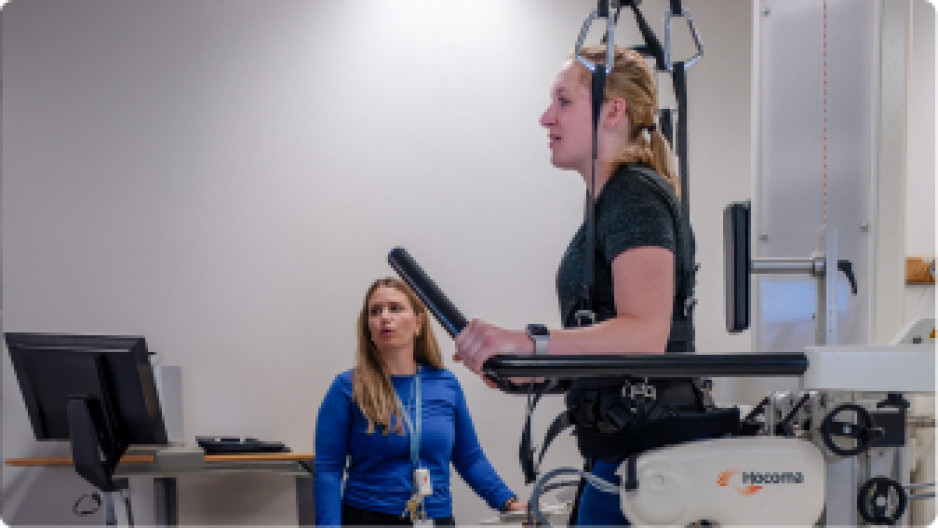Search
Search
Responding to the call for action during the COVID-19 pandemic
Quickly after the COVID-19 pandemic began to grip the world, Lawson Health Research Institute responded with action. Lawson is the research arm of London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London. With hospitals focused on providing excellent patient care in the face of an unknown virus, hospital researchers in London, Ontario began critical COVID-19 studies.
“A lot was unknown during the first wave of the pandemic. Any research that wasn’t essential was put on hold. At the same time, we had people with different expertise coming together with different perspectives to see how we could better understand the SARS-CoV-2 virus and the COVID-19 infection,” explains Dr. David Hill, Lawson Scientific Director and VP, Research at LHSC and. St. Joseph's. “Our hospital researchers formulated ideas and very quickly came up with research proposals. These were fast tracked through our processes and within two months we approved over 50 new studies surrounding COVID-19.”

Dr. David Hill, Lawson Scientific Director and VP, Research at LHSC and. St. Joseph's
Some of these studies were clinical trials, which are research studies performed with people. Many patients from London hospitals get involved as patient participants and when COVID-19 hit, many agreed to be a part of this important research.
“We saw the pandemic happening across the world, and suddenly it was happening here in London. This has probably been the biggest challenge of my career,” says Carol Young-Ritchie, Executive Vice President at LHSC. “We had to look at many of our processes and how we were doing things, and adjust appropriately and nimbly.”
Young-Ritchie adds that as the hospital continued to admit a growing number of COVID-19 patients, a strong focus on research was needed. “It was absolutely critical and important for LHSC as a leader and academic centre to contribute to our collective knowledge. We needed to keep that research going and although it has been challenging, it has also taught us to be innovative.”

Carol Young-Ritchie, Executive Vice President at LHSC
The same focus was happening at St. Joseph’s Health Care London, with health care providers and researchers finding ways to improve care and outcomes for patients who had contracted the virus. “COVID-19 research through the hospital has been incredibly important,” says Karen Perkin, Vice President of Patient Care at St. Joseph’s. “We had researchers busy looking at the impacts of COVID-19. We had patients on ventilators and we were trying to understand that more. We also had research looking at the impacts for staff members looking after patients. All important, helpful knowledge as we move forward.”

Karen Perkin, Vice President of Patient Care at St. Joseph’s
Hospital research in London through Lawson is proudly affiliated with Western University. At Western’s Schulich School of Medicine & Dentistry, the new state-of-the-art Imaging Pathogens for Knowledge Translation (ImPaKT) Facility was the perfect environment to conduct COVID-19 research.
“ImPaKT is a special containment facility where research on viruses like SARS-CoV-2 can be done safely,” says Dr. David Litchfield, Vice Dean of Research and Innovation at Schulich Medicine & Dentistry. “It has become a focal point for dozens of studies involving research through Schulich Medicine & Dentistry, as well as partners from the hospitals and other academic institutions and industries.”

Dr. Litchfield adds that collaboration between hospital partners and scientists has been the key to successful COVID-19 research. “This collaboration has enabled advances leading to new diagnostic testing for COVID-19, as well as studies using MRI or related imaging tools to investigate long-term impacts of the infection on individuals.”
The rapid research response to COVID-19 couldn’t have happened without community and foundation financial support. “Funding support from our hospital Foundation is something we are so grateful for,” says Perkin, referring to St. Joseph’s Health Care Foundation. “They came right out at the beginning and asked how they could help, as did our donors.”
LHSC’s London Health Sciences Foundation and Children’s Health Foundation were also pivotal in research funding during the pandemic. “Funding is a crucial part to how we do hospital research and the Foundations have been important partners in making sure our research continued,” says Young-Ritchie.
As the pandemic continues, so does the research within our community. Hospital research has already improved diagnostics, treatments and patient outcomes related to COVID-19 and helped people all around the world.
“If you look at some of the achievements that have occurred in just a little more than a year, we have had a number of landmark publications on ways to diagnose COVID-19 compared to other respiratory disorders,” notes Dr. Hill. “We have had many rapid advances and it can take a crisis to bring out the best in people. Then things come together quickly, such as expertise, talent and money – and the job gets done.”
Revealing the culprit behind Parkinson’s disease
An estimated 55,000 Canadians are living with Parkinson’s disease. While researchers are advancing therapies to treat symptoms, such as tremors, there is currently no method to stop progression.
To begin addressing this problem, a team of scientists at Lawson Health Research Institute is developing an imaging tracer.
“There’s a protein in the brain called alpha-synuclein (α-syn) that scientists believe is a culprit in causing Parkinson’s disease. The protein forms in ‘clumps’ called Lewy bodies that kill brain cells and potentially lead to disease,” explains Dr. Justin Hicks, Lawson Imaging Scientist. “Unfortunately, we have no way to study it in human brains and this has limited our ability to test therapies against it.”
Efforts have been made to study the elusive protein through modern imaging techniques like positron-emitting tomography (PET). Scientists have attempted to develop a PET probe – a radioactive molecule that targets the specific protein in order to produce highly specific images or scans – but they have been unsuccessful.

Above: Dr. Justin Hicks working in the Nordal Cyclotron & PET Radiochemistry Facility
“Unfortunately, the Lewy bodies caused by α-syn are hard to distinguish from protein clumps found in Alzheimer’s disease and other dementias. This makes it very difficult to know whether a PET probe has found clumps associated with Parkinson’s disease.”
Through a new study, Dr. Hicks and his team are working to find a solution. To do so, they will examine a different but related protein.
“There’s another protein called fatty acid binding protein 3 (FABP3) and one of its roles is to ‘chaperone’ the α-syn protein in human cells. Past studies have shown that levels FABP3 are higher in patients with Parkinson’s disease when compared to healthy controls,” explains Dr. Hicks. “This suggests that high concentrations of FABP3 can be used as an alternate measure of α-syn.”
They hope to measure levels of the FABP3 protein in place of the α-syn protein, and gain a better understanding of the role that both proteins play in the development and progression of Parkinson’s disease. To image Lewy bodies associated with Parkinson’s disease, the researchers are working to produce a PET probe that targets FABP3.
To accomplish this, they will be working in their lab to find a chemical that targets FABP3. Once found, they will attach a radioactive isotope to the chemical and produce a finished tracer. The tracer will then be tested in preclinical models.
Once injected, the PET probe will find and stick to FABP3. The PET isotope will emit a small amount of radioactivity and these emissions will show up as PET images.
“The ultimate goal is to develop a PET probe that can be used to distinguish Parkinson’s disease from other neurodegenerative diseases. The probe could also be used to assess new therapies that reduce levels of the α-syn protein,” says Dr. Hicks. “If successful, we hope this research will lead to a better understanding of the progression of Parkinson’s disease and ways to prevent it.”
Dr. Hicks and his team are being funded for this project through Lawson’s Internal Research Fund (IRF) competition. “Lawson’s IRF is extremely important for early career researchers. It allows us to generate data and publications to then apply for larger external funding. It also permits an added level of risk to pursue projects that may not reach their end goal but often spur new lines of research.”
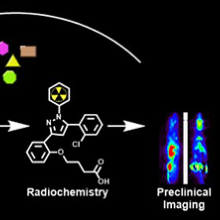
Above: A graphic depiction of this research project and its goals.
Revealing the secrets of dementia
The immune system is one of our greatest defenses against disease and injury. But what happens when it betrays us?
With conditions like rheumatoid arthritis the immune system is manipulated to attack the human body. Inflammation, normally a protective immune response, can be employed to cause symptoms like pain.
Surprisingly, research suggests our immune system may be similarly affected in patients with neurodegenerative dementias.
“We know there are increased numbers of inflammatory cells in the brains of patients with dementia but we don’t know what role they’re playing,” says Dr. Elizabeth Finger, a scientist at Lawson Health Research Institute and neurologist at St. Joseph’s Health Care London’s Parkwood Institute. “Are they doing their proper job of cleaning up damaged cells or is their presence more sinister?”
Dr. Finger’s research group aims to identify and understand changes in the brain that lead to symptoms of dementia, find novel treatments to improve patient quality of life and hopefully prevent the disease altogether. Critical to this work is Dr. Finger’s collaboration with Lawson Imaging scientists Drs. Keith St. Lawrence, Udunna Anazodo, and Justin Hicks.
The researchers utilize Canada’s first hybrid positron emission tomography and magnetic resonance imaging (PET/MRI) machine located at St. Joseph’s Hospital. This high-powered imaging allows them to assess changes to both structure and function in the brains of patients with neurodegenerative dementias like Alzheimer’s disease, frontotemporal dementia and Lewy body dementia.
In one of their many studies they are examining whether there is inflammation in the brains of patients with frontotemporal dementia and, if so, whether this inflammation is present in areas of the brain not yet damaged by the disease.
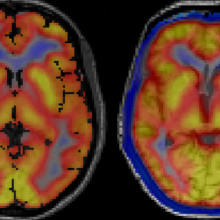
Images captured using a hybrid PET/MRI machine show activated immune cells in the frontal brain regions in a patient with frontotemporal dementia (right) compared to a healthy volunteer (left).
“A presence in those parts of the brain would suggest that inflammation is not playing its normal role of cleaning up damaged cells,” explains Dr. Finger. “It would suggest the brain’s immune response is overactive and that we should consider clinical trials for medications that modulate this response.”
Dr. Finger is an active investigator for novel therapies. In 2019, her group will participate in at least two clinical trials for medications that target genetic mutations that can cause frontotemporal dementia. The studies are phase I trials, which means they are the first time the medications are being tested in humans.
Dr. Finger is also leading a North American multi-centre trial called FOXY. The study will examine the therapeutic potential of a hormone called oxytocin to improve the loss of emotion and empathy that frequently occurs in patients with frontotemporal dementia.
“In the past there were very few treatments for frontotemporal dementia,” explains Dr. Finger. “We are glad to say that Lawson and St. Joseph’s will offer the opportunity to take part in these advances. Words cannot adequately express the appreciation we have for our patients, caregivers and healthy volunteers who participate in research. The time and effort they selflessly donate with the goal of helping future patients is truly inspiring and motivating.”

This story originally appeared in an annual publication from the Alzheimer Society London and Middlesex.
Revolutionizing rehab
St. Joseph’s Health Care London is taking giant strides in the science of rehabilitation and movement, with direct benefit to patients.
St. Joseph’s is setting a long-time vision into motion.
“Five years ago, we had a vision of leveraging our long history and expertise in providing innovative rehabilitation treatments to improve the lives of people with mobility needs on a larger scale,” says Roy Butler, President and CEO of St. Joseph’s Health Care London (St. Joseph’s). “That dream has come to life.”
While experts at St. Joseph’s had the knowledge, innovative spirit and passion to achieve the vision, they needed a partner who shared the same enthusiasm.
William and Lynn Gray answered that call. With their generosity and ground-breaking investment, The Gray Centre for Mobility and Activity was created.
“Lynne and I are very pleased with the steady forward advancement of the centre’s mission since its establishment just a few short years ago,” says Bill Gray. “The innovative thinking and idea generation that seeks new solutions to the issue of mobility have really taken root. We hoped that The Gray Centre would have an impact on care ... and it has.”
“We’ve watched the development of The Gray Centre with enormous pride and are pleased to have our name associated with it, and the excellence it stands for,” adds Lynne Gray.
A unique concept
Established in 2020, The Gray Centre at St. Joseph’s Parkwood Institute is a regional hub focused on researching leading-edge treatments and interventions in mobility and activity. The centre’s unique model of linking research and care allows researchers to work side-by-side with clinicians, patients, and caregivers to uncover optimal methods for maintaining mobility throughout a person’s life.
“Scientists at The Gray Centre are leading the way in integrating technology and solutions in care to better understand how we can enhance each patient’s treatment plan to improve their functionality and ability to move,” says Butler.
Pioneering Research
More than 50 ongoing rehabilitation research projects at Parkwood Institute are exploring areas such as spinal cord and traumatic brain injury rehabilitation, pain, outcomes for amputees, virtual exercise and cognitive behavioral therapy, gait analysis as a measure of dementia progression, and stroke rehabilitation and recovery.
The Gray Centre is a catalyst and connector for these projects by investing in cutting-edge technology, providing seed grants, embedding researchers from Western University, leveraging clinical expertise, attracting world-class researchers and translating new knowledge into clinical practice by training students and clinicians, and fostering sustainable practice change.
More than $1.3 million granted through St. Joseph’s Health Care Foundation has advanced work at The Gray Centre over the past year. From researcher support to new equipment such as two transcranial magnetic stimulators, a portable handheld ultrasound and several sensored mats for gait assessment donors have stepped up to advance this work.
Leadership with Purpose
At the helm of The Gray Centre is Siobhan Schabrun, PhD, a world-renowned neuroscientist and the inaugural William and Lynne Gray Research Chair in Mobility and Activity. Thanks to a partnership with Western University’s Faculty of Health Sciences and Schulich School of Medicine & Dentistry, donor funding for the chair made through St. Joseph’s Health Care Foundation was matched, creating a $5-million endowed position.
Schabrun’s innovative research benefits people suffering from chronic pain. With a focus on non-invasive brain stimulation techniques to enhance neuroplasticity and improve mobility and activity outcomes, she and her team are, in essence, retraining the brain’s pain response. This innovative work bridges the gap between neuroscience and rehabilitation, offering new hope for individuals with musculoskeletal and neurological conditions.
Originally trained as a physiotherapist with a PhD in neuroscience from the University of Adelaide in Australia, Schabrun has attracted more than $15 million in competitive research funding and written or contributed to more than 140 scholarly publications.
FLOATing Forwards
The newest advancement is a first-in-Canada and a marvel of medical engineering that is transforming options in rehabilitation research and practice.
The Reha-Stim Medtec FLOAT system at St. Joseph’s Parkwood Institute enables patients with mobility limitations to walk, supported, without fear of falling. They "float" in a controlled environment using a combination of robotics, body-weight support and real-time feedback. The device has a harness attached to a robotic arm, which adjusts the level of support based on the patient's movements. Sensors provide continuous feedback for maximum learning and greatest benefit to physical therapists and patients alike. The FLOAT system has shown significant improvements in patients' mobility, balance and overall functional independence.
“Innovative equipment like the new FLOAT System is an example of the type of innovation that does not exist anywhere else in Canada,” says Bill Gray. “The real-life application of technologies like this are what The Gray Centre is intended to be about.”
Through the combined efforts of dedicated professionals, cutting-edge technology and philanthropist partners, St. Joseph’s Gray Centre has combined vision with passion and is transforming lives, one step at a time.
Running Against Ruptures
This event is raising funds for brain aneurysms research.
Did you know, ruptured brain aneurysms account for 3–5% of all new strokes?
How about that women, more than men, suffer from brain aneurysms at a ratio of 3:2?
It is a devastating medical issue many Canadians face.
You are invited to Running Against Ruptures on June 23, 2019 at Greenway Park in London, ON
Running Against Ruptures is committed to raising funds for patients and families affected by brain aneurysms so people can get the help they need earlier and with better results. By conducting research, we can help alleviate the pain many families encounter due to brain aneurysms.
However, each of these projects requires funding. That’s why Running Against Ruptures looks to raise money to support these life-saving research projects.
For more information, please visit the London Health Sciences Foundation.
Save the Date: London Health Research Day 2021
Discover London's health research community by joining learners and researchers virtually at the 2021 London Health Research Day scheduled for May 11.
London Health Research Day is an opportunity to learn about research happening in labs and clinics across the city while engaging in scientific discussion. This year’s event will be presented virtually.
Featuring Keynote Speaker: Andrew Au

Find out more about Andrew Au, LHRD 2021 keynote speaker as part of The Lucille & Norton Wolf Health Research Lecture Series.
Academic Program for Learners
Abstract submissions:
Submissions will open on February 16 and close on March 3, 2021. Go to the LHRD website for more information for participants.
The Lucille & Norton Wolf London Health Research Day Trainee Publication Awards:
Thanks to the personal generosity of Lucille and Norton Wolf, we are pleased to issue a call for The Lucille & Norton Wolf London Health Research Day Trainee Publication Awards. Learn more about the eligibility criteria and how to apply.
London Health Research Day is presented in partnership by Lawson Health Research Institute and the Schulich School of Medicine & Dentistry.
Scientists
Our scientists
Lawson leads research, with more than 250 principal investigators, technicians, support staff and trainees making health discoveries every day. As award-winning leaders and emerging experts in their fields, they share their innovations with doctors, patients, peers and the world.
They are engaged in more than 800 clinical studies and receive about 600 funded grants totalling more than $39.4 million in grant funding.
Search or browse the directory below to find scientist profiles and contact information.
Scientists studying carbon monoxide as a possible treatment for sepsis
Sepsis is the leading cause of death worldwide with limited treatment options
MEDIA RELEASE
For immediate release
LONDON, ON – Sepsis is a life-threatening condition that occurs when the body’s response to an infection triggers excessive inflammation. The inflammatory response can cause damage to organs such as the heart, liver, lungs and brain. While there are currently limited treatments for sepsis, researchers at Lawson Health Research Institute are working to change that by examining the use of carbon monoxide-releasing molecules to treat patients. “This is an unusual approach that is looking at using carbon monoxide which is the infamous gas molecule,” says Dr. Gediminas Cepinskas, Scientist and Director of the Centre for Critical Illness Research at Lawson. “If administered and used in small non-toxic concentrations, carbon monoxide can offer very potent protective and anti-inflammatory effects.”
In studies on the subject, including the most recent one published in the journal of Experimental Biology and Medicine, the research team was able to demonstrate efficacy in using carbon monoxide-releasing molecules to protect individual cells in the liver and lungs of sepsis induced inflammation in preclinical models. “We have been working on isolated organs and organ specific cells to test carbon monoxide-releasing molecules to narrow down which specific cells are more sensitive to treatment and which biochemical pathways are involved,” Says Dr. Cepinskas. “We are making great progress in our work and have had success in addressing the efficacy of carbon monoxide-releasing molecules in preclinical models.”
Dr. Cepinskas is one of just a few scientists worldwide studying carbon monoxide-releasing molecules to treat inflammatory conditions such as sepsis. While carbon monoxide is commonly known as dangerous, using it in a controlled manner does not pose a danger and may have therapeutic potential. “Our immune system is usually our defense system, but with sepsis it becomes so activated it starts to attack our own cell tissues, resulting in injury and dysfunction of the affected organs,” explains Dr. Cepinskas. “Almost each and every cell in our body naturally produces carbon monoxide which is used in defense against harmful and injured stimuli. We are taking advantage of this knowledge and currently we are the only lab in Canada working on this potential carbon monoxide-based therapy.”
Dr. Cepinskas is also collaborating with clinicians at London Health Sciences Centre (LHSC) to study the use of carbon monoxide-releasing molecules to treat limb compartment syndrome and to improve organ transplantation.
The research team, which has patents in the area of carbon monoxide-releasing molecules, is now working with the pharmaceutical industry to move this potential therapy into human clinical trials in the future.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca