Search
Search
Leveraging technology to diagnose psychiatric disorders
Psychiatric disorders are often difficult to diagnose. As research advances, we are learning there are multiple subtypes of illness that differ in symptoms and treatment needs, making classification even harder. Post-traumatic stress disorder (PTSD) is one example. Individuals with the more common type of PTSD experience active defensive responses like hyperarousal or outbursts of emotion while those with the dissociative subtype experience additional passive defensive responses like ‘shutting down’ or out-of-body experiences.
In a new study from Lawson Health Research Institute and Western University, researchers combined brain imaging and machine learning to classify with 92 per cent accuracy whether individuals had PTSD and whether or not it was the dissociative subtype. The results highlight the promise of brain imaging as a tool for early diagnosis of psychiatric illness, helping to predict symptom development and treatment needs.
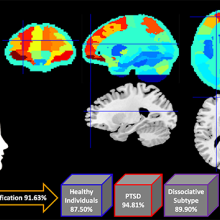
Brains scans and machine learning were combined to classify PTSD with 92 per cent accuracy.
The study involved 181 research participants, including those diagnosed with the more common form of PTSD, the dissociative subtype of PTSD, and healthy individuals with no history of PTSD. They participated in functional magnetic resonance imaging (fMRI) at St. Joseph’s Health Care London and Robarts Research Institute.
Researchers used the high-powered imaging to analyze patterns of resting-state brain activity where participants simply remained in a state of restful wakefulness in an fMRI scanner. The team found that unique patterns of brain activity differed significantly between the three groups.
“Our research group has been leading a number of studies that have shown differences in brain activity and neural connections between healthy individuals and those with different subtypes of PTSD,” says Dr. Ruth Lanius, a researcher at Lawson, professor at Schulich School of Medicine & Dentistry at Western University and psychiatrist at London Health Sciences Centre. “This study further validates that unique patterns of brain activity are associated with different forms of PTSD.”
In the second part of the study, the research team inputted the patterns of brain activity into a machine learning computer algorithm. They found the machine learning system could analyze brain scans to predict whether an individual had PTSD, the dissociative subtype of PTSD or no PTSD with 92 per cent accuracy.
“Our study suggests brain activity can be used to assist diagnosis of psychiatric disorders and help predict symptoms,” says Andrew Nicholson, PhD, lead author on the study and a post-doctoral fellow at Schulich Medicine & Dentistry who is conducting research at Lawson. “Patterns of brain activity are objective biomarkers that could be used to diagnose PTSD and, with more research, even predict response to treatment.”
Objective biomarkers hold promise for transforming psychiatric medicine.
“The field of psychiatry does not currently have objective biomarkers like those used to diagnose and understand other illnesses or diseases like cancer,” says Nicholson. “By discovering and validating patterns of brain activity as biomarkers, we can bring objective measures to psychiatry and transform patient care.”
The study, “Machine learning multivariate pattern analysis predicts classification of posttraumatic stress disorder and its dissociative subtype: A multimodal neuroimaging approach,” is published in Psychological Medicine.
Leveraging virtual reality to manage pain in paediatric patients
London - A new study underway through Lawson Health Research Institute and Children’s Hospital at London Health Sciences Centre (LHSC), using virtual reality (VR) to help pediatric patients during painful and distressing procedures.
“Technology holds immense potential for improving the experience of our young patients and their families,” explains Dr. Naveen Poonai, Lawson Scientist, principal investigator and Emergency Department Physician at Children’s Hospital. “VR is becoming increasingly popular amongst young people and some early research shows VR has been helpful in painful procedures, even in adults.”
The study is focusing on pediatric patients who need port access. A port is a little reservoir that sits underneath the skin that allows access to blood or medication with the use of a needle. Ports are most commonly used in pediatric cancer patients.
“This can be very distressing for a patient and it can set the tone for their entire clinic day and course of treatment,” says Dr. Alexandra Zorzi, Lawson Associate Scientist and Pediatric Oncologist at Children’s Hospital. “Minimizing the stress, anxiety, and pain of the procedure is key to avoiding a negative experience.”
The study team is recruiting 90 pediatric patients with existing medical ports. Participants will be randomized into three groups. One group will be using a VR headset that will allow them to play interactive games. The second group will have access to tablet technology, and the final group will be provided with non-technology distractions. Each procedure and the patient’s response will be recorded. Responses will then be compared using a tool called the ‘Observational Scale of Behavioral Distress’ to determine which intervention leads to the best outcomes.
“My hopes are that we develop a variety of skills we can tailor to patients,” adds Dr. Zorzi. “There are patients who receive all kinds of support but still struggle, so having a variety of techniques available to see what works best is a positive step forward.”
The study is expected to be completed by the end of this year. The research team is already collaborating with Children’s Hospital staff and leadership to use VR as a clinical tool if the study proves the technology to be effective.
“We have plans in place to allow whatever we find as the best option to be part of routine care for kids needing port access,” notes Dr. Poonai. “We are also speaking with various medical teams to determine how we can incorporate this into practices across the hospital.”
The use of the VR devices has been made possible with generous support from the Children’s Health Foundation.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
LHSC and St. Joseph’s introduce new research institutes
Lawson Research Institute at St. Joseph’s and London Health Sciences Centre Research Institute will strengthen hospital-based innovation in London, Ontario
LONDON, Ont. – Today, London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London (St. Joseph’s) unveiled new research institutes designed to strengthen hospital-based innovation. Lawson Research Institute (Lawson) at St. Joseph’s and London Health Sciences Centre Research Institute (LHSCRI) will leverage each hospital’s unique areas of clinical focus while further integrating research with care, helping to advance discoveries that lead to improved patient outcomes.
The new institutes were announced at a launch event with guided open house tours taking place across LHSC’s Victoria Hospital, Children’s Hospital and University Hospital, as well as at St. Joseph’s Hospital and Parkwood Institute. Attendees were able to experience signature research areas, including aging, mental health and microbiome research at Lawson, as well as cancer, children’s and mental health research at LHSCRI. The day included demonstrations of discoveries that are reshaping care in Ontario and around the world, including a new robotic, body-weight support for people with mobility difficulties and studies using artificial intelligence (AI) to diagnose rare diseases.
“When research takes place in a hospital context, scientists have more direct connection to the needs of the patients they serve,” said Roy Butler, President and CEO of St. Joseph’s. “There’s data to show that patients treated in research-intensive hospitals live longer because they have access to cutting-edge science. All patients benefit, not just those involved in clinical trials – and that’s the power of health research. That’s why this milestone day and the discoveries to come are real cause for celebration.”
LHSC and St. Joseph’s have been innovating for more than 150 years. The research institutes will build on the legacy of scientific excellence at both organizations. Their launch marks the completion of the transition from Lawson Health Research Institute, a research brand shared between the two organizations since 2000.
“We’re building on our history while introducing the next era in health research excellence, ensuring we will continue to attract the brightest minds in science and that patients will receive world-class, innovative care,” said David Musyj, Supervisor, LHSC. “We will continue to collaborate with each other, Western University, and health research partners across the country and around the world, bolstering London’s position as a national hub for health research.”
Research teams across Lawson and LHSCRI will continue to collaborate closely on projects and large scientific initiatives. LHSC and St. Joseph’s will also continue to share administrative support for research activities.
Learn more about the new research institutes and their transformative work at:
Lawson Research Institute
London Health Sciences Centre Research Institute
-30-
For more information, please contact:
Celine Zadorsky
Senior Media Relations Consultant
London Health Sciences Centre
(226) 927-2309
OR
Debora (Flaherty) Van Brenk
Communications Consultant
St. Joseph’s Health Care London
226-577-1429 or 519-318-0657
About Lawson Research Institute: Lawson Research Institute, the health innovation arm of St. Joseph’s Health Care London, is committed to making and sharing discoveries that improve lives locally and internationally. Every day, Lawson’s 250-plus scientists work to transform imagination to innovation to patient impact. Lawson leads health-care research. Find us online at sjhc.london.on.ca/research and on social media @stjosephslondon
About London Health Sciences Centre Research Institute: At London Health Sciences Centre Research Institute (LHSCRI), our teams pioneer discoveries that transform the health of adult and paediatric patients around the world. As the research institute of London Health Sciences Centre (LHSC), we conduct research where patient care is delivered, working alongside patients, families, health-care providers and academic partners like Western University. We are leaders in advancing the understanding, diagnosis, treatment and management of diseases and health conditions through a diverse research program that ranges from laboratory-based science to clinical trials. Our research has a global impact as we build on LHSC’s 150-year legacy of health innovation and drive forward medical breakthroughs that make a difference in the lives of patients and their families. Find us online at www.lhscri.ca and on social media @LHSCRI.
Local COVID-19 research supported by St. Joseph's Health Crisis Fund
St. Joseph’s Health Care London and Lawson Health Research Institute have announced plans to move forward with clinical trials testing a drug that could potentially be used to prevent and treat COVID-19. St. Joseph’s Health Care Foundation will accelerate the creation of the studies by providing seed funding to get the research started through donor support. Based on the immediate need, The St. Joseph’s Health Crisis Fund has been created by St. Joseph’s Health Care Foundation to enable these and other research studies currently in development through Lawson, the research arm of St. Joseph’s.
While supporting urgent COVID-19 clinical trials will be an immediate focus, The St. Joseph’s Health Crisis Fund will also support critical patient care equipment and care and comfort items for healthcare staff and volunteers working on the frontlines of the pandemic across St. Joseph’s.
Led locally by Dr. Michael Silverman, Medical Director of St. Joseph’s Infectious Diseases Care Program, one trial will assess the safety and efficacy of using hydroxychloroquine (HCQ) to prevent COVID-19 in health care workers recently exposed to the virus. This trial will also assess the drug as a treatment for non-hospitalized patients with mild cases of the illness. St. Joseph’s will be one of many participating sites in the trial, which is being led by the Research Institute of the McGill University Health Centre.
“There is much debate surrounding the drug hydroxychloroquine. We do not yet know whether it’s safe or effective, and it should not be routinely recommended until we do,” says Dr. Silverman, also a Lawson Associate Scientist and city-wide Chair/Chief of Infectious Diseases. “We plan to carefully study the drug through a randomized controlled trial and assess whether it can help combat COVID-19.”
Dr. Silverman is also partnering with Dr. Michael Borrie, Geriatrician at St. Joseph’s and Lawson Scientist, on a prevention trial to test the safety and efficacy of the drug for patients and residents at Parkwood Institute who have been exposed to COVID-19. They are at a higher risk of infection, as well as serious complications and potential admission to acute care.
“There are two critical goals with this prophylactic trial,” explains Dr. Borrie. “First, we want to see if the drug, taken for five days, is safe for the participants in the study. We will then look to see whether it is effective to prevent illness or lessen symptoms and complications.”
They are testing whether HCQ may inhibit the coronavirus similar to how the antiviral drug Tamiflu is used to prevent influenza after exposure. The research team will recruit patients and residents who have been accidentally exposed to the virus by a confirmed or presumed case of COVID-19, but who aren’t yet experiencing symptoms. In addition to cardiograms and blood tests for safety, they are collaborating with Dr. Saman Maleki, Lawson Scientist and Immunologist, to analyze the blood for a variety of indicators including the presence of antibodies and immune response. They will collect clinical data and information on common health conditions to gain insights into why some vulnerable individuals get the disease and others don’t.
“We are aware of two small studies that were published rapidly last week, one in France and the other in China, testing the use of chloroquine for potentially treating COVID-19. Further studies are greatly needed,” adds Dr. Borrie. “This study at Parkwood Institute is a good start and we hope to have other Canadian sites join us in recruiting participants so that we can offer statistically significant results as soon as possible.”
Those interested in donating to St. Joseph’s Health Crisis Fund are asked to visit St. Joseph’s Health Care Foundation’s website to learn more at sjhcfoundation.org. Donations can be made online, through direct mail submissions or by calling the Foundation directly at 519-646-6085.
“The Sisters of St. Joseph, who founded our organization, faced contagious diseases and other pandemics at different times in our 150+ year history,” says Michelle Campbell. “Today, it’s a different time, and a new disease. Now, more than ever, we ask our community to help us address the crisis facing us all.”
In the news:
Local researchers using artificial intelligence to lead the way in bedside lung imaging
LONDON, ON- A team at Lawson Health Research Institute are testing a new form of artificial intelligence (AI), paired with portable ultrasound machines, to image and identify lung concerns in real time, right at the beside of critically ill patients.
Approximately 100 critical care patients at London Health Sciences Centre (LHSC) will be part of this study which will test whether an AI model can automatically determine the presence of abnormal lung signals. Past studies have suggested that the AI model is very accurate in reading stored images, but this study will evaluate if it retains accuracy when asked to interpret live images being generated at the beside.
The study is made possible through the use of novel hardware created in Waterloo, Ontario by startup tech company, Wavebase.
“The (WaveBase) device attaches to the ultrasound machine and mirrors the ultrasound image in a second screen,” explains Dr. Robert Arntfield, Lawson researcher and Medical Director of the Critical Care Trauma Centre at LHSC. “The AI model searches the images for patterns in real time and predicts whether it is ‘seeing’ normal or abnormal lung tissue.”
Although bedside lung ultrasounds are commonly used in critical care to detect concerns such as infections, pneumonia or a collapsed lung, the pairing with real time diagnostic AI is a research milestone. It could expand the usage of bedside ultrasounds by enabling those with little or no ultrasound training to use the device.
“Bedside lung ultrasounds in critical care can often have a large impact in identifying life-threatening conditions within minutes,” says Dr. Chintan Dave, Critical Care Medicine Fellow at LHSC and Western University. “We would like to see members of the healthcare team, like critical care nurses or respiratory therapists, be able to use AI to accurately determine the health of the lungs rapidly at the bedside. Employing AI into the clinical workflow, could improve access to immediate diagnoses and treatments.”
In order to be certain that the AI’s predictions are accurate, the phase one study will compare its interpretations to a gold standard experts’ interpretation of the same lung ultrasound scans. Once this accuracy is assured, the team will proceed with a second phase to assess the device with non-expert users and customized settings for more in-depth diagnostics.
“We see a bright future for lung ultrasound imaging with AI within the critical care environment,” adds Dr. Arntfield. “We are trying to write the first chapter of this meaningful AI story here at LHSC and Lawson.”
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Local scientists creates novel test that could easily diagnose repetitive blast injury
LONDON, ON- In a world first, researchers at Lawson Health Research Institute, together with scientists from Defence Research and Development Canada, have developed a breath test that could be used to diagnose repetitive blast injury – a mild traumatic brain injury resulting from pressure changes that occur during explosions. The device will soon go through clinical trials to validate its efficacy.
“A pressure wave is sent through the head and brain after an explosion, resulting in effects similar to a concussion,” says Dr. Douglas Fraser, Scientist at Lawson and Professor at Western University’s Schulich School of Medicine and Dentistry. “Examples of individuals who are most at risk of this condition include military personnel, police, individuals in the mining industry and tragically the public, who are currently experiencing this first hand through the war in Ukraine.”
The test leverages findings from a new peer-reviewed study in the Journal, Frontiers in Neurology. The research team examined blood biomarkers in members of the Canadian Armed Forces who have experienced repetitive blasts.
“When we looked at these service personnel there were certain metabolites in their blood that had changed quite dramatically compared to those who had not been exposed to blast injury,” explains Dr. Fraser, who is also a Paediatric Critical Care Physician at London Health Sciences Centre. “What was remarkable about these metabolites is that some of them are expelled in a person’s breath.”
Currently there is no accurate way to diagnose repetitive blast injury other than relying on a patient’s history and symptoms. Using their findings, the research team has identified a combination of metabolites that can be measured in breath as a diagnostic test.
“The individual would blow into what looks like a straw and the breath would go into a device which would measure the metabolites of interest,” adds Dr. Fraser. “The device would then determine if the person is in the danger zone, or if they have been exposed to too many blasts.”
Dr. Vivian McAllister, Director of the Office of Military Academic Medicine at Schulich Medicine & Dentistry says this discovery could be a game changer when it comes to this condition.
“The symptoms of blast injury overlap with other neurological conditions, especially depression, so accurate diagnosis is essential,” says Dr. McAllister. “Early diagnosis allows for interventions that we know to be successful in reducing the symptoms and consequences of mild traumatic brain injury.”
The test has been developed and patented with WORLDiscoveries, the technology transfer and business development office for Lawson and Western, and licensed to Neuroltixs Inc. for development. The next steps will be to confirm the efficacy of the test through upcoming clinical trials.
“We hope to validate the breath aspect of the test, which could then be used as a health surveillance tool,” says Dr. Fraser. “Once validated through clinical trials, this portable device could be easily developed and it will allow us to determine who has been over exposed to blast injuries and how we can protect them in the future.”
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Locally developed test found to increase diagnosis of rare hereditary disorders
LONDON, ON – A clinical trial named “EpiSign-CAN,” led by researchers at Lawson Health Research Institute (Lawson) has been awarded $4.8 million to measure the clinical impact of a new molecular genomics test for diagnosing genetic neurodevelopmental conditions.
Developed at Lawson, the diagnostic test, called EpiSign, uses machine learning to analyze the EpiSign Knowledge Database. This database compiles information on rare genetic diseases using laboratory analyses of the entire genome, referred to as the epigenome, from patients with suspected genetic abnormalities.
A recent paper describes the newly discovered biomarkers for over 50 neurodevelopmental conditions. Dr. Bekim Sadikovic, Lawson Scientist and Head of the Molecular Diagnostics Division at London Health Sciences Centre (LHSC) explains, “before this study, many such conditions required targeted, and often labour intensive and costly assays for a diagnosis, which in many cases provided no conclusive answers. Now, using our EpiSign Knowledge Database which includes the epigenomic information of thousands of patients and controls, we are able to diagnose over 50 conditions with a single test, including in patients where targeted genetic testing was inconclusive.”
The upcoming clinical trial hopes to validate the use of this test in the first-line of diagnosing rare genetic disorders across Canada. “Patients and families typically wait years, and undergo multiple exams and lab tests in search of a definitive diagnosis. With EpiSign, we estimate that we will be able to increase the number of people who receive a diagnoses by five per cent, or more in the future as the database develops” explains Dr. Sadikovic. “Though individual genetic conditions are rare, there are over 4,000 recognized genetic disorders which affect thousands of patients in Canada.”
EpiSign-CAN will study 4,000 patients, who will either receive EpiSign testing as part of the initial diagnostic workup or after classical genetic testing approaches have been exhausted. The goal is to assess the impact of using EpiSign in the first stage of diagnosis vs. after other tests have failed to provide answers in this patient population.
Timely diagnosis will prevent the so called “diagnostic odyssey,” and by doing so has the potential to improve healthcare outcomes for these patients and decrease cost to the health system.
As the EpiSign Knowledge Database continues to grow, researchers are finding correlations between specific episignatures, or molecular DNA markers, and related physiological features across a syndrome.
This research is co-funded through the collaboration of three partners; LHSC, Illumina, and Genome Canada. This is the first time researchers at Lawson have been awarded a Genome Canada Genomic Applications Partnership Program (GAPP) grant. “Genome Canada focuses its resources on new innovation that has a strong likelihood of translating directly to patient care. Their support of our work is extremely meaningful,” says Dr. Sadikovic.
The study describing the most recent advancements in EpiSign technology, “Evaluation of DNA methylation episignatures for diagnosis and phenotype correlations in 42 Mendelian neurodevelopmental disorders,” is published in The American Journal of Human Genetics.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
London comes in eighth place in Canada’s Top 40 for hospital-based research
Lawson Health Research Institute has ranked eighth in the country for the 2021 edition of Canada’s Top 40 Research Hospitals List by Re$earch Infosource. This is the eighth consecutive year that Lawson has maintained this strong national position, which puts the institute within the top five in Ontario.
Lawson, the research institute of London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London, has also maintained the top ranking for research intensity among the large tier institutions with a little more than $600,000 of research spending per researcher.
“This is a validation of the extensive support from LHSC and St. Joseph’s, our hospital foundations, Western University and our staff and physicians,” says Lawson’s Scientific Director Dr. David Hill. “These strong partnerships make the hospital environment in London a nationally recognized centre of discovery and knowledge translation.”
Hospital-based researchers belong to a health system at the forefront of the ongoing COVID-19 pandemic. With close proximity to patients and access to samples, they have mobilized to address COVID-19 in many different ways, and are making a difference around the world when it comes to advances and discoveries.
“The Province of Ontario designated health research as an essential service early in the pandemic,” explains Dr. Hill. “They understood that only science can get us through this, be it through vaccine development, surveillance and testing, evaluating new drugs to help patients in ICU survive, or studying the long-term health impacts. We have made substantial contributions of new knowledge through Lawson.”
The top 40 list analyzes hospital-based research institutes from across the country on several metrics, including total research income from the previous fiscal year. According to the report, Lawson received $121,888 million in research income in 2021.The ranking looks at funds received from all sources, including both internal and external, to support research at LHSC and St. Joseph’s.
Quick summary of Lawson’s ranking
- Rank in Top 40 Research Hospitals 2021: 8 (same as 2020)
- FY2020 research spending: $121.888 million
- Percentage change 2019-2020: 2.6%
- Research intensity: $618,700 per researcher
- Research intensity - percentage of total hospital spending: 7.0%
London expands approach to prevent discharge from hospital to homelessness
LONDON, ON - During a virtual event for Londoners hosted by Lawson Health Research Institute and the City of London, a multi-sectoral research team announced two projects representing a collaborative approach to preventing homelessness from within hospital walls.
Built on the unique and successful No Fixed Address (NFA) strategy, these projects are being tested as a potential best practice for preventing hospital discharge to homelessness. NFA seeks to stop the cycle between hospital admissions and homelessness by providing timely and accessible supports to patients who would otherwise be discharged into homelessness. It brings housing and financial supports into the health-care system, starting as soon as upon admission, to assist in finding appropriate housing and supports or avoiding a potential eviction.
“Canada lacks a validated and coordinated service model to address the issue of hospital stay to no fixed address, which can often be the beginning of an individual’s experience with homelessness,” explains Dr. Cheryl Forchuk, Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, and Assistant Scientific Director at Lawson. “There are multiple factors that cause people to be discharged into homelessness - systemic, organizational and personal. We need a collaborative and coordinated approach that honours housing as a basic human right.”
Several departments at London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London collaborate with staff from the City of London, Canadian Mental Health Association (CMHA) Elgin-Middlesex, Youth Opportunities Unlimited (YOU), Salvation Army’s Housing Stability Bank and Ontario Works in the City of London to provide direct, on-site (or virtual) support for patients at risk of homelessness.
“Implementing a coordinated approach to addressing homelessness allows our staff to actively work alongside our partners in health care to prevent and divert individuals and families from an experience of homelessness by assessing their needs and connecting them to the housing supports.,” says John D’Oria, Coordinated Access Manager, City of London. “Whether it’s financial, social service or mental health support, this partnership and approach allows for a holistic approach to client care at the right time.”
Patients discharged from hospital to homelessness in Canada face many challenges that make recovery more difficult. They often experience higher readmission rates and emergency department visits. This is particularly concerning for youth, who have been found to be the fastest growing segment of the homeless population.
NFA was initially tested with strong success for mental health patients across the city and the second version of the project was extended to medical units at LHSC’s University and Victoria Hospitals.
PROJECT 1: Collaboration to Address Homelessness - Health, Housing and Income (H2I)
This research study will evaluate the City of London’s Coordinated Access Outreach program at hospital sites. A Coordinated Access Outreach worker will support individuals at risk of homelessness to maintain or obtain housing. Ontario Works will assist with the provision of income and employment supports and the Salvation Army Housing Stability Bank may be accessed for needed financial resources to secure or maintain housing.
Over two years, 106 participants will be interviewed in hospital and again six months post-discharge. Focus groups with participants, health care providers and community partners will provide further insight into the effectiveness of NFA. This project is funded by the Canada Mortgage and Housing Corporation (CMHC)’s National Housing Strategy.
PROJECT 2: Preventing discharge to No Fixed Address – Youth (NFA-Y)
This research study will customize, implement and evaluate the NFA strategy for vulnerable youth ages 16-24. The unique health and housing needs of youth at-risk will be explored by streamlining housing and financial support into a coordinated system of care, with additional support provided by Youth Opportunities Unlimited and Children’s Aid Society London and Middlesex.
Over 3-4 years, data to be collected from 93 youth at three time points. Focus groups with youth participants, health care providers, and community agency partners will help enhance the NFA strategy to meet the unique needs of youth. This project is funded by the National Centres of Excellence (NCE) Making the Shift (MtS) Youth Social Innovation Lab.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca