Search
Search
Study finds high percentage of patients with a severe COVID-19 infection will end up with kidney injury, often fatal
Acute kidney injury associated with severe COVID-19 leads to high mortality rates
For Immediate Release
Severe cases of a COVID-19 infection can cause a host of serious complications, one of them being acute kidney injury. In a recent published study, scientists at Lawson Health Research Institute (Lawson) have found that acute kidney injury in patients with a severe COVID-19 infection is leading to a high mortality rate.
“These are patients who did not have kidney disease, or kidney injury prior to contracting COVID-19,” explains Dr. Peter Blake, Lawson researcher and Provincial Medical Director at the Ontario Renal Network. “This is what we call acute kidney injury, and in the case of these severe COVID-19 patients the kidney injury led to the need for acute dialysis.”
By accessing data collected through the Ontario Renal Network (ORN), Dr. Blake and his colleagues were able to examine 271 people at 27 renal programs across the province, including patients at London Health Sciences Centre (LHSC), who received acute dialysis for acute kidney injury due to a COVID-19 infection. The data examined was from the duration of the first two waves of the pandemic, up to January 31st, 2021.
“This is a complication that is occurs in 10 per cent of ICU COVID-19 cases,” says Dr. Blake, who is also a nephrologist at LHSC. “Men accounted for more than 75 per cent of this condition, half of the patients were diabetic and the majority of these patients were not seniors in the later stages of life, but rather middle-aged people.”
The provincially-collected data through the ORN also showed that patient populations living in postal codes with high ethnocultural deprivation were more likely to get this condition, at a rate of more than 60 per cent, and survival rates were not promising.
“The mortality rate was shockingly high with 64 per cent of these patients dying within 90 days,” adds Dr. Blake. “Many of those who survived remained in hospital for a long period of time and the one in five that did survive have remained on long-term dialysis.”
This study has been published in the Clinical Kidney Journal. Looking ahead, the research team plans to follow up with patients who have survived this severe complication to track what lasting health affects occur within a six-to twelve-month post-survival period.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Study results prove success of project aimed at preventing family homelessness
Lawson Health Research Institute, Western University, City of London, and Mission Services of London, Ontario, partnered on the Prevention of Homelessness Among Families (PHAF) project to assess the effectiveness of a shelter diversion pilot-program at Rotholme Women’s and Family Shelter (Mission Services).
The results of the study illustrate that a low percentage of families ended up in shelter when accessing the program, and as many as 90 per cent of the families were known to still be housed 18-months later.
The project was supported by $134,000 in funding delivered through the Government of Ontario’s Local Poverty Reduction Fund (LPRF). The grant, funded by the Government of Ontario and administered by its agency, the Ontario Trillium Foundation, is helping groups disproportionately affected by poverty get into housing, develop skills and find employment in London, Ontario.
This project focuses on local community partnerships and includes a third-party evaluation component, which is important because better data will help communities develop better solutions to increasing food security, reducing child poverty and homelessness, and helping people find jobs and earn a stable income.
Rotholme’s shelter diversion program aims to divert family homelessness by working with families to maintain stable housing prior to eviction. Families at risk of homelessness who contact the shelter before leaving their home are immediately connected with a housing crisis worker. Together, parents and the crisis worker explore alternate housing arrangements, services, and supports.
“To keep families in their home we have a ‘whatever it takes approach.’ Once families have left their homes and belongings it is very difficult to escape homelessness,” says Gordon Russell, director of shelters, Mission Services, of London. A variety of tactics are used to divert families from shelter, such as negotiating with landlords to keep the family in their home or move them into an available unit.
To evaluate the success of the program, researchers assessed administrative shelter data, interviewed parents who participated in the program, and conducted focus groups with staff and families who did not access the program.

Researchers interviewed 20 families at four time points, approximately six months apart. Thirteen families were able to complete all four interviews. In total the information of 75 individuals, including 29 parents and 46 dependents, was collected, and included demographics, specific needs, utilization of health services, and quality of life metrics. A majority of the parents interviewed had never experienced homelessness before accessing Mission Services.
“We found that Rotholme’s pilot program was effective for preventing family homelessness,” explains Dr. Cheryl Forchuk, assistant scientific director at Lawson, and professor of Nursing at Western University. “Family homelessness is a serious problem, one that can be prevented with early intervention according to our results.”
Other themes that emerge from the study suggest:
- families at risk of homelessness may have life challenges such as mental health and addiction issues, language issues, or low level education levels;
- families at risk of homelessness may have a lack of understanding the system including shelter rules, social assistance and school supports and their own rights;
- and, families at risk of homelessness may experience difficulty with conflict, both within the family dynamic and in resolving conflicts with landlords.
“When we know the challenges that families face, we are better equipped to meet their needs and continue to help them live in stable housing,” continues Dr. Forchuk. “Understanding issues of service preference and outcomes from the context of the whole family are critical to planning appropriate services.”
This investment by the Government of Ontario is just one way the province is bolstering innovative local programs that support groups disproportionately affected by poverty. Through the Local Poverty Reduction Fund, Ontario is helping to break the cycle of poverty for children and youth, increase employment and income security, and end homelessness in Ontario.
Study shows fewer higher-dose radiation treatments safe and well tolerated by women with uterine cancer
MEDIA RELEASE
FOR IMMEDIATE RELEASE
Sunnybrook Health Sciences Centre and Lawson Health Research Institute
April 14, 2022
LONDON,ON - Five high-dose radiation treatments targeting uterine cancer rather than the current standard 25 treatments are safe and well-tolerated by patients, a new study published in JAMA Oncology has found.
SPARTACUS (Stereotactic Pelvic Adjuvant Radiation Therapy in Cancers of the Uterus) — a multi-institutional non-randomized controlled trial — looked to assess the feasibility and safety of using a specialized technique called stereotactic body radiation therapy (SBRT) for women with uterine cancer where instead of 25 treatments over five weeks, five treatments can be delivered over 1.5 weeks.
SBRT uses many precise beams of radiation to target tumours or cancerous cells. It uses a higher dose of radiation in a smaller number of treatments. It can be done on a standard linear accelerator, the machine that delivers radiation treatments.
Sixty-one women were enrolled in SPARTACUS at two centres — Sunnybrook Health Sciences Centre and the London Regional Cancer Program (LRCP) at London Health Sciences Centre (LHSC).
“Uterine cancer is a common cancer in women, usually treated with surgical removal followed by radiation and/or chemotherapy to reduce the risk of recurrence,” said Dr. Eric Leung, radiation oncologist at Sunnybrook’s Odette Cancer Centre. “External beam radiation is usually given over five weeks, and that can place a heavy burden on women who have to travel to a radiation centre every day, spend time away from home and work, and incur the financial burden of these factors as well.”
With a median follow-up of nine months, the patients enrolled in SPARTACUS reported an acceptable level of side effects from the radiation that resolved, and also reported a reasonable quality of life during treatment, Dr. Leung said.
“We were interested in examining the toxicity of the higher dose – would it affect the nearby bowels or bladder and place a heavy symptom burden on patients? We were pleased to find that patients reported their symptoms as manageable.”
“This study represents a novel way of treating uterine cancer in a shorter time. It was conducted mainly through the COVID pandemic and gave women a chance to receive treatment in less time with fewer visits to our centres,” said Dr. David D’Souza, radiation oncologist at LHSC and the study co-lead through Lawson Health Research Institute.
Patients will continue to be followed on the study for late side effects and further research is planned to further compare this more convenient schedule to the standard five-week course of radiation.
“This novel treatment could lead to a practice change that places less burden on patients and on the healthcare system,” Dr. Leung said. “Delivering radiation over the course of a week and half rather than over five weeks for patients facing uterine cancer would open up healthcare resources by reducing visits and usage of the linear accelerators.”
-30-
ADDIONAL QUOTES – Dr. David D’Souza:
“Giving radiation in a shorter time can have several advantages for both the patient and the health care system."
“Our study assessed the safety of delivering a higher dose of radiation in fewer treatments for patients with uterine cancer by adapting what has successfully been done for other types of cancer in the pelvis like prostate and rectal cancer.”
“This study was made possible with advances in treatment planning, radiation machine capabilities, and an outstanding radiation therapy program at LRCP.”
ABOUT LAWSON HEALTH RESEARCH INSTITUTE
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
ABOUT SUNNYBROOK HEALTH SCIENCES CENTRE
Sunnybrook Health Sciences Centre is inventing the future of health care for the 1.2 million patients the hospital cares for each year through the dedication of its more than 10,000 staff and volunteers. An internationally recognized leader in research and education and a full affiliation with the University of Toronto distinguishes Sunnybrook as one of Canada’s premier academic health sciences centres. Sunnybrook specializes in caring for high-risk pregnancies, critically-ill newborns and adults, offering specialized rehabilitation and treating and preventing cancer, cardiovascular disease, neurological and psychiatric disorders, orthopaedic and arthritic conditions and traumatic injuries. The Hospital also has a unique and national leading program for the care of Canada’s war veterans.
Media Contacts:
Celine Zadorsky
Communications & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. 75664
C: 519-619-3872
@email
Sunnybrook Health Sciences Centre
Communications & Stakeholder Relations
416-480-4040
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Study validates methods for tracking prevalence and service use of people who experience homelessness
LONDON, ON – A new population-based retrospective validation study, using ICES data collected between 2007 and 2014 in Ontario, has found that health records can be used to track service use as well as the needs of individuals experiencing homelessness. Researchers found that the algorithms tested were able to accurately identify up to 35 per cent of individuals who experience homelessness in a given year.
The best performing algorithm estimated a large increase in homelessness prevalence between 2007 and 2016, with approximately one in 200 adults in Ontario experiencing homelessness in 2016.
“We do not know how many people experience homelessness yearly in Ontario, or in the country as a whole. Current methods rely on shelter data, or large point-in-time counts that require large investments, and are only done in specific communities,” explains Lucie Richard, Lawson researcher and lead author of the study. “Also, not all people who are homeless use shelters. This approach gives us an alternative that can include a wide range of communities and different types of homelessness over time.”
While numerous computer algorithms are already used to analyze administrative databases and identify disease populations to measure the burden of chronic diseases in Canada, this study, conducted by researchers at Lawson Health Research Institute and Western University, is one of the first to validate and track a social determinant of health with good accuracy.
People who experience homelessness often face mental and physical health challenges, have an increased risk of illness and death, and are among the highest users of emergency and other health care services. Homelessness is an important health issue for Canadians.
This ability to track individuals experiencing homelessness over time using administrative databases provides inexpensive, long-term monitoring, which will inform efforts to improve housing and health status in the community and across the country. Researchers and health care providers can now track health status and health care usage of individuals experiencing homelessness.
Understanding how many people experience homelessness and what demographics correlate with homelessness will allow for better service planning, and providers will have the information needed to more appropriately meet the needs of this vulnerable population.
The study, “Validation study of health administrative data algorithms to identify individuals experiencing homelessness and estimate population prevalence of homelessness in Ontario, Canada” is published in BMJ Open.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Western University’s Faculty of Health Sciences (FHS) is committed to bettering the human condition through outstanding training of health professionals, the education of students in the fundamentals of health, disability, and sport, and through the actions of our graduates who integrate the art and science of their disciplines.
The Institute for Clinical Evaluative Sciences (ICES) is an independent, non-profit organization that uses population-based health information to produce knowledge on a broad range of health care issues. Our unbiased evidence provides measures of health system performance, a clearer understanding of the shifting health care needs of Ontarians, and a stimulus for discussion of practical solutions to optimize scarce resources. ICES knowledge is highly regarded in Canada and abroad, and is widely used by government, hospitals, planners, and practitioners to make decisions about care delivery and to develop policy. For the latest ICES news, follow us on Twitter: @ICESOntario
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Study validates methods for tracking prevalence and service use of people who experience homelessness
A new population-based retrospective validation study, using ICES data collected between 2007 and 2014 in Ontario, has found that health records can be used to track service use as well as the needs of individuals experiencing homelessness. Researchers found that the algorithms tested were able to accurately identify up to 35 per cent of individuals who experience homelessness in a given year.
The best performing algorithm estimated a large increase in homelessness prevalence between 2007 and 2016, with approximately one in 200 adults in Ontario experiencing homelessness in 2016.
“We do not know how many people experience homelessness yearly in Ontario, or in the country as a whole. Current methods rely on shelter data, or large point-in-time counts that require large investments, and are only done in specific communities,” explains Lucie Richard, Lawson researcher and lead author of the study. “Also, not all people who are homeless use shelters. This approach gives us an alternative that can include a wide range of communities and different types of homelessness over time.”

While numerous computer algorithms are already used to analyze administrative databases and identify disease populations to measure the burden of chronic diseases in Canada, this study, conducted by researchers at Lawson Health Research Institute and Western University, is one of the first to validate and track a social determinant of health with good accuracy.
People who experience homelessness often face mental and physical health challenges, have an increased risk of illness and death, and are among the highest users of emergency and other health care services. Homelessness is an important health issue for Canadians.
This ability to track individuals experiencing homelessness over time using administrative databases provides inexpensive, long-term monitoring, which will inform efforts to improve housing and health status in the community and across the country. Researchers and health care providers can now track health status and health care usage of individuals experiencing homelessness.
Understanding how many people experience homelessness and what demographics correlate with homelessness will allow for better service planning, and providers will have the information needed to more appropriately meet the needs of this vulnerable population.
The study, “Validation study of health administrative data algorithms to identify individuals experiencing homelessness and estimate population prevalence of homelessness in Ontario, Canada” is published in BMJ Open.
Supporting a rapid research response during the pandemic
LONDON, ON – Hospital-based research is uniquely positioned to tackle the unprecedented COVID-19 challenge and quickly translate results into illness prevention and care for patients. Lawson Health Research Institute, the research institute of London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London, has awarded more than $202,000 to its research teams to support critical discoveries during the pandemic.
Over 14 projects ranging from improved diagnostics to understanding the impact of the COVID-19 pandemic on frontline health-care workers have been funded through Lawson’s Internal Research Fund (IRF) COVID-19 Pandemic Response Competition.
“Lawson researchers are an intrinsic part of health care in London. Our research community has mobilized quickly to the COVID-19 pandemic and has come forth with innovative ideas to prevent infections, aid recovery and reduce the likelihood of mortality in those most seriously affected,” says Dr. David Hill, Scientific Director for Lawson. “Lawson has reallocated internal granting resources to enable some of the most exciting and credible ideas to be explored.”
Launched in March, this rapid response competition was focused on funding projects, such as two described below, that could impact the management of the pandemic and enhance our understanding of the novel coronavirus.
Using genetic therapy to block entry of the virus
Progression of COVID-19 depends on human proteins that the virus uses to escort itself into lung cells to cause disease. “There are three such ‘virus entry’ proteins that are particularly important for infection. We see them as potential targets for drugs to prevent and treat COVID-19,” explains Dr. James Koropatnick, Lawson Scientist and Principal Investigator for one of the funded studies.
There could be dangers in targeting these proteins, particularly for patients taking certain blood pressure-reducing drugs. The team is studying the safe use of a new type of drug – powerful “antisense” agents that block messenger RNAs which are the biological “blueprints” for the target virus entry proteins – to stop the virus from using those proteins to infect lung cells. They are testing two types of antisense molecules that reduce the amount of the virus entry proteins. “With our existing knowledge and infrastructure in place, this testing could rapidly lead to new, non-vaccine agents to prevent and treat COVID-19, as well as future coronaviruses with pandemic potential,” adds Dr. Koropatnick.
The impact of the pandemic response for those with disabilities
The COVID-19 pandemic has disrupted the daily lives of Canadians, with worsening mental health as people adapt to different stressors. “While many are struggling with this new normal, the degree of disruption resulting from the pandemic presents unique challenges for those with spinal cord injury and brain injury,” says Dr. Eldon Loh, Lawson Associate Scientist also leading one of the funded studies.
Relatively simple tasks such as frequent hand washing can be challenging for those with disability, and they may be more vulnerable to poor outcomes because of the decreased respiratory function many already face. The research team will document and evaluate the effect of the pandemic on the physical and mental health of those with spinal cord and brain injuries. “We plan to use our findings to provide guidance to those living with spinal cord and brain injury, and improve their quality of life during this challenging time. We expect that this study will not only help those with spinal cord and brain injuries, but also people living with other disabilities as well,” notes Dr. Loh. He is also a Physical Medicine and Rehabilitation Specialist at St. Joseph’s.
The IRF competition is supported with funding from clinical departments at LHSC and St. Joseph’s, and from London Health Sciences Foundation and St. Joseph’s Health Care Foundation.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Supporting a rapid research response during the pandemic
Hospital-based research is uniquely positioned to tackle the unprecedented COVID-19 challenge and quickly translate results into illness prevention and care for patients. Lawson Health Research Institute, the research institute of London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London, has awarded more than $202,000 to its research teams to support critical discoveries during the pandemic.
Over 14 projects ranging from improved diagnostics to understanding the impact of the COVID-19 pandemic on frontline health-care workers have been funded through Lawson’s Internal Research Fund (IRF) COVID-19 Pandemic Response Competition.
“Lawson researchers are an intrinsic part of health care in London. Our research community has mobilized quickly to the COVID-19 pandemic and has come forth with innovative ideas to prevent infections, aid recovery and reduce the likelihood of mortality in those most seriously affected,” says Dr. David Hill, Scientific Director for Lawson. “Lawson has reallocated internal granting resources to enable some of the most exciting and credible ideas to be explored.”
Launched in March, this rapid response competition was focused on funding projects, such as two described below, that could impact the management of the pandemic and enhance our understanding of the novel coronavirus.
Using genetic therapy to block entry of the virus
Progression of COVID-19 depends on human proteins that the virus uses to escort itself into lung cells to cause disease. “There are three such ‘virus entry’ proteins that are particularly important for infection. We see them as potential targets for drugs to prevent and treat COVID-19,” explains Dr. James Koropatnick, Lawson Scientist and Principal Investigator for one of the funded studies.
There could be dangers in targeting these proteins, particularly for patients taking certain blood pressure-reducing drugs. The team is studying the safe use of a new type of drug – powerful “antisense” agents that block messenger RNAs which are the biological “blueprints” for the target virus entry proteins – to stop the virus from using those proteins to infect lung cells. They are testing two types of antisense molecules that reduce the amount of the virus entry proteins. “With our existing knowledge and infrastructure in place, this testing could rapidly lead to new, non-vaccine agents to prevent and treat COVID-19, as well as future coronaviruses with pandemic potential,” adds Dr. Koropatnick.
The impact of the pandemic response for those with disabilities
The COVID-19 pandemic has disrupted the daily lives of Canadians, with worsening mental health as people adapt to different stressors. “While many are struggling with this new normal, the degree of disruption resulting from the pandemic presents unique challenges for those with spinal cord injury and brain injury,” says Dr. Eldon Loh, Lawson Associate Scientist also leading one of the funded studies.
Relatively simple tasks such as frequent hand washing can be challenging for those with disability, and they may be more vulnerable to poor outcomes because of the decreased respiratory function many already face. The research team will document and evaluate the effect of the pandemic on the physical and mental health of those with spinal cord and brain injuries. “We plan to use our findings to provide guidance to those living with spinal cord and brain injury, and improve their quality of life during this challenging time. We expect that this study will not only help those with spinal cord and brain injuries, but also people living with other disabilities as well,” notes Dr. Loh. He is also a Physical Medicine and Rehabilitation Specialist at St. Joseph’s.
The IRF competition is supported with funding from clinical departments at LHSC and St. Joseph’s, and from London Health Sciences Foundation and St. Joseph’s Health Care Foundation.
Congratulations to all of the researchers and their teams who have been awarded funding:
- Dr. Ian Ball - Predictors of clinical deterioration in hospitalized patients with COVID-19: The CORAL study
- Dr. Doug Fraser - Translational Research Centre: Repository of biological specimens from patients
- Dr. Sean Gill - Rapid identification of therapeutic targets mediating pulmonary microvascular endothelial cell dysfunction in COVID-19 patients
- Dr. Marnin Heisel - Testing Online Meaning-Centered Men’s Groups to Promote Psychological Well-Being and Reduce Despair in the Face of the COVID-19 Pandemic
- Dr. Kimia Honarmand - The impact of the COVID-19 pandemic on frontline healthcare workers: A Southwest Ontario survey
- Dr. Michael Knauer - Improving diagnostic and epidemiologic detection of SARS-CoV-2
- Dr. Jim Koropatnick - Targeting the SARS-CoV-2 receptor with candidate antisense drugs to prevent infection and disease progression
- Dr. Eldon Loh - COVID-19 and Disability: The Impact of a Societal Lockdown on those with Spinal Cord and Brain Injuries
- Dr. Len Luyt - Stapled Peptides as SARS-CoV-2 Fusion Inhibitors
- Dr. Claudio Martin - COVIDOPATHY – An observational study of coagulation abnormalities in patients with COVID-19
- Dr. Tianqing Peng - Developing new ssDNA aptamers targeting S protein receptor binding domain of SARS-CoV-2 to disrupt virus infection cycle as a potential therapy
- Dr. Eva Turley - Hyaluronan signaling through the inflammasome is a target for blunting acute respiratory distress syndrome (ARDS) in COVID-19 patients
- Dr. Ruud Veldhuizen - Next generation exogenous surfactants for COVID-19 and future respiratory pandemics
- Dr. Blayne Welk - Characterizing the burden of surgical care in COVID-19 positive patients
Team players: FMT and microbiome research could have widespread impact
There is still much to learn about the human microbiome and its role in fighting disease, but ongoing studies at Lawson Health Research Institute, including a focus on fecal microbial transplants (FMT), are making strides in harnessing this complex system.
FMT is being studied in connection with conditions as varied as non-alcoholic fatty liver disease, rheumatoid arthritis, atherosclerosis, HIV, cancer and multiple sclerosis.
FMT is already in clinical use for the treatment of C. diff (Clostridium difficile), and in addition to showing promise in the treatment of other diseases, it is also being studied as a way to improve response to existing cancer treatments and ease treatment side effects.
Dr. Saman Maleki, a Scientist at Lawson Health Research Institute and the London Regional Cancer Program (LRCP) at London Health Sciences Centre (LHSC), says they’ve just begun to explore the possibilities.
"We are just starting to study FMT as an intervention outside its traditional use in patients with C. difficile infection, and we will be expanding to other areas, particularly in cancer.”
FMT can overhaul a patient’s microbiome, Dr. Maleki explains, and a healthy microbiome is beneficial especially when a treatment is trying to activate the body’s immune system.
Dr. Michael Silverman, Lawson Associate Scientist and Medical Director of St. Joseph’s Health Care London’s Infectious Diseases Care Program, is a pioneer in the field of FMT. He has been performing the procedure since 2003 with C. difficile patients and was one of the first in North America to do so. He sees a wide range of possible applications.
“FMT has enormous potential in being an important adjunctive therapy in many cancers. It may, for example, help cancer patients respond to immunotherapy,” says Dr. Silverman, who is also Chair/Chief of Infectious Disease at St. Joseph’s Health Care London, LHSC and Western University. “The potential to impact autoimmune and metabolic diseases is also quite exciting, but still in early development.”
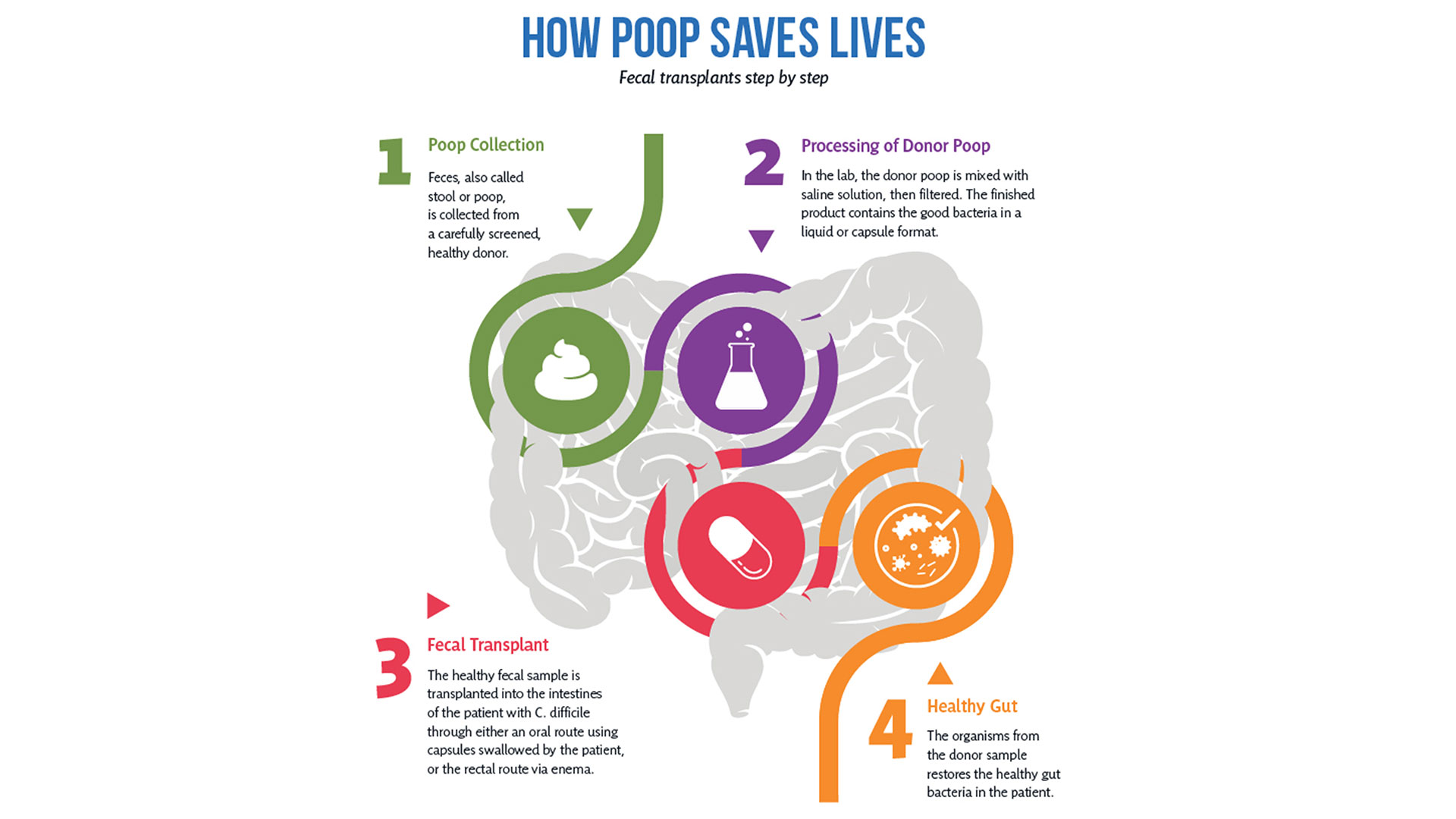
So how does it work?
After rigorous screening, stool from a healthy donor is collected and then processed in a lab into a liquid or capsule containing the good bacteria, which can then be administered to a patient’s gastrointestinal tract.
The Lawson team is also one of few delivering FMT using specially-prepared oral capsules. Introduced in 2018, they have been a game changer in patient acceptance and ease of administration, according to Research Coordinator Dr. SeemaNair Parvathy, who has been coordinating the program since 2015.
“There is a link between the fitness of the intestinal microbiome and the fitness of the immune system,” says Dr. John Lenehan, Associate Scientist at Lawson and Medical Oncologist at LHSC. “A ‘healthy’ microbiome leads to a more robust immune response when using immunotherapy. FMT from a healthy donor is expected to improve the fitness of the recipient’s intestinal microbiome and promote a better immune response.”
People with chronic disease can often experience what’s called a ‘leaky gut,’ allowing food, bacterial and microbial components to pass through the intestinal wall, negatively impacting the immune system.
“When people get FMTs their intestinal permeability improves – meaning it actually reduces,” says Dr. Jeremy Burton, Lawson Scientist and Research Chair of Human Microbiome and Probiotics at Lawson and St. Joseph’s. “What changes that intestinal permeability? The microbes at the site. They play a role in interacting with the host cells, providing nutrients and vitamins.”
With the immune system so closely tied to the health of the microbiome, it’s not surprising scientists are exploring how strengthening one can have a big impact on the other.
Boosting immunotherapy
Immunotherapy can be used to either stimulate or suppress the immune system to help the body fight disease, and FMT is showing promise in reducing resistance to the treatment.
While immunotherapy has been effective in treating a number of cancers – the number one cause of death in Canada – not all patients respond to the treatment.
But early work presented at a conference by the Lawson team for the Journal for ImmunoTherapy of Cancer has shown that using FMT to modify the microbiome could reduce resistance to immunotherapy. The study involved patients from LHSC with advanced melanoma, a type of skin cancer.
While in the very early stages, the combination of FMT and anti-PD1 immunotherapy has been found to be safe, and it appears that FMT could make tumours more responsive to the immunotherapy treatment.
“Microbiome-based treatment strategies, including FMT, have a high potential in oncology,” says Dr. Maleki. “Our team is also exploring its potential in treating pancreatic cancer.”
The research is so interesting that a recent Nature article listed the Phase I melanoma trial as “seminal” research. The study was also unique in that it used healthy donors, as opposed to donors who had previously responded to immunotherapy treatment.
A separate Lawson study with LHSC patients with metastatic renal cell carcinoma, a type of kidney cancer, published in the Journal of Clinical Oncology, also looked at combining immunotherapy and FMT to ease the adverse effects of the treatment.
The Phase I study, led by Dr. Maleki and Dr. Ricardo Fernandes, Medical Oncologist at LHSC, found adding FMT to doublet immunotherapy was safe, but further study is needed to determine whether it could bring about changes in the microbiome and immune system.
Dr. Lenehan says Lawson researchers are in a position to be leaders in this field in the near future for two reasons.
“One is that other academic researchers have not been able to assemble the expertise, and some who have, do not have the access to healthy donor stool. The second is that some biotechnology companies are interested in FMT, but almost exclusively for C. difficile infections.”
Autoimmune, metabolic and other illnesses
Two other areas that have seen recent advances include FMT for the treatment of non-alcoholic fatty liver disease (NAFLD) and multiple sclerosis.
“The gut microbiome is very important in the metabolism of foods and metabolic products. It can therefore have a major effect on obesity and atherosclerosis,” says Dr. Silverman. “It also is tightly involved in regulating the immune system and therefore moderating the microbiome may potentially impact autoimmune diseases.”
A study published in 2020 by the team in The American Journal of Gastroenterology showed that FMT appears to reduce intestinal permeability in patients with NAFLD.
The number of people with NAFLD is growing rapidly and studies show patients have different microbiota than healthy persons.
The trial included 21 NAFLD patients from LHSC and St. Joseph’s. While the researchers found no changes in percentage of liver fat or insulin resistance, they observed significant reduction in intestinal permeability in those patients who had elevated intestinal permeability at the study’s start (seven patients in total). They also observed changes to the gut microbiome in all patients who received a fecal transplant from a healthy donor.
“Metabolic syndromes including obesity and its complications of NAFLD and atherosclerosis are massive public health problems. Any impact on these would be of huge importance,” Dr. Silverman adds. “Autoimmune diseases also cause major morbidity and mortality. We have a lot of work to do before we can consider FMT as a routine therapy for any of these conditions, but the long-term promise is great.”
Research into the use of FMT for treatment of patients with multiple sclerosis is in the very early stages. But patients with MS show a difference in gut microbiota and higher small intestine permeability, which could contribute to the development of the disease.
A Phase I trial by the Lawson team published in the Multiple Sclerosis Journal – Experimental, Translational and Clinical, found FMT to be safe and tolerable.
While the study was very small, MS patients treated with FMT were found to have beneficial changes to gut microbiota and intestinal permeability, but further study is needed to determine if FMT could be used as a treatment.
Lawson scientists are also currently studying the use of FMT for patients with atherosclerosis, along with ongoing studies on melanoma and lung cancer. Funding for a study on pancreatic cancer has been secured and researchers are in the process of planning trials for a number of other applications.
Dr. Lenehan says, “The microbiome is connected to several diseases and their treatments. Evidence is growing that an individual’s health is related to their microbiome.”

The donor challenge
The challenge of finding fecal donors for FMT and the cost of that process remain an issue for research into this promising treatment, even as more potential applications are discovered.
There is currently no process in place to match donors and recipients – as with organ donation – but there is an extensive screening process for both infectious and non-infectious conditions, one that needs to be repeated if a donor experiences any lifestyle changes.
Dr. Burton says, “We still don't understand the full role of the microbiota. We have to ensure that we're not giving patients a microbiota that might cause them some other issue in the future, so the donors are screened very thoroughly for that.”
Screening also excludes donors with an increased risk of developing the diseases scientists are hoping to treat, such as metabolic syndrome related conditions.
A 2017 article published in Open Forum Infectious Diseases by Drs. Silverman and Burton found the cost of screening high numbers of potential donors could make establishing local programs extremely difficult, so having a central program such as the one in London could help patients in many regions.
In the study, only five of 46 potential donors passed the history, examination, blood, stool and urine tests, and of the five, four later travelled or had illnesses that made donation inadvisable.
The search continues in London for potential donors to help drive this research forward. You can read one donor’s story and learn how you can get involved here.
More on FMT and the microbiome:
Drugs vs. bugs: Harnessing the microbiome to improve treatments
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Third-party review of animal research at Lawson Research Institute, St. Joseph’s Health Care London
In August 2025, members of our community raised concerns about our animal research program at Lawson Research Institute (Lawson). While we were confident we followed all regulations and ethical standards, we commissioned an independent third-party review of animal research at Lawson and indicated we would make the results of that review public.
What the third-party review found:
- Lawson met all regulatory, ethical and professional standards in animal research.
- There was no evidence of intentional secrecy, concealment or avoidance of oversight. The research is reported in peer-reviewed publications, grant disclosures and academic presentations - all available to the public.
- No other animal or non-animal model could have been used to achieve the translational outcomes the researchers were trying to achieve.
What areas of improvement did they identify?
Recommendations include improved communication between St. Joseph’s, Lawson, Western University and Western’s Animal Care Committee, with clear accountabilities for decision making, to ensure all parties are aware of their unique roles and responsibilities, to update shared agreements and policies, including transparency plans and enhance the process for reporting of concerns.
What other reviews were completed?
- Western Animal Care Committee Report
- Canadian Council on Animal Care Special Assessment Report
- Ontario Ministry of Agriculture, Food and Agribusiness inspection Report
The majority of the key findings of these reports align with those of the third-party panel.
What’s next?
We are developing an action plan to address all recommendations and are working with our partners on next steps.
Animal research remains an important part of medical discovery. The life-saving imaging approaches developed at Lawson are now standard of care worldwide for people suffering from heart disease and heart attacks. We are immensely proud of the work our researchers conduct every day to save and improve lives.
Thank you,
Roy Butler, PhD
President and CEO
Jeremy Burton, PhD
Interim Vice-President
Research and Scientific Director Lawson Research Institute
This will be a huge benefit for society because sepsis is the leading cause of death worldwide
It’s a discovery that has been more than ten years in the making: the use of a human protein to potentially treat patients with sepsis.
Lawson Scientist Dr. Qingping Feng noticed that a human protein called annexin A5 showed positive results with sepsis back in 2007.

Fast forward 14 years later to now, and this discovery could very well be the first ever viable treatment for sepsis patients, including severe COVID-19 patients who develop sepsis. “With COVID initially, it is in the airway and then in the lungs, then from there the inflammatory response in fact spreads to the whole body,” says Dr. Feng, Ivey Chair in Molecular Technology at Western University's Schulich School of Medicine & Dentistry. “Sepsis causes major organ dysfunction and carries a high mortality unfortunately.”
It has become a challenging issue for Intensive Care Physician at London Health Sciences Centre (LHSC), Dr. Claudio Martin, who can only do so much to treat severe COVID-19 patients that develop sepsis.
“What we have seen is a very primary severe respiratory failure to the lungs for severe COVID patients,” says Dr. Martin, Associate Scientist at Lawson. “We have used steroids and other treatments to try to help, but the results and effects aren’t dramatic and we see patients who have these treatments and still progress and end up in the ICU.”
However, Dr. Feng and his team has found in a pre-clinical study, that annexin A5 can inhibit inflammation, improve organ function, and survival when treating sepsis.
Another potentially deadly situation for COVID-19 patients is cell death and blood clots, specifically near the lungs. The good news is that the research team also believes the annexin A5 drug will prevent these complications through the drugs anti-apoptotic (cell death prevention) and anti-coagulant (blood clot prevention) properties.

Supported by provincial funding through Ontario's COVID-19 Rapid Research Fund, the research team has launched a clinical trial with critically ill COVID-19 patients at LHSC, using a manufactured form of annexin A5. The goal is to enroll a total of 60 patients for the clinical trial, and enrollment has already begun. “Patients are receiving standard treatment and then those enrolled will also receive the annexin,” says Dr. Martin. “It’s a placebo blinded clinical trial, so patients will either get a lower dose of annexin, a higher dose of annexin, or a placebo.”
If the clinical trial shows promising results, Dr. Feng says the team plans on expanding into a larger phase three trial with not just COVID-19 patients with sepsis, but other sepsis patients as well. “If in fact annexin A5 is shown to be effective in sepsis, then this will be a huge benefit for society because sepsis is the leading cause of death worldwide.”
The drug is currently being produced through a partnership with Suzhou Yabao Pharmaceutical R&D Co., Ltd., based in China, Lawson Health Research Institute, and WorldDiscoveries. “Our long-standing partnership with Suzhou Yabao has enabled annexin A5 drug development to proceed to this point,” says Kirk Brown, Manager of Business Development, Lawson Health Research Institute. “We are now in a unique position through this trial to offer a potential life-saving treatment for this emergent global disease, with the objective of soon expanding to all cause septic patients.”