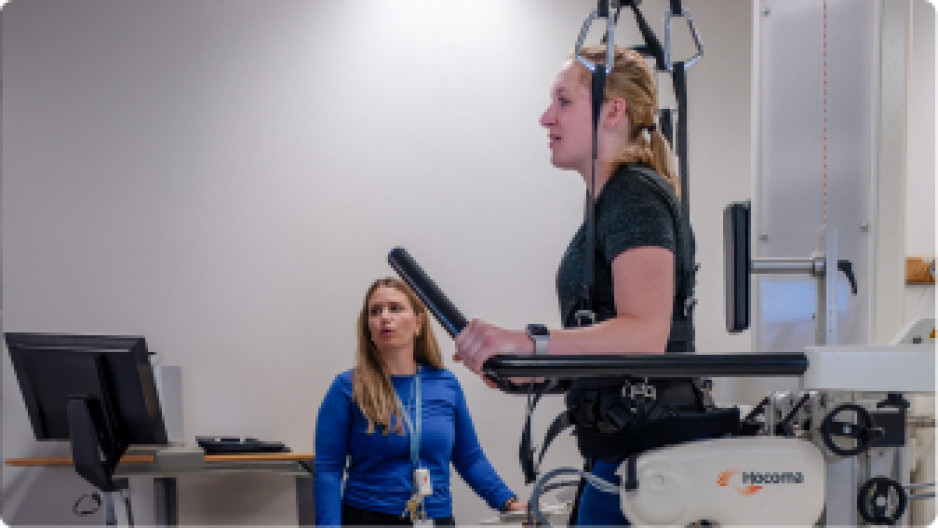Search
Search
Assessing neurofeedback in stroke survivors
Researchers are testing whether a specialized form of imaging can help in stroke rehab.
A new study aims to assess the use of functional near-infrared spectroscopy (fNIRS), a type of imaging, to provide neurofeedback during stroke rehabilitation with a goal of eventually improving patient outcomes.
fNIRS is used to detect changes in brain oxygen levels using light. More recently it has also been used to develop brain-computer interfaces (BCIs), which allow patients with brain injuries to control devices like robotic arms with their thoughts.
Dr. Sue Peters, a Scientist at Lawson Health Research Institute and Director of the Neurorehabilitation Physiology Lab at St. Joseph Health Care London’s Parkwood Institute, was one of the recipients of the Spring 2022 Lawson Internal Research Fund (IRF) Awards.
The funds will go towards a new study to assess whether fNIRS can be used to direct neurofeedback in stroke survivors – helping them with rehabilitation.
“Currently, there's no real measure of brain activity that is used in stroke rehabilitation to help make clinical decisions,” says Dr. Peters, who is also a Professor at Western University.

Over 400,000 Canadians live with the effects of a stroke, according to the Heart and Stroke Foundation, and there’s hope that fNIRS could make a big difference by eventually improving movement and independence.
“We're going to use the device in some common tasks that people might do with their arm and determine whether we can use this device reliably and accurately in a stroke-related context,” Dr. Peters explains.
Participants in the study will imagine moving while remaining still. This activates very similar parts of the brain to when people actually move. If done correctly, patients will see a visual cue generated through measurement using fNIRS.
“We know from MRI studies that when I move my right hand, the left side of my brain is activated,” notes Dr. Peters. “We think we can use this concept in stroke rehab.”
Dr. Peters is recruiting 40 people from the community who are at least six months post stroke and 40 healthy adults of all ages. They will first participate in motor assessment with a physiotherapist and then wear an fNIRS cap while thinking about moving their wrist to measure brain activity.
Previously, there were a lack of methods to image the brain during real-life movement.
“The hope is to eventually conduct a clinical trial where we're testing motor interventions to see whether some things are more effective than others at activating the regions of the brain that were impacted by the stroke.”
Dr. Peters believes the study has the potential to have a big impact on the future of rehabilitation for stroke patients, leading to lasting changes in quality of life.
Celebrating Clinical Trials Day
Clinical trials are the gold standard in medical research, used to test new treatments and medical devices to ensure they are safe and improve patient outcomes.
Each year on May 20, Clinical Trials Day aims to raise awareness about the importance of clinical trials. At Lawson Health Research Institute, our researchers, research staff and learners across London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London (St. Joseph’s) are working daily to advance clinical trials for some of the most pressing health challenges.
“If you look at many areas of medicine, like cancer and cardiovascular disease, part of why those conditions have had dramatic improvements in outcomes over the last several decades is because of clinical trials,” says Dr. Amit Garg, Scientist at Lawson, Lead for the Kidney, Dialysis & Transplantation Research Program at ICES Western, and a Nephrologist at LHSC.
Clinical trials can also provide patient participants with new treatment options and can demonstrate when existing treatments have applications for other diseases.
“We could not conduct clinical trials without patients participating in them,” adds Dr. David Palma, Associate Scientist at Lawson and Radiation Oncologist at LHSC. “A clinical trial is a very rigorous process where we carefully define a treatment and follow patients very closely with extra interventions and tests to see not only how the disease is responding to treatment, but also any effects on a patient’s quality of life.”
It also takes a team to make clinical trials a success, including the critical work of research coordinators, associates and assistants, adds Dr. Swati Mehta, Lawson Scientist based at St. Joseph’s Parkwood Institute.
Dr. Palma also notes that while clinical trials require investment to conduct them, they can ultimately lead to savings in the health system.
“While the primary goal of a clinical trial is to improve or save lives, they often lead to cost savings down the road. Improving cure rates means people don’t need as much treatment and that can save the initial investment many, many times over,” Palma says.
Looking ahead, work is ongoing to make clinical trials more efficient and equitable.
“Eliminating specialized infrastructure would help make trials more equitable, so they are available in smaller communities and at distant sites that otherwise would not have access. Making study materials available in multiple languages and to anyone with accessibility issues can also help,” Garg adds.
“Future clinical trials will need to follow more pragmatic, adaptive study designs that allow us to evaluate therapies or interventions in a more realistic setting,” Dr. Mehta says. “These would also allow us to follow-up with patients that were potentially underrepresented in past research.”
According to researchers at Lawson, the future of clinical trials is bright with hundreds of trials currently underway at LHSC and St. Joseph’s with the goal of improving patient outcomes.
Could online programming reduce barriers for those with mobility impairments?
LONDON, ON – A new study at Lawson Health Research Institute will offer online exercise and behavioral intervention for adults who are mobility impaired. The goal is to reduce barriers to accessing activity programs.
“Many people with mobility concerns experience barriers to physical activity, such as fear of falling because of their past injuries,” says Dr. Swati Mehta, Lawson Scientist. “This project aims to help them cope and learn skills to continually, actively engage in physical activity.”
The 10-week virtual program is being coordinated through St. Joseph’s Health Care London’s Parkwood Institute. It will consist of weekly personal behavioral coaching. Participants will also be asked to complete two or three group physical activity programs each week, such as seated aerobics, seated boxercise and seated yoga.

“This study is really exciting because it brings together both behavioral coaching and physical activity classes, which are normally offered separately,” explains Dr. Dalton Wolfe, Lawson Scientist. “This provides extra support to help those with mobility impairments overcome barriers to maintaining an active lifestyle.”

Those barriers can include things like fatigue and transportation challenges that often accompany neurological conditions like multiple sclerosis, spinal cord injury, brain injury and stroke.
“Ultimately this study is about enhancing quality of life and wellbeing while improving participants’ ability to engage in the community,” says Dr. Wolfe.
The research team is currently recruiting 20 participants for the study. For more information on the study you can email @email.
Dementia doesn’t have to be your destiny
Tackling a “dirty dozen” list of health and lifestyle factors can go a long way in lowering the risk of dementia, say London experts.
Many people could greatly improve their odds against developing dementia by making four, low-cost lifestyle changes – today.
In the first study of its kind, researchers at Lawson Research Institute (Lawson) and Western University have found that about half of dementia cases in Canada can be influenced by 12 lifestyle factors.
Topping the “dirty dozen” list across Canadians’ lifespan, and especially notable from mid-life onwards, are physical inactivity, hearing loss, obesity and hypertension.
The solutions:
- Get off the couch and get moving
- Tackle hearing loss early
- Lose weight
- Get assessed and treated for high blood pressure
“While lifestyle changes aren’t a magic pill to prevent all dementias, they’re an empowering way to reduce the overall risk,” says Lawson researcher and study lead author, Surim Son, a Western University PhD candidate who with the dementia research program at St. Joseph’s Health Care London (St. Joseph’s).
“We’re talking about significant benefits to Canadian health and health systems,” adds Son.
The findings could also have profound implications in refocusing health policy priorities. The Public Health Agency of Canada is already highlighting the study as part of its resources for national health policy advisors, she notes.
This study is the first to weigh Canadians’ lifestyles and habits against 12 potentially modifiable risk factors for dementia, and the first globally to include sleep disruption on the list.
Son’s paper, published in The Journal of Prevention of Alzheimer’s Disease, builds on a 2017 study in the Lancet that shows 12 modifiable risk factors throughout the course of life could contribute to 40 per cent of dementias around the world.
But Canada’s numbers are considerably higher because more of us indulge in weightier lifestyle risks. For example, four of every five older Canadian adults don’t exercise regularly; one in three is obese or has hypertension; and one in five has hearing loss.
"If half of the dementia cases in Canada are linked to modifiable lifestyle risk factors, this suggests that, today, prevention may be the most effective form of treatment," says Dr. Manuel Montero-Odasso, co-author of the paper and Director of the Brain & Gait Lab at St. Joseph’s Parkwood Institute.
“Dementia doesn’t have to be your destiny, even if that’s part of your genetic story. Our results from the SYNERGIC Trial shows almost everyone can change their risk factors and improve their cognitive resilience,” says Montero-Odasso, who was recently awarded a $2.4-million Canadian Institutes of Health Research grant to train professionals in risk reduction and care for people living with cognitive impairment.
Montero-Odasso’s advice: “Go out for a walk and keep moving. Get a hearing assessment. Keep your blood pressure in check. It’s low-cost and easy to implement. It’s good for your body health, even beyond improving your brain health and reducing your dementia risk.”
The 12 potential modifiable factors (based on a study of 30,000 Canadians over the age of 45), weighted from most significant factor to least:
- Physical inactivity
- Hearing loss
- Obesity
- Hypertension
- Traumatic brain injury
- Depression
- Less education in early life
- Sleep disturbances
- Diabetes
- Smoking
- Excessive alcohol
- Social isolation
Groundbreaking Alzheimer’s and cancer studies receive $7.2M boost
Lawson Research Institute scientists and partners will focus on molecular imaging and theranostics to potentially transform the detection and treatment of neurodegeneration and cancer.
The quest to advance detection and treatment of Alzheimer’s disease and to personalize cancer care has received a major boost, with $7.2 million in funding to Lawson Research Institute (Lawson) of St. Joseph’s Health Care London (St. Joseph’s) for first-of-its kind research.
Lawson scientists will partner with a broad team of researchers at London Health Sciences Centre Research Institute (LHSCRI), McMaster University, University Health Network and BC Cancer on the ground-breaking studies focused on molecular imaging and theranostics as a potential game-changer in detecting and treating neurodegeneration and cancer, particularly prostate, brain and breast cancer.
Principal investigator Ting-Yim Lee, PhD, Lawson’s Director of PET/CT Research, and his team of investigators were awarded $2 million through the Ontario Research Fund – Research Excellence for the study titled “Improving Cancer and Alzheimer’s Disease Diagnosis and Treatment Through Cutting-edge Molecular Imaging and Theranostics”. Co-Principal Investigator is radiation oncologist Dr. Glenn Bauman at LHSCRI.
Additional funding from private-sector partners and Lawson, as well as from donors through St. Joseph’s Health Care Foundation, brings the total research investment to $7.2 million.
The research has the potential to offer hope for solutions to some of the most prevalent and pernicious diseases affecting Canadians, explains Lee.
“Both research projects are the first of their kind in Canada aimed at advancing how we diagnose and treat Alzheimer’s disease and cancer,” he says. “This collaborative funding initiative will also drive innovation in the exciting field of molecular imaging and theranostics at St. Joseph’s, at the heart of which is St. Joseph’s new, high-sensitivity GE HealthCare Omni Legend 2 PET/CT – the first in Canada.”
The studies encompass the following:
- Alzheimer’s disease: The new PET/CT at St. Joseph’s allows researchers to simultaneously study both blood flow and glucose metabolism in the brain. Both these mechanisms are believed to be contributing factors in the onset of Alzheimer’s. By measuring both at the same time, the research team hopes to uncover early signs that the brain is in trouble and at risk of plaque deposits and toxic proteins that have been linked to the development of Alzheimer’s.
- Cancer: The cancer study will focus on developing theranostic techniques to achieve personalized dosimetry – a method used to determine the exact amount of radiation a patient should receive during treatment, based on their individual characteristics. This maximizes effective treatment while minimizing harm to healthy tissues.
Molecular imaging and theranostics is a rapidly emerging field of medicine that combines ultra-precise scans and theranostics (a term that melds the words therapeutics and diagnostics). Together, they offer a one-two punch by integrating imaging and radiotracers that can identify the location and extent of diseased tissues and selectively destroy the abnormal cells while leaving surrounding healthy cells undamaged. In collaboration with GE HealthCare, St. Joseph’s is developing Canada’s first GE HealthCare Centre of Excellence in Molecular Imaging and Theranostics.
“By bridging the gap between research and clinical practice, we hope to ease the burden on patients and their families, offering more effective and compassionate care”
-Ting-Yim Lee, PhD, Director of PET/CT Research at Lawson Research Institute.
“We are already seeing the impact of novel theranostics for treatment of men with advanced prostate cancer,” says Bauman. “Promising new theranostic approaches are emerging for many cancers and this investment further positions London to be a leader in this area of research.”
In the initial phase of the studies, 100 patients will be recruited from St. Joseph’s Aging Brain and Memory Clinic at Parkwood Institute for the Alzheimer’s study; while 90 patients will be recruited from London Health Sciences Centre’s Verspeeten Family Cancer Centre for cancer studies. There are plans to recruit patients from the collaborating centres once results from the initial phase are confirmed.
“By bridging the gap between research and clinical practice, we hope to ease the burden on patients and their families, offering more effective and compassionate care,” says Lee. “We are deeply grateful for the opportunity to turn our research into real-world solutions that can make a meaningful impact.”
With dozens of 'firsts' in imaging research, “Lawson is a powerhouse of innovation,” adds Michael Kovacs, PhD, Program Lead, Lawson’s Imaging Research Program, and Lead, Cyclotron & PET Radiochemistry Facility. “We're excited to explore how this work could transform care."
Investing in life-changing research
Through donor support, endowed research chairs are exploring and answering some of the most profound and complex research questions of our time.
Among cherished family photos and special mementos in the office of Jeremy Burton, PhD, is a slightly faded photo of a young woman. Burton points out the framed photo as he enthusiastically talks about his work. It’s a young Miriam Burnett, after whom the Miriam Burnett Chair in Urological Sciences is named. It’s also the first endowed research chair position Burton held at St. Joseph’s Health Care London (St. Joseph’s).
As the research chair for seven years, Burton speaks fondly about the relationship he has with the Burnett family and the crucial role their support has played in advancing his research.
“Thanks to their funding, we became one of the world leaders in urological microbiome research,” he says.
Endowed research chairs at St. Joseph’s receive consistent and sustainable funding so that research leaders and their teams can answer the most profound and complex health questions of our time.
For decades, donors have been inspired by the clinical research taking place at St. Joseph’s and have heavily invested in endowed research chairs. Today, St. Joseph’s Health Care Foundation manages seven endowed chairs focused on several areas, including molecular imaging, fetal and newborn growth and diabetes. Working in partnership with Western University, and with donor support, the foundation recently established four new endowed chairs in mobility, medical biophysics, medical imaging and ophthalmology.
“Medical research in Canada is chronically underfunded, and there is almost no sustainable funding for hospital-based research positions,” says Michelle Campbell, President & CEO, St. Joseph’s Health Care Foundation. “Private philanthropy has filled that gap for years. When a donor gives to an endowed research chair, they are building capacity in the present day and creating future value and opportunity. An endowed gift has a multiplier effect.”
Burton, now the endowed Research Chair in Human Microbiome and Probiotics, has many reasons to be grateful for this support. Not only does the endowed fund pay for Burton’s research salary, it also partially supports the salaries of a lab manager and technical team – all vital for a sophisticated lab to be successful.
The funding also provides the gift of time – a diminishing commodity for any busy research team.
“Scientists need more time to think,” says Burton, a Lawson Research Institute (Lawson) scientist. “We are incrementally being stretched in multiple directions, and the funding gives us the time to do what we are meant to do – find answers to important clinical questions and find solutions to medical problems.”
Distinguished Lawson scientist and university professor Cheryl Forchuk, PhD, wholeheartedly agrees. She recently completed her final term as The Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation & Recovery, another endowed position. As Chair, Forchuk provided scientific and administrative leadership to a large group of researchers based at St. Joseph’s Parkwood Institute focused on mental health, activity and mobility, and cognitive vitality and brain health.
Many research leaders, she explains, can afford to spend only two days a week on their own research projects. Endowed chair positions change that.
“Imagine travelling across the country to create a national study focused on homelessness, two days a week at a time,” she suggests candidly. “You couldn’t.”
Forchuk is referring to her landmark project to better understand how many people in Canada are homeless and who they are. The goal was to develop more accurate sources of data and recommend appropriate support and services. Her work is already resulting in important changes.
Today, Forchuk is embarking on another cross-country research project to find solutions related to homelessness for Canadian veterans who are women.
Like Forchuk, Burton’s Chair position requires him to provide operational and research leadership, including developing research networks and partnerships nationally and internationally to advance studies that will revolutionize care.
“As the Chair, I think it is important that I have wide-ranging projects that benefit people in our own community and beyond,” says Burton, who is optimistic about the outcomes of several of his team’s studies.
He recently partnered with London’s First Episode Mood and Anxiety Program to study the impact of fermented foods on the microbiome of young people taking medications for mental health conditions.
One of the side effects of these medications is weight gain, which deters some patients from taking it. By providing patients with slow-release apple cider capsules, which have similar properties to fermented foods and positively affect the microbiome, they have seen an overall improvement in participants’ mental health and cholesterol after just a few months.
Reflecting on his team’s research achievements to date and the potential of what’s to come, Burton emphasizes how vital endowed chairs are to the sustainability of research and the hope to translate newly discovered knowledge into medical practice.
“Research funding from other sources comes and goes,” he says, “but endowed chair positions that are focused on improving human health provide continuity, build research and create change benefiting all of us.”
Lawson researchers elected to Royal Society of Canada
Drs. Cheryl Forchuk and Ruth Lanius have been elected as Fellows with the Royal Society of Canada (RSC) in recognition of their significant contributions to mental health research.
Dr. Forchuk, Assistant Scientific Director at Lawson and the Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery at St. Joseph Health Care London’s Parkwood Institute, has worked tirelessly to advance research that has resulted in improved hospital discharge models, harm reduction strategies and support for those living without housing, among other concerns. Most recently she has hosted forums across Canada in an effort to better understand homelessness and the number of people experiencing it.
“It’s an honour to be included among such a talented group and alongside my mental health colleague,” says Dr. Forchuk, who is also a Distinguished University Professor at Western University. “A lot of important work remains to be done to better support those living with mental health challenges.”

Dr. Lanius, Associate Scientist at Lawson and Psychiatrist at London Health Sciences Centre, is world-renowned for advancing the understanding and treatment of post-traumatic stress disorder (PTSD) through her research. She has been instrumental in defining different types of PTSD and combining imaging and psychiatry to develop new therapies that use neurofeedback or sensory processing to ‘train the brain.’
“Advancing knowledge is crucial to improving quality of life,” notes Dr. Lanius, who is also the Harris Woodman Chair in Mind-Body Medicine and a Professor at Western’s Schulich School of Medicine & Dentistry. “I’m very excited to be recognized with such a distinguished group of contributors to research and academics.”
RSC fellows are elected by peers for their outstanding scholarly, scientific and artistic achievement. This year’s 101 new fellows will be inducted into the RSC on November 17.
London researchers part of a federal funding boost to enhance transition in care research
How can we improve health care for Canadians experiencing “transitions in care” to ensure they don’t fall through the cracks as they move through the health care system?
That’s the question two London researchers are aiming to answer, with the support of nearly $1.5 million in federal funding announced today at Western University's Schulich School of Medicine & Dentistry.
Peter Fragiskatos, MP for London North Centre, announced the funding boost on behalf of Federal Health Minister Jean-Yves Duclos, alongside Dr. Jane Rylett, Scientific Director of the Institute of Aging with the Canadian Institutes of Health Research (CIHR).

“When a person experiences a transition in care, whether moving from surgery to rehabilitation or aging out of pediatric care, the quality of their care and their health can be at risk,” said Bryan Neff, Western’s acting vice president of research, who hosted the funding announcement. “With federal investments like this, Western will continue to lead the way in identifying how to provide the best possible care for Canadians while improving efficiency in the health-care system.”
Transitions in care happen when responsibility for a person’s care shifts between providers, institutions or sectors. Some groups, such as patients with complex medical conditions, Indigenous peoples, and new immigrants, are particularly vulnerable to poor outcomes during transitions.
People with diabetes – a complex, typically life-long condition – fall into this category, which is why London’s Primary Care Diabetes Support Program (PCDSP) was developed. The clinic, which is part of the Centre for Diabetes, Endocrinology and Metabolism at St. Joseph’s Health Care London, is based at St. Joseph’s Family Medical and Dental Centre. The program provides diabetes support and management for individuals with type 2 diabetes who don’t have a family doctor or who may have additional medical and social issues that make diabetes management particularly challenging.
Maria Mathews, PhD, and her team at Schulich Medicine will evaluate the program to determine its impact on patient health, and on health-care providers, diabetes-related complications, and health system costs.
“While this program has already been shown to deliver high-quality care, my team is examining its overall impact to determine whether this model could be expanded to other sites and to support other chronic conditions,” said Mathews, a professor in the department of family medicine. With the $895,000 investment in her research, Mathews will determine “how we can best provide high- quality care for people with chronic conditions in a way that supports their health, eases strain on family doctors, and creates efficiencies in the health care system.”

Laura Brunton, PhD, an assistant professor at the School of Physical Therapy in Western’s Faculty of Health Sciences, received more than half a million dollars in CIHR funding.
Her team will examine a local program based at St. Joseph’s Parkwood Institute – called the Transitional and Lifelong Care Program (TLC) – that supports people with childhood-onset disabilities as they transition to adult care. This includes many patients with brain-based, neurodevelopmental conditions, such as cerebral palsy, spina bifida and developmental disabilities, as they move into adult care.
“Many of these patients have experienced severe health inequities because of the gaps in care when transitioning from pediatric care to the adult sector,” said Brunton, also a physiotherapist at St. Joseph’s Health Care London and affiliate scientist at Lawson Health Research Institute. “We’re going to evaluate the TLC model as an intervention that provides transitional, lifelong care and reduces the barriers experienced.”
Roy Butler, president of St. Joseph’s Health Care London, said today’s announcement highlights the synergy and collaboration among these organizations.
“We are happy to hear that work being done by both Laura Brunton and Maria Mathews to improve patient care is being recognized through this funding announcement. The two areas these talented researchers will be studying are innovative and ground-breaking with compassionate, forward-thinking teams who provide highly acclaimed care to vulnerable patients.”

Fragiskatos emphasized the vital importance of funding this field of research, given that most Canadians will experience a ‘transition in care’ at some point.
“People living in Canada routinely experience transitions in care as they navigate the health system. The important research that will be done here in London and at institutions across the country will help develop meaningful approaches to make these transitions easier for patients and caregivers,” he said.
Local researchers were among 14 groups across Canada that received approximately $12 million in federal funding to improve continuity of care for Canadians through the “Transitions in Care” initiative, which is provided in partnership with the Azrieli Foundation, Mitacs, and the Rossy Family Foundation.
Revolutionizing rehab
St. Joseph’s Health Care London is taking giant strides in the science of rehabilitation and movement, with direct benefit to patients.
St. Joseph’s is setting a long-time vision into motion.
“Five years ago, we had a vision of leveraging our long history and expertise in providing innovative rehabilitation treatments to improve the lives of people with mobility needs on a larger scale,” says Roy Butler, President and CEO of St. Joseph’s Health Care London (St. Joseph’s). “That dream has come to life.”
While experts at St. Joseph’s had the knowledge, innovative spirit and passion to achieve the vision, they needed a partner who shared the same enthusiasm.
William and Lynn Gray answered that call. With their generosity and ground-breaking investment, The Gray Centre for Mobility and Activity was created.
“Lynne and I are very pleased with the steady forward advancement of the centre’s mission since its establishment just a few short years ago,” says Bill Gray. “The innovative thinking and idea generation that seeks new solutions to the issue of mobility have really taken root. We hoped that The Gray Centre would have an impact on care ... and it has.”
“We’ve watched the development of The Gray Centre with enormous pride and are pleased to have our name associated with it, and the excellence it stands for,” adds Lynne Gray.
A unique concept
Established in 2020, The Gray Centre at St. Joseph’s Parkwood Institute is a regional hub focused on researching leading-edge treatments and interventions in mobility and activity. The centre’s unique model of linking research and care allows researchers to work side-by-side with clinicians, patients, and caregivers to uncover optimal methods for maintaining mobility throughout a person’s life.
“Scientists at The Gray Centre are leading the way in integrating technology and solutions in care to better understand how we can enhance each patient’s treatment plan to improve their functionality and ability to move,” says Butler.
Pioneering Research
More than 50 ongoing rehabilitation research projects at Parkwood Institute are exploring areas such as spinal cord and traumatic brain injury rehabilitation, pain, outcomes for amputees, virtual exercise and cognitive behavioral therapy, gait analysis as a measure of dementia progression, and stroke rehabilitation and recovery.
The Gray Centre is a catalyst and connector for these projects by investing in cutting-edge technology, providing seed grants, embedding researchers from Western University, leveraging clinical expertise, attracting world-class researchers and translating new knowledge into clinical practice by training students and clinicians, and fostering sustainable practice change.
More than $1.3 million granted through St. Joseph’s Health Care Foundation has advanced work at The Gray Centre over the past year. From researcher support to new equipment such as two transcranial magnetic stimulators, a portable handheld ultrasound and several sensored mats for gait assessment donors have stepped up to advance this work.
Leadership with Purpose
At the helm of The Gray Centre is Siobhan Schabrun, PhD, a world-renowned neuroscientist and the inaugural William and Lynne Gray Research Chair in Mobility and Activity. Thanks to a partnership with Western University’s Faculty of Health Sciences and Schulich School of Medicine & Dentistry, donor funding for the chair made through St. Joseph’s Health Care Foundation was matched, creating a $5-million endowed position.
Schabrun’s innovative research benefits people suffering from chronic pain. With a focus on non-invasive brain stimulation techniques to enhance neuroplasticity and improve mobility and activity outcomes, she and her team are, in essence, retraining the brain’s pain response. This innovative work bridges the gap between neuroscience and rehabilitation, offering new hope for individuals with musculoskeletal and neurological conditions.
Originally trained as a physiotherapist with a PhD in neuroscience from the University of Adelaide in Australia, Schabrun has attracted more than $15 million in competitive research funding and written or contributed to more than 140 scholarly publications.
FLOATing Forwards
The newest advancement is a first-in-Canada and a marvel of medical engineering that is transforming options in rehabilitation research and practice.
The Reha-Stim Medtec FLOAT system at St. Joseph’s Parkwood Institute enables patients with mobility limitations to walk, supported, without fear of falling. They "float" in a controlled environment using a combination of robotics, body-weight support and real-time feedback. The device has a harness attached to a robotic arm, which adjusts the level of support based on the patient's movements. Sensors provide continuous feedback for maximum learning and greatest benefit to physical therapists and patients alike. The FLOAT system has shown significant improvements in patients' mobility, balance and overall functional independence.
“Innovative equipment like the new FLOAT System is an example of the type of innovation that does not exist anywhere else in Canada,” says Bill Gray. “The real-life application of technologies like this are what The Gray Centre is intended to be about.”
Through the combined efforts of dedicated professionals, cutting-edge technology and philanthropist partners, St. Joseph’s Gray Centre has combined vision with passion and is transforming lives, one step at a time.
Standing up to falls
By merging world class care with research and artificial intelligence, St. Joseph’s Health Care London is catching falls before they happen.
They wreak havoc on independence and well-being, making them one Canada’s most pressing health challenges: falls.
A leading cause of injury-related hospitalizations, even death, among older adults, a fall can happen anytime, anywhere – with 50 per cent occurring at home. But what if we could predict and prevent falls before they happen?
A pioneering initiative at St. Joseph’s Health Care London (St. Joseph’s) is doing just that. The 3FM Clinic, short for Falls, Fractures, Frailty and Mobility, at St. Joseph’s Parkwood Insitute is at the leading edge of falls prevention in Canada, integrating research with clinical practice to offer hope and practical solutions to older adults.
Led by St. Joseph’s geriatrician Dr. Jaspreet Bhangu and Western University rehabilitation scientist and physiotherapist Janelle Unger, PhD, the visionary 3FM Clinic is working to prevent falls before they happen.
“We know there are a number of factors that can cause an older adult to fall such as illness, medication side effects, balance and gait issues, cognitive impairment, visual changes and environmental hazards,” says Bhangu. “What we’re working to understand is how those factors together impact individual patients and their risk of falling.”
To do so, the 3FM Clinic team – one of the largest, most diverse teams of its kind in the country – completes a multi-step evaluation of patients:
- Nurses gather their medical history, current medications, functional abilities and personal goals.
- Physical therapists measure the patient’s gait (how they walk) and balance to understand their physical capabilities.
- Occupational therapists test their vision, cognitive function and identify issues that might hinder the individual’s ability to perform routine tasks safely.
- A geriatrician focuses on medical risk factors such as bone health, medications and cardiovascular health to help manage risks associated with aging. The team then creates a customized care plan that incorporates exercises, therapeutic interventions and educational strategies.
On the research side, Unger and her team in the RED Neuro Lab at St. Joseph’s Gray Centre for Mobility and Activity are leveraging artificial intelligence (AI) to predict falls more accurately.
“Traditional fall prediction models often rely on limited data and lack real-world input from clinicians and patients,” explains Unger. “By partnering with Bhangu and the clinical team, as well as the patients in the 3FM Clinic, we’re able to integrate clinical information with biomechanical data collected from wearable sensors known as inertial measurement units (IMUs).”
An IMU is a device that tracks and measures a person’s movement and orientation and provides valuable data on how that person moves and stays stable.
“We plan to use AI to analyze the data collected through the IMU’s and are working to create accurate fall prediction models,” says Unger. “This research, funded by Western’s Bone and Joint Institute, has the potential to improve care decisions, enhance preventive strategies and ultimately reduce the incidence of fall-related injuries and hospitalizations for our patients and people across the globe.”
By embracing innovative research and compassionate care, the 3FM Clinic is a model for future efforts in fall prevention and geriatric care, offering a safer, more independent future for older adults.
You can prevent falls too:
- Use assistive devices: Properly fitted walkers or canes provide essential support and stability.
- Fitted footwear: Shoes (not slippers or flip-flops) with appropriate tread and low heels help prevent slips and falls. They should also fit your feet.
- Home improvements: Improved lighting, clear walkways and assistive bathroom fixtures.
- Exercise: Participate in strength and balance exercises to enhance physical fitness.
- Medication reviews: Regularly have your medications reviewed to identify if you are at risk of falling.
Study aiming to slow cognitive decline in older adults gets $1.5M
Led by Dr. Manuel Montero-Odasso and his team at Lawson Health Research Institute, the first large-scale Canadian clinical trial using personalized lifestyle intervention delivered at home to help older adults with mild cognitive impairment is getting underway with support from a Weston Foundation grant of $1.5 million.
Mild cognitive impairment (MCI) is an intermediate stage between the expected cognitive decline of normal aging and the more serious decline of dementia. There is growing evidence that enhancing physical activity, stimulating cognitive training and addressing cardiovascular factors could delay or prevent the decline to dementia.
Part of the Canadian Consortium on Neurodegeneration in Aging (CCNA), the SYNERGIC-2 trial will provide virtual at-home interventions to 550 study participants with MCI, including personalized one-on-one coaching, to help make lifestyle and behavioural changes. This trial builds upon the successful SYNERGIC-1 trial, which used face-to-face interventions, by delivering them remotely using digital technology.
These interventions will target five areas including physical exercise, cognitive training, diet recommendations, sleep interventions and vascular risk factor management, with the goal of enhancing health and maintaining independence for individuals at risk for developing dementia.

“There are important risk factors related to exercise, diet, sleep and socialization,” says Dr. Montero-Odasso, Lawson Scientist, Geriatrician at St. Joseph’s Health Care London’s Parkwood Institute and a Professor at Western University. “If we can make the brain a little healthier with multiple lifestyle interventions, we may be able to delay or even prevent dementia.”
The year-long study includes 35 researchers recruiting a diverse population of older adults with MCI across 10 Canadian cities. The research teams are currently looking for participants ages 60-85 with MCI and additional dementia risk factors.
Researchers have created a digital platform to deliver the interventions at home with effective coaching strategies that will help to overcome barriers to lifestyle interventions, like difficulty accessing intervention sites, lack of time to attend gym sessions or living in rural/remote areas.
“There are many Canadians who are at high risk of developing dementia, based on their family history and genetics,” explains Dr. Howard Chertkow, Chair of Cognitive Neurology and Innovation at Baycrest Health Sciences, Scientific Director at CCNA and a co-investigator on the study. “Other risk factors include having high blood pressure and diabetes. We have seen that we can reduce the risk of getting dementia if we can get people to improve their lifestyles in multiple ways.”
Those interested in taking part in the study can contact @email for additional details.
The study is part of a global initiative known as World-Wide FINGERS, an interdisciplinary network working on the prevention of cognitive impairment and dementia, and is supported by The Gray Centre for Mobility and Activity at St. Joseph’s.
World Labyrinth Days highlight how this form of ‘walking meditation’ can benefit everyone
Following a labyrinth is a spiritual practice that’s good for body, mind and spirit.
It leads to increased calm, reduced blood pressure and stress, and improved mental health and well-being, say researchers and patient care experts at St. Joseph’s Southwest Centre for Forensic Mental Health Care (Southwest Centre).
On World Labyrinth Days - May 3 and May 4, staff, patients and residents at St. Joseph’s are invited to join thousands across the globe who “walk as one at 1 pm.”
While books and movie culture often show labyrinths as places where people get hopelessly lost, ground-breaking studies conducted through Lawson Health Research Institute show labyrinths can be just the opposite: they’re places people can find hope and find themselves.
Unlike mazes that are puzzles with many choices and many dead ends, labyrinths have continuous lines that lead to and from the centre.
“Walking a labyrinth is a form of walking mediation,” says Rev. Stephen Yeo, spiritual care practitioner at Southwest Centre and a Lawson researcher. “It is a wonderful way to look after one’s body, mind and spirit. It is a very inclusive practice, regardless of how you engage the sacred in your life and in the world.”
There are two permanent labyrinths at Southwest Centre – one indoors and one outdoors. In addition, this spiritual tradition is available at all St. Joseph’s sites. The Parkwood Institute Mental Health Care Building has an indoor labyrinth in the Multifaith Room and an outdoor labyrinth as well—all of them suitable for people who walk or wheel.
In addition, Mount Hope and St. Joseph’s Hospital each have finger labyrinths available for meditation in their multifaith rooms. Other labyrinth opportunities exist across sites including an opportunity to walk a portable labyrinth at the Parkwood Institute Main Building in the Multifaith Room every Friday at noon.
Southwest Centre in Elgin County also has a portable labyrinth, with lines painted on canvas, that’s often used at other locations. “Have labyrinth, will travel,” Stephen quips.
For nearly a decade, he has facilitated walking labyrinths at Southwest Centre with larger groups during seasonal times of solstice and equinox, as a purposeful step that’s also part of truth and reconciliation practices with Indigenous peoples.
“While it may be world labyrinth day this weekend, it’s labyrinth day here at Southwest Centre regularly as something that’s incorporated into our care and practice,” Stephen says.
The research team’s work examining the benefits of labyrinth-walking in a forensic mental health care setting has been cited globally.
Says principal investigator Clark Heard, “I see significant benefit in labyrinth-walking in settings such as mental health care facilities, although I would stress that these benefits could also be generalized to any participant in a community setting.”
“Walking a labyrinth is a regenerative and restorative experience that helps people connect with the personally sacred,” says Clark, who is an occupational therapist at Southwest Centre and is an Associate Scientist at Lawson.
They promote self-care, hope, resilience and coping. They help connect people to the spiritual side of themselves and to relationships sacred to ourselves and the environment.
“Our team’s work identified that labyrinth participation can support meaning-making in the most difficult of circumstances, while at the same time making room for important aspects of mental wellness such as the quest for hope and search for meaning,” Clark says.
Stephen first walked a labyrinth three decades ago during a retreat at a monastery in Winnipeg. It became part of his regular practice of engaging the sacred in his life, and he is now a certified labyrinth facilitator.
“A labyrinth is so simple that you don’t need someone to lead you through. Whether it's facilitated or not, a person inevitably benefits from walking one,” he says.