Search
Search
Database funding could improve diagnosis and treatment of prostate cancer
A $125,000 grant from the Canadian Cancer Society will help create a database of PET/CT (positron emission tomography/computed tomography) and PET/MR (magnetic resonance) images of prostate cancer. The hope is that this database will be used to help improve diagnosis and treatment of men with prostate cancer.
The scans use radiopharmaceuticals to target prostate specific membrane antigen (PSMA), a transmembrane protein commonly found on prostate cancer cells.
“The idea behind this grant is to put together a database of PSMA PET/CT and PET/MR scans with annotated findings so medical professionals can scroll through cases and see the sites of prostate cancer. Our hope is this will help clinicians learn how to interpret these scans and ultimately help them to make informed treatment decisions for their patients,” says Dr. Katherine Zukotynski, Adjunct Scientist at Lawson Health Research Institute and lead researcher on the project.
The use of PSMA PET/CT and PET/MR scans in clinical practice is relatively new and currently only accessible through clinical trials. In fact, the first PSMA PET/MR scan in Canada was performed at St. Joseph’s Health Care London in 2016 by Dr. Glenn Bauman, Lawson Scientist and Radiation Oncologist at the London Regional Cancer Program at London Health Sciences Centre. Dr. Bauman is also part of this database project.
Studies have found these scans more accurately detect sites of prostate cancer than earlier imaging techniques, which then helps inform treatment decisions.
Dr. Zukotynski explains, “If you have an idea of the amount of disease and where it is located, and you can correlate it with prognosis, this could be very helpful. It might also allow physicians to compare current patients with patients who have similar findings, which may help determine the best therapies to try.”
There is hope that eventually this same database could lead to the use of artificial intelligence (AI) to assist in diagnosis and treatment planning.
“PSMA PET/CT and PET/MR may be tools helpful to categorize the total burden of disease, and then establish how that disease changes with therapy. Our first step down this path is to assemble a database that can be used both for research and educational purposes.”
The database will include data from centres across Canada, with a number of researchers contributing to the project funded by the Canadian Cancer Society.
Other principal investigators include: Dr. Bauman; Dr. François Bénard of the BC Cancer Research Institute; Dr. Vincent Gaudet, University of Waterloo; Dr. Phil Kuo, University of Arizona; Dr. Cynthia Ménard, Centre Hospitalier Universitaire de Montreal; and Dr. Ur Metser of the Princess Margaret Hospital. Dr. Carlos Uribe of the BC Cancer Research Centre and Dr. Aaron Ward of Lawson are co-applicants for the grant.
This is the part three of a three-part series on PSMA PET imaging research. Check out part one and two.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Dementia research hits the ‘mark’
St. Joseph’s Health Care London is at the forefront of national research exploring biomarkers to better predict dementia and slow its onset.
Dr. Michael Borrie is now seeing grandchildren of patients who came to his clinic when he first started Alzheimer’s research 30 years ago.
His message to this new generation is more hopeful than ever, bolstered by ever-more-reliable ways of early detection and being tantalizingly close to a future of predicting dementia and intervening even before symptoms appear.
“The ultimate goal is to slow cognitive decline – and to stop it if we can – so that people can live independently, and happier, for a lot longer,” says Borrie, Medical Director of the Aging Brain and Memory Clinic at St. Joseph’s Health Care London (St. Joseph’s).
“We’re aiming to alter the trajectory of dementia,” he says.
A geriatrician, clinician and researcher, Borrie is also Platform Lead for the Comprehensive Assessment of Neurodegeneration and Dementia (COMPASS-ND), a long-term study within the Canadian Consortium on Neurodegeneration and Aging (CCNA).
Recently, the Canadian Institutes of Health Research announced $20.6 million in funding to continue the work of CCNA, a 30-site, multi-pronged project of which the St. Joseph’s-based team is the lead player. The grant will enable them to advance the frontiers of dementia research to benefit real-world patients here and across the country.
Solving mysteries with biomarkers
Despite the prevalence of Alzheimer’s and other neurodegenerative diseases – and with more than 10,000 new diagnoses in Canada each year – there are still many mysteries to solve: Why do some people have early-onset dementia while others, super-agers, remain alert and active in their 90s? What’s happening genetically, in their environment and personal medical history to advance or protect against the disease?
What is known, however, is the link between damaged nerve cells and specific proteins that misfold and clump together to form amyloid plaques and tau tangles in the brain. Detecting these abnormal proteins early is an important key to diagnosis and prediction.
Locally, the most comprehensive tool has been state-of-the-art brain Positron Emission Tomography (PET) scanning at St. Joseph’s Imaging. Lawson researchers are also involved in reliably detecting amyloid proteins by analyzing participants’ cerebrospinal fluid (CSF) – a surprisingly accurate way of confirming imaging results, says geriatrician Dr. Jaspreet Bhangu, a Lawson scientist and head of the biomarker project.
Through the BioMIND regional research project, Lawson scientists are analyzing PET scans, blood and CSF samples to check for specific protein biomarkers. If shown to be reliable, a series of these tests over time could signal whether the disease is progressing, and could predict whether it will progress or respond to treatment.
All that gets added to an arsenal that includes tests of behaviour, memory and cognitive function.
“It’s a triple assessment, or even a quadruple one, that we can conduct over time. We hope to use these advanced tests to provide vital information, similar to what is done in certain types of cancer,” Bhangu says.
But that’s not all.
Testing potential treatments
St. Joseph’s is also one of the country’s most active sites for clinical trials into whether novel medications might be able to directly pinpoint and destroy the proteins that cause Alzheimer disease.
“This is the intersection of cutting-edge research, top-notch resources and excellent clinical practice to develop personalized treatments,” says Bhangu. “What makes us unique in Canada among dementia researchers is that our science is taking us from bench to bedside – a rapid turnaround from research to direct patient benefit.”
If a person has a strong family history of Alzheimer disease and no symptoms – but does have positive biomarkers confirming presence of disease – they may then choose to take part in a randomized controlled trial to try to alter the trajectory of the disease.
“It’s still in a research context, still in clinical trials – but if Health Canada ultimately approves a treatment, we’ll have the ability and the patient database to be able to translate our findings into clinical practice much more quickly instead of waiting for years,” says Borrie.
All this is good news for a generation eager for answers, Borrie says.
“When we learn more about the mechanisms of the disease, we can find more effective, earlier treatments. And if we can treat people earlier, we hope to move the disease progression curve to the right, to add more years of good cognitive health to someone’s life.”
Detecting prostate cancer with a drop of blood and Gulf War technology
London, Ontario - Gulf War technology is making it possible for researchers to detect prostate cancer with a single drop of blood.
Hon Leong, PhD, assistant professor at Western University’s Schulich School of Medicine and Dentistry and scientist at Lawson Health Research Institute, and his team have repurposed a machine once used to detect airborne pathogens in the second Gulf War. The machine is now used for fluid biopsies – a non-invasive way to detect prostate microparticles in the blood in a matter of minutes. Microparticles are essentially garbage released by prostate cells that circulate throughout the bloodstream.
Most men who are more than 40 years old, regardless of their health, have detectable levels of prostate microparticles in their bloodstream. Leong’s research is the first clinical cancer research project to correlate the number of microparticles in the blood to the risk of having prostate cancer – the more microparticles, the higher the risk.
Used in the Gulf War, and more commonly to test water purity, the machine uses flow cytometry to detect microparticles. Flow cytometry measures the specific characteristics of a fluid, such as blood, as it passes through a laser.
Leong’s research provides a more accurate and less invasive testing method for patients suspected of having prostate cancer, and helps to identify patients who are at a higher risk of dying from prostate cancer.
Current methods of detecting prostate cancer, such as the prostate-specific antigen (PSA) test and biopsies, have limitations. PSA tests are based on measuring a specific protein released by the prostate gland, but do not provide a definitive diagnosis. A physical exam and biopsy are needed if PSA levels are elevated. However, even the painful biopsy procedure has a 15 per cent error rate. During biopsies, a painful and invasive procedure, 12 needles are inserted into the rectum, with the hope of extracting material from an area with a tumour.
“Our findings point to a new direction in how we can better identify patients who actually have prostate cancer,” said Leong. “With this test, we can improve the clinical outcomes for patients, reducing costs for unnecessary procedures and reducing errors in diagnosis.”
- 30 -
See all Lawson Media Releases
Western delivers an academic experience second to none. Since 1878, The Western Experience has combined academic excellence with life-long opportunities for intellectual, social and cultural growth in order to better serve our communities. Our research excellence expands knowledge and drives discovery with real-world application. Western attracts individuals with a broad worldview, seeking to study, influence and lead in the international community.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Detecting the Undetectable
A simple fall can lead to long-term hand problems such as arthritis due to fracturing the scaphoid bone in the wrist. Scaphoid fractures are known to have the highest rate of healing failures. While this bone’s fragile blood supply is commonly thought to be the main reason for why it is difficult to heal, Dr. Ruby Grewal is looking into a different reason – infection.
Infections are known to cause difficulty in healing bones, but traditional tests for infections in the scaphoid have come up negative. With new advancements in detecting microbial DNA, scientists can now test for ‘clinically undetectable’ infections.

In a new study, Dr. Grewal will use microbial DNA test whether or not there are infections in the scaphoid fracture which causes improper healing of the bone.
“The goal of this study is to use advanced DNA sequencing technology to test whether or not we can detect evidence of microorganisms in non-healing scaphoids,” explains Dr. Grewal, Lawson Scientist and Orthopaedic Surgeon at the Roth McFarlane Hand and Upper Limb Centre (HULC) at St. Joseph’s Health Care London.
Finding new causes of improper healing of the scaphoid bone could improve treatments for individuals with these injuries and prevent long-term problems with hand function. These insights into the causes of improper healing could also prevent young patients from developing wrist arthritis.
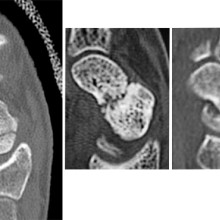
From left to right: Normal scaphoid fracture. Scaphoid fracture that is struggling to heal. Scaphoid non-union where the bone has failed to heal.
Dr. Grewal’s study is being funded through the Lawson Internal Research Fund (IRF).
“The financial support provided by Lawson’s IRF is of utmost importance to researchers. These funds will allow our team to embark on a new area of research and test a novel hypothesis,” says Dr. Grewal, “While traditional granting agencies are reluctant to fund completely novel areas of research without pilot data to prove feasibility, the Lawson IRF allows researchers to investigate new theories in a sound scientific manner. Without the ability to test new ideas we cannot innovate and make advancements in health care. Support for this project allows for that.”
Lawson’s IRF is designed to provide Lawson scientists the opportunity to obtain start-up funds for new projects with the potential to obtain larger funding, be published in a high-impact journal, or provide a clinical benefit to patients. Funding is provided by the clinical departments of London Health Sciences Centre and St. Joseph’s Health Care London, as well as the hospital foundations (London Health Sciences Foundation and St. Joseph’s Health Care Foundation).
Diagnosing COVID-19 using artificial intelligence
LONDON, ON – A team of researchers at Lawson Health Research Institute is investigating whether an artificial neural network could be used to diagnose COVID-19. The AI system is being trained to learn and recognize patterns in ultrasound lung scans of patients with confirmed COVID-19 at London Health Sciences Centre (LHSC) by comparing them to ultrasound scans of patients with other types of lung infections.
“Machines are able to find patterns that humans cannot see or even imagine. Lung ultrasound scans of patients with COVID-19 pneumonia produce a highly abnormal imaging pattern. This pattern isn’t unique to COVID-19, and can be seen in other causes of pneumonia. It is plausible, however, that there are details that distinguish COVID-19 at the pixel level that cannot be perceived by the human eye,” explains Dr. Robert Arntfield, Lawson Researcher and Medical Director of the Critical Care Trauma Centre at LHSC. “If we can train a neural network to learn and identify these unique characteristics among different scans, we can apply this AI to enhance the diagnostic power of portable ultrasound.”
Point-of-care ultrasound has become increasingly important for the care of critically ill patients and LHSC is a global leader in the use of this technology at the bedside. Lung ultrasound has proven to be effective in diagnosing different types of lung infections and illnesses, such as pneumonia, with a high degree of accuracy. The convenience, portability and low cost of using these machines has helped them become a standard bedside tool in emergency departments and intensive care units worldwide.
This research project is part of a grassroots effort by a small group of local clinicians to innovate and create technology to solve sophisticated problems with AI. With many of Dr. Arntfield’s team having a background in computer programming, they were able to code the neural network being tested. Minimal funding was required, with the project being driven largely by the urgency of COVID-19 coinciding with the recent creation of this clinical AI working group.
“Our research team has used AI to help improve diagnostics related to other parts of the body. This project is a great example of the unique ability we have here in London to be agile: that is, to identify a gap and move quickly towards finding a solution,” says Dr. Arntfield. “I am thrilled that we were able to move through the approval process quickly, and get our ideas working in such a short amount of time.”
-30-
Downloadable Media
Dr. Robert Arntfield
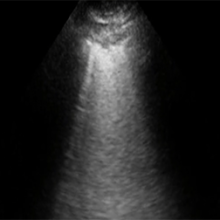
COVID-19 pneumonia ultrasound
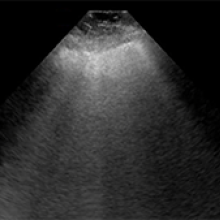
NON COVID-19 pneumonia ultrasound
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca

