Search
Search
Could microorganisms in poop help treat the deadliest form of skin cancer?
A multidisciplinary team at Lawson Health Research Institute is exploring whether fecal transplants can improve outcomes in melanoma patients treated with immunotherapy.
Immunotherapy drugs stimulate a person’s immune system to attack and destroy cancer. While they can significantly improve survival outcomes in those with melanoma, they are only effective in 40 to 50 per cent of patients. Preliminary research has suggested that the human microbiome – the diverse collection of microbes in our body – may play a role in whether or not a patient responds.
“The gut microbiome helps establish immunity from an early age. It makes sense that a healthy gut could improve response to immunotherapy,” explains Dr. Jeremy Burton, a Lawson Scientist who specializes in human microbiome research. “This led us to consider the potential of fecal transplants.”
Fecal transplants involve collecting stool from a healthy donor, preparing it in a lab and transplanting it to the patient. The goal is to transplant the donor’s microbiome so that healthy bacteria will colonize in the patient’s gut.

Above (from left): Drs. Michael Silverman and Jeremy Burton
In a phase I clinical trial, the research team is the first in Canada to study the use of fecal transplants to alter a cancer patient’s microbiome and improve their response to anti-PD1 immunotherapy drugs.
Research participants will be 20 melanoma patients recruited from the London Regional Cancer Program (LRCP) at London Health Sciences Centre (LHSC). They will undergo a fecal transplant at St. Joseph’s Hospital, a part of St. Joseph’s Health Care London, followed by immunotherapy at LRCP. The transplant will consist of taking a number of specially-prepared oral capsules.
Patients will be assessed over time for any changes to their cancer, microbiome, immune system and overall health. The primary goal of the study is to evaluate safety of the novel treatment combination, but researchers will also evaluate patient outcomes.
“Melanoma is the least common skin cancer but it is the most deadly and rates are going up,” says Dr. John Lenehan, Associate Scientist at Lawson and Oncologist at LHSC. “Anti-PD1 immunotherapy drugs can be extremely effective but we want to help more patients respond. That’s our goal.”

Above (from left): Drs. Saman Maleki and John Lenehan
While the team is studying the combination of fecal transplants and immunotherapy for melanoma, they see potential for other cancers as well.
“We’re one of the first in the world to study fecal transplants in cancer patients. This study is as cutting-edge as it gets with potential applications for multiple disease sites,” notes Dr. Saman Maleki, a Lawson Associate Scientist who specializes in cancer immunology. “With experts in microbiology, infectious disease, cancer and immunology, our institute is well-positioned to carry this forward.”

Dr. Michael Silverman, Lawson Associate Scientist and Chief of Infectious Disease at St. Joseph’s and LHSC, is a pioneer in the field of fecal transplants. St. Joseph’s is a leading centre for the procedure, performing them for Clostridium difficile (C. diff) patients across the province.
“Fecal transplants have saved the lives of countless patients with recurrent C. diff,” says Dr. Silverman. “We’re now starting to see its potential for the treatment of other diseases.”
Lawson researchers are planning fecal transplant studies for multiple other conditions including non-alcoholic fatty liver disease, multiple sclerosis (MS) and cancer treatment toxicity.“But in order to conduct this research, we need stool donors,” notes Dr. Silverman.
Check out media coverage of this research:
- CTV News: Why fecal transplants could be the next frontier in fighting skin cancer
- Forbes: Could poop be the next treatment for cancer?
- London Free Press: Researchers seeking poop donors for skin cancer treatment study
- Daily Mirror: How human poo 'transplants' could help doctors treat deadliest form of skin cancer
- CBC: London cancer researchers make number 2 their number 1 priority
Cultivating ‘eureka’ moments
Discovery should be ‘everyone, everywhere,’ says Lawson Research Institute Scientific Director Lisa Porter.
Lisa Porter believes excellence in health research is a continuum of inquiry, inspiration, innovation and improved patient care.
That’s why she is so energized by the promise and potential of Lawson Research Institute (Lawson) at St. Joseph’s Health Care London (St. Joseph’s), where she is Scientific Director and Vice President Research.
“Discovery comes from exploring great questions. You can’t have a ‘eureka’ moment without asking why things work, or don’t work – and that’s what we do so well here at St. Joseph’s,” says Porter.
A distinguished scientist herself with a passion for asking those probing questions, Porter leads strategic planning for research across the organization. Her vision includes growing the rich culture of research in several specialty pillars, while also reinforcing direct links between scientific inquiry and patient health.
“There’s data to show that patients who are treated in research-intensive hospitals live longer. That’s not just patients in clinical trials who benefit; that’s all patients who live longer,” she notes.
Other elements of her vision for Lawson include elevating data sharing and research support, expanding training opportunities for young researchers, growing grant support, strengthening collaboration and partnerships, and building relationships and reputation.
“I love that excellence is one of the values of St. Joseph’s. Excellence doesn’t mean we have all the answers. It means we’re continuously striving to be better. It means we’re asking questions that can drive better health care – not just for the patients we serve, but for national and global impact, too.”
Porter comes from a family of knowledge-seekers and problem-solvers. Her father repaired electronics and was an avid inventor. Her mother was a self-taught income –tax preparer with meticulous attention to detail. They ignited in her a curiosity that continued through her undergraduate studies in biology and pharmacology, her graduate and postdoctoral work, and her research as a cancer scientist at University of Windsor and founding director of its WE-SPARK Health Research Institute.
Now at Lawson, she wants to encourage, inspire and spotlight the innovative work of researchers, scientists, clinicians and students who are passionate about improving health.
“I want research to be everyone, everywhere,” she says. “We need hospitals, industry, people with lived experience, and policy makers coming into the fray. It can’t be just the researcher, the scientist. It’s about having champions embedded in all walks of life, from first line of care to people who can influence systemic change. It’s a messy piece, but it’s also how we fulfil this bigger mission to help everyone who comes to us for health care.”
Database funding could improve diagnosis and treatment of prostate cancer
A $125,000 grant from the Canadian Cancer Society will help create a database of PET/CT (positron emission tomography/computed tomography) and PET/MR (magnetic resonance) images of prostate cancer. The hope is that this database will be used to help improve diagnosis and treatment of men with prostate cancer.
The scans use radiopharmaceuticals to target prostate specific membrane antigen (PSMA), a transmembrane protein commonly found on prostate cancer cells.
“The idea behind this grant is to put together a database of PSMA PET/CT and PET/MR scans with annotated findings so medical professionals can scroll through cases and see the sites of prostate cancer. Our hope is this will help clinicians learn how to interpret these scans and ultimately help them to make informed treatment decisions for their patients,” says Dr. Katherine Zukotynski, Adjunct Scientist at Lawson Health Research Institute and lead researcher on the project.
The use of PSMA PET/CT and PET/MR scans in clinical practice is relatively new and currently only accessible through clinical trials. In fact, the first PSMA PET/MR scan in Canada was performed at St. Joseph’s Health Care London in 2016 by Dr. Glenn Bauman, Lawson Scientist and Radiation Oncologist at the London Regional Cancer Program at London Health Sciences Centre. Dr. Bauman is also part of this database project.
Studies have found these scans more accurately detect sites of prostate cancer than earlier imaging techniques, which then helps inform treatment decisions.
Dr. Zukotynski explains, “If you have an idea of the amount of disease and where it is located, and you can correlate it with prognosis, this could be very helpful. It might also allow physicians to compare current patients with patients who have similar findings, which may help determine the best therapies to try.”
There is hope that eventually this same database could lead to the use of artificial intelligence (AI) to assist in diagnosis and treatment planning.
“PSMA PET/CT and PET/MR may be tools helpful to categorize the total burden of disease, and then establish how that disease changes with therapy. Our first step down this path is to assemble a database that can be used both for research and educational purposes.”
The database will include data from centres across Canada, with a number of researchers contributing to the project funded by the Canadian Cancer Society.
Other principal investigators include: Dr. Bauman; Dr. François Bénard of the BC Cancer Research Institute; Dr. Vincent Gaudet, University of Waterloo; Dr. Phil Kuo, University of Arizona; Dr. Cynthia Ménard, Centre Hospitalier Universitaire de Montreal; and Dr. Ur Metser of the Princess Margaret Hospital. Dr. Carlos Uribe of the BC Cancer Research Centre and Dr. Aaron Ward of Lawson are co-applicants for the grant.
This is the part three of a three-part series on PSMA PET imaging research. Check out part one and two.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Easing the pressure for patients with chronic wounds
Chronic wounds represent a significant burden in Canada. Between four and 30 per cent of patients develop a chronic wound, depending on the health care setting. Over 85 per cent of all Spinal Cord Injury (SCI) survivors will experience health complications related to pressure ulcers, injuries to the skin and underlying tissue resulting from prolonged pressure. These types of wounds can significantly reduce participation in meaningful activities and overall quality of life.
Research from around the world shows that electrical stimulation can help speed the healing of pressure ulcers. This therapy is currently done by a trained health care provider and is not readily available for people across Canada.Electrical stimulation therapy (E-Stim) is a wound treatment that involves applying low levels of electrical current to the wound bed and surrounding tissues. It stimulates several healing processes, promotes local circulation and prevents infections.
The E-Stim Collaboration: A Best Practice Implementation Project for Better Pressure Ulcer Care aims to improve the coordination of pressure ulcer care and promote the use of evidence-informed wound treatments for people living with SCI. In particular, the research project is studying how to best provide E-Stim to people with pressure ulcers, in their own communities.
“Over the years I’ve seen the serious impact pressure ulcers have on the lives of people with spinal cord injury and other health challenges. This is what drives my commitment to not only develop best practice guidelines, but also to ensure they are put into action,” says Dr. Pamela Houghton, Associate Scientist, Lawson and Professor, School of Physical Therapy at Western University. “Advances in technology make it possible for more people with care needs to live at home.”
The pilot project in the South West LHIN has a unique model that builds capacity in the community and taps into the lived experience of people with pressure ulcers and SCI. It brings together the expertise of researchers, clinicians and managers from academia, hospital centres and community care.
Partners include the Parkwood Institute Research program at Lawson Health Research Institute, Western University, Saint Elizabeth’s Health Care Research Centre, Sunnybrook Health Sciences Centre and the South West Community Care Access Centre. An interdisciplinary specialized team, called SCIPUT, has been established within the Spinal Cord Injury Rehabilitation program provided at Parkwood Institute, St. Joseph’s Health Care London.
“Our collaborative team is using the PLAN-DO-STUDY-ACT quality improvement model. This allows us to learn from each cycle and make adjustments as we go,” says Dr. Houghton. “We have just completed the first cycle and are reporting on lessons learned.” Funded by the Rick Hansen Foundation, the team hopes this will set the stage for a larger cross-country initiative.
Those interested in participating can contact phoughto@uwo.ca. The study is open to:
- Individuals with an open pressure ulcer and with a condition that causes limited mobility and/or requires a wheelchair;
- Those who are able and willing to participate in treatment plan, and communicate feedback; and,
- People who are eligible to receive services from South West CCAC.
|
Image
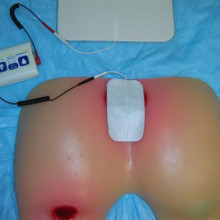
Electrical stimulation (E-Stim) directly stimulates several wound healing processes, promotes local circulation and prevents wound infections. It produces faster healing and wound closure. A trained health care provider applies low levels of electrical current to the pressure ulcer using specialized equipment. |
