Search
Search
New study shows technology could play an important role in mental health support
In a study published in MDPI Journal, a team of researchers at Lawson Health Research Institute have shown that the use of technology may assist in better outcomes for those living with both mental health and physical disorders.
Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson, and her team embarked on a pilot study that used smart home monitoring solutions to assist those living with both a mental health disorder and other health challenges. The purpose of this pilot study was to see if technology could improve overall lifestyle and wellbeing.
“We began our research by using hospital prototype apartments – apartment style care spaces within hospital settings – that were equipped with smart home technology solutions such as a screen device, activity trackers, weigh scales and medication dispensers,” says Dr. Forchuk who is also the Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery at St. Joseph’s Health care London. “Once we tested it in a hospital setting, we wanted to find a way to take this idea out into the community in different kinds of housing and living situations to see if it would be beneficial.”
The research team partnered with the Canadian Mental Health Association (CMHA) and the London and Middlesex Community Housing (LMCH) to work together to retrofit the homes of the 13 study participants.
“We worked together with the participants and their care providers to choose what combination of technology they felt would be best for them,” says Dr. Forchuk. “No matter their health condition each participant wanted to be more active and independent, with the goal of staying out of hospital.”
All smart devices were connected to the Lawson Integrated Database, which is a database that can securely collect data from multiple sources such as health devices. This allowed care providers to send reminders to participants, while also tracking usage and results.
“The key benefits we noted was that study participants started to live healthier lives,” says Jonathan Serrato, Lawson Research Associate. “Participants logged going for walks and exercising more often, as well as making healthier food choices. Those who used the medication dispensers did not miss a single dose. The touch screen devices also allowed participants to easily communicate with care providers and support networks, and access more resources.”
Following the pilot study, the research team also published a subsequent paper, as a ‘how-to guide’ for utilizing smart home technology interventions as a health care tool.
“This paper is a helpful resource that outlines implications and considerations when it comes to smart home technologies,” adds Serrato. “There are many areas we touch upon such as security, privacy and feasibility as well as hardware and software information for those who would like to take on their own similar type of smart home technology project.”
A vision for the future of ICES Western: Q&A with Dr. Kristin Clemens
Dr. Kristin Clemens has been selected as the new Site Director for ICES Western, the London, Ontario division of a province-wide non-profit focused on using health-related data to evaluate outcomes. ICES Western is a collaborative initiative between Lawson Health Research Institute, Western University, London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London.
Dr. Clemens is a Scientist at Lawson and an Endocrinologist at St. Joseph’s. She is also an Assistant Professor in epidemiology and biostatistics at Western’s Schulich School of Medicine & Dentistry. Dr. Clemens recently sat down to discuss the impact of the work being done through ICES Western and her hopes for the future.

1. What are you most excited for as ICES Western’s new site director?
I get to continue to work closely with an amazing group of ICES Western staff and scientists. ICES Western is already a well-oiled machine and home to scientific hubs of research in neurological health, homelessness and socioeconomic disparities, surgery, mental health, kidney disease and more. As a leader, I will not only be able to help harness some of our existing strengths, but have a chance to continue to move our institution forward. For example, Dr. Amit Garg (outgoing Site Director) will be advancing new and innovative randomized controlled trials in London, and ICES Western's going to continue to play a major role in that. There is so much more potential for innovation using our data sources; I think it's going to be a really exciting next few years for us.
2. Why did you choose to become involved with ICES Western?
I have been with ICES for about 14 years. I have lived it as an ICES trainee as a Medical Student and Resident/Fellow and became an ICES Adjunct Scientist after completing the inaugural ICES Faculty Scholars program hosted by ICES Western. I became more and more engaged with the community as a member of local ICES committees and then started to lead some of the larger research programs at ICES Western. It was the perfect time and really a natural fit for me to embark on a new leadership journey with the institution.
3. What do you hope to bring to your new position?
I'm an enabling and collaborative researcher and have been fortunate to work with multidisciplinary teams of scientists from across Western and Lawson. What I hope to do is not only support existing ICES staff, scientists, and initiatives, but also attract new researchers to the institution. I think London, Ontario, is such an incredible city for academia. I really want to use my collaborative skills and strong relationships to try to grow and expand our reach.
4. Has the work at ICES played a role in your research?
Yes, absolutely. My clinical and research focus has been on improving the care and outcomes of patients who live with complex comorbidities and disparities. ICES research allows us to focus on real-world gaps in care in Ontario and it gives us an opportunity to study people and patients who have not been able to participate in randomized trials or traditional research studies.
5. What impact does the work at ICES have on research being done in Ontario and across Canada?
ICES is home to one of the world's largest collections of administrative data sets that contain everything from hospital visits and physician encounters to use of medications and long-term care. We also have the unique ability to link data from national surveys or existing cohorts with administrative data. Because of this, ICES is very much at the forefront of improving care and quality for all Ontarians. Our research is shared internationally with both academics and non-academics, and it has changed practice and policy; it's an extremely impactful organization.
6. What do you see in the future for the organization?
I think in the future we will continue to do what we're already great at, like studying the use of health services and existing hubs of research, but also find ways to use our rich data sources, methods and talented staff to really innovate and advance research in London. With new collaborations in the city, we can also continue to grow and contribute.
7. What is the most important thing people should know about ICES?
ICES Western is here for London’s community of researchers, health care providers and decision makers. We have more than 20 scientists and dozens of highly qualified staff who are passionate about advancing high-quality, impactful work. ICES Western is a valuable resource for the community.
Assessing neurofeedback in stroke survivors
Researchers are testing whether a specialized form of imaging can help in stroke rehab.
A new study aims to assess the use of functional near-infrared spectroscopy (fNIRS), a type of imaging, to provide neurofeedback during stroke rehabilitation with a goal of eventually improving patient outcomes.
fNIRS is used to detect changes in brain oxygen levels using light. More recently it has also been used to develop brain-computer interfaces (BCIs), which allow patients with brain injuries to control devices like robotic arms with their thoughts.
Dr. Sue Peters, a Scientist at Lawson Health Research Institute and Director of the Neurorehabilitation Physiology Lab at St. Joseph Health Care London’s Parkwood Institute, was one of the recipients of the Spring 2022 Lawson Internal Research Fund (IRF) Awards.
The funds will go towards a new study to assess whether fNIRS can be used to direct neurofeedback in stroke survivors – helping them with rehabilitation.
“Currently, there's no real measure of brain activity that is used in stroke rehabilitation to help make clinical decisions,” says Dr. Peters, who is also a Professor at Western University.

Over 400,000 Canadians live with the effects of a stroke, according to the Heart and Stroke Foundation, and there’s hope that fNIRS could make a big difference by eventually improving movement and independence.
“We're going to use the device in some common tasks that people might do with their arm and determine whether we can use this device reliably and accurately in a stroke-related context,” Dr. Peters explains.
Participants in the study will imagine moving while remaining still. This activates very similar parts of the brain to when people actually move. If done correctly, patients will see a visual cue generated through measurement using fNIRS.
“We know from MRI studies that when I move my right hand, the left side of my brain is activated,” notes Dr. Peters. “We think we can use this concept in stroke rehab.”
Dr. Peters is recruiting 40 people from the community who are at least six months post stroke and 40 healthy adults of all ages. They will first participate in motor assessment with a physiotherapist and then wear an fNIRS cap while thinking about moving their wrist to measure brain activity.
Previously, there were a lack of methods to image the brain during real-life movement.
“The hope is to eventually conduct a clinical trial where we're testing motor interventions to see whether some things are more effective than others at activating the regions of the brain that were impacted by the stroke.”
Dr. Peters believes the study has the potential to have a big impact on the future of rehabilitation for stroke patients, leading to lasting changes in quality of life.
Capturing bacteria’s grand ballet
In a world first, scientists at Lawson Research Institute are leveraging imaging technology to see and track microbes and provide an unprecedented glimpse of the human microbiome.
Within each of us is a world populated by a bustling metropolis of microorganisms – a tapestry of trillions in a delicate dance to balance health, well-being and vitality.
Far outnumbering human cells, this dynamic ecosystem of busy bacteria, industrious fungi and elusive viruses is the body’s microbiome. This invisible hive of ceaseless activity is so intrinsic to human health, its explorers say it should perhaps be considered an organ in its own right.
Now, in a world first, Lawson Health Research scientists studying this microcosmic underworld are making the invisible visible – in real time.
The team of Jeremy Burton, PhD, Research Chair of Human Microbiome and Probiotics and Director of the Canadian Centre for Human Microbiome and Probiotic Research at St. Joseph’s Health Care London (St. Joseph’s), is using imaging technology to see and track microbes, providing a perspective never before achieved.
“Typically, we track microbes by analyzing samples from patients after treatment to improve their gut health with probiotics or microbiota transplantation (FMT),” explains Burton, whose endowed research chair is funded through St. Joseph’s Health Care Foundation. “While we can get detailed information through DNA sequencing techniques, this often takes many months and relies on collecting fecal samples and other samples that may not be easily obtained. It also doesn’t provide all the information we need, like exactly where the microbes have travelled and how long they live.”
'Fantastic insight'
Imaging the microbes allows the Lawson team “to see things in real-time and not worry about clinical samples,” he adds.
Donna Goldhawk, PhD, molecular imaging scientist with Lawson’s Imaging Research Program, explains that imaging is done by attaching a radioactive tracer to cells, such as bacteria, that can be ingested and visualized in the body with positron emission tomography-magnetic resonance imaging (PET/MRI).
Imagine it as a biological version of an AirTag that tracks specific microbes.
“Lawson's environment has been a catalyst for new ideas, collaborations and many Canadian firsts.” - Michael Kovacs, Program Lead, Lawson’s Imaging Research Program, and Lead, Cyclotron & PET Radiochemistry Facility
“It’s through this pipeline that we gain fantastic insight into how the microbiome supports human health,” she says.
As an example, tracking microbes allows the scientists to see if they are close to or crossing over the gut cell wall.
“This is critical information because the proximity of microbes to the cell wall will likely determine if the probiotic or FMT therapy is effective or not,” says Burton. “We can now potentially track microbes that we administer to people in real-time and, in the future, be able to tell how sick people are and if they have a dysfunctional microbiota. Eventually, this information will be linked to their other health information for a complete picture.”
Uniquely St. Joseph’s
He notes the work “could only happen here” at St. Joseph’s, with its leading-edge imaging, production of novel tracers (isotopes) within Lawson’s Cyclotron & PET Radiochemistry Facility, and with world-class collaborative expertise – all fueled by the generosity of donors.
Working with Burton and Goldhawk are Lawson scientists, Michael Kovacs, PhD, Frank Prato, PhD, Dr. Michael Silverman, Seema Nair Parvathy, PhD, and Neil Gelman, PhD.
“This exciting work illustrates how innovative technologies can emerge when diverse groups collaborate closely in a multi-disciplinary approach to research within a hospital setting,” says Michael Kovacs, Program Lead, Lawson’s Imaging Research Program, and Lead, Cyclotron & PET Radiochemistry Facility. “Lawson's environment has been a catalyst for new ideas, collaborations and many Canadian firsts.”
The potential impact cannot be over-stated, adds Burton.
“This is the pathway to revolutionizing the way we understand the microbiome in people,” he says. “We’ve spent so long trying to eradicate microbes and studying the ones that cause ill health. Only relatively recently have we begun to study the ones that cause good health. That’s a dramatic shift in approach and, while we’ve come a long way, we’re really only getting started.”
Celebrating Clinical Trials Day
Clinical trials are the gold standard in medical research, used to test new treatments and medical devices to ensure they are safe and improve patient outcomes.
Each year on May 20, Clinical Trials Day aims to raise awareness about the importance of clinical trials. At Lawson Health Research Institute, our researchers, research staff and learners across London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London (St. Joseph’s) are working daily to advance clinical trials for some of the most pressing health challenges.
“If you look at many areas of medicine, like cancer and cardiovascular disease, part of why those conditions have had dramatic improvements in outcomes over the last several decades is because of clinical trials,” says Dr. Amit Garg, Scientist at Lawson, Lead for the Kidney, Dialysis & Transplantation Research Program at ICES Western, and a Nephrologist at LHSC.
Clinical trials can also provide patient participants with new treatment options and can demonstrate when existing treatments have applications for other diseases.
“We could not conduct clinical trials without patients participating in them,” adds Dr. David Palma, Associate Scientist at Lawson and Radiation Oncologist at LHSC. “A clinical trial is a very rigorous process where we carefully define a treatment and follow patients very closely with extra interventions and tests to see not only how the disease is responding to treatment, but also any effects on a patient’s quality of life.”
It also takes a team to make clinical trials a success, including the critical work of research coordinators, associates and assistants, adds Dr. Swati Mehta, Lawson Scientist based at St. Joseph’s Parkwood Institute.
Dr. Palma also notes that while clinical trials require investment to conduct them, they can ultimately lead to savings in the health system.
“While the primary goal of a clinical trial is to improve or save lives, they often lead to cost savings down the road. Improving cure rates means people don’t need as much treatment and that can save the initial investment many, many times over,” Palma says.
Looking ahead, work is ongoing to make clinical trials more efficient and equitable.
“Eliminating specialized infrastructure would help make trials more equitable, so they are available in smaller communities and at distant sites that otherwise would not have access. Making study materials available in multiple languages and to anyone with accessibility issues can also help,” Garg adds.
“Future clinical trials will need to follow more pragmatic, adaptive study designs that allow us to evaluate therapies or interventions in a more realistic setting,” Dr. Mehta says. “These would also allow us to follow-up with patients that were potentially underrepresented in past research.”
According to researchers at Lawson, the future of clinical trials is bright with hundreds of trials currently underway at LHSC and St. Joseph’s with the goal of improving patient outcomes.
Celebrating health research excellence with the 2023 Lawson Impact Awards
For the first time since 2019, Lawson Health Research Institute hosted its annual Lawson Impact Awards in-person on November 28 at RBC Place London. Approximately 130 people gathered to celebrate scientists, staff members, learners and partners who have made remarkable contributions to hospital-based research at London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London (St. Joseph’s).
“Important and groundbreaking science is conducted daily at Lawson, improving patient care locally and around the globe,” says Dr. David Hill, Scientific Director at Lawson. “The Lawson Impact Awards provides an opportunity for us to recognize the scientists, staff members, learners and partners who drive medical research forward.”

Eight Lawson Impact Award recipients were celebrated at the event, including:
- Leadership Award for Fellows & Students: Dr. John Tran
- Staff Award of Excellence: Alexandria Roa Agudelo
- Community Partner of the Year Award: Keith and Leanne Lavergne
- Community Partner of the Year Award: Jack and Jean Wettlaufer Family
- Community Partner of the Year Award: Ryan Finch
- Dr. Joseph Gilbert Research Contribution of The Year Award: Dr. David Palma for “Stereotactic ablative radiotherapy versus standard of care palliative treatment in patients with oligometastatic cancers (SABR-COMET): a randomised, phase 2, open-label trial”
- Innovation Award: Dr. Manuel Montero-Odasso
- Scientist of The Year Award: Dr. Cheryl Forchuk
Two Children’s Health Research Institute (CHRI) award recipients were also recognized. As a program of Lawson, CHRI awards a Scientist and Trainee of the Year annually, sponsored by the Children’s Health Foundation. CHRI’s 2022 award recipients are: Dr. Emma Duerden (CHRI Scientist of the Year) and Kendrick Lee (CHRI Deb Comuzzi Trainee of the Year).
“This year, we recognized a number of leading research professionals from across LHSC and St. Joseph’s who are helping to advance patient care in London and around the world,” adds Dr. Hill. “We were also honoured to recognize three Community Partners of the Year for their generous support of health research.”
Learn more about each recipient on our Impact Awards page and visit the Lawson YouTube channel to watch videos highlighting each of the award recipients.
Celebrating International Women’s Day
To mark International Women’s Day, two early career researchers at Lawson Health Research Institute are sharing their experiences as women in STEM (science, technology, engineering and math). They shared the support they’ve experienced in their careers, the importance of women’s voices in medical research and how to encourage more women to pursue careers in STEM.
Early access and mentorship are key: Dr. Funmbi Babalola
Dr. Babalola is a Paediatric Endocrinologist at Children’s Hospital at London Health Sciences Centre (LHSC) and an Associate Scientist at Lawson Health Research Institute. She helped pioneer the start of a Paediatric Rare Bone Disease Clinic at Children’s Hospital in 2022 which provides multi-disciplinary care for patients, so they no longer have to travel outside of London for treatment. As a clinician researcher, her areas of interest are paediatric diabetes and calcium and bone metabolism disorders. She is currently involved in several clinical trials and studies.
She credits mentorship and the support of educators early in her career journey with encouraging her interest in science and says that is key for being more welcoming to women in STEM.
“In Grade 12 my biology teacher recommended I go to an advanced placement school. That was when I had my first experience with research,” says Dr. Babalola. “When I got to my undergraduate work, I found a woman mentor who was a powerhouse and had a vision, and I was able to publish two papers during that time and had such a positive experience. I went straight to medical school after that and continued to do research. I think I’ve been really lucky with all the people that I’ve worked with and who have encouraged me as I built my research career.”
Dr. Babalola says she is fortunate to be a researcher in a time when women’s voices are finally being heard and welcomed.
“I think my perspective is probably different than women who were starting work 10 or 20 years ago,” she notes. “I think I’m very lucky that I entered the medical research world where a lot of women are at the table. They’re great role models and they really support and help each other.”
But she says support for research in hospitals is also crucial.
“It takes both good mentors and a culture of research to make it easier to get studies done.”
Dr. Babalola has already started mentoring new researchers, many of them women, who have approached her.
“I’m all about paying it forward. I’ve been super fortunate to have great mentors that are still continuing to mentor me, so I want to pass that knowledge on.”

Women in science are inspirational: Dr. Kait Al
Dr. Kait Al is a Postdoctoral Research Fellow at Western University’s Schulich School of Medicine & Dentistry, working in a Lawson Health Research Institute lab at St. Joseph’s Health Care London. Dr. Al’s research focus is the role of the microbiome in urological conditions like kidney stone disease. She’s currently looking at how a microbiome with beneficial microbes could help protect healthy individuals from forming kidney stones and how optimizing the microbiome could help prevent stone recurrence in stone formers.
She believes women’s voices need to be included in research so that it is more representative of the world we live in and better addresses everyone’s health needs.
“Women bring diverse experiences and perspectives that have been historically excluded from research, along with many other underrepresented groups.”
And mentors among those voices are one of the best ways to encourage more women to get interested in science, she says, so women can see themselves in those positions.
“Seeing someone like yourself as a role model in a successful position that is passionate and curious about science can be so influential to young people,” shares Dr. Al. “As scientists, it’s important to share your work widely.”
She notes that organizations that encourage and support mentorship, as well as a flexible work culture and networking opportunities, are likely to be more welcoming to women in STEM and benefit from having them as part of the team.
“It is crucial to prioritize an inclusive and supportive mentorship environment for trainees and professionals,” says Dr. Al. “I believe work that lets you balance professional and personal commitments, which can otherwise be biased against women, is key.”
The theme for International Women’s Day in 2024 is ‘Inspire Inclusion,’ and that’s exactly what Dr. Al says she sees in other women in science.
“I am constantly inspired by women in science, from my direct colleagues to world leaders I’ve never met. I have witnessed firsthand my colleagues breaking down barriers, succeeding in challenging areas, and lifting each other up, and it really creates a culture of empowerment.”
Changing our MINDS
Local youth use art and storytelling to illustrate the personal and system challenges in mental health.
The words and images are both heartbreaking and hopeful.
“Nobody likes you if you are sad.”
you are enough. stay strong. let life surprise you.
“Please don’t leave like everyone else.”
1 year sober. 1 year of school. 1 year building a safe home. 1 year loving myself.
Zine-writing, a personal and introspective medium often used by people who have been marginalized, is an important part of local research that is finding solutions to complex mental health challenges among young adults. Its name derives from its magazine (“zine”) format.
“When we make the voices of people with lived experience central to our research, we can learn from each other and then change the system together,” says Dr. Arlene MacDougall, founder of MINDS of London-Middlesex.
The social innovation and research lab based at St. Joseph’s Health Care London (St. Joseph’s) is dedicated to designing, piloting and testing mental health innovations for teens and young adults. Its recent evolution into MINDS 2.0 adds insights by and for people up to age 35 who have complex, pervasive mental health and addiction issues.
Learning from experts
Rin, a London artist, who has published independent zines for a decade, created three for this project, including one that, with irony, asks the reader to ponder which vulnerable people aren’t worth saving.
“I believe making art can be very healing,” says Rin. “I wanted to share some of my story to help myself and help others. I want to play a part in shaping a mental health system that’s better than the one I encountered.”
The zines weave art, prose and poetry into story:
3 things I would change: affordability, stigma, waitlists.
“If I had a magic wand, I would use it to heal the waters, grow the trees, foster animal growth.”
Look in the mirror, see how far you’ve come.
They also raise and propose solutions to troubling issues among people with mental illness: housing and homelessness, sparse resources for people with addictions, lack of coordination among service providers, and dehumanizing attitudes in health and criminal justice systems.
“Participants experienced catharsis just in telling their stories,” says Renee Hunt PhD, Associate Director of Research and Operations at MINDS. “And because they’re the experts, they’re also playing an important part in changing systems that need an overhaul.”
Adds Rin, “It feels empowering knowing people are listening to us – people who care and are committed to making change to the system.”
MacDougall notes the pivotal role of St. Joseph’s Health Care Foundation – in particular, a groundbreaking $5-million donation towards mental health research from philanthropist Ryan Finch – in advancing mental health innovation through MINDS and MINDS 2.0.
“They’ve been our biggest supporters since day one. This wouldn’t have happened without support from Ryan and the foundation and all the many donors who believe in mental health research,” says MacDougall, who is also Director of Research and Innovation with St. Joseph’s Mental Health Care Program.
“MINDS has been a catalyst for system change,” MacDougall adds. “Research is always about finding answers and generating impact.”
Many findings from MINDS research have been put into practice, among them are the creation of guidebooks for peer support, free taxi service for rural youth needing urban mental health or addiction services, and educational resources to support 2SLGBTQI+ students.
MacDougall says MINDS 2.0 expands that work with new voices and the exploration of more in-depth solutions.
What’s next for MINDS 2.0
- Workshopping ideas and prototypes for mental health systems change. Sessions will be held where people with lived/living experience and service providers propose and develop potential solutions.
- Leadership-building. Twenty mental health practitioners will be trained to become “agents of change” who will collectively create, implement and evaluate mental health programs, technology, interventions and training.
- Imaginarium conference. In 2025, a first-of-its-kind national conference will take place to share system innovations in mental health and addiction.
Could online programming reduce barriers for those with mobility impairments?
LONDON, ON – A new study at Lawson Health Research Institute will offer online exercise and behavioral intervention for adults who are mobility impaired. The goal is to reduce barriers to accessing activity programs.
“Many people with mobility concerns experience barriers to physical activity, such as fear of falling because of their past injuries,” says Dr. Swati Mehta, Lawson Scientist. “This project aims to help them cope and learn skills to continually, actively engage in physical activity.”
The 10-week virtual program is being coordinated through St. Joseph’s Health Care London’s Parkwood Institute. It will consist of weekly personal behavioral coaching. Participants will also be asked to complete two or three group physical activity programs each week, such as seated aerobics, seated boxercise and seated yoga.

“This study is really exciting because it brings together both behavioral coaching and physical activity classes, which are normally offered separately,” explains Dr. Dalton Wolfe, Lawson Scientist. “This provides extra support to help those with mobility impairments overcome barriers to maintaining an active lifestyle.”

Those barriers can include things like fatigue and transportation challenges that often accompany neurological conditions like multiple sclerosis, spinal cord injury, brain injury and stroke.
“Ultimately this study is about enhancing quality of life and wellbeing while improving participants’ ability to engage in the community,” says Dr. Wolfe.
The research team is currently recruiting 20 participants for the study. For more information on the study you can email @email.
Cutting Edge: Surgical advancement through research
Before the bright lights of the operating room are turned on and the surgeons and operating room staff are gowned and ready, research conducted at Lawson Health Research Institute has backed many of the surgical innovations and firsts performed at London Health Sciences Centre and St. Joseph’s Health Care London.
On October 5, Lawson hosted a Café Scientifique event where a panel of surgeons who are also Lawson scientists discussed their cutting-edge work. Guests had the opportunity to ask questions as part of an open-forum discussion to gain insights from the speakers, and from one another.
In celebration of Canada’s 150th anniversary as a nation, this event was the second of a two-part series focusing on the future vision for health care in Canada and the legacy that research at Lawson will leave. Research and knowledge-creation have been a hallmark of the various surgical areas at LHSC and St. Joseph’s since their inception, and the relationship between innovation and improving patient care has been an enduring trademark. Surgeon scientists have conducted and published research that has changed clinical practice worldwide.
Hand surgery: How small advances turn into complex surgical achievements
Dr. Bing Siang Gan, Lawson scientist, plastic surgeon, Hand and Upper Limb Centre, St. Joseph's

Dr. Gan has a particular research interest in the biology and treatment of Dupuytren's contracture and he uses conventional as well as minimal invasive procedures such as needle aponeurotomy and new collagenase enzyme injections to treat patients.
Dr. Gan explained how a better surgical understanding of Dupuytren's contracture combined with an understanding of the underlying gene factors, DNA, RNA, proteins, receptors, and collagen formation of the condition has led to pharmacological treatment options. The next step will be developing treatment options at every stage of Dupuytren's contracture to keep patients away from the operating room.
Transplant organ preservation: The best option may be “Stinky”
Dr. Alp Sener, Lawson scientist, transplant surgeon, Multi-organ Transplant Program, LHSC

Dr. Sener maintains an active basic sciences and translational research laboratory focusing on gasotransmitter biology and therapeutics. Dr. Sener discussed the need to use “marginal” deceased donor kidneys - those from older donors, younger donors with existing medical issues, and donors post circulatory death – to treat end stage renal disease because due to a lack of donor supply.
Dr. Sener’s laboratory pioneered the use of hydrogen sulphide, a colourless gas with a strong “rotten egg” odor, to prolong organ storage, improve kidney re-perfusion, decrease dangerous inflammatory cells, promote quicker kidney function recovery, greater urine output and improve recipient survival.
Computer-assisted gastrointestinal surgery: Why can’t they see what I see?
Dr. Christopher Schlachta, Lawson scientist, medical director, Canadian Surgical Technologies and Advanced Robotics (CSTAR), LHSC

Dr. Schlachta’s current research interests are focused on development of computer-assisted surgical techniques and technologies to enhance care and training. Dr. Schlachta demonstrated how computer-assisted technologies in the operating room can enhance communication among surgeons and trainees to produce better outcomes for patients. He is currently partnering with industry to commercialize operating room technology he and a team of engineers at CSTAR have developed.
See more photos from this Café Scientifique on Lawson's Facebook page.
Dementia doesn’t have to be your destiny
Tackling a “dirty dozen” list of health and lifestyle factors can go a long way in lowering the risk of dementia, say London experts.
Many people could greatly improve their odds against developing dementia by making four, low-cost lifestyle changes – today.
In the first study of its kind, researchers at Lawson Research Institute (Lawson) and Western University have found that about half of dementia cases in Canada can be influenced by 12 lifestyle factors.
Topping the “dirty dozen” list across Canadians’ lifespan, and especially notable from mid-life onwards, are physical inactivity, hearing loss, obesity and hypertension.
The solutions:
- Get off the couch and get moving
- Tackle hearing loss early
- Lose weight
- Get assessed and treated for high blood pressure
“While lifestyle changes aren’t a magic pill to prevent all dementias, they’re an empowering way to reduce the overall risk,” says Lawson researcher and study lead author, Surim Son, a Western University PhD candidate who with the dementia research program at St. Joseph’s Health Care London (St. Joseph’s).
“We’re talking about significant benefits to Canadian health and health systems,” adds Son.
The findings could also have profound implications in refocusing health policy priorities. The Public Health Agency of Canada is already highlighting the study as part of its resources for national health policy advisors, she notes.
This study is the first to weigh Canadians’ lifestyles and habits against 12 potentially modifiable risk factors for dementia, and the first globally to include sleep disruption on the list.
Son’s paper, published in The Journal of Prevention of Alzheimer’s Disease, builds on a 2017 study in the Lancet that shows 12 modifiable risk factors throughout the course of life could contribute to 40 per cent of dementias around the world.
But Canada’s numbers are considerably higher because more of us indulge in weightier lifestyle risks. For example, four of every five older Canadian adults don’t exercise regularly; one in three is obese or has hypertension; and one in five has hearing loss.
"If half of the dementia cases in Canada are linked to modifiable lifestyle risk factors, this suggests that, today, prevention may be the most effective form of treatment," says Dr. Manuel Montero-Odasso, co-author of the paper and Director of the Brain & Gait Lab at St. Joseph’s Parkwood Institute.
“Dementia doesn’t have to be your destiny, even if that’s part of your genetic story. Our results from the SYNERGIC Trial shows almost everyone can change their risk factors and improve their cognitive resilience,” says Montero-Odasso, who was recently awarded a $2.4-million Canadian Institutes of Health Research grant to train professionals in risk reduction and care for people living with cognitive impairment.
Montero-Odasso’s advice: “Go out for a walk and keep moving. Get a hearing assessment. Keep your blood pressure in check. It’s low-cost and easy to implement. It’s good for your body health, even beyond improving your brain health and reducing your dementia risk.”
The 12 potential modifiable factors (based on a study of 30,000 Canadians over the age of 45), weighted from most significant factor to least:
- Physical inactivity
- Hearing loss
- Obesity
- Hypertension
- Traumatic brain injury
- Depression
- Less education in early life
- Sleep disturbances
- Diabetes
- Smoking
- Excessive alcohol
- Social isolation
Dementia research hits the ‘mark’
St. Joseph’s Health Care London is at the forefront of national research exploring biomarkers to better predict dementia and slow its onset.
Dr. Michael Borrie is now seeing grandchildren of patients who came to his clinic when he first started Alzheimer’s research 30 years ago.
His message to this new generation is more hopeful than ever, bolstered by ever-more-reliable ways of early detection and being tantalizingly close to a future of predicting dementia and intervening even before symptoms appear.
“The ultimate goal is to slow cognitive decline – and to stop it if we can – so that people can live independently, and happier, for a lot longer,” says Borrie, Medical Director of the Aging Brain and Memory Clinic at St. Joseph’s Health Care London (St. Joseph’s).
“We’re aiming to alter the trajectory of dementia,” he says.
A geriatrician, clinician and researcher, Borrie is also Platform Lead for the Comprehensive Assessment of Neurodegeneration and Dementia (COMPASS-ND), a long-term study within the Canadian Consortium on Neurodegeneration and Aging (CCNA).
Recently, the Canadian Institutes of Health Research announced $20.6 million in funding to continue the work of CCNA, a 30-site, multi-pronged project of which the St. Joseph’s-based team is the lead player. The grant will enable them to advance the frontiers of dementia research to benefit real-world patients here and across the country.
Solving mysteries with biomarkers
Despite the prevalence of Alzheimer’s and other neurodegenerative diseases – and with more than 10,000 new diagnoses in Canada each year – there are still many mysteries to solve: Why do some people have early-onset dementia while others, super-agers, remain alert and active in their 90s? What’s happening genetically, in their environment and personal medical history to advance or protect against the disease?
What is known, however, is the link between damaged nerve cells and specific proteins that misfold and clump together to form amyloid plaques and tau tangles in the brain. Detecting these abnormal proteins early is an important key to diagnosis and prediction.
Locally, the most comprehensive tool has been state-of-the-art brain Positron Emission Tomography (PET) scanning at St. Joseph’s Imaging. Lawson researchers are also involved in reliably detecting amyloid proteins by analyzing participants’ cerebrospinal fluid (CSF) – a surprisingly accurate way of confirming imaging results, says geriatrician Dr. Jaspreet Bhangu, a Lawson scientist and head of the biomarker project.
Through the BioMIND regional research project, Lawson scientists are analyzing PET scans, blood and CSF samples to check for specific protein biomarkers. If shown to be reliable, a series of these tests over time could signal whether the disease is progressing, and could predict whether it will progress or respond to treatment.
All that gets added to an arsenal that includes tests of behaviour, memory and cognitive function.
“It’s a triple assessment, or even a quadruple one, that we can conduct over time. We hope to use these advanced tests to provide vital information, similar to what is done in certain types of cancer,” Bhangu says.
But that’s not all.
Testing potential treatments
St. Joseph’s is also one of the country’s most active sites for clinical trials into whether novel medications might be able to directly pinpoint and destroy the proteins that cause Alzheimer disease.
“This is the intersection of cutting-edge research, top-notch resources and excellent clinical practice to develop personalized treatments,” says Bhangu. “What makes us unique in Canada among dementia researchers is that our science is taking us from bench to bedside – a rapid turnaround from research to direct patient benefit.”
If a person has a strong family history of Alzheimer disease and no symptoms – but does have positive biomarkers confirming presence of disease – they may then choose to take part in a randomized controlled trial to try to alter the trajectory of the disease.
“It’s still in a research context, still in clinical trials – but if Health Canada ultimately approves a treatment, we’ll have the ability and the patient database to be able to translate our findings into clinical practice much more quickly instead of waiting for years,” says Borrie.
All this is good news for a generation eager for answers, Borrie says.
“When we learn more about the mechanisms of the disease, we can find more effective, earlier treatments. And if we can treat people earlier, we hope to move the disease progression curve to the right, to add more years of good cognitive health to someone’s life.”
Detecting the Undetectable
A simple fall can lead to long-term hand problems such as arthritis due to fracturing the scaphoid bone in the wrist. Scaphoid fractures are known to have the highest rate of healing failures. While this bone’s fragile blood supply is commonly thought to be the main reason for why it is difficult to heal, Dr. Ruby Grewal is looking into a different reason – infection.
Infections are known to cause difficulty in healing bones, but traditional tests for infections in the scaphoid have come up negative. With new advancements in detecting microbial DNA, scientists can now test for ‘clinically undetectable’ infections.

In a new study, Dr. Grewal will use microbial DNA test whether or not there are infections in the scaphoid fracture which causes improper healing of the bone.
“The goal of this study is to use advanced DNA sequencing technology to test whether or not we can detect evidence of microorganisms in non-healing scaphoids,” explains Dr. Grewal, Lawson Scientist and Orthopaedic Surgeon at the Roth McFarlane Hand and Upper Limb Centre (HULC) at St. Joseph’s Health Care London.
Finding new causes of improper healing of the scaphoid bone could improve treatments for individuals with these injuries and prevent long-term problems with hand function. These insights into the causes of improper healing could also prevent young patients from developing wrist arthritis.
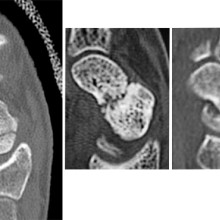
From left to right: Normal scaphoid fracture. Scaphoid fracture that is struggling to heal. Scaphoid non-union where the bone has failed to heal.
Dr. Grewal’s study is being funded through the Lawson Internal Research Fund (IRF).
“The financial support provided by Lawson’s IRF is of utmost importance to researchers. These funds will allow our team to embark on a new area of research and test a novel hypothesis,” says Dr. Grewal, “While traditional granting agencies are reluctant to fund completely novel areas of research without pilot data to prove feasibility, the Lawson IRF allows researchers to investigate new theories in a sound scientific manner. Without the ability to test new ideas we cannot innovate and make advancements in health care. Support for this project allows for that.”
Lawson’s IRF is designed to provide Lawson scientists the opportunity to obtain start-up funds for new projects with the potential to obtain larger funding, be published in a high-impact journal, or provide a clinical benefit to patients. Funding is provided by the clinical departments of London Health Sciences Centre and St. Joseph’s Health Care London, as well as the hospital foundations (London Health Sciences Foundation and St. Joseph’s Health Care Foundation).
Dr. Ting-Yim Lee recognized by WORLDiscoveries for medical imaging innovation
An exceptional career of innovation prowess, influence and leadership has won Dr. Ting-Yim Lee the inaugural Career Achievement Award presented by WorldDiscoveries.
Dr. Lee, Director of PET/CT Research at Lawson Health Research Institute and Medical Physicist at St. Joseph’s Health Care London, is being recognized for the significance of his work in the field of medical imaging and outstanding success in turning innovative ideas into tangible products and services.
Each year, WORLDiscoveries, the technology transfer and business development office for Western University, Lawson, and Robarts Research Institute, hosts the Vanguard Awards. These prestigious awards honour the community’s brightest minds, visionary entrepreneurs, and the exceptional achievements they have made in technology and research. By partnering with WORLDiscoveries, recipients of the Vanguard Awards have reached significant market-readiness milestones, propelling their ideas toward real-world impact. All recipients have made remarkable strides in their respective fields, shaping the future of innovation.
Dr. Lee pioneered use of advanced methods to analyze medical images from machines like CT, MRI and PET to gather important information about diseases. Over the years, he has published 290 research papers, which have been cited nearly 19,000 times – an indication of their impact in the medical community.

His work initially focused on using dynamic CT scans to study blood flow in stroke and cancer patients and to address challenges related to imaging the heart. With dynamic CT scans, images are taken continuously as change in vessels, organs and other structures is happening. The effect is similar to a real-time video. Dr. Lee also played a role in developing guidelines for using these scans to study the growth of new blood vessels that nourish the proliferation of cancer cells.
More recently, he shifted his focus to PET scans to examine biological processes in the body, demonstrating their effectiveness in detecting prostate cancer in a short, 22-minute scan. One of his notable contributions was the development of CT Perfusion software, which played a crucial role in a U.S. nation-wide ovarian cancer trial involving more than 20 medical centres. This software proved valuable as an early biomarker for assessing treatment response.
In addition to research, this world-renowned researcher has obtained eight patents and has licensed five enhanced versions of the CT Perfusion software to GE HealthCare, making it easier for clinicians to apply his techniques in real-world hospital settings.
Dedicated to creating the next generation of scientists, Dr. Lee has mentored and trained 70 graduate students, post-doctoral fellows, clinicians and research associates, many of them going on to earn prestigious research awards themselves.
“I am grateful for the support received over the decades from colleagues and trainees,” says Dr. Lee. “Without them, the work cannot be done. This award is not just for myself but for all collaborators and contributors on this journey.”
In presenting the award, WORLDiscoveries says Dr. Lee’s work has transformed industries, inspired countless individuals within the field to pursue innovation and entrepreneurship, and has left a lasting impact on society at large.
St. Joseph’s congratulates this remarkable and dedicated scientist on this prestigious and well-deserved award.
More on the Vanguard Awards and the 2023 recipients are available on the WORLDiscoveries website.
Drug combats underlying causes of Alzheimer-related dementia
A “game-changing” new drug offers both hope and time to some people diagnosed with Alzheimer’s disease, says the head of a St. Joseph’s program that played a key role in the medication’s clinical trials. Health Canada has newly approved lecanemab (brand name Leqembi, developed by Eisai Co. and Biogen), which has been shown to slow progression of Alzheimer’s disease in people with mild symptoms.
St. Joseph’s Health Care London, and its innovation arm at Lawson Research Institute, has played a key role as one of multiple sites that have trialed the drug.
“This is game-changing,” says Dr. Michael Borrie, medical director of the Aging Brain and Memory Clinic at St. Joseph’s, whose work in dementia research and clinical practice spans more than three decades.
“We’ve been working for over 20 years to find a compound that is disease-modifying. This is the first approved drug in Canada that addresses the underlying pathology of Alzheimer’s, not just the symptoms.”
Lecanemab works by removing amyloid proteins that accumulate as sticky clumps in the brain and are associated with cognitive decline in people with Alzheimer’s. “It reverses one aspect of the disease by removing the plaque from the brain ,” Borrie explains.
“You can characterize its benefit in terms of time saved. If you were to have this medication for four years, you can ‘save’ one year of cognitive decline. It totally changes the course of their neurodegeneration in a way we haven’t seen before.”
Lecanemab was one of many clinical drug trials assigned to research coordinator Kayla Vander Ploeg when she arrived to work at St. Joseph’s more than a decade ago. “For so long, we had hope that one of these medications would benefit patients long-term. Now we have more than hope. We have results,” Vander Ploeg says.
“Today I’m seeing people who say, ‘my dad or my mom was in this study, and now there’s hope for me.’ ”
There are specific eligibility criteria, including confirmed diagnosis – through cognitive testing and through advanced brain imaging and biomarker tests – plus screening to rule out two gene variations that couldresult in more side effects.
Canada is now one of 51 countries to have approved lecanemab.
Borrie cautioned that Health Canada approval doesn’t necessarily translate to funding coverage. It’s not yet determined who will pay for the medication, or how: when lecanemab was approved in the United States in 2023, the annual cost per patient was more than $26,000.
The length of time from drug development to trials to approval illustrates how painstaking pharmaceutical research can be. But it also highlights how integrating health research into hospital settings can translate more quickly into improved patient care.
Exemplary leadership earns Ting-Yim Lee medical physics Gold Medal
Medical physicist Ting-Yim Lee still isn’t sure exactly what interviewers saw in him when they recruited him in 1988 to work in radiology research at St. Joseph’s Health Care London.
But he’s honoured they saw and cultivated that kernel of possibility.
Lee is now recognized as an innovative imaging scientist transforming research and patient care. In June, Lee will receive the Canadian Organization of Medical Physicists’ (COMP) Gold Medal Award for exemplary achievement. It is the organization’s most prestigious award.
“I was hired from Winnipeg to work here,” he says. “I had a thin CV, and very few publications. I was a nobody, I thought. But St. Joseph’s recognizes the potential in people and they saw potential in me. If not for St. Joseph’s nurturing environment, our imaging program would not be what it is today.”
Lee is director of PET/CT Research at Lawson Research Institute (Lawson) and medical physicist at St. Joseph’s Hospital. He is also a professor at Western University’s Schulich School of Medicine & Dentistry and a scientist at Robarts Research Institute.
At St. Joseph’s and Lawson, he has sparked the growth of the Molecular Imaging and Theranostics program. Recently it was chosen to be Canada’s first a GE Centre of Excellence in Molecular Imaging and Theranostics based on the past track record of the Lawson Imaging program of achieving a number of national and global firsts.
Mustard-seed growth
Lee says the Lawson Imaging Program’s development is symbolized by the mustard seed in the St. Joseph’s logo: “The mustard seed is the smallest of seeds and it grows into a strong and beautiful tree. When I started at St. Joseph’s, we’d installed a CT scanner one year earlier, and we were quite behind other hospitals. Then we started developing it bit by bit, piece by piece, leaf by leaf.”
Among his most celebrated achievements is developing CT Perfusion technology, a world-first in 2000 that has revolutionized stroke diagnosis and treatment by providing detailed images of blood flow in and to the brain.
The technology is used in more than 8,000 hospitals worldwide and more than 25,000 licences of the technology have been sold over the last 22 years– the royalties enabling the purchase of new, state-of-the-art CT and PET/CT equipment at St. Joseph’s to the benefit of researchers and patients alike.
Lee’s contribution helped secure a $30-million Canada Foundation for Innovation initiative in 2006, introducing hybrid imaging to Canada—including the nation’s first PET/MRI systems. His
expertise has turned contrast-enhanced CT into a powerful functional imaging tool with applications to oncology, cardiology, and neurology.
Excellence, multiplied
“It is no exaggeration to state that without Dr. Lee, the Lawson Imaging Research Program and the medical physics team would never have achieved the heights of success that it has,” says Frank Prato, PhD, founder of the program in 1982 and its leader until 2024.
Prato says Lee has had “a profound influence” on the careers of hundreds of medical physicists, including training and mentoring 60 graduate and postdoctoral students – many of whom are now training students of their own.
“These multipliers/amplifiers of Dr. Lee’s mentorship have had a profound effect on the excellence of the medical physicists we have in Canada and the excellence of the ones we train for the world,” Prato says.
Lee has published 290 research papers, which have been cited nearly 19,000 times – an indication of their impact in the medical community. He has been awarded the Meritorious Service Cross from the Governor General of Canada and received the Career Achievement Award as a WORLDiscoveries innovator.
The St. Joseph’s difference
More recently, Lee created, in partnership with St. Joseph’s Health Care Foundation and Western, two endowed chairs to research and translate liquid radiation therapy.
His considerable accomplishments are matched by his humility and his eagerness to deflect credit to his colleagues, St. Joseph’s, the St. Joseph’s Health Care Foundation and the broader imaging and research communities.
Excellent technology and research are an outgrowth of the people and culture of St. Joseph’s, Lee emphasizes. “I always feel that when I walk into St. Joseph’s, it immediately has that warm feeling that envelops you. It’s different. It’s a nurturing environment.”
The COMP Gold Medal is the highest award given by the Canadian Organization of Medical Physicists and is given to currently active or retired individuals to recognize medical physicists who have made outstanding contributions:
- A body of work fundamentally altering the knowledge base and practice of medical physics
- Leadership positions in medical physics organizations leading to improvements in the status and public image of medical physicists in Canada
- Significant influence on the professional development of the careers of medical physicists in Canada through educational activities or mentorship
Several London and Lawson-affiliated researchers have won the COMP Gold Medal, including Prato in 2024.
This year’s annual scientific meeting takes place in London on June 4 – 7.
Fecal transplants show promise in improving melanoma treatment
In a world-first clinical trial published in the journal Nature Medicine, a multi-centre study from Lawson Health Research Institute, the Centre hospitalier de l’Université de Montréal (CHUM) and the Jewish General Hospital (JGH) has found fecal microbiota transplants (FMT) from healthy donors are safe and show promise in improving response to immunotherapy in patients with advanced melanoma.
Immunotherapy drugs stimulate a person’s immune system to attack and destroy cancer. While they can significantly improve survival outcomes in those with melanoma, they are only effective in 40 to 50 per cent of patients. Preliminary research has suggested that the human microbiome – the diverse collection of microbes in our body – may play a role in whether or not a patient responds.
“In this study, we aimed to improve melanoma patients’ response to immunotherapy by improving the health of their microbiome through fecal transplants,” says Dr. John Lenehan, Medical Oncologist at London Health Sciences Centre’s (LHSC) London Regional Cancer Program (LRCP), Associate Scientist at Lawson and Associate Professor in the Department of Oncology at Western University’s Schulich School of Medicine & Dentistry.
A fecal transplant involves collecting stool from a healthy donor, screening and preparing it in a lab, and transplanting it to the patient. The goal is to transplant the donor’s microbiome so that healthy bacteria will prosper in the patient’s gut.
“The connection between the microbiome, the immune system and cancer treatment is a growing field in science,” explains Dr. Saman Maleki, Scientist at Lawson and LHSC’s LRCP, Assistant Professor in Schulich Medicine’s Departments of Oncology, Pathology and Laboratory Medicine, and Medical Biophysics, and senior investigator on the study. “This study aimed to harness microbes to improve outcomes for patients with melanoma.”
The phase I trial included 20 melanoma patients recruited from LHSC, CHUM and Jewish General Hospital. Patients were administered approximately 40 fecal transplant capsules orally during a single session, one week before they started immunotherapy treatment.
The study found that combining fecal transplants with immunotherapy is safe for patients – which is the primary objective of a phase I trial (also called ‘safety trials’). The study also found 65 per cent of patients who retained the donors’ microbiome had a clinical response to the combination treatment. Five patients experienced adverse events sometimes associated with immunotherapy and had their treatment discontinued.

“We have reached a plateau in treating melanoma with immunotherapy, but the microbiome has the potential to be a paradigm shift,” says Dr. Bertrand Routy, Oncologist and Director of CHUM’s Microbiome Center. “This study puts Canada at the forefront of microbiome research by showing we can safely improve patients’ response to immunotherapy through fecal transplants.”
“These exciting results add to a rapidly growing list of publications suggesting that targeting the microbiome may provide a major advance in the use of immunotherapy for our patients with cancer,” adds Dr. Wilson H. Miller Jr. of the JGH and Professor in the Departments of Medicine and Oncology at McGill University.
Previous studies looking at patients receiving immunotherapy who do not respond have found many had an unhealthy microbiome, explains Dr. Lenehan.
“There's a portion of people who don't respond or the treatment just doesn't work,” says Dr. Lenehan. “The hope with the fecal transplant is to make more people respond to treatment.”
These results have also led to a closer examination of the role of the microbiome in regulating how the body responds to disease and how the drugs themselves interact with the microbiome.

“The microbes on and in us - and there's actually a huge amount of those – play a critical role, including modulating some of our immune responses,” explains Dr. Jeremy Burton, Research Chair of Human Microbiome and Probiotics, Scientist at Lawson and St. Joseph’s Health Care London and Associate Professor in the Department of Microbiology and Immunology at Schulich Medicine.
The study is unique due to its administration of fecal transplants (from healthy donors) in capsule form to cancer patients – a technique pioneered in London by Dr. Michael Silverman, Lawson Scientist, Chair of Infectious Diseases at Schulich Medicine and Medical Director of the Infectious Disease Care Program at St. Joseph’s Health Care London.
“Our group has been doing fecal transplants for 20 years, initially finding success treating C. difficile infections. This has enabled us to refine our methods and provide an exceptionally high rate of the donor microbes surviving in the recipient’s gut with just a single dose,” says Dr. Silverman. “Our data suggests at least some of the success we are seeing in melanoma patients is related to the efficacy of the capsules."

The team has already started a larger phase II trial involving centres in Ontario and Quebec. Lawson researchers are also studying the potential of fecal transplants in the treatment of other cancers, including renal cell carcinoma, pancreatic cancer and lung cancer, as well as HIV and rheumatoid arthritis.
This work is not possible without poop donors, and there is a critical need for more. Donors must be between the ages of 18 to 50 and reside in the London, Ont. area. To learn more about eligibility and donating, call the 519 646-6100, ext. 61726 or email Dr. Seema Nair Parvathy, Research Scientist, at SeemaNair.Parvathy@sjhc.london.on.ca.
This research is supported in part through donor funding from London Health Sciences Foundation, Western University, the Lotte and John Hecht Memorial Foundation, the JGH Foundation, Canadian Cancer Society’s Impact Grant program and The Terry Fox Foundation.
Groundbreaking Alzheimer’s and cancer studies receive $7.2M boost
Lawson Research Institute scientists and partners will focus on molecular imaging and theranostics to potentially transform the detection and treatment of neurodegeneration and cancer.
The quest to advance detection and treatment of Alzheimer’s disease and to personalize cancer care has received a major boost, with $7.2 million in funding to Lawson Research Institute (Lawson) of St. Joseph’s Health Care London (St. Joseph’s) for first-of-its kind research.
Lawson scientists will partner with a broad team of researchers at London Health Sciences Centre Research Institute (LHSCRI), McMaster University, University Health Network and BC Cancer on the ground-breaking studies focused on molecular imaging and theranostics as a potential game-changer in detecting and treating neurodegeneration and cancer, particularly prostate, brain and breast cancer.
Principal investigator Ting-Yim Lee, PhD, Lawson’s Director of PET/CT Research, and his team of investigators were awarded $2 million through the Ontario Research Fund – Research Excellence for the study titled “Improving Cancer and Alzheimer’s Disease Diagnosis and Treatment Through Cutting-edge Molecular Imaging and Theranostics”. Co-Principal Investigator is radiation oncologist Dr. Glenn Bauman at LHSCRI.
Additional funding from private-sector partners and Lawson, as well as from donors through St. Joseph’s Health Care Foundation, brings the total research investment to $7.2 million.
The research has the potential to offer hope for solutions to some of the most prevalent and pernicious diseases affecting Canadians, explains Lee.
“Both research projects are the first of their kind in Canada aimed at advancing how we diagnose and treat Alzheimer’s disease and cancer,” he says. “This collaborative funding initiative will also drive innovation in the exciting field of molecular imaging and theranostics at St. Joseph’s, at the heart of which is St. Joseph’s new, high-sensitivity GE HealthCare Omni Legend 2 PET/CT – the first in Canada.”
The studies encompass the following:
- Alzheimer’s disease: The new PET/CT at St. Joseph’s allows researchers to simultaneously study both blood flow and glucose metabolism in the brain. Both these mechanisms are believed to be contributing factors in the onset of Alzheimer’s. By measuring both at the same time, the research team hopes to uncover early signs that the brain is in trouble and at risk of plaque deposits and toxic proteins that have been linked to the development of Alzheimer’s.
- Cancer: The cancer study will focus on developing theranostic techniques to achieve personalized dosimetry – a method used to determine the exact amount of radiation a patient should receive during treatment, based on their individual characteristics. This maximizes effective treatment while minimizing harm to healthy tissues.
Molecular imaging and theranostics is a rapidly emerging field of medicine that combines ultra-precise scans and theranostics (a term that melds the words therapeutics and diagnostics). Together, they offer a one-two punch by integrating imaging and radiotracers that can identify the location and extent of diseased tissues and selectively destroy the abnormal cells while leaving surrounding healthy cells undamaged. In collaboration with GE HealthCare, St. Joseph’s is developing Canada’s first GE HealthCare Centre of Excellence in Molecular Imaging and Theranostics.
“By bridging the gap between research and clinical practice, we hope to ease the burden on patients and their families, offering more effective and compassionate care”
-Ting-Yim Lee, PhD, Director of PET/CT Research at Lawson Research Institute.
“We are already seeing the impact of novel theranostics for treatment of men with advanced prostate cancer,” says Bauman. “Promising new theranostic approaches are emerging for many cancers and this investment further positions London to be a leader in this area of research.”
In the initial phase of the studies, 100 patients will be recruited from St. Joseph’s Aging Brain and Memory Clinic at Parkwood Institute for the Alzheimer’s study; while 90 patients will be recruited from London Health Sciences Centre’s Verspeeten Family Cancer Centre for cancer studies. There are plans to recruit patients from the collaborating centres once results from the initial phase are confirmed.
“By bridging the gap between research and clinical practice, we hope to ease the burden on patients and their families, offering more effective and compassionate care,” says Lee. “We are deeply grateful for the opportunity to turn our research into real-world solutions that can make a meaningful impact.”
With dozens of 'firsts' in imaging research, “Lawson is a powerhouse of innovation,” adds Michael Kovacs, PhD, Program Lead, Lawson’s Imaging Research Program, and Lead, Cyclotron & PET Radiochemistry Facility. “We're excited to explore how this work could transform care."
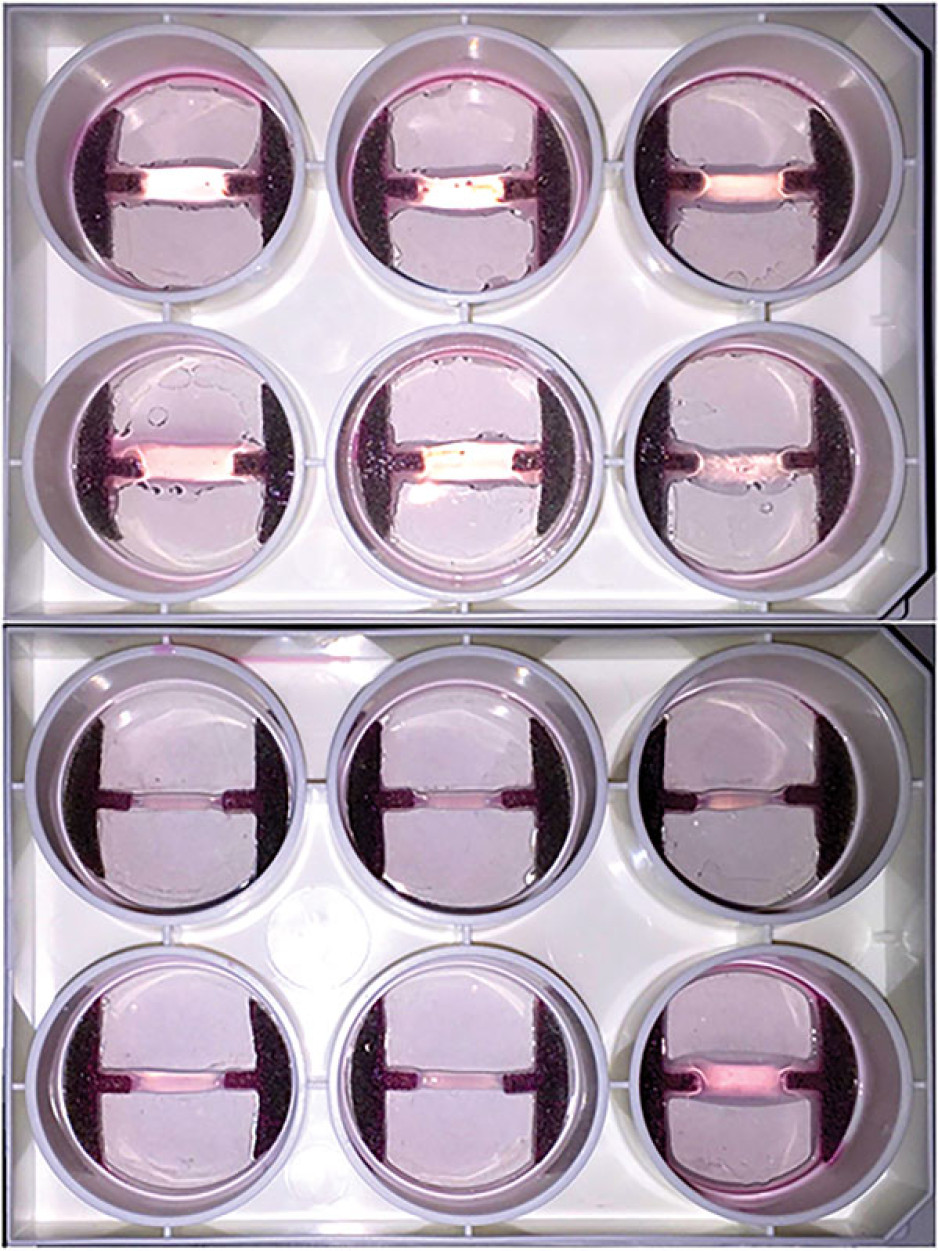
Growing Tissues in the Lab
When challenged by surgeons to find better treatments for difficult-to-manage connective tissue diseases, Dr. David O’Gorman gladly accepted.
Dr. O’Gorman is a Molecular Biologist and Lawson Scientist based at St. Joseph’s Hospital, a part of St. Joseph’s Health Care London. His research focuses on understanding normal and abnormal connective tissue repair. He collaborates with researchers and clinicians working in many different disciplines, including those specializing in reconstructive surgery, orthopedics and urology.
Surgical reconstructions can be hampered by a lack of graft tissue, or graft tissue of insufficient quality, making it difficult to achieve optimal outcomes for the patients.
An example is a condition called urethral stricture disease (urethral scarring). This condition occurs in males and typically causes symptoms such as frequent and urgent urination, and slow urinary stream. In extreme cases, it can cause urinary tract infections, permanent bladder dysfunction and renal failure. Recurrence rates after minimally invasive treatments are high, and so many urologists recommend open surgical approaches.
Surgeons can use the patient’s own tissues to reconstruct the urethra after stricture removal. This tissue is normally sourced from the buccal cavity in the mouth but taking large tissue grafts can result in complications. In cases where buccal grafts have been used for previous reconstructions, there may not be enough intact tissue left.
Dr. O’Gorman sees a solution in growing sheets of human buccal tissues in the lab.
“We are currently using buccal graft trimmings as a source of cells, culturing them in a 3D environment and expanding them to create tissues of suitable size, density and elasticity.”
The patient’s own cells are used to generate a tissue graft for urethral reconstruction. While several research groups have developed this approach in the past, few have attempted to translate their models for clinical use.
“Our immediate goal is to provide proof of principle – that we can consistently generate grafts of suitable size and functional characteristics,” explains Dr. O’Gorman, “In the future, we could be providing bioengineered graft tissues for reconstructive surgeries here in London.”
Bioengineered human tissues can also be used as ‘mimetics’ – replications of human tissues – to study diseases, especially those difficult to model using routine laboratory methods.
Instead of a using a growth media or sterile plastic dishes, 3D cell culture is achieved by embedding cells in a matrix of proteins and other molecules normally found in those tissues. In this environment, gene expression and growth is more similar to cells of connective tissues in the body being replicated.
Dupuytren’s disease (or Dupuytren’s Contracture) affects the palmar fascia in the hand, a connective tissue beneath the skin that extends from the base of the palm into the fingers. This disease can be understood as a type of excessive scarring, where normal tissue repair processes have gone awry and dense scar tissue forms, typically causing permanent palm or finger flexion that restricts hand function.
This condition is surprisingly common and may affect more than one million people in Canada. While there are surgical treatment options available, none consistently prevent this disease from recurring in at least a third of patients.
“Due to its high recurrence rate after treatment, Dupuytren’s disease is currently considered incurable. Our challenge is to understand it well enough to develop truly effective treatments,” says Dr. O’Gorman.
Human hands have unique characteristics not found in other species, making animal models impractical. Instead, Dr. O’Gorman’s team extracts cells from the diseased palmar fascia of patients undergoing hand surgeries and bioengineers them into palmar fascia ‘contractures’ in the lab.
“Since the cells from a single palmar fascia sample can be used to grow dozens of little contractures, we can test many different treatments simultaneously to see what works best for each patient.”
This approach may also allow them to determine if Dupuytren’s disease is truly one disease, or a group of similar diseases that cause palm and finger contractures.
“Often, Dupuytren’s disease is clearly heritable, but some individuals have no family history of it and develop apparently sporadic disease,” notes Dr. O’Gorman. “We want to determine if these are truly the same disease at the molecular level.”
Another major cause of abnormal connective tissue repair is infection, and tissue mimetics can play a role here, too. While rare, infections of artificial joint replacements are particularly devastating for patients, as they typically require readmission to hospital to remove the infected joint, weeks of antibiotic-based treatment, and an additional surgery to replace the artificial joint.
In addition to the associated pain and suffering, these procedures are technically challenging and costly to our health care system.
Artificial shoulder joint infections are most frequently caused by the microorganism Cutibacterium acnes (C. acnes). C. acnes infections disrupt normal tissue repair processes after surgery, cause shoulder tissues to die and promote loosening of the artificial joint. These infections are difficult to diagnose, and there is a lack of reproducible
models in which to study them. Dr O’Gorman’s team has set out to create the first human Shoulder-Joint Implant Mimetic (S-JIM) of C. acnes infection.
“While S-JIMs are more complex, they are 3D in vitro cell culture systems designed to mimic human tissues, like those that we use for studying Dupuytren’s disease.”
S-JIMs include layers of artificial human tissue, wrapped around cores of titanium alloy or cobalt chrome, the metals used to create artificial joints. They are co-cultured with C. acnes under low oxygen conditions similar to those that normally occur around artificial shoulder joints.
“We are bioengineering simple 3D cell cultures to more closely mimic the complexity of human tissues, with blood supply, nerves and interactions with other cells.” – Dr. David O’Gorman
Studying the connective tissue layers close to the infection allows researchers to investigate processes that promote infection, such as the formation of a biofilm that harbours and protects the bacteria from the body’s immune system. They are also able to test whether novel treatments can disrupt biofilm formation and increase the effectiveness of antibiotics.
Dr. O’Gorman predicts that in the future, medical researchers will routinely use bioengineered 3D human tissue and organ mimetics to accelerate our understanding of disease.
“The technology is in its infancy, but the potential for using bioengineered human tissues for surgical reconstructions or as disease models is huge. At Lawson, we’re ready to take on health care challenges and build on innovative approaches to improve the quality of life for patients.”
ONLINE EXCLUSIVE: What is 3D cell culture?
Medical researchers have grown human cells in culture media on or in sterile plastic dishes, such as Petri dishes, for more than 50 years.
Some cells, such as blood cells, can survive and grow in suspension, while others like smooth muscle cells need¬ to adhere to a surface to survive and grow. These are often called “2D cell cultures” because the cells grow horizontally across the bottom of the dish.
Some cells derived from connective tissues, such as fibroblasts, are not only adherent, but also very sensitive to the stiffness of their environment (“biomechanically sensitive” cells). Plastic dishes are at least 10,000 times stiffer than most connective tissues, and when biomechanically sensitive cells detect stiff surfaces, they can change the expression of their genes and behave abnormally.
The most common proteins in these tissues - and in the entire human body - are collagens, and one routine 3D cell culture approach is to embed fibroblasts in a collagen gel (gelatin). Fibroblasts in this environment can grow in any direction they choose, and their gene expression is more similar to cells in connective tissues.
These simple 3D cell cultures represent tissue engineering in its most basic form.
“Our challenge is to bioengineer simple 3D cell cultures in the lab to more closely mimic the complexity of human tissues, which have blood supply, nerves and interactions with other cells and tissues that modify their function and ability to heal after injury,” explains Dr. O’Gorman.
Dr. David O’Gorman is a Lawson Scientist and Co-director, Cell and Molecular Biology Laboratory at The Roth | McFarlane Hand and Upper Limb Centre in London, Ontario. He is also an Assistant Professor at Western University.
Harm reduction research is improving care for patients who use substances
Research from Lawson Health Research Institute is helping to advance harm reduction strategies in hospitals for people who use substances. In an announcement today, Arielle Kayabaga, Member of Parliament for London West, on behalf of the Honourable Ya’ara Saks, Canada’s Minister of Mental Health and Addictions, announced how $72,768 in funding from Health Canada’s Substance Use and Addictions Program is supporting this ongoing work at London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London (St. Joseph’s).
“Here in London, just like many other cities across Canada, we’re seeing substance use harms continue to take a tragic toll on our families and friends,” says MP Kayabaga. “We are committed to supporting organizations who are on the ground in communities, helping to keep people who use substances safe.”
Research from Lawson has found patients who use methamphetamine reported stigma and a lack of understanding about addiction among health-care providers and hospital staff. This can sometimes result in patients not seeking care, experiencing withdrawal while receiving care or leaving a hospital against medical advice.

Building on those findings, a team led by Lawson researchers, Drs. Cheryl Forchuk and Michael Silverman, has been working to implement and study harm reduction strategies at LHSC and St. Joseph’s, including those aimed at facilitating changes in attitude, knowledge, organizational support and safety approaches.
“There’s a lot of stigma and misunderstanding about substance use,” says Dr. Forchuk, Scientist and Assistant Scientific Director at Lawson. “This project aims to embed education on substance use and harm reduction as a foundational way to improve care and outcomes.”

As part of the research project, Darren Scott, a Peer Harm Reduction Worker with Regional HIV/AIDS Connection who has lived experience with substance use, and Tammy Fischer, a Clinical Nursing Educator in LHSC’s Mental Health and Addictions Program, have been working to educate health-care workers about harm reduction practices.
“I am able to share with patient caregivers how I was treated while I was in active addiction,” shares Scott. “I can let them know what people are going through from the other side and provide advice on how to care for them. The health-care teams have been fantastic and very open-minded throughout this project. I have received feedback that it is vital to include people with lived experience in this education.”
One area of focus from this study has been education around sharps boxes in inpatient hospital rooms. Sharps boxes allow for the safe disposal of sharps like needles to protect the health and safety of patients and health-care teams. Through this study, the research team identified that when sharps boxes are removed from the rooms of patients suspected of using substances to discourage substance use it leads to harm.
“About half of patients who use substances are still using in-hospital, since suddenly stopping use is often not feasible nor safe. Access to sharps boxes decreases the risk of injury to health-care teams and patients,” Fischer explains. “People who use any injection must have safe means to dispose of used equipment.”
The team launched a campaign to educate health-care teams on the importance of keeping sharps boxes in patient rooms. Preliminary data from interviews with patients who use substances found they noticed a difference after this education. Patients felt more comfortable speaking to health-care teams and noted they could be more open about discussing their addiction.
Government of Canada funding is critically important to this work and builds on just over $1 million in previously announced funding. The project is one of several harm reduction research initiatives being explored collaboratively through LHSC and St. Joseph’s to ensure people who use substances receive the highest quality of equitable care.
“This investment is part of our comprehensive and compassionate approach to reducing harms as a result of substance use. We will continue to use every tool at our disposal to build a safer, healthier and more caring future for all Canadians,” says Minister Saks. “Supporting local organizations who have deep roots in their communities and have the trust of their patients is making a real difference in people’s lives in the community of London, Ontario.”