research in Budget 2018 much of that money will not be available to researchers until 2020 and beyond, and the Canadian Institutes of Health Research (CIHR) continues to be limited by a low funding rate of around 14 per cent. Funding for large, definitive clinical trials is especially difficult to support with public funds. Too many good ideas are left unfunded, and in that environment researchers can feel it’s wiser to propose incremental and ‘safe’ science that avoids controversy and the risk of losing support for experienced research teams built up over many years.
Yet researchers are persistent and manage to secure funding from a range of smaller agencies. Unfortunately, many of these do not fund the indirect costs of research necessary to cover administration, infrastructure, equipment maintenance and upgrades, and the investigator’s salaries. Indirect costs are estimated to be approximately 40 per cent on top of direct study costs. In research hospitals these costs generally fall on the institutions to find funding outside of the provincial government budget that covers the costs of hospital care. This is a negative spiral whereby the more successful a hospital becomes in attracting research funds, the bigger the gap in finding the resources to support that research.
When innovative solutions to health care problems are delivered, backed by solid evidence, adoption into our hospital-based care is often far from rapid. Currently, in most provinces, there is no funding mechanism to translate health innovation to the ‘real world’ setting of our front-line care. Yet, such a mechanism is crucial to the translation of science. Clinical trials are carefully designed with strict protocols and criteria for a highly specific population of patients. Innovations that work in a clinical trial do not always work in the real world where patient populations and settings are much more complex.
Following a clinical trial, innovation needs to be tested at the point of care. Without funding to do this, research innovation hits a roadblock. Scientists are left waiting and hoping that one day their provincial government might look to incorporating their innovations into the health system funding schedule. Meanwhile, their work may be used to inform health care improvements in other nations.
An example can be found in medical imaging research. Canadian scientists, including those at Lawson Health Research Institute, are leaders in the development of positron emission tomography (PET) biomarkers to improve diagnosis and understanding of disease using PET scans. PET biomarkers are successfully created and then validated in clinical trials across our nation, but there is little funding to translate them back in a timely fashion to patient care in our hospitals. While countries like the US and Europe readily adopt these innovations, Canada lags behind.
This gap was addressed in a report to the Federal government by the Advisory Panel on Healthcare Innovation entitled “Unleashing Innovation: Excellent Healthcare for Canada” and published in 2015. The panel recommended the formation of a Healthcare Innovation Agency of Canada open to hospitals and other care providers in order to evaluate health innovations in the real-world setting of our health system. Scientists would apply by putting forward evidence from their research, including that collected from clinical trials. They would then design a new translational study to test their innovation at the point of care, with the goal of building evidence for presentation to provincial government.
Will everything tested at the point of care succeed? No; some things will fail in the real world. This is why such a fund is so important. It will show whether or not an innovation truly benefits patients and if it’s ready for wider adoption. If successful, the evidence will highlight the right time to bring innovations into the mainstream standard of care. By bridging this gap in the system, we can improve patient care and ensure a timely return on the investment in science.
Dr. David Hill is scientific director at Lawson Health Research Institute, the research institute of London Health Sciences Centre and St. Joseph’s Health Care London.
Can type 2 diabetes go into remission?
For Wayne Kristoff, the possibility of getting off all medication for his type 2 diabetes was so intriguing he jumped at a chance to participate in an innovative trial in London. The REMIT study aims to induce remission of the condition – an exciting new concept being tested by researchers at Lawson Health Research Institute.
Kristoff was diagnosed in June 2014, which was difficult but not unexpected because there is a history of the illness in his family. He had to work his way up to taking four pills a day for his diabetes, which came with significant side effects. “If there was a way to get off medication, I wanted to be part of it,” says the 68 year-old.

He met the study criteria and was enrolled in February 2016. The results, so far, have been life changing for the Londoner. Since May 2016 Kristoff (right) has been off all medication, his blood sugar levels are good, and he has more energy and feels better than he has in years. He’s also lost 30 pounds thanks to the support offered by the research team.
“I remember well where I was and what I was doing when I received the call telling me that I could stop taking all of my diabetic medication,” adds Kristoff.
A second REMIT trial is now being launched, providing another opportunity for individuals with type 2 diabetes to take part. The trial challenges traditional type 2 diabetes treatment by testing an aggressive approach in recently diagnosed patients. St. Joseph’s Hospital in London is one of seven Canadian sites taking part in the landmark REMIT study. Being led by the Population Health Research Institute (PHRI), a joint institute of McMaster University and Hamilton Health Sciences, the trial follows a PHRI pilot study of early aggressive treatment that resulted in up to 40 per cent of 83 patients with type 2 diabetes going into remission and not needing any diabetes treatment for at least three months.
When Lawson launched the initial trial in December 2015, it generated a surge of interest with more than 200 people with type 2 diabetes asking to participate.
“The idea of remission in type 2 diabetes is obviously captivating to both patients and clinicians,” says Lawson researcher and endocrinologist Dr. Irene Hramiak, Chief of the Centre for Diabetes, Endocrinology and Metabolism at St. Joseph’s. “This overwhelming interest in the REMIT trial tells me that patients want solutions that will optimize care and reduce the complications associated with this disease.”

The standard treatment for people diagnosed with type 2 diabetes is to start on a single medication, which is then followed by the addition of more drugs and insulin as the disease progresses, explains Dr. Hramiak. In the REMIT study, patients undergo an experimental intensive treatment - two diabetes oral medications plus insulin at bedtime - for three months to see if remission can be induced and how long patients can go without any medication.
“By being proactive with aggressive treatment early on, the theory is that we may slow the progression of the disease,” says Dr. Hramiak. “We are attempting to actually change the disease and induce remission, which is a significant departure from the current approach.”
Those who would like more information about the trial can call 519 646-6100 ext. 65373.
Canadian researchers will test a promising new fecal microbiota treatment on patients to cure advanced melanoma
The Canadian Cancer Society (CCS) is uniting with a team of 12 researchers and collaborators to lead one of the world’s largest randomized controlled clinical trials using fecal microbiota transplantation (FMT) to improve the effectiveness of the standard of care for advanced melanoma. This phase II trial is made possible by investments of $1 million each from CCS and the Weston Family Foundation and will be overseen by the Canadian Cancer Trials Group.
An estimated 11,300 Canadians are expected to be diagnosed with melanoma in 2024. The current standard of care for patients with advanced melanoma is a type of immunotherapy called immune checkpoint blockade (ICB) and while it plays an important role in treatment, more than half of patients will still experience disease progression and unfortunately die of the disease. Finding a path to make this treatment effective for more people would have enormous impact on patient care and significantly improve the odds of surviving advanced melanoma.
The funding from CCS and the Weston Family Foundation supports all translational research and part of the trial costs (study ME17). The study is being co-led by researchers from Université de Montréal's affiliated hospital research centre (CRCHUM) and Lawson Health Research Institute, alongside collaborators and close to 130 patients with advanced melanoma who will be recruited throughout Canada to participate in this study.
The phase II trial builds on previous research that also received funding support from CCS. Those studies showed the safety and therapeutic potential of using healthy donors’ stool to influence a patient’s gut microbiota and make treatment for advanced melanoma more effective. The study will administer fecal microbiota transplants using specially-prepared oral capsules produced and pioneered at Lawson Health Research Institute, which have been a game changer in patient acceptance and ease of use.
For the past five years, the Weston Family Foundation has supported Canadian researchers working to leverage the microbiome to improve cancer diagnostics, therapy and patient care.
The biggest and most critical issues related to cancer, such as improving treatment effectiveness for people living with melanoma, are issues that require collaboration. From researchers to clinical trial leaders, to academic and scientific institutions, to caring funders and generous donors, it takes a society to transform cancer. To support cancer research and clinical trials, visit cancer.ca.
Quotes
“What saved me was trusting the scientists who knew what they were doing and the promising results of the clinical trial. To someone who is diagnosed, I would say that if you are offered this treatment, it may sound strange, but it is to help you. Thank you to the partners and the CRCHUM team for their support and for the treatments that went wonderfully well and saved my life." - Louise-Hélène Giroux, diagnosed in 2021 with stage 4 melanoma, first patient in the phase I clinical trial in Quebec to try FMT treatment
“Because of the generosity of our donors, we are able to invest in world-leading cancer research and clinical trials like this trial focused on advanced melanoma. In 2020, together with the Lotte and John Hecht Memorial Foundation, we committed nearly $1.5M into this research through an Impact Grant. Today, we are joining with the Weston Family Foundation to double down on our original investment through this clinical trial because we believe this work will transform the future of melanoma, saving lives and bringing hope to thousands of people facing the disease every year in this country.” – Dr. Stuart Edmonds, Executive Vice President, Mission, Research and Advocacy, Canadian Cancer Society
“The Weston Family Foundation is thrilled to support this pioneering research into the role of the microbiome in the fight against cancer, which has real potential to transform treatments and care for this devastating disease. It's a bold step forward in our mission to invest in innovation that delivers measurable impacts to the well-being of Canadians. Working alongside forward-thinking researchers and partners like the Canadian Cancer Society will make way for advancements that help to bring hope to patients and families affected by melanoma.” – Garfield Mitchell, Chair, Weston Family Foundation
“We are aiming to safely change the patient’s gut microbiota to improve the benefit of immunotherapy in several cancers, including melanoma. This experimental treatment consists of transplanting stool from healthy donors using a Health Canada-approved process - known as fecal microbiota transplantation (FMT). With this investment, we can pursue our randomized trial, with the goal of improving the lives of patients with advanced melanoma. We are optimistic that we will see promising results.” – Dr. Arielle Elkrief, principal investigator, Clinician-Scientist, Université de Montréal-affiliated hospital research centre (CRCHUM)
“Our early research has shown the safety of combining FMT with immunotherapy and that it may improve outcomes for patients with melanoma. Through this new trial, we hope to demonstrate that the combination is more effective than immunotherapy alone. A positive result would lead to a phase III trial with the potential to make FMT with immunotherapy the new standard of care.” - Dr. John Lenehan, Medical Oncologist at the Verspeeten Family Cancer Centre at London Health Sciences Centre and Associate Scientist at Lawson Health Research Institute, Co-chair of ME17 trial
The researchers and collaborators
The phase II clinical trial, known as the ME17 Fecal microbiota transplantation (FMT) in combination with immune checkpoint blockade in patients with advanced melanoma: A randomized phase II trial, involves several highly collaborative experts who will be working with the Canadian Cancer Trials Group (CCTG) who will administer the trial nationally. For the translational research associated with the trial, the project team includes:
Co-Principal Investigators:
Dr. Janet Dancey, Medical Oncologist and Professor, Queen’s University, Director of the Canadian Cancer Trials Group
Dr. Arielle Elkrief, Clinician-Scientist and Assistant Professor, Université de Montréal-affiliated hospital research centre (CRCHUM)
Dr. John Lenehan, Medical Oncologist at LHSC’s Verspeeten Family Cancer Centre, Associate Scientist, Lawson Health Research Institute
Dr. Bertrand Routy, Clinician-Scientist and Associate Professor, Université de Montréal-affiliated hospital research centre (CRCHUM)
Dr. Saman Maleki, Scientist, Lawson Health Research Institute, London Health Sciences Centre's (LHSC) Verspeeten Family Cancer Centre and Ontario Institute of Cancer Research (OICR)
Dr. Michael Silverman, Scientist, Lawson Health Research Institute, Medical Director of the Infectious Disease Care Program at St. Joseph’s Health Care London
Collaborators:
Dr. Seema Parvathy, Lawson Health Research Institute
Dr. Marcus Butler, Leader of the CCTG Melanoma Disease Site Committee, Princess Margaret Cancer Center
Dr. Rahima Jamal, hemato-oncologist, researcher and medical director at the Unit for Innovative Therapies (Phase I-II Unit), Université de Montréal-affiliated hospital research centre (CRCHUM)
Dr. Ian Watson, Associate Professor and Co-chair CCTG Melanoma Disease Committee, McGill University
Dr. Bingshu Chen, Professor, Queen’s University
Dr. Meriem Messaoudene, Research Associate, Université de Montréal-affiliated hospital research centre (CRCHUM)
About the Canadian Cancer Society
The Canadian Cancer Society works tirelessly to save and improve lives. We raise funds to fuel the brightest minds in cancer research. We provide a compassionate support system for all those affected by cancer, across Canada and for all types of cancer. Together with patients, supporters, donors and volunteers, we work to create a healthier future for everyone. Because to take on cancer, it takes all of us. It takes a society. Help us make a difference. Call 1-888-939-3333 or visit cancer.ca today.
About the Weston Family Foundation
At the Weston Family Foundation (formerly The W. Garfield Weston Foundation), more than 60 years of philanthropy have taught us that there’s a relationship between healthy landscapes and healthy people. That’s why we champion world-class health research and innovation with the same passion that we support initiatives to protect and restore biodiversity on our unique landscapes. We take a collaborative approach to philanthropy, working alongside forward-thinking partners to advance Canada and create lasting impacts. We aspire to do more than provide funding; we want to enable others to find transformational ways to improve the well-being of Canadians.
CIHR funding for COVID-19 enables researchers to investigate virus transmission during surgery and pandemic planning
Researchers at Western University and Lawson Health Research Institute continue to make important contributions to help mitigate the spread of COVID-19 and its negative consequences. Two projects in London will address virus transmission during surgery and pandemic planning for COVID-19, thanks to new funding announced by the Government of Canada, through the Canadian Institutes of Health Research (CIHR), along with provincial partners.
Researchers in London received more than $400,000 in funding through this latest round.
“Accelerating high-quality research and real-time evidence is a priority for Canada in its fight against COVID-19. I congratulate the successful teams for their essential work aimed at better preventing, detecting and treating COVID-19 at the individual and population levels,” said Patty Hajdu, Minister of Health in a press release. “Our government believes that it’s through collaboration and data sharing that we will respond efficiently to this global health emergency.”
Virus transmission in surgical smoke
In an effort to perform surgery during the pandemic as effectively and safely as possible, Dr. Leigh Sowerby, Associate Professor at Schulich Medicine & Dentistry and Associate Scientist at Lawson, will be investigating whether or not the virus that causes COVID-19 can be transmitted in surgical smoke. Surgical smoke is the aerosol produced by an essential surgical tool called electrocautery.
“Electrocautery is a ubiquitous tool for surgery, and is known to generate aerosol and smoke. We do not know if the SARS-CoV-2 virus can be transmitted in this plume, and this is important to answer for all surgeons, but in particular, for surgeons working in the respiratory and aerodigestive tract,” said Dr. Sowerby, who is also a head and neck surgeon at London Health Sciences Centre and St. Joseph’s Health Care London. “CIHR funding will allow us to rapidly execute this project. Without this funding, the project would not be possible.”
Dr. Sowerby says the results from this study, whether positive or negative, will have important implications. If positive, it will have a critical and direct impact on ensuring the safety of health care workers performing procedures on patients. Procedures using cautery will continue to require high level protection if the COVID-19 status of the patient is unknown. If negative, it will allow these surgical procedures to continue safely and effectively while conserving critical protective equipment for cases that need it.
The family physician’s role in pandemic plans
Maria Mathews, PhD, Associate Professor at Schulich Medicine & Dentistry, is investigating how the role of family physicians can be better incorporated into pandemic plans. Family physicians play important roles during a pandemic, from detecting potential outbreaks and screening and testing patients to providing care to infected patients and contributing to surge capacity in hospitals.
“During the early stages of the COVID-19 pandemic, family physicians had concerns about roles they were asked to fill for a variety of reasons, including the lack of appropriate personal protective equipment, availability of tests, and concerns about infection risks to other patients and staff in a family practice clinic,” said Mathews.
Mathews will examine the experiences in four regions in Canada – Newfoundland and Labrador, Nova Scotia, Ontario and British Columbia – to identify key roles, supports and best practices. The results will provide government ministries, public health units, and other health organizations with evidence and tools in order to incorporate family physicians in the response to a potential second COVID-19 wave and plan for future pandemics.
Could cannabis consumption during pregnancy lead to type 2 diabetes in adulthood?
The legalization of cannabis in Canada in October 2018 created an important concern for the health of mothers and babies during pregnancy and beyond. Studies from 2002 – 2014 indicate that one in five pregnant women between the ages of 18 and 25 use cannabis, as the perception is common that it will reduce anxiety and pregnancy-induced nausea.
Although there is a large body of evidence detailing the mode of action of the main component of cannabis (Δ9-tetrahydrocannabinol (THC)) in adults, little research has focused on understanding how it may impact development of the fetus. This is a critical knowledge gap considering that fetal growth deficits are accompanied with an increased risk of developing chronic metabolic disease later in life.

Dr. Edith Arany, Scientist at Lawson, is studying the implications of cannabis use during pregnancy on the offspring’s pancreas development “in utero” and its effects on glucose control in adulthood.
With the increased epidemic of Type 2 diabetes due to environmental factors, her research in cannabis consumption might bring to light another contributor to this burden.
Dr. Arany’s study is being funded through Lawson’s Internal Research Fund (IRF).
“I’m extremely grateful for this IRF award as it will help me open up a new direction in my research program.” Dr. Arany states. “These IRF grants are crucial to basic scientists to get preliminary data to support future grant applications. Without this support, it is difficult to test novel directions of research and to maintain research programs.”
Lawson’s IRF is designed to provide Lawson scientists the opportunity to obtain start-up funds for new projects with the potential to obtain larger funding, be published in a high-impact journal, or provide a clinical benefit to patients. Funding is provided by the clinical departments of London Health Sciences Centre and St. Joseph’s Health Care London, as well as the hospital foundations (London Health Sciences Foundation and St. Joseph’s Health Care Foundation).
Differences in walking patterns could predict type of cognitive decline in older adults
Canadian researchers are the first to study how patterns in the way older adults walk could more accurately diagnose different types of dementia and identify Alzheimer’s disease.
A new study by a Canadian research team, led by London researchers from Lawson Health Research Institute and Western University, evaluated the walking patterns and brain function of 500 participants currently enrolled in clinical trials. Their findings are published in Alzheimer's & Dementia: The Journal of the Alzheimer's Association.

Dr. Montero-Odasso is world renowned for his research on the relationship between mobility and cognitive decline in aging. Leading the Mobility, Exercise and Cognition (MEC) team in London, he is pioneering novel diagnostic approaches and treatments to prevent and combat early dementia. Dr. Montero-Odasso is also co-lead of the Mobility, Exercise and Cognition Team at CCNA, a team composed of 22 researchers and 6 trainees.
This study compared gait impairments across the cognitive spectrum, including people with Subjective Cognitive Impairment, Parkinson’s Disease, Mild Cognitive Impairment, Alzheimer’s disease, Lewy body dementia and Frontotemporal dementia, as well as cognitively healthy controls. The study used data from the COMPASS-ND Cohort and the Gait and Brain Study Cohort.

Gait assessment looks at the way in which we move our whole body from one point to another, helping to analyze mobility and the brain processes involved.
Four independent gait patterns were identified: rhythm, pace, variability and postural control. Only high gait variability was associated with lower cognitive performance and it identified Alzheimer’s disease with 70 per cent accuracy. Gait variability means the stride-to-stride fluctuations in distance and timing that happen when we walk.
“This is the first strong evidence showing that gait variability is an important marker for processes happening in areas of the brain that are linked to both cognitive impairment and motor control,” notes Dr. Frederico Perruccini-Faria, Research Assistant at Lawson and Postdoctoral Associate at Western’s Schulich School of Medicine & Dentistry, who is first author on the paper.
“We’ve shown that high gait variability as a marker of this cognitive-cortical dysfunction can reliably identify Alzheimer’s disease compared to other neurodegenerative disorders.”
When cognitive-cortical dysfunction is happening, the person’s ability to perform multiple tasks at the same time is impacted, such as talking while walking or chopping vegetables while chatting with family.
“Having gait variability as a motor marker for cognitive decline and different types of conditions could allow for gait assessment to be used as a clinical test, for example having patients use wearable technology,” says Dr. Richard Camicioli, Professor at the University of Alberta and co-senior author on the paper.
The London team collaborated with researchers at the University of Toronto, University of Calgary and University of Alberta. They are part of the Canadian Consortium on Neurodegeneration of Aging (CCNA), a collaborative research program tackling the challenge of dementia and other neurodegenerative illnesses.
Dr. Montero-Odasso adds that this gait variability could be perceived as similar to an arrhythmia. Health care providers could potentially measure it in clinical settings, like how heart rhythm is assessed with electrocardiograms.
This study was primarily funded by CCNA, supported by a grant from the Canadian Institutes of Health Research.
Discovery shows promise for treatment of glaucoma
In a new study from Lawson Health Research Institute (Lawson), scientists have discovered that a specific protein has the potential to be used to treat some patients with primary open-angle glaucoma.
Primary open-angle glaucoma is the most common type of glaucoma, which is a group of diseases that affect nearly 70 million people worldwide. Glaucoma is characterized by progressive damage to the optic nerve which ultimately leads to blindness. In this new study, led by Dr. Sunil Parapuram, researchers examined the role of a protein called “phosphatase and tensin homolog” (PTEN) in the trabecular meshwork. The trabecular meshwork is a porous tissue in the eye through which the clear fluid that fills the eye drains out.
In some primary open-angle glaucoma patients, the structure of the trabecular meshwork is damaged by fibrosis. Fibrosis is a thickening or scarring of tissue which is caused by an excess amount of matrix molecules such as collagen. Fibrosis of the trabecular meshwork prevents the fluid in the eye from draining out normally, which leads to increased pressure in the eye and damage to the optic nerve.
Dr. Parapuram’s team found that the inactivation of the protein PTEN can cause too many matrix molecules to be deposited in the trabecular meshwork, leading to fibrosis. On the other hand, when PTEN activity was increased, it reduced the amount of matrix molecules being deposited in the trabecular meshwork. These results indicate that drugs that can activate PTEN have high potential to be used as a treatment for open-angle glaucoma.
“There’s an immediate need for a new generation of therapeutic drugs for more effective treatment of glaucoma,” says Dr. Parapuram, a Lawson scientist at St. Joseph’s Health Care London and an assistant professor in the Departments of Ophthalmology and Pathology at the Schulich School of Medicine & Dentistry, Western University. “While further research is needed, drugs that activate PTEN could be the answer.”
Dr. Parapuram’s team will continue to study the function of PTEN in the trabecular meshwork in more detail and test the role of drugs that activate the protein as a potential treatment for primary open angle glaucoma.

Dr. Michael Motolko (left), Chair/Chief, Department of Ophthalmology, and Dr. Sunil Parapuram (right).
“This study highlights the expansion of our department’s research activities into basic science application and its findings are relevant to many other fibrotic diseases,” says Dr. Michael Motolko, Chair/Chief, Department of Ophthalmology, Schulich School of Medicine & Dentistry,Western University, London Health Sciences Centre and St. Joseph’s Health Care London.
The study, “TGF-β induces phosphorylation of phosphatase and tensin homolog: implications for fibrosis of the trabecular meshwork tissue in glaucoma,” is published in Nature’s Scientific Reports.
Expanded No Fixed Address strategy houses half of those in danger of homelessness
At a community symposium on health care and homelessness attended by over 250 Londoners, a research team from Lawson Health Research Institute announced the results of a nine-month, federally funded project tackling the issue of homelessness from within hospital walls.
The No Fixed Address (NFA) strategy reaches and supports patients during the crucial transitional period when they are being discharged from the hospital and re-integrated into the community. The approach was initially tested with strong success for mental health patients across the city and the second ‘version’ of the project was extended to medical units at London Health Sciences Centre’s University Hospital and Victoria Hospital.

“Many of our patients with lived experience of homelessness were saying that their journey started with a hospital discharge,” explains Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson and NFA project lead. “They were often experiencing major transitions in their lives and then experienced a hospital stay. Normally a relatively short visit, they aren’t able to gather the information and make a plan to be able to leave the hospital with somewhere to stay.”
Through partnerships between service providers and non-profit organizations, the NFA strategy helps prevent homelessness by providing timely and accessible supports to patients who would otherwise be discharged into homelessness. Staff from the Canadian Mental Health Association Middlesex, Salvation Army’s Housing Stability Bank, and Ontario Works in the City of London provided direct, on-site patient access to housing and income support databases
“Lawson’s No Fixed Address research project is the first evaluation anywhere of a strategy that aims to reduce the number of hospital patients being discharged into homelessness,” says Dr. Forchuk.
Over nine months, 74 people experiencing medical health issues accessed the NFA program. Of those, 54 per cent were also experiencing mental health challenges.
All of the study participants were in imminent danger of homelessness. Through the supports provided as part of this research study, half were able to arrange housing before being discharged.
“We were able to help a lot of people, with 50 per cent successfully securing housing,” shares Dr. Forchuk. “With the results and feedback we received, we learned a lot about how we can make the program even better.”
They found that there is a need for the supports to be extended as a transitional program in the community post-discharge, as the length of stay in the medical units tended to be short.
The project’s previous phase, involving acute and tertiary psychiatric care in the London region, prevented homelessness in 95 per cent of cases. “Going into the medical units, we found that people have highly complex needs that often involved mental health challenges.
By simply using the same approach that we did for those in psychiatric care, we helped half of the people find housing. To best serve the needs of everyone, we want to follow them after discharge.”
The team sees a solution in having a housing support worker provide transitional, wrap-around services that follow the person. They would continue to meet and work together after the hospital stay, helping to access community programs.
“This role would be embedded in both the health care system and the homeless serving system, supporting individuals who have complex physical and mental health issues as they are also navigating homeless resources.”
This project is funded by the Government of Canada's Homelessness Partnering Strategy’s (HPS) Innovative Solutions to Homelessness funding stream.
Overview and Numbers
Fast facts on homelessness and health care
- Stable housing after discharge is associated with higher quality of life, reduced substance abuse and fewer hospital admissions.
- Homeless clients are four times more likely to be readmitted to hospital within a month compared to low-income matched controls.
- Hospital care for homeless clients costs an average of $2,559 more per client.
- Finding appropriate housing or avoiding a potential eviction takes time – it is important to start as soon as possible during the discharge process.
Implementation of first phases of No Fixed Address
- Access on the unit to a housing advocate and income support staff.
- The initial intervention was accessed by 219 acute psychiatric clients, as well as 32 clients within a specialized tertiary care psychiatric hospital - only 3 became or remained homeless.
- Expanded to be an immediate wrap-around service with offices set up in the hospital mental health units.
- Staff from the Canadian Mental Health Association Middlesex (CMHA), Ontario Works (OW), and Salvation Army’s Housing Stability Bank (HSB) have on-site access to housing and income support databases.
- Clients can access service by drop-in or appointment.
- Services include assistance for finding housing, financial assistance, such as rent/utilities in arrears or first/last months’ rent for a new home, and access to high quality used furnishings, household supplies and a cleaning service.
Expanded second phase of No Fixed Address
- Program ran from July 2018 to March 2019 (9 months).
- 74 people accessed the program.
- Complex situations with both mental health and physical problems: 100% had medical issues and 54% had mental health issues.
- Lengths of stay were very short.
- People could not attend drop-in due to medical issues, so they relied on referral from staff.
- Although they were all in imminent danger of homelessness, 38 people (50%) were housed as a result of this program.

What were the main housing needs?
- Help finding a place to live
- Money for deposit
- Financial support
- Transportation support
- Help getting benefits
Recommendations and learnings for future models
- Housing support worker needs to be a transitional support since work will be needed after discharge.
- Social work not the only key players (patient care facilitators, nursing staff, etc.).
- The transitional housing support role needs to be well embedded in the homeless serving system, as well as health care.
- People have physical and mental health issues and are also going to be navigating homeless resources.
- Despite the low success rate, many people were housed who would have otherwise been discharged to homelessness.
- We learned a lot about what was needed in an area where there was a knowledge vacuum.
- Future plans involve implementation with improvements to the model.


