Search
Search
Team players: FMT and microbiome research could have widespread impact
There is still much to learn about the human microbiome and its role in fighting disease, but ongoing studies at Lawson Health Research Institute, including a focus on fecal microbial transplants (FMT), are making strides in harnessing this complex system.
FMT is being studied in connection with conditions as varied as non-alcoholic fatty liver disease, rheumatoid arthritis, atherosclerosis, HIV, cancer and multiple sclerosis.
FMT is already in clinical use for the treatment of C. diff (Clostridium difficile), and in addition to showing promise in the treatment of other diseases, it is also being studied as a way to improve response to existing cancer treatments and ease treatment side effects.
Dr. Saman Maleki, a Scientist at Lawson Health Research Institute and the London Regional Cancer Program (LRCP) at London Health Sciences Centre (LHSC), says they’ve just begun to explore the possibilities.
"We are just starting to study FMT as an intervention outside its traditional use in patients with C. difficile infection, and we will be expanding to other areas, particularly in cancer.”
FMT can overhaul a patient’s microbiome, Dr. Maleki explains, and a healthy microbiome is beneficial especially when a treatment is trying to activate the body’s immune system.
Dr. Michael Silverman, Lawson Associate Scientist and Medical Director of St. Joseph’s Health Care London’s Infectious Diseases Care Program, is a pioneer in the field of FMT. He has been performing the procedure since 2003 with C. difficile patients and was one of the first in North America to do so. He sees a wide range of possible applications.
“FMT has enormous potential in being an important adjunctive therapy in many cancers. It may, for example, help cancer patients respond to immunotherapy,” says Dr. Silverman, who is also Chair/Chief of Infectious Disease at St. Joseph’s Health Care London, LHSC and Western University. “The potential to impact autoimmune and metabolic diseases is also quite exciting, but still in early development.”
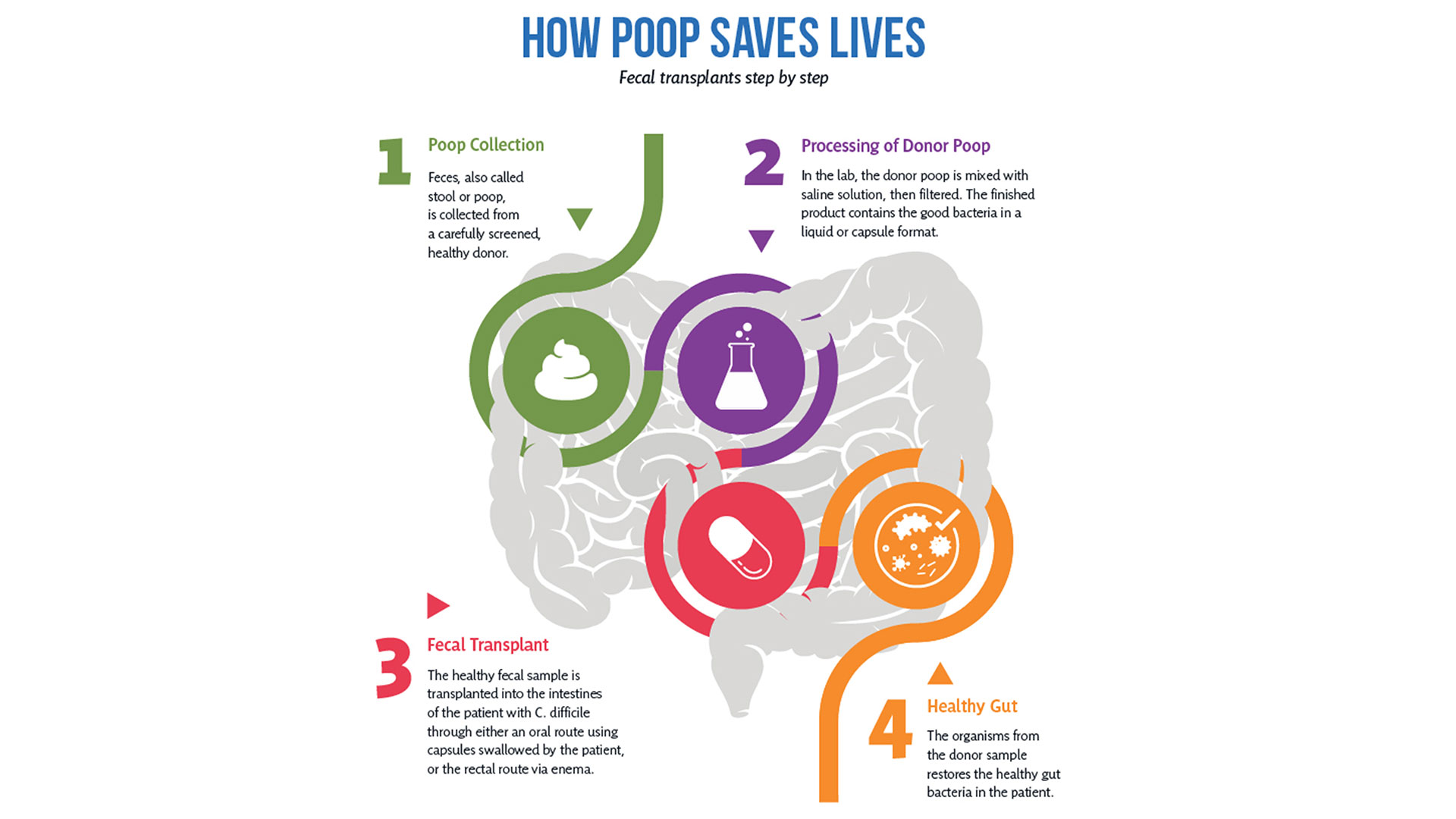
So how does it work?
After rigorous screening, stool from a healthy donor is collected and then processed in a lab into a liquid or capsule containing the good bacteria, which can then be administered to a patient’s gastrointestinal tract.
The Lawson team is also one of few delivering FMT using specially-prepared oral capsules. Introduced in 2018, they have been a game changer in patient acceptance and ease of administration, according to Research Coordinator Dr. SeemaNair Parvathy, who has been coordinating the program since 2015.
“There is a link between the fitness of the intestinal microbiome and the fitness of the immune system,” says Dr. John Lenehan, Associate Scientist at Lawson and Medical Oncologist at LHSC. “A ‘healthy’ microbiome leads to a more robust immune response when using immunotherapy. FMT from a healthy donor is expected to improve the fitness of the recipient’s intestinal microbiome and promote a better immune response.”
People with chronic disease can often experience what’s called a ‘leaky gut,’ allowing food, bacterial and microbial components to pass through the intestinal wall, negatively impacting the immune system.
“When people get FMTs their intestinal permeability improves – meaning it actually reduces,” says Dr. Jeremy Burton, Lawson Scientist and Research Chair of Human Microbiome and Probiotics at Lawson and St. Joseph’s. “What changes that intestinal permeability? The microbes at the site. They play a role in interacting with the host cells, providing nutrients and vitamins.”
With the immune system so closely tied to the health of the microbiome, it’s not surprising scientists are exploring how strengthening one can have a big impact on the other.
Boosting immunotherapy
Immunotherapy can be used to either stimulate or suppress the immune system to help the body fight disease, and FMT is showing promise in reducing resistance to the treatment.
While immunotherapy has been effective in treating a number of cancers – the number one cause of death in Canada – not all patients respond to the treatment.
But early work presented at a conference by the Lawson team for the Journal for ImmunoTherapy of Cancer has shown that using FMT to modify the microbiome could reduce resistance to immunotherapy. The study involved patients from LHSC with advanced melanoma, a type of skin cancer.
While in the very early stages, the combination of FMT and anti-PD1 immunotherapy has been found to be safe, and it appears that FMT could make tumours more responsive to the immunotherapy treatment.
“Microbiome-based treatment strategies, including FMT, have a high potential in oncology,” says Dr. Maleki. “Our team is also exploring its potential in treating pancreatic cancer.”
The research is so interesting that a recent Nature article listed the Phase I melanoma trial as “seminal” research. The study was also unique in that it used healthy donors, as opposed to donors who had previously responded to immunotherapy treatment.
A separate Lawson study with LHSC patients with metastatic renal cell carcinoma, a type of kidney cancer, published in the Journal of Clinical Oncology, also looked at combining immunotherapy and FMT to ease the adverse effects of the treatment.
The Phase I study, led by Dr. Maleki and Dr. Ricardo Fernandes, Medical Oncologist at LHSC, found adding FMT to doublet immunotherapy was safe, but further study is needed to determine whether it could bring about changes in the microbiome and immune system.
Dr. Lenehan says Lawson researchers are in a position to be leaders in this field in the near future for two reasons.
“One is that other academic researchers have not been able to assemble the expertise, and some who have, do not have the access to healthy donor stool. The second is that some biotechnology companies are interested in FMT, but almost exclusively for C. difficile infections.”
Autoimmune, metabolic and other illnesses
Two other areas that have seen recent advances include FMT for the treatment of non-alcoholic fatty liver disease (NAFLD) and multiple sclerosis.
“The gut microbiome is very important in the metabolism of foods and metabolic products. It can therefore have a major effect on obesity and atherosclerosis,” says Dr. Silverman. “It also is tightly involved in regulating the immune system and therefore moderating the microbiome may potentially impact autoimmune diseases.”
A study published in 2020 by the team in The American Journal of Gastroenterology showed that FMT appears to reduce intestinal permeability in patients with NAFLD.
The number of people with NAFLD is growing rapidly and studies show patients have different microbiota than healthy persons.
The trial included 21 NAFLD patients from LHSC and St. Joseph’s. While the researchers found no changes in percentage of liver fat or insulin resistance, they observed significant reduction in intestinal permeability in those patients who had elevated intestinal permeability at the study’s start (seven patients in total). They also observed changes to the gut microbiome in all patients who received a fecal transplant from a healthy donor.
“Metabolic syndromes including obesity and its complications of NAFLD and atherosclerosis are massive public health problems. Any impact on these would be of huge importance,” Dr. Silverman adds. “Autoimmune diseases also cause major morbidity and mortality. We have a lot of work to do before we can consider FMT as a routine therapy for any of these conditions, but the long-term promise is great.”
Research into the use of FMT for treatment of patients with multiple sclerosis is in the very early stages. But patients with MS show a difference in gut microbiota and higher small intestine permeability, which could contribute to the development of the disease.
A Phase I trial by the Lawson team published in the Multiple Sclerosis Journal – Experimental, Translational and Clinical, found FMT to be safe and tolerable.
While the study was very small, MS patients treated with FMT were found to have beneficial changes to gut microbiota and intestinal permeability, but further study is needed to determine if FMT could be used as a treatment.
Lawson scientists are also currently studying the use of FMT for patients with atherosclerosis, along with ongoing studies on melanoma and lung cancer. Funding for a study on pancreatic cancer has been secured and researchers are in the process of planning trials for a number of other applications.
Dr. Lenehan says, “The microbiome is connected to several diseases and their treatments. Evidence is growing that an individual’s health is related to their microbiome.”

The donor challenge
The challenge of finding fecal donors for FMT and the cost of that process remain an issue for research into this promising treatment, even as more potential applications are discovered.
There is currently no process in place to match donors and recipients – as with organ donation – but there is an extensive screening process for both infectious and non-infectious conditions, one that needs to be repeated if a donor experiences any lifestyle changes.
Dr. Burton says, “We still don't understand the full role of the microbiota. We have to ensure that we're not giving patients a microbiota that might cause them some other issue in the future, so the donors are screened very thoroughly for that.”
Screening also excludes donors with an increased risk of developing the diseases scientists are hoping to treat, such as metabolic syndrome related conditions.
A 2017 article published in Open Forum Infectious Diseases by Drs. Silverman and Burton found the cost of screening high numbers of potential donors could make establishing local programs extremely difficult, so having a central program such as the one in London could help patients in many regions.
In the study, only five of 46 potential donors passed the history, examination, blood, stool and urine tests, and of the five, four later travelled or had illnesses that made donation inadvisable.
The search continues in London for potential donors to help drive this research forward. You can read one donor’s story and learn how you can get involved here.
More on FMT and the microbiome:
Drugs vs. bugs: Harnessing the microbiome to improve treatments
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
The invisible world inside us
The human microbiome is a wonder of nature.
Trillions of microbes call our body home. They live in our gut and many other places throughout our body. They are involved in virtually every aspect of how we function and we are learning that they are essential to staying healthy. An unhealthy microbiome has been linked to many diseases from allergies to cancer and even mental health.
Most people out there have heard about probiotics and fermented foods, and chances are you’re trying to get more of them in your diet.
Drinking kombucha or eating yogurt, anyone?
Join Lawson Health Research Institute for our next Café Scientifique event, "The invisible world inside us: Exploring the human microbiome."
Hear from a panel of researchers who are unraveling the mysteries about the microbiome and using that knowledge to improve health and health care. They will also bust some myths and share the important facts when it comes to probiotics, prebiotics and the microbiome.
Image

SPEAKERS
- Dr. Gregor Reid, Lawson Scientist and Professor of Microbiology & Immunology and Surgery at Western University.
Presenting: Probiotics and Prebiotics - Look beyond the fake news - Dr. Michael Silverman, Lawson Associate Scientist, Chair of Infectious Diseases, Schulich School of Medicine & Dentistry at Western University and Chief of Infectious Diseases for St. Joseph’s Health Care London and London Health Sciences Centre.
Presenting: Fecal Transplants: What does this crap have to do with me? - Dr. Jeremy Burton, Lawson Scientist and Assistant Professor of Surgery (Urology) and Microbiology & Immunology at Western University.
EVENT DETAILS
Date: Wednesday, November 27, 2019
Time: 7-9 pm (doors open at 6:30 pm)
Location: Best Western Plus Lamplighter Inn & Conference Centre (Regency Room), 591 Wellington Rd, London, ON N6C 4R3
Map and directions.
Parking: Free on-site parking
This is a free event and online registration is REQUIRED.
Registration for this evengt is now FULL.
Please fill out the form here to be added to the waitlist.
You will be notified should a spot open up.

Third-party review of animal research at Lawson Research Institute, St. Joseph’s Health Care London
In August 2025, members of our community raised concerns about our animal research program at Lawson Research Institute (Lawson). While we were confident we followed all regulations and ethical standards, we commissioned an independent third-party review of animal research at Lawson and indicated we would make the results of that review public.
What the third-party review found:
- Lawson met all regulatory, ethical and professional standards in animal research.
- There was no evidence of intentional secrecy, concealment or avoidance of oversight. The research is reported in peer-reviewed publications, grant disclosures and academic presentations - all available to the public.
- No other animal or non-animal model could have been used to achieve the translational outcomes the researchers were trying to achieve.
What areas of improvement did they identify?
Recommendations include improved communication between St. Joseph’s, Lawson, Western University and Western’s Animal Care Committee, with clear accountabilities for decision making, to ensure all parties are aware of their unique roles and responsibilities, to update shared agreements and policies, including transparency plans and enhance the process for reporting of concerns.
What other reviews were completed?
- Western Animal Care Committee Report
- Canadian Council on Animal Care Special Assessment Report
- Ontario Ministry of Agriculture, Food and Agribusiness inspection Report
The majority of the key findings of these reports align with those of the third-party panel.
What’s next?
We are developing an action plan to address all recommendations and are working with our partners on next steps.
Animal research remains an important part of medical discovery. The life-saving imaging approaches developed at Lawson are now standard of care worldwide for people suffering from heart disease and heart attacks. We are immensely proud of the work our researchers conduct every day to save and improve lives.
Thank you,
Roy Butler, PhD
President and CEO
Jeremy Burton, PhD
Interim Vice-President
Research and Scientific Director Lawson Research Institute
This will be a huge benefit for society because sepsis is the leading cause of death worldwide
It’s a discovery that has been more than ten years in the making: the use of a human protein to potentially treat patients with sepsis.
Lawson Scientist Dr. Qingping Feng noticed that a human protein called annexin A5 showed positive results with sepsis back in 2007.

Fast forward 14 years later to now, and this discovery could very well be the first ever viable treatment for sepsis patients, including severe COVID-19 patients who develop sepsis. “With COVID initially, it is in the airway and then in the lungs, then from there the inflammatory response in fact spreads to the whole body,” says Dr. Feng, Ivey Chair in Molecular Technology at Western University's Schulich School of Medicine & Dentistry. “Sepsis causes major organ dysfunction and carries a high mortality unfortunately.”
It has become a challenging issue for Intensive Care Physician at London Health Sciences Centre (LHSC), Dr. Claudio Martin, who can only do so much to treat severe COVID-19 patients that develop sepsis.
“What we have seen is a very primary severe respiratory failure to the lungs for severe COVID patients,” says Dr. Martin, Associate Scientist at Lawson. “We have used steroids and other treatments to try to help, but the results and effects aren’t dramatic and we see patients who have these treatments and still progress and end up in the ICU.”
However, Dr. Feng and his team has found in a pre-clinical study, that annexin A5 can inhibit inflammation, improve organ function, and survival when treating sepsis.
Another potentially deadly situation for COVID-19 patients is cell death and blood clots, specifically near the lungs. The good news is that the research team also believes the annexin A5 drug will prevent these complications through the drugs anti-apoptotic (cell death prevention) and anti-coagulant (blood clot prevention) properties.

Supported by provincial funding through Ontario's COVID-19 Rapid Research Fund, the research team has launched a clinical trial with critically ill COVID-19 patients at LHSC, using a manufactured form of annexin A5. The goal is to enroll a total of 60 patients for the clinical trial, and enrollment has already begun. “Patients are receiving standard treatment and then those enrolled will also receive the annexin,” says Dr. Martin. “It’s a placebo blinded clinical trial, so patients will either get a lower dose of annexin, a higher dose of annexin, or a placebo.”
If the clinical trial shows promising results, Dr. Feng says the team plans on expanding into a larger phase three trial with not just COVID-19 patients with sepsis, but other sepsis patients as well. “If in fact annexin A5 is shown to be effective in sepsis, then this will be a huge benefit for society because sepsis is the leading cause of death worldwide.”
The drug is currently being produced through a partnership with Suzhou Yabao Pharmaceutical R&D Co., Ltd., based in China, Lawson Health Research Institute, and WorldDiscoveries. “Our long-standing partnership with Suzhou Yabao has enabled annexin A5 drug development to proceed to this point,” says Kirk Brown, Manager of Business Development, Lawson Health Research Institute. “We are now in a unique position through this trial to offer a potential life-saving treatment for this emergent global disease, with the objective of soon expanding to all cause septic patients.”
Time for Canada to reclaim its place as a leader in scientific discovery
The following editorial was provided to Post Media by Dr. David Hill, scientific director, Lawson Health Research Institute.
Last week the Nobel Prizes for 2017 were announced, recognizing incredible advances in science that will impact all our lives for the better. If you were looking for Canadian scientists amongst the teams, you would be disappointed.
According to a federal government report commissioned by the minister of science titled Investing in Canada’s Future — Strengthening the Foundations of Canadian Research and released in April, Canada’s momentum in the sciences has never been worse.
Our country’s investment in key emerging areas such as artificial intelligence, clean technology, nanotechnology, immunotherapy, bioinformatics or bio-engineering is flat-lined or declining, and falling seriously behind competitor nations.
We are not talking about matching the United States or Germany. Canada invests less in science research and development relative to gross domestic product than does Taiwan or Singapore.
Why should we care?
Because smart science delivers technologies we take for granted every day, such as Siri on our iPhones, minimally invasive surgery and secure online banking.
Science also creates companies, delivers high-paying and rewarding jobs, and is the backbone of the economy.
In London, Ont., jobs that depend on advancing science include those at Lawson Health Research Institute, the research institute of London Health Sciences Centre and St. Joseph’s Health Care London and where I work; academic institutions such as Western University and Fanshawe College; and local businesses generating health devices, computer software and engineered products. A lack of investment in science could be devastating to our city.
This report places the failure to invest in science at the door of successive federal governments during the past decade.
Of course, it is not only government that should invest in science. It is industry that takes proven scientific findings and translates them into products we all consume.
But these innovative products need to start somewhere, most often in the laboratory. Fostering high risk, fundamental discovery science should be a core responsibility of government in a knowledge-driven economy.
In Canada, the contribution of federal funds to discovery science is now below 25 per cent of the total research investment, and lower than most of our competitor nations. Consequently, research funds are scarce, laboratories are closing, fewer students are receiving advanced training, and fewer new businesses are emerging.
It is not too late.
The report provides evidence to show that Canadian scientists are still respected leaders in their fields. The engine simply needs fuel.
To return Canada’s discovery science enterprise back to 2006 productivity levels, we require an additional investment of $1.3 billion during four years, representing 0.1 per cent of the entire federal budget for each of those years.
The investment quickly pays for itself. Every $1 invested in fundamental research has been calculated to return $2.20 to $2.50 in direct and indirect economic activity.
Next year’s federal budget is being put together right now in Ottawa, and we have an opportunity to reclaim our past reputation as a discovery nation; a nation that brought the world insulin, the Canadarm, Pablum, canola and the electron microscope.
The journey toward that next Canadian Nobel Prize needs to start now.
Dr. David Hill
Scientific Director
Lawson Health Research Institute
Tomorrow’s scientists tour Lawson research facilities
A group of senior chemistry students from H.B. Beal Secondary School visited Lawson Health Research Institute (Lawson) facilities at St. Joseph’s Hospital on Wednesday, November 8. In addition to learning about Lawson’s world-renowned imaging research, the group toured the Cyclotron and PET Radiochemistry Facility and Dr. Alexandre Legros’ brain stimulation lab.
The students first learned about Lawson’s simultaneous PET/MRI – the first in Canada – and its associated research. Led by Dr. Jonathan Thiessen, Lawson imaging scientist, the presentation focused on the benefits of combining Positron Emission Tomography (PET) with Magnetic Resonance Imaging (MRI) across multiple disciplines.

Above: Dr. Jonathan Thiessen discusses Lawson's simultaneous PET/MRI
Benjamin Wilk, a PhD candidate working under Dr. Thiessen’s supervision, presented on his research which is focused on developing methods to image the heart after myocardial infarction, or heart attack, using PET/MRI. Qi Qi, another of Dr. Thiessen’s PhD candidates, discussed his research that looks at multimodal imaging to evaluate tumour perfusion and glycolysis in brain tumours.
"It is an incredible opportunity to present our work to high school students,” said Dr. Thiessen. “By seeing examples of the research happening in their own community, my hope is that some of them will be inspired and work hard to become the scientists and healthcare professionals of tomorrow."
The students were then split into two tour groups. The first group toured Lawson’s Nordal Cyclotron and PET Radiochemistry Facility with the facility’s director, Dr. Michael Kovacs; Jeff Corsaut, engineer; and Dr. Justin Hicks, Lawson imaging scientist.

Above: Dr. Justin Hicks provides a tour of The Cyclotron and PET Radiochemistry Facility
The Cyclotron and PET Radiochemistry Facility is used to produce positron-emitting radiopharmaceuticals (PERs). PERs are injected into patients undergoing a positron emission tomography (PET) scan. The half-life of the radioactive isotopes in PERs is short, which necessitates generating them with a cyclotron that is in close proximity to the clinic where they are used.
The students learned how PERs are produced in the Cyclotron and research being conducted with PERs to advance imaging of complex diseases.
The second group toured Dr. Alexandre Legros’ brain stimulation lab which is part of the Bioelectromagnetics and Human Threshold Research Group at Lawson. Dr. Legros’ research focuses on the effects of specific electromagnetic stimuli - from deep brain stimulation to power-frequency magnetic fields - on human brain processing, motor control and cognitive functions. The students were guided by lab manager, Michael Corbacio, and postdoctoral scholar, Dr. Sebastien Villard.

Above: Dr. Sebastien Villard (second from right) and Michael Corbacio (far right) provide a demonstration of research being conducted in Dr. Alexandre Legros' Bioelectromagnetics and Human Threshold Research Group
The two groups of students then traded places, touring the facility they had not yet visited.
“The H.B Beal senior chemistry class was impressed and grateful with the opportunity to visit the facilities at Lawson Health Research Institute,” said Andrew Holmes, the class’ teacher and head of science at H.B. Beal. “The presentations, cyclotron tour and research lab gave students some valuable insight into some of the roads available to them with a scientific path in education. Students were particularly impressed with how enthusiastic and excited the researchers were in talking about their work at Lawson, and came away with a very positive view of scientific career paths.”
Top 12 research stories of 2022
As the research institute of London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London, our teams impact the lives of people in Ontario, Canada and around the globe with groundbreaking studies, world firsts and translational research that enhances care, health and wellbeing. Here are some of Lawson Health Research Institute’s top research highlights of 2022.
Researchers looking to better personalize treatment for PTSD

In a new study through Lawson and Western University’s Schulich School of Medicine & Dentistry, scientists are looking at a form of treatment called deep brain reorienting (DBR) for those suffering from post-traumatic stress disorder (PTSD). Read more.
Virtual care associated with significant environmental and patient cost savings

A new study by researchers at ICES, Lawson and Western finds that virtual care during the COVID-19 pandemic led to a significant reduction in carbon dioxide emissions and patient travel-related expenses, such as gasoline, parking or public transit costs. Read more.
Novel test that could easily diagnose blast injury created by local scientists

In a world first, researchers at Lawson and Defence Research and Development Canada have developed a breath test that could be used to diagnose repetitive blast injury – a mild traumatic brain injury resulting from pressure changes that occur during explosions. The device will soon go through clinical trials to validate its efficacy. Read more.
Local researchers using artificial intelligence to lead the way in bedside lung imaging
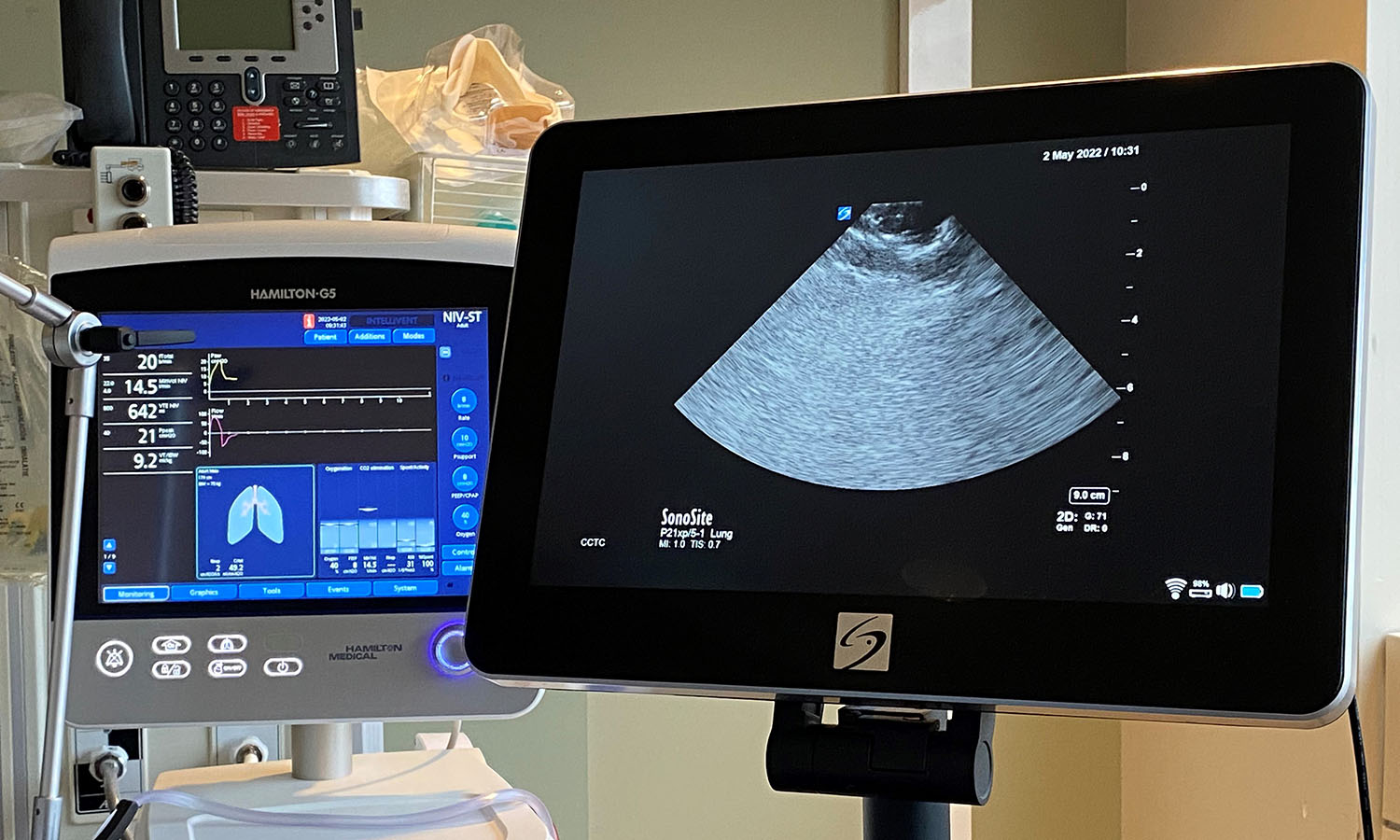
A team at Lawson is testing a new form of artificial intelligence (AI), paired with portable ultrasound machines, to image and identify lung concerns in real time, right at the beside of critically ill patients. Approximately 100 critical care patients at LHSC will be part of this study. Read more.
New tool shows promise in helping people manage traumatic brain injuries one pace at a time

A team at Lawson has developed a new app called MyBrainPacer™ which aims to better assist and treat those living with mild traumatic brain injuries (mTBI), including concussions. mTBI may come with lasting effects that can alter a person’s life. Although a person with a mTBI may appear fine on the outside, many have to pace their day-to-day activities in order to allow the time needed for the brain to properly heal. Much like point tracking used by dieters to monitor food choices, through MyBrainPacer™ App, users can assign values to tasks like driving, grocery shopping, screen use and exercise so they can plan and pace their daily activity. Read more.
Study shows a decline in Veterans' mental health throughout the pandemic

When it comes to mental health conditions, Veterans are an at-risk population, often having higher rates of depression and post-traumatic stress disorder (PTSD). When the COVID-19 pandemic hit, scientists at Lawson wanted to understand its effects on this already at-risk population. They found that more than half of Canadian Veterans reported a decline in their mental health. Read more.
Growing evidence that PSMA imaging improves prostate cancer detection
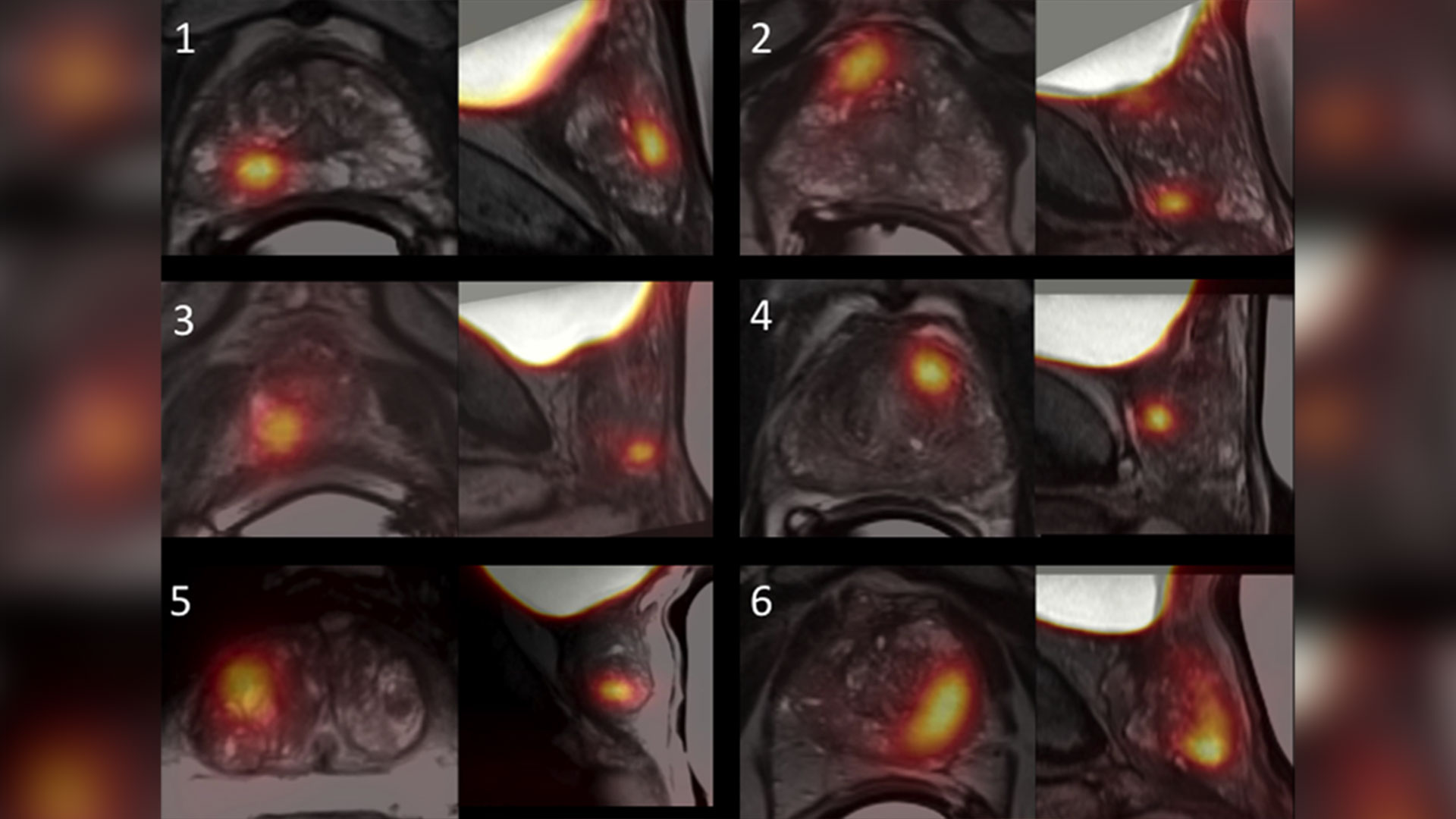
Scientists at Lawson are leading the way in using specialized imaging to detect prostate cancer – the fifth leading cause of cancer death in men around the world. Early evidence indicates that PSMA PET scans have changed how prostate cancer is being treated, but more work is underway to understand the impact of those treatment changes. Read more.
Leveraging virtual reality to manage pain in paediatric patients

A study underway through Lawson and Children’s Hospital at LHSC is using virtual reality (VR) to help paediatric patients during painful and distressing procedures. The study is focusing on paediatric patients who need port access. A port is a little reservoir that sits underneath the skin that allows access to blood or medication with the use of a needle. Ports are most commonly used in paediatric cancer patients. Read more.
Team players: FMT and microbiome research could have widespread impact

There is still much to learn about the human microbiome and its role in fighting disease, but ongoing studies at Lawson, including a focus on fecal microbial transplants (FMT), are making strides in harnessing this complex system. FMT is being studied in connection with conditions as varied as non-alcoholic fatty liver disease, rheumatoid arthritis, atherosclerosis, HIV, cancer and multiple sclerosis. Read more.
London researchers adapt MRI technology to image salt within the kidneys
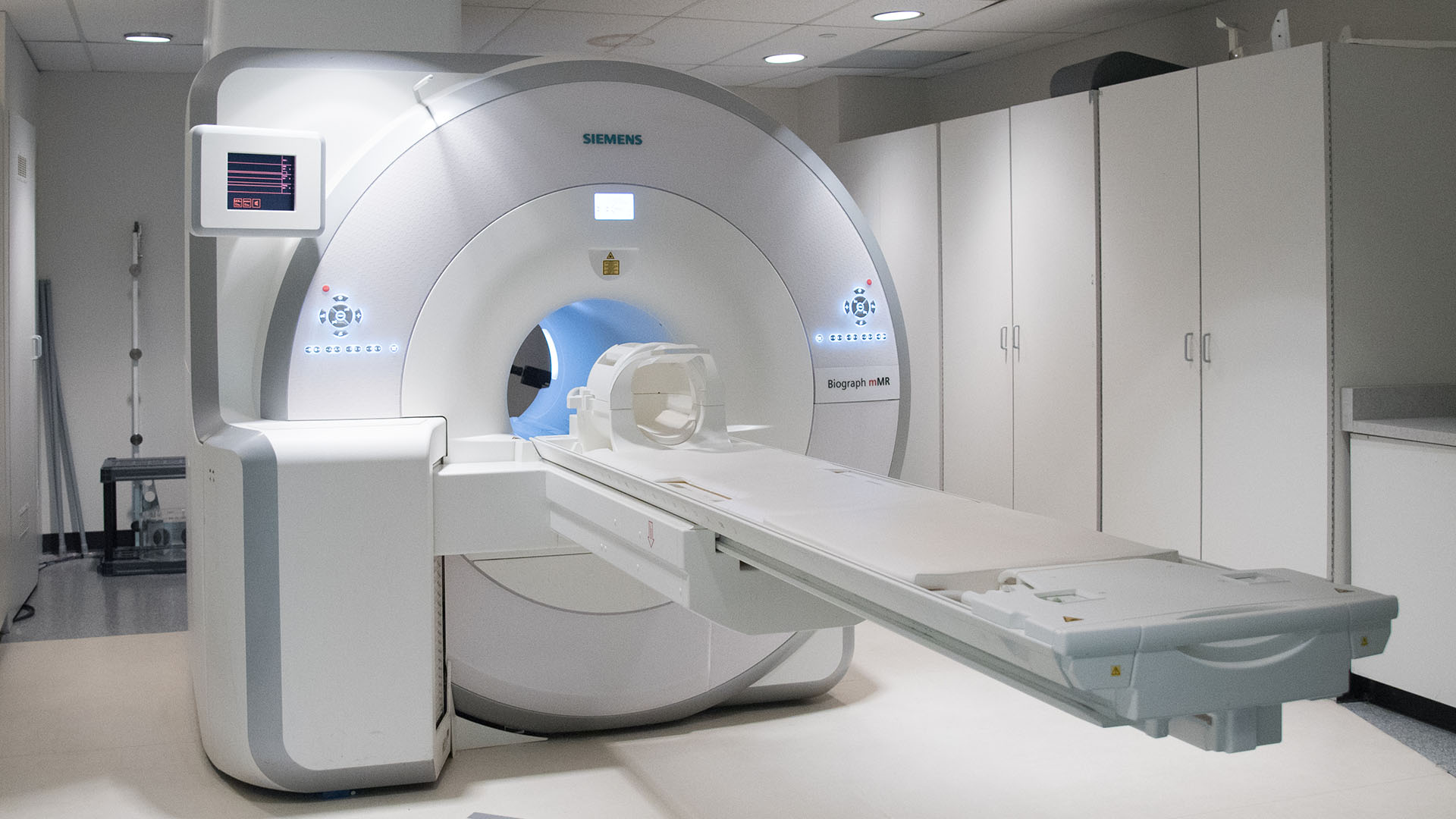
Scientists at Lawson have adapted PET/MRI technology to accurately image salt within the kidneys of patients with kidney disease. Imaging salt within the kidneys has never been accurately accomplished in patients with kidney disease, but Dr. McIntyre and his team developed new technology and software that was adaptable to a PET/MRI machine at St. Joseph’s. Read more.
London researchers discover novel method to diagnose long COVID
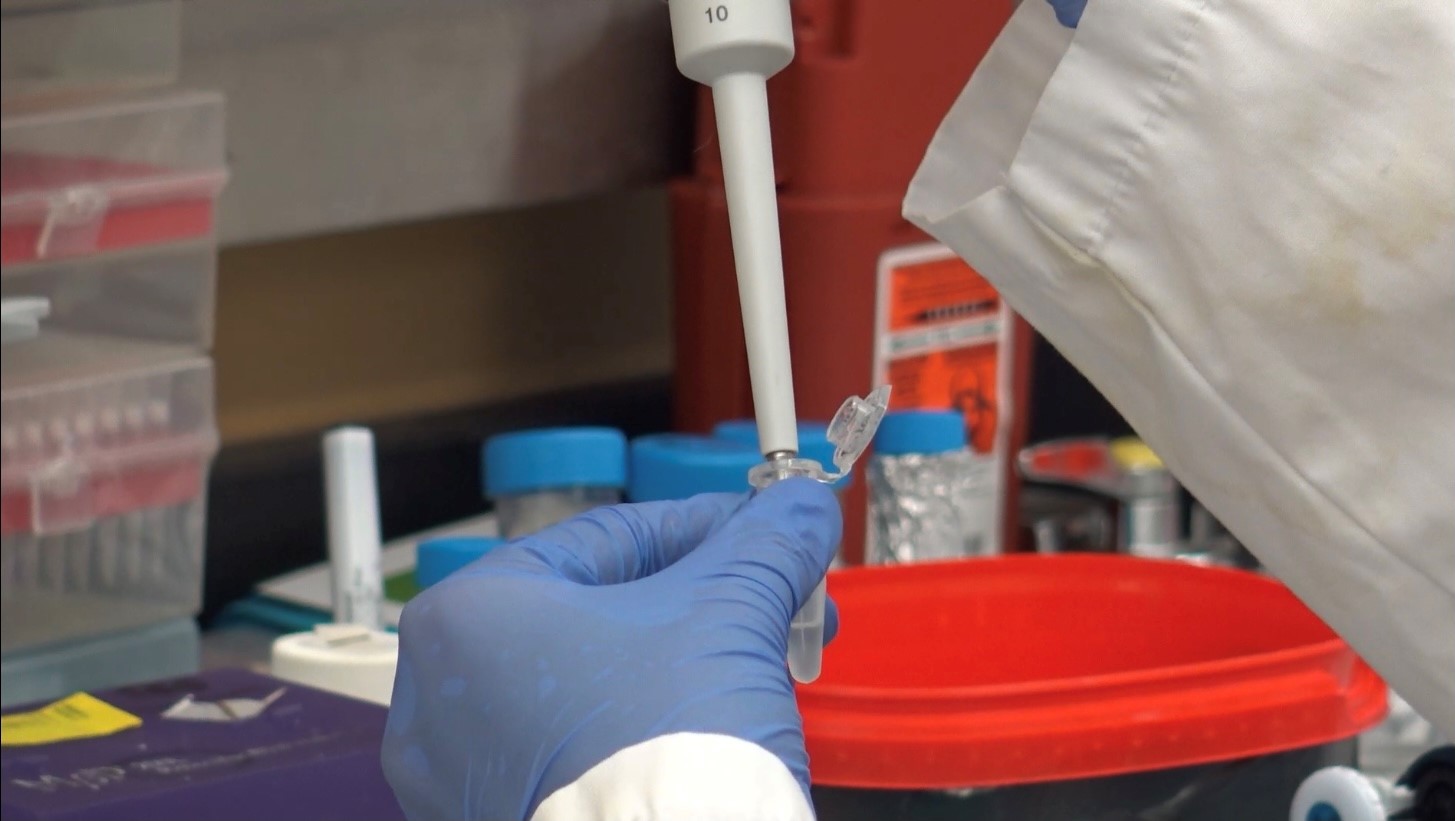
Published in Molecular Medicine, researchers at Lawson have found that patients with post-COVID-19 condition (long COVID) have unique biomarkers in their blood. The team is now working on developing a first of its kind blood test that could be used to diagnose long COVID. The discovery could also lead to new therapeutics for this condition. Read more.
Largest trial ever done in hemodialysis care examines optimal dialysis temperature
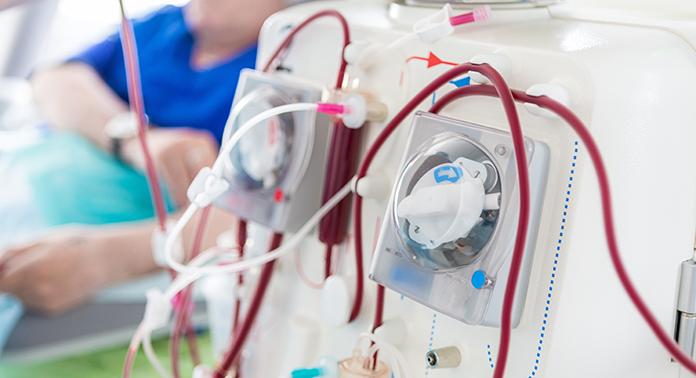
Published in the Lancet findings from a large clinical trial through Lawson, ICES Western and Western University suggest that lowering dialysis temperatures does not lead to improved patient outcomes, despite previous studies suggesting otherwise. Read more.
To learn more about Lawson research studies, please visit our News and Media page
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Two new research chairs announced for imaging
In a historical-first, St. Joseph’s Health Care Foundation and Western University announced two research chairs that are a critical step toward new approaches in imaging research and patient care in London and around the world. The combined value of both innovative new research chairs is $6.5M, which will be endowed in perpetuity to advance imaging research at Western University and Lawson Health Research Institute.
The research chairs have been named after the two scientists who are revolutionizing health care through their groundbreaking imaging research – Drs. Ting-Yim Lee and Frank Prato.
“These Chairs build on the legacy of exceptional imaging leadership across our academic, research and healthcare organizations. They are a critical step towards new approaches in medical technology and hospital-based research that will revolutionize patient care,” says Dr. Gillian Kernaghan, President and CEO, St. Joseph’s Health Care London.
Research teams in the city are using state-of-the-art imaging technology to help clinicians better predict and diagnose illnesses before their unset. And uncover why, and how, illness forms to one day find a cure to some of the most devastating diseases in the world.
“We’ve come to know medical imaging as one of the cornerstones of innovation and discovery at Lawson, and the two new research chairs represent two monumental leaps forward in the field of imaging research,” adds Dr. David Hill, Lawson Scientific Director.
The Ting-Yim Lee Chair in Cardiac Computerized Tomography (CT) Imaging Research has been established through the generosity of Ting-Yim and Maggie Lee and a joint funding collaboration between St. Joseph’s Foundation and Western University.
Dr. Ting Yim Lee is a scientist and professor of the Schulich School of Medicine & Dentistry, medical physicist at St. Joseph’s Health Care London and a scientist with Lawson’s Imaging program. Through his leadership, The Ting-Yim Lee Chair in Cardiac Computerized Tomography (CT) Imaging Research will transform the way clinicians diagnose, and prevent, severe tissue damage in persons who have experienced a cardiac event.
“Over the past 28 years, St. Joseph’s and Western have created opportunities for me and supported my research endeavor in many ways. I feel this gift is the best way to repay the help that I have received. We are onto something that is worthwhile and successful. By setting up this Chair, there would be a significant person – a clinician-scientist – to lead the next phase of the cardiac CT program. I am really humbled that the institutions see the value in this research and have contributed to guarantee that we have the necessary leader to carry forth this development,” says Dr. Lee.
This Chair represents the next phase of CT imaging research, focused on developing software and new methods that will save people’s lives.
The Dr. Frank Prato Research Chair in Molecular Imaging has been established to further enhance scientific understanding in the specialty of molecular imaging – building upon St. Joseph’s internationally-recognized leadership in imaging excellence.
Dr. Frank Prato is a scientist and professor of the Schulich School of Medicine & Dentistry, Chief Medical Physicist at St. Joseph’s Health Care London and the Founder and Program Leader of Lawson’s Imaging Program. Through his visionary leadership, The Dr. Frank Prato Research Chair in Molecular Imaging will improve the way clinicians effectively diagnose disease and actively correct the course of treatments in real time for life-threatening illnesses.
“I am truly honoured to have this Research Chair in Molecular Imaging named after myself. Over the past 40 years I have been privileged to work with outstanding people and incredible resources. Today Medical Imaging has become a cornerstone of care at St Joseph's Hospital. Here at St Joseph's we realize patient stewardship includes research as an essential part of the patient care continuum and that discovery, through research, leads to improved patient care. The holder of this chair will help lead us into the next frontier of medical imaging directly benefiting our local, national and global communities,” says Dr. Prato.
This Chair represents the next phase of precision medicine using molecular imaging to distinguish between varying forms of dementias, cancers, and to detect the early onset of cardiac disease and diabetes before symptoms emerge.
“With this historic announcement, we are marking a new phase of partnership and collaboration between our institutions and celebrating the generosity of donors who have helped create two significant research chairs,” explains Dr. Amit Chakma, President and Vice-Chancellor, Western University. “Together we will ensure that London remains at the forefront of medical imaging research and teaching.”
These Chairs will also have a greater role to play in the local health care community by attracting, and retaining, the research talent needed to innovate the way London’s hospitals and Western tackle the most pressing health issues Canadians face today.
Understanding the COVID-19 virus through health research
In the early months of the COVID-19 pandemic, there was little known about the virus that was causing the COVID-19 illness. Hospital researchers in London, Ontario, through Lawson Health Research Institute, quickly got to work to study and better understand the SARS-CoV-2 virus. Lawson is the research arm of London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London.
“When the pandemic hit, we were well prepared in London to start research studies. We had existing expertise, laboratories and teams through the hospitals, Lawson and Western University that could be mobilized quickly,” explains Dr. Douglas Fraser, Critical Care Physician at LHSC and Scientist at Lawson. “Patients started coming to hospital with COVID-19 and we began research that involved collecting human samples and bringing them to the lab for analysis.”
Dr. Fraser, who is also a Professor at Western’s Schulich School of Medicine & Dentistry, led the research team studying the samples from COVID-19 patients in hospital. “We learned very quickly that COVID-19 patients were experiencing a strong inflammatory response to the virus. We looked at the molecules involved because many of these are signaling molecules to the immune system.”

Dr. Douglas Fraser, Critical Care Physician (LHSC) and Lawson Scientist
“By studying the molecules, we were able to determine the pathways. This is important because it also points to how we should be targeting our diagnostics and therapeutics,” adds Dr Fraser.
As a hospital research institute, Lawson is uniquely positioned to address the medical questions posed by a new virus. Its Clinical Research Services (LCRS) and Center for Clinical Investigation and Therapeutics (CCIT) teams responded rapidly when researchers initiated COVID-19 studies, including Dr. Fraser’s study to examine the immune response in patients with COVID-19.
“Starting a clinical trial usually takes a certain amount of time to put together, but the pandemic created a perfect storm,” explains Sue Tereschyn, Manager of LCRS at Lawson. “Clinical researchers had to develop studies at a speed they have never seen, and they needed implementation support at the same speed. In Dr. Fraser’s case, we needed samples from the Intensive Care Unit (ICU) and we were processing samples from COVID-19 patients seven days a week. A high level of skill was needed.”
Dr. Fraser and his team soon became the first in the world to understand the immune response and several pathophysiological features of the virus. This work led to a critical understanding of how the virus was impacting patients and potential avenues for therapy.
“It’s important to understand what’s happening in the body when someone has COVID-19 because that gives us information as to why some patients don’t do well and why others recover,” shares Dr. Fraser. “This helps us know who is vulnerable to COVID-19 and how to best offer treatments in the future.”
Read about Dr. Fraser's COVID-19 research:
- Researchers team up with Diagnostics Biochem Canada to study COVID-19
- Study identifies biomarkers that could be used in a quick, inexpensive COVID-19 blood screening tool
- Researchers unravel two mysteries of COVID-19
Work is also underway to find the unique fingerprint that the COVID-19 virus can leave on the lungs. Hospital researchers at Lawson have developed and tested an artificial neural network for diagnosing COVID-19.

Dr. Robert Arntfield, Medical Director, Critical Care Trauma Centre (LHSC) and Lawson Researcher
“The lung ultrasound techniques and the findings of COVID-19 by looking at the lungs didn’t initially look unique when compared to other conditions like pneumonia. Our group wanted to investigate whether or not there were differences that were possibly subvisible,” says Dr. Robert Arntfield, Medical Director of Critical Care Trauma Centre at LHSC and Lawson Researcher. “Through our work, we were able to show that in fact artificial intelligence could outperform a trained clinician in identifying a COVID-19 lung from a similar affected lung that was not due to COVID-19.”
This new technique just scratches the surface of the beneficial use of AI when it comes to medical imaging for patients. “It shone a light on the idea that there were hidden details within all the noise of the image,” adds. Dr. Arntfield. “When you can input that into a machine that is extremely portable the way ultrasounds are, you have a precise diagnostic machine that you can take anywhere a tablet can go.”
The team is now expanding on these findings with further research. Lawson has recently approved Dr. Arntfield’s “Project Deep Breath” which aims to go beyond COVID-19 and explore multiple conditions where lung ultrasounds and AI can be paired together.