Search
Search
‘The scariest part is the uncertainty’ – New therapeutic tool proven effective for MS patients with mental health challenges
It was a diagnosis that came as a shock for 28-year-old Mitch Kuska who found out he had Multiple Sclerosis (MS) at the age of 26. “I went from being a young 26-year-old doing regular things, to having to learn about this disease and everything that goes along with it and how it will affect my life." Kuska, an avid cyclist, says knowing that one day he may not be able to physically do the things he loves has been the hardest part of his MS journey so far. “The scariest part for sure is the uncertainty, because I don’t know what the future holds for me. Before I could look into the future and feel for the most part that I would be healthy.”

“It can be a stressful time for people as they have just been diagnosed with a chronic neurological disease that will last the rest of their life,” says Dr. Sarah Morrow, Neurologist and Associate Scientist at Lawson.

As part of the study, 24 newly diagnosed RMS patients were recruited including Kuska. Participants were split up into two groups, either the treatment group or the control group. The treatment group took part in ten sessions of the Mindfulness Without Borders program.

The participants were evaluated before the sessions and then six months later to see if there was a difference between the two groups. “Immediately after the sessions when we compared the two groups, those in the mindfulness were reporting better coping skills and less perceived stress, and their symptoms of depression had been reduced,” adds Dr. Morrow.
“During the study treatment, I definitely noticed myself being more mindful of my symptoms. Sensing little changes in my body and little feelings here and there,” explains Kuska. “I was more in tune with myself and I felt this mindfulness tool helped me get into the right mindset to start dealing with MS.”
Following these initial findings published in Multiple Sclerosis and Related Disorders, the London research team plans to examine them in a larger study. They are also working to examine if the use of mindfulness would be helpful for people who are in the more progressive stages of MS.
2017 SRF Spotlight: Drs. Muriel Brackstone & Gregor Reid
Announced at the 2017 Lawson Impact Awards, Drs. Muriel Brackstone and Gregor Reid were recipients of Lawson’s annual Strategic Research Fund (SRF) competition. Their project, “Re-setting the breast microbiome to lower inflammation and risk of cancer,” will examine whether taking an oral probiotic can reduce inflammation and lower the risk of breast cancer.
One in nine Canadian women will develop breast cancer during her lifetime (Canadian Breast Cancer Foundation). Many cancers are considered to be the result of inflammatory processes. While inflammation has been a focus of research in breast cancer, the role of bacteria has not.
Recently, Drs. Reid and Brackstone were collaborators on a study that was the first to describe the breast microbiome, proving the existence of bacteria in human breast tissue. Led by Dr. Reid and his former PhD student, Dr. Camilla Urbaniak, further research demonstrated that the types of bacteria found in women with breast cancer differ significantly from those found in healthy tissue.
One bacterial species from the cancerous tissue, Escherichia coli (E. coli), is capable of producing low amounts of substances known to cause cancer and induce inflammation, while the bacteria found in healthy tissue, like Lactobacillus, are known to interfere with cancer processes.
“The question is whether we can manipulate this to essentially get rid of more harmful bacteria and replace them with beneficial ones like Lactobacillus,” says Dr. Reid, a Lawson scientist and Director of the Canadian Centre for Human Microbiome and Probiotic Research.
In this new study, Dr. Brackstone and Dr. Reid will join forces to test their theory that taking an oral probiotic lactobacilli will lead to these organisms reaching the breast tissue, displacing harmful bacteria and reducing inflammation.
Drs. Brackstone and Reid will compare bacteria from the breast tissues of women at risk for breast cancer who are taking the probiotic against those at risk who are taking a placebo. They will also compare to the breast tissue of healthy women who are not at risk. The research participants will provide nipple and needle aspirates for their bacteria to be analyzed both at the beginning of the study and after three months of either taking the probiotic or a placebo. The samples will also be tested for inflammatory compounds, levels of heavy metals and pesticides that may influence cancer risk.
“I think this study will shed light into what actually occurs in the milk ducts where most breast cancers originate,” says Dr. Brackstone, a Lawson scientist, surgical oncologist and medical director for the London Breast Care Clinic. “If successful, this project could lead to larger studies and contribute to a new way of approaching breast cancer management.”
Now in its third year, Lawson’s Strategic Research Fund (SRF) supports research projects that will advance science in alignment with Lawson’s strategic research goals, as outlined in Lawson’s 2014-2018 Strategic Plan. This year’s competition once again focused on “inflammation”. Chosen projects received $50,000 over a two-year period.
Learn more about this research project:
2017 SRF Spotlight: Drs. Stewart Gaede and Gerald Wisenberg
Announced at the 2017 Lawson Impact Awards, Drs. Stewart Gaede and Gerald Wisenberg were recipients of Lawson’s annual Strategic Research Fund (SRF) competition. With their project, “Assessing acute cardiac inflammation after left-sided breast cancer radiotherapy with hybrid PET/MRI,” the Lawson researchers will explore the cardiovascular effects of radiation therapy for left-sided breast cancer.
Radiation therapy is critical to modern breast cancer treatment. It has led to improved survival rates with many patients living long lives following their treatment.
Unfortunately, when delivering radiation therapy, we cannot avoid irradiation around surrounding tissues, including the heart. This is a concern since such irradiation may lead to cardiovascular disease later in life.
Currently, the effects of radiation to the heart can only be detected one or two years afterwards. With the help of their Lawson SRF award, Drs. Gaede and Dr. Wisenberg will use PET/MR imaging to detect earlier effects of radiation and construct new guidelines and treatment strategies for left-sided breast cancer patients.
“We’re seeing more and more breast cancer survivors, but many women with left-sided breast cancer are now developing heart disease later in life,” says Dr. Gerald Wisenberg, Director of Cardiac Imaging Research at Lawson and cardiologist at London Health Sciences Centre (LHSC). “We hope to improve their outcomes through this research.”
Recently, Drs. Gaede and Wisenberg discovered that an increase in cardiac inflammation can be detected as early as one week after radiation using PET/MR imaging. This inflammation may be the cause of cardiovascular disease seen in women 10 to 15 years after treatment.
In the new pilot study, the researchers will follow 15 left-sided breast cancer patients undergoing radiation therapy. They will be imaged one week before as well as one week and one year after radiation therapy with Lawson’s hybrid PET/MRI scanner at St. Joseph’s Hospital in London, Ontario.
Areas of inflammation, changes in blood flow, scar formation and fibrosis will be measured by looking at the differences between images. The data will help in the design of new treatment strategies that can hopefully decrease or eliminate inadvertent heart damage. By doing so, it could help to improve patients’ quality of life.
“The earlier we can detect the effects of radiation for left-sided breast cancer, the earlier we can intervene,” says Dr. Gaede, a Lawson imaging scientist and medical physicist at LHSC’s London Regional Cancer Program. “We hope to learn more about the ways in which radiation is affecting the heart so that we can construct new radiation techniques to better spare the heart.”
Learn more about this research:
Now in its third year, Lawson’s Strategic Research Fund (SRF) supports research projects that will advance science in alignment with Lawson’s strategic research goals, as outlined in Lawson’s 2014-2018 Strategic Plan. This year’s competition once again focused on “inflammation”. Chosen projects received $50,000 over a two-year period.
2018 Scientist of the Year Award: Dr. Robert Teasell
Lawson scientist Dr. Robert Teasell is considered a global leader in neurorehabilitation research and has been instrumental in transforming clinical care in this area across Canada by ensuring that clinical practices are informed by the best available and up-to-date research evidence. In recognition of his accomplishments, he received the Scientist of the Year Award at the 2018 Lawson Impact Awards event this past spring.
Dr. Teasell leads the Collaboration of Rehabilitation Research Evidence (CORRE) research team at St. Joseph’s Health Care London’s Parkwood Institute. He is also the Medical Director of the Stroke Rehabilitation Unit at Parkwood Institute and has an active outpatient chronic pain practice.
He has led the development of three internationally renowned evidence-based reviews for stroke rehabilitation, brain injury and spinal cord injury, which are regarded as the three most comprehensive research syntheses in neurorehabilitation in the world. Dr. Teasell has advised and helped plan stroke care for all of Ontario’s 14 Local Health Integration Networks (LHINs) and six provincial healthcare systems. This is in addition to the many clinical guidelines and models of care he has helped develop and update.
Dr. Teasell also bridges the gap between research and clinical practice through collaborations between his research and clinical teams. His multidisciplinary Rehabilitation Knowledge to Action Project (REKAP) team received the 2014 Sandra Letton Quality Award for their quality improvement project designed to make Parkwood Institute a leader in stroke rehabilitation by improving care through implementation of best practices.
In addition to his neurorehabilitation research, Dr. Teasell has published extensively on chronic pain with a recent focus on the role of obsessive personality traits in determining chronic pain disability and coping abilities.
Drawing on his clinical and research expertise, Dr. Teasell has supervised many students and has been committed to developing the next generation of medical researchers.
“Dr. Teasell has been successful in a number of areas. Certainly in terms of publications and mentorship of students who have gone on and had very successful careers of their own. Despite a busy clinical schedule, he always makes a point of engaging with his research team every day. His staff and students really appreciate the opportunity to work with him,” says Dr. Cheryl Forchuk, Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, and Assistant Director, Lawson Health Research Institute.
Dr. Teasell has authored 335 peer-reviewed articles, as well as many other collaborative group peer-reviewed articles, book chapters, published abstracts, posters, presentations and monographs. He has also been the editor for 14 special journal editions and is on the editorial boards for Topics in Stroke Rehabilitation, Journal of Rehabilitation, and Pain Research and Management.
In 2016, he was invited to present the Ramon J. Hnatyshyn Lecture, the leading annual national stroke lecture at the Canadian Stroke Congress in Quebec City. In 2010, he received the Canadian Association of Physical Medicine and Rehabilitation Merit award for his many contributions to the field of physiatry. He was also awarded the Royal College of Physicians and Surgeons of Canada McLaughlin-Gallie Visiting Professor in 2012. This year he will be awarded the Post-Acute Stroke Award of Excellence from the American Congress of Rehabilitation Medicine and the National Stroke Association in the United States.
“I’ve received a lot of national and international awards but there’s nothing better than being recognized by your peers and particularly your peers in the city where you work. It’s been a nice acknowledgement of not just my work, but also the work by the whole research team and all the people who have supported me over the years,” says Dr. Teasell.
2018 Staff Award of Excellence: Sheila Fleming
Sheila Fleming, executive assistant to Dr. David Hill, scientific director of Lawson Health Research Institute, was the recipient of a Staff Award of Excellence at the 2018 Lawson Impact Awards event this past spring.
In addition to carrying out her administrative support functions for Dr. Hill – in itself a significant responsibility – Fleming goes above and beyond to provide support in a variety of ways to the entire Lawson administration team and research community.
Just one of the many examples of this is the key role she plays in the planning of Lawson’s annual signature events: London Health Research Day (LHRD), Lawson Impact Awards and Café Scientifiques.
Fleming has built strong relationships across Lawson and its hospital and academic partners. She often acts as a liaison connecting administrative team members to key senior leaders and researchers, and vice versa, so they are able to do their jobs more effectively.
“Sheila is the ‘hub’ of Lawson. Almost all of us on the administration team, and I’m sure many members of our research community, view Sheila as their go-to person. She has a wealth of knowledge that has guided many of us,” says Stacey Larizza, Chief Operating Officer, Lawson. “She always considers the needs of scientists, staff and trainees, and she is a passionate advocate for them. She does whatever she can to help ensure they succeed.”
Her relationship-building skills have also strengthened Dr. Hill’s advocacy efforts as Lawson continues to join research institutes across the country campaigning for increased funding, diversity in science and support for young researchers from the Canadian government.
“As a scientist it’s not just doing the research, it’s leading people; it’s really knowing how to run a business. So anyway I can help them jump those hurdles, I’m happy to do that,” says Fleming. “In my view, relationships drive everything and that’s how we get work done. If you’re fair and helpful and collaborative, people will respond in kind and then it’s easy to move things forward.”
Fleming also participates in a number of volunteer initiatives. For example, she is President of the Ingersoll District Nature Club, a group that stewards the 36 acre Lawson Nature Reserve south of Ingersoll; helps lead local advocacy efforts in opposing a proposed mega landfill adjacent to Ingersoll aquifers; and provides administrative support to the Diabetic Pregnancy Study Group, a European not-for-profit organization that fosters research and education in diabetic pregnancy.
2019 Innovation Award: Dr. Don Richardson
Dr. Don Richardson was recognized at the 2019 Lawson Impact Awards for his research and innovation in working with veterans with military-related post-traumatic stress disorder (PTSD). His study titled, “Predicators of Long-Term Treatment Outcome in Combat and Peacekeeping Veterans with Military-Related PTSD,” was recently published in the Journal of Clinical Psychiatry.
Throughout Dr. Richardson’s career, he has worked diligently to develop and implement best practice assessment and treatment guidelines for Canadian Armed Forces (CAF) members and veterans. He has developed and maintained two clinical research databases ̶ a database of self-reported health status, by working with patients at the Operational Stress Injuries (OSI) clinic, and a treatment outcomes database. Through this data, he has demonstrated that military trauma populations are complex and are at greater risk of becoming resistant to treatment than most civilian trauma populations.
“Don is extremely deserving of this award,” says Dr. Cheryl Forchuk, Dr. Richardson’s nominator. “When I think of someone who does a great job of linking together research and clinical practice, Don is always someone who comes to mind.”
The treatment outcomes database gives researchers unparalleled insight into the pharmacologic interventions best suited for CAF members and veterans. With the ability to identify when individual patients are experiencing less-than-optimal outcomes, the research team can adjust their treatment plan accordingly.
Over the past 20 years, Dr. Richardson has published over 40 peer-reviewed manuscripts and book chapters on the assessment and treatment of operational stress injuries, PTSD, major depressive disorder, substance use disorders, and suicidal behaviour. He has elevated awareness for the unique mental health challenges faced by CAF members and veterans who present with operational stress injuries.
In light of Dr. Richardson’s findings, he works to assess the current treatment modalities for PTSD, their utility for treating military populations, as well as complementary therapies that may prove beneficial.
Dr. Richardson’s dedication to military mental health research is evident through his unwavering effort and has attracted the attention of many prominent figures in the field of military and veteran health. In 2017, he was granted the opportunity to build a research and innovation center for advancing military and veteran health research and clinical practice. Through a generous donation from two community peers, Dr. Richardson established and leads the Macdonald/Franklin OSI Research Centre, located at Parkwood Institute.
“It is certainly an honour to receive this award,” says Dr. Richardson. “I wish to thank all of my clients for taking the time to fill out the repeated questionnaires, as well as the research staff who support this program, and who work tirelessly to help our CAF members and veterans.”
CIHR funding for COVID-19 enables researchers to investigate virus transmission during surgery and pandemic planning
Researchers at Western University and Lawson Health Research Institute continue to make important contributions to help mitigate the spread of COVID-19 and its negative consequences. Two projects in London will address virus transmission during surgery and pandemic planning for COVID-19, thanks to new funding announced by the Government of Canada, through the Canadian Institutes of Health Research (CIHR), along with provincial partners.
Researchers in London received more than $400,000 in funding through this latest round.
“Accelerating high-quality research and real-time evidence is a priority for Canada in its fight against COVID-19. I congratulate the successful teams for their essential work aimed at better preventing, detecting and treating COVID-19 at the individual and population levels,” said Patty Hajdu, Minister of Health in a press release. “Our government believes that it’s through collaboration and data sharing that we will respond efficiently to this global health emergency.”
Virus transmission in surgical smoke
In an effort to perform surgery during the pandemic as effectively and safely as possible, Dr. Leigh Sowerby, Associate Professor at Schulich Medicine & Dentistry and Associate Scientist at Lawson, will be investigating whether or not the virus that causes COVID-19 can be transmitted in surgical smoke. Surgical smoke is the aerosol produced by an essential surgical tool called electrocautery.
“Electrocautery is a ubiquitous tool for surgery, and is known to generate aerosol and smoke. We do not know if the SARS-CoV-2 virus can be transmitted in this plume, and this is important to answer for all surgeons, but in particular, for surgeons working in the respiratory and aerodigestive tract,” said Dr. Sowerby, who is also a head and neck surgeon at London Health Sciences Centre and St. Joseph’s Health Care London. “CIHR funding will allow us to rapidly execute this project. Without this funding, the project would not be possible.”
Dr. Sowerby says the results from this study, whether positive or negative, will have important implications. If positive, it will have a critical and direct impact on ensuring the safety of health care workers performing procedures on patients. Procedures using cautery will continue to require high level protection if the COVID-19 status of the patient is unknown. If negative, it will allow these surgical procedures to continue safely and effectively while conserving critical protective equipment for cases that need it.
The family physician’s role in pandemic plans
Maria Mathews, PhD, Associate Professor at Schulich Medicine & Dentistry, is investigating how the role of family physicians can be better incorporated into pandemic plans. Family physicians play important roles during a pandemic, from detecting potential outbreaks and screening and testing patients to providing care to infected patients and contributing to surge capacity in hospitals.
“During the early stages of the COVID-19 pandemic, family physicians had concerns about roles they were asked to fill for a variety of reasons, including the lack of appropriate personal protective equipment, availability of tests, and concerns about infection risks to other patients and staff in a family practice clinic,” said Mathews.
Mathews will examine the experiences in four regions in Canada – Newfoundland and Labrador, Nova Scotia, Ontario and British Columbia – to identify key roles, supports and best practices. The results will provide government ministries, public health units, and other health organizations with evidence and tools in order to incorporate family physicians in the response to a potential second COVID-19 wave and plan for future pandemics.
Could microorganisms in poop help treat the deadliest form of skin cancer?
A multidisciplinary team at Lawson Health Research Institute is exploring whether fecal transplants can improve outcomes in melanoma patients treated with immunotherapy.
Immunotherapy drugs stimulate a person’s immune system to attack and destroy cancer. While they can significantly improve survival outcomes in those with melanoma, they are only effective in 40 to 50 per cent of patients. Preliminary research has suggested that the human microbiome – the diverse collection of microbes in our body – may play a role in whether or not a patient responds.
“The gut microbiome helps establish immunity from an early age. It makes sense that a healthy gut could improve response to immunotherapy,” explains Dr. Jeremy Burton, a Lawson Scientist who specializes in human microbiome research. “This led us to consider the potential of fecal transplants.”
Fecal transplants involve collecting stool from a healthy donor, preparing it in a lab and transplanting it to the patient. The goal is to transplant the donor’s microbiome so that healthy bacteria will colonize in the patient’s gut.

Above (from left): Drs. Michael Silverman and Jeremy Burton
In a phase I clinical trial, the research team is the first in Canada to study the use of fecal transplants to alter a cancer patient’s microbiome and improve their response to anti-PD1 immunotherapy drugs.
Research participants will be 20 melanoma patients recruited from the London Regional Cancer Program (LRCP) at London Health Sciences Centre (LHSC). They will undergo a fecal transplant at St. Joseph’s Hospital, a part of St. Joseph’s Health Care London, followed by immunotherapy at LRCP. The transplant will consist of taking a number of specially-prepared oral capsules.
Patients will be assessed over time for any changes to their cancer, microbiome, immune system and overall health. The primary goal of the study is to evaluate safety of the novel treatment combination, but researchers will also evaluate patient outcomes.
“Melanoma is the least common skin cancer but it is the most deadly and rates are going up,” says Dr. John Lenehan, Associate Scientist at Lawson and Oncologist at LHSC. “Anti-PD1 immunotherapy drugs can be extremely effective but we want to help more patients respond. That’s our goal.”

Above (from left): Drs. Saman Maleki and John Lenehan
While the team is studying the combination of fecal transplants and immunotherapy for melanoma, they see potential for other cancers as well.
“We’re one of the first in the world to study fecal transplants in cancer patients. This study is as cutting-edge as it gets with potential applications for multiple disease sites,” notes Dr. Saman Maleki, a Lawson Associate Scientist who specializes in cancer immunology. “With experts in microbiology, infectious disease, cancer and immunology, our institute is well-positioned to carry this forward.”

Dr. Michael Silverman, Lawson Associate Scientist and Chief of Infectious Disease at St. Joseph’s and LHSC, is a pioneer in the field of fecal transplants. St. Joseph’s is a leading centre for the procedure, performing them for Clostridium difficile (C. diff) patients across the province.
“Fecal transplants have saved the lives of countless patients with recurrent C. diff,” says Dr. Silverman. “We’re now starting to see its potential for the treatment of other diseases.”
Lawson researchers are planning fecal transplant studies for multiple other conditions including non-alcoholic fatty liver disease, multiple sclerosis (MS) and cancer treatment toxicity.“But in order to conduct this research, we need stool donors,” notes Dr. Silverman.
Check out media coverage of this research:
- CTV News: Why fecal transplants could be the next frontier in fighting skin cancer
- Forbes: Could poop be the next treatment for cancer?
- London Free Press: Researchers seeking poop donors for skin cancer treatment study
- Daily Mirror: How human poo 'transplants' could help doctors treat deadliest form of skin cancer
- CBC: London cancer researchers make number 2 their number 1 priority
Database funding could improve diagnosis and treatment of prostate cancer
A $125,000 grant from the Canadian Cancer Society will help create a database of PET/CT (positron emission tomography/computed tomography) and PET/MR (magnetic resonance) images of prostate cancer. The hope is that this database will be used to help improve diagnosis and treatment of men with prostate cancer.
The scans use radiopharmaceuticals to target prostate specific membrane antigen (PSMA), a transmembrane protein commonly found on prostate cancer cells.
“The idea behind this grant is to put together a database of PSMA PET/CT and PET/MR scans with annotated findings so medical professionals can scroll through cases and see the sites of prostate cancer. Our hope is this will help clinicians learn how to interpret these scans and ultimately help them to make informed treatment decisions for their patients,” says Dr. Katherine Zukotynski, Adjunct Scientist at Lawson Health Research Institute and lead researcher on the project.
The use of PSMA PET/CT and PET/MR scans in clinical practice is relatively new and currently only accessible through clinical trials. In fact, the first PSMA PET/MR scan in Canada was performed at St. Joseph’s Health Care London in 2016 by Dr. Glenn Bauman, Lawson Scientist and Radiation Oncologist at the London Regional Cancer Program at London Health Sciences Centre. Dr. Bauman is also part of this database project.
Studies have found these scans more accurately detect sites of prostate cancer than earlier imaging techniques, which then helps inform treatment decisions.
Dr. Zukotynski explains, “If you have an idea of the amount of disease and where it is located, and you can correlate it with prognosis, this could be very helpful. It might also allow physicians to compare current patients with patients who have similar findings, which may help determine the best therapies to try.”
There is hope that eventually this same database could lead to the use of artificial intelligence (AI) to assist in diagnosis and treatment planning.
“PSMA PET/CT and PET/MR may be tools helpful to categorize the total burden of disease, and then establish how that disease changes with therapy. Our first step down this path is to assemble a database that can be used both for research and educational purposes.”
The database will include data from centres across Canada, with a number of researchers contributing to the project funded by the Canadian Cancer Society.
Other principal investigators include: Dr. Bauman; Dr. François Bénard of the BC Cancer Research Institute; Dr. Vincent Gaudet, University of Waterloo; Dr. Phil Kuo, University of Arizona; Dr. Cynthia Ménard, Centre Hospitalier Universitaire de Montreal; and Dr. Ur Metser of the Princess Margaret Hospital. Dr. Carlos Uribe of the BC Cancer Research Centre and Dr. Aaron Ward of Lawson are co-applicants for the grant.
This is the part three of a three-part series on PSMA PET imaging research. Check out part one and two.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Easing the pressure for patients with chronic wounds
Chronic wounds represent a significant burden in Canada. Between four and 30 per cent of patients develop a chronic wound, depending on the health care setting. Over 85 per cent of all Spinal Cord Injury (SCI) survivors will experience health complications related to pressure ulcers, injuries to the skin and underlying tissue resulting from prolonged pressure. These types of wounds can significantly reduce participation in meaningful activities and overall quality of life.
Research from around the world shows that electrical stimulation can help speed the healing of pressure ulcers. This therapy is currently done by a trained health care provider and is not readily available for people across Canada.Electrical stimulation therapy (E-Stim) is a wound treatment that involves applying low levels of electrical current to the wound bed and surrounding tissues. It stimulates several healing processes, promotes local circulation and prevents infections.
The E-Stim Collaboration: A Best Practice Implementation Project for Better Pressure Ulcer Care aims to improve the coordination of pressure ulcer care and promote the use of evidence-informed wound treatments for people living with SCI. In particular, the research project is studying how to best provide E-Stim to people with pressure ulcers, in their own communities.
“Over the years I’ve seen the serious impact pressure ulcers have on the lives of people with spinal cord injury and other health challenges. This is what drives my commitment to not only develop best practice guidelines, but also to ensure they are put into action,” says Dr. Pamela Houghton, Associate Scientist, Lawson and Professor, School of Physical Therapy at Western University. “Advances in technology make it possible for more people with care needs to live at home.”
The pilot project in the South West LHIN has a unique model that builds capacity in the community and taps into the lived experience of people with pressure ulcers and SCI. It brings together the expertise of researchers, clinicians and managers from academia, hospital centres and community care.
Partners include the Parkwood Institute Research program at Lawson Health Research Institute, Western University, Saint Elizabeth’s Health Care Research Centre, Sunnybrook Health Sciences Centre and the South West Community Care Access Centre. An interdisciplinary specialized team, called SCIPUT, has been established within the Spinal Cord Injury Rehabilitation program provided at Parkwood Institute, St. Joseph’s Health Care London.
“Our collaborative team is using the PLAN-DO-STUDY-ACT quality improvement model. This allows us to learn from each cycle and make adjustments as we go,” says Dr. Houghton. “We have just completed the first cycle and are reporting on lessons learned.” Funded by the Rick Hansen Foundation, the team hopes this will set the stage for a larger cross-country initiative.
Those interested in participating can contact phoughto@uwo.ca. The study is open to:
- Individuals with an open pressure ulcer and with a condition that causes limited mobility and/or requires a wheelchair;
- Those who are able and willing to participate in treatment plan, and communicate feedback; and,
- People who are eligible to receive services from South West CCAC.
|
Image
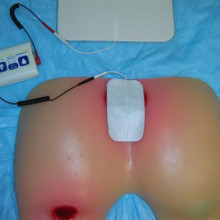
Electrical stimulation (E-Stim) directly stimulates several wound healing processes, promotes local circulation and prevents wound infections. It produces faster healing and wound closure. A trained health care provider applies low levels of electrical current to the pressure ulcer using specialized equipment. |
Expanded No Fixed Address strategy houses half of those in danger of homelessness
At a community symposium on health care and homelessness attended by over 250 Londoners, a research team from Lawson Health Research Institute announced the results of a nine-month, federally funded project tackling the issue of homelessness from within hospital walls.
The No Fixed Address (NFA) strategy reaches and supports patients during the crucial transitional period when they are being discharged from the hospital and re-integrated into the community. The approach was initially tested with strong success for mental health patients across the city and the second ‘version’ of the project was extended to medical units at London Health Sciences Centre’s University Hospital and Victoria Hospital.

“Many of our patients with lived experience of homelessness were saying that their journey started with a hospital discharge,” explains Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson and NFA project lead. “They were often experiencing major transitions in their lives and then experienced a hospital stay. Normally a relatively short visit, they aren’t able to gather the information and make a plan to be able to leave the hospital with somewhere to stay.”
Through partnerships between service providers and non-profit organizations, the NFA strategy helps prevent homelessness by providing timely and accessible supports to patients who would otherwise be discharged into homelessness. Staff from the Canadian Mental Health Association Middlesex, Salvation Army’s Housing Stability Bank, and Ontario Works in the City of London provided direct, on-site patient access to housing and income support databases
“Lawson’s No Fixed Address research project is the first evaluation anywhere of a strategy that aims to reduce the number of hospital patients being discharged into homelessness,” says Dr. Forchuk.
Over nine months, 74 people experiencing medical health issues accessed the NFA program. Of those, 54 per cent were also experiencing mental health challenges.
All of the study participants were in imminent danger of homelessness. Through the supports provided as part of this research study, half were able to arrange housing before being discharged.
“We were able to help a lot of people, with 50 per cent successfully securing housing,” shares Dr. Forchuk. “With the results and feedback we received, we learned a lot about how we can make the program even better.”
They found that there is a need for the supports to be extended as a transitional program in the community post-discharge, as the length of stay in the medical units tended to be short.
The project’s previous phase, involving acute and tertiary psychiatric care in the London region, prevented homelessness in 95 per cent of cases. “Going into the medical units, we found that people have highly complex needs that often involved mental health challenges.
By simply using the same approach that we did for those in psychiatric care, we helped half of the people find housing. To best serve the needs of everyone, we want to follow them after discharge.”
The team sees a solution in having a housing support worker provide transitional, wrap-around services that follow the person. They would continue to meet and work together after the hospital stay, helping to access community programs.
“This role would be embedded in both the health care system and the homeless serving system, supporting individuals who have complex physical and mental health issues as they are also navigating homeless resources.”
This project is funded by the Government of Canada's Homelessness Partnering Strategy’s (HPS) Innovative Solutions to Homelessness funding stream.
Overview and Numbers
Fast facts on homelessness and health care
- Stable housing after discharge is associated with higher quality of life, reduced substance abuse and fewer hospital admissions.
- Homeless clients are four times more likely to be readmitted to hospital within a month compared to low-income matched controls.
- Hospital care for homeless clients costs an average of $2,559 more per client.
- Finding appropriate housing or avoiding a potential eviction takes time – it is important to start as soon as possible during the discharge process.
Implementation of first phases of No Fixed Address
- Access on the unit to a housing advocate and income support staff.
- The initial intervention was accessed by 219 acute psychiatric clients, as well as 32 clients within a specialized tertiary care psychiatric hospital - only 3 became or remained homeless.
- Expanded to be an immediate wrap-around service with offices set up in the hospital mental health units.
- Staff from the Canadian Mental Health Association Middlesex (CMHA), Ontario Works (OW), and Salvation Army’s Housing Stability Bank (HSB) have on-site access to housing and income support databases.
- Clients can access service by drop-in or appointment.
- Services include assistance for finding housing, financial assistance, such as rent/utilities in arrears or first/last months’ rent for a new home, and access to high quality used furnishings, household supplies and a cleaning service.
Expanded second phase of No Fixed Address
- Program ran from July 2018 to March 2019 (9 months).
- 74 people accessed the program.
- Complex situations with both mental health and physical problems: 100% had medical issues and 54% had mental health issues.
- Lengths of stay were very short.
- People could not attend drop-in due to medical issues, so they relied on referral from staff.
- Although they were all in imminent danger of homelessness, 38 people (50%) were housed as a result of this program.

What were the main housing needs?
- Help finding a place to live
- Money for deposit
- Financial support
- Transportation support
- Help getting benefits
Recommendations and learnings for future models
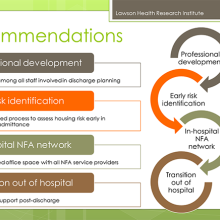
- Housing support worker needs to be a transitional support since work will be needed after discharge.
- Social work not the only key players (patient care facilitators, nursing staff, etc.).
- The transitional housing support role needs to be well embedded in the homeless serving system, as well as health care.
- People have physical and mental health issues and are also going to be navigating homeless resources.
- Despite the low success rate, many people were housed who would have otherwise been discharged to homelessness.
- We learned a lot about what was needed in an area where there was a knowledge vacuum.
- Future plans involve implementation with improvements to the model.
Expanding transitional support for young adults with diabetes
In 2012, researchers from across Ontario, led by a team at Lawson Health Research Institute, started the first multicenter randomized controlled trial to evaluate implementation of a transition coordinator for young adults with type 1 diabetes as they transferred from paediatric to adult care.
“There is a huge difference between the kind of care that they receive as children compared to adults, and that is consistent across Canada and most other countries,” explains Dr. Cheril Clarson, associate scientist at Children’s Health Research Institute, a program of Lawson, and a paediatric endocrinologist at Children’s Hospital, London Health Sciences Centre.
With children, patient visits involve a variety of specialists from different areas, such as the physician, nurse educator, dietitian and social worker. “The naturally build up a long-term relationship with the team, as some children might start the program when they are 2 or 3 years old as an example.” Dr. Clarson adds that the child’s caregivers are an integral part of the process and the care team also gets to know them very well.
Moving into the adult program means that the patient now has more responsibility and autonomy over their own care. They have to remember to go to appointments, fill prescriptions and maintain their daily diabetes care.
“During the emerging adulthood period, your attention is taken up by many other things – leaving home, starting post-secondary education, figuring out your identity and independence,” says Dr. Tamara Spaic, Lawson associate scientist and adult endocrinologist at St. Joseph’s Health Care London. “And on top of that they need to manage their diabetes every day. They are in a completely new system with a new care team – it’s a major transition. For many, they stop coming to appointments regularly and they don’t keep up with all of their own care.”
As young adults struggle to find their footing in a new system, there are significant short and long-term consequences when it comes to their health. Some will experience acute complications like high sugars leading to diabetic ketoacidosis and hospital admission or severe low blood sugars where they can lose consciousness and have a seizure.
“Different studies show between 30 to 60 per cent increased risk of complications like retinopathy, myocardial infraction, stroke and kidney disease in those who do not follow their care plan,” notes Dr. Spaic. “We see a bump in this young adult period where levels spike and their diabetes isn’t being controlled – this has impacts for both the individual and the system.”
The study enrolled 205 young adults with type 1 diabetes between the ages of 17 and 20. Patients were recruited from three paediatric centres and their care was transitioned to three adult centres. The multi-centre partnership included Children’s Hospital; St. Joseph’s; Children’s Hospital of Eastern Ontario; The Ottawa Hospital; and, Trillium Health Partners in Mississauga.
Participants were randomly assigned to two groups, with 104 patients in the structured transition program and 101 patients receiving standard care. Patients were seen in the paediatric care setting for six months and then transferred to adult care, where they continued with either the transition program or standard care for one year.
The core component of the program was a transition coordinator, a nurse who is a certified diabetes educator. The coordinator followed the young adults throughout the transition, interacting with the paediatric health care team to establish a base of support as they moved into adult care. They attended visits, established appropriate contacts for the patient, provided support for diabetic care, problem solved and helped navigate the system. In addition to face-to-face meetings, they were available via text messages, emails and phones calls.
“We had a high recruitment rate for the population and type of study, and a high number of participants followed the full program,” says Dr. Clarson. “Our results at the end of the intervention showed that the program worked very well. By providing additional support through a transitional coordinator, the results showed better outcomes all around.”
Compared to the baseline, study participants attended more care visits, were more satisfied with their care, suffered much less distress associated with diabetes, had better management on a daily basis and reported less emotional burden of diabetes.
The team then took it a step further and spent another year following the participants to see if they were able to sustain the behaviour and positive outcomes. They did not find a difference between the control and intervention groups.
“Unfortunately, we found no difference in the number of visits they attended, their satisfaction with care and management of their diabetes,” explains Dr. Spaic. “When they didn’t have the intervention, they essentially went back to baseline. Out hope is to see the program extended.”
Dr. Clarson adds that they developed the program so that it can be integrated in different ways, and also in difference areas of health care beyond diabetes. For example, they found that the preferred method of communication with the coordinator was text. This is an easy way to provide the fundamental support of a coordinator for longer, and it is cost-effective.
“Our patients really loved the intervention. By the end of the study, they felt more comfortable being able to navigate the adult health care system. They felt empowered and responded well. They wanted to continue the program.” The next step for the researchers is to evaluate support through a virtual transition coordinator.
“Closing the Gap: Results of the Multicenter Canadian Randomized Controlled Trial of Structured Transition in Young Adults With Type 1 Diabetes” was recently published in the journal Diabetes Care by the American Diabetes Association.
Learn more about the study and read about Nicole Pelcz, study participant, who found out at 13 years old that she had type 1 diabetes.
In the media:
Diabetic teens fall back to old habits after transition care, study says – London Free Press
Fifth annual Lawson Impact Awards honours research excellence
Over 300 guests attended the fifth annual Lawson Impact Awards on Wednesday, April 18 at the London Convention Centre to honour research making a difference and to recognize the accomplishments of our scientists, staff, trainees and partners.
“There are many individuals, groups and partners at Lawson who regularly go above and beyond to drive innovative new discoveries. For the past five years, the Lawson Impact Awards have given us the opportunity to step back and reflect on the importance of the work we do here and how these contributions ultimately improve patient care,” says Dr. David Hill, Scientific Director, Lawson Health Research Institute.
This year’s Lawson Impact Award winners include:
- Dr. Robert Teasell – Scientist of the Year Award
- Dr. Mandar Jog – Innovation Award
- Dr. Manuel Montero-Odasso – Dr. Joseph Gilbert Research Contribution of the Year Award
- London X-Ray Associates – Industry Partner of the Year Awards
- CAISA Fashion Show; London Run for Ovarian Cancer; and Kyle MacDonald and John Franklin – Community Partner of the Year Award
- Sarah Best – Staff Award of Excellence
- Sheila Fleming – Staff Award of Excellence
- Amanda McIntyre – Leadership Award for Fellows & Students
The recipients of Lawson’s 2018 Strategic Research Fund (SRF) were also revealed at the Lawson Impact Awards. The Lawson SRF is an annual competition that supports projects that will advance science in alignment with Lawson’s strategic research goals, as outlined in the Lawson Strategic Plan 2014-2018. This year’s competition was open to all areas of research. The following two projects were awarded $50,000 over a two-year period:
- “Mindfulness group intervention for newly diagnosed persons with Multiple Sclerosis: A pilot study” – Drs. Sarah A. Morrow and Arlene MacDougall
- “Extending routinely collected data research at Western: Does enhanced medical reconciliation improve care at London hospitals?” – Drs. Blayne Welk and Amit Garg
In addition to the Lawson Impact Award and SRF recipients, two Children’s Health Research Institute (CHRI) award recipients were recognized at the event. CHRI is a program of Lawson and awards a Scientist and Trainee of the Year annually. These awards are sponsored by the Children’s Health Foundation. CHRI’s 2017 award recipients were honoured at the Lawson Impact Awards: Dr. Lina Dagnino (CHRI Scientist of the Year) and Dr. Amer Youssef (CHRI Deb Comuzzi Trainee of the Year).
A highlight of the event was a keynote presentation from physician-scientist and 3D innovator, Dr. Julielynn Wong, titled “How Technology is Enhancing Our Future.” Dr. Wong delivered an engaging talk on how technology trends such as 3D printing and drones can improve health care accessibility. Her presentation included a 3D printing demonstration and guests were given the opportunity to examine samples of 3D printed medical supplies.
To view videos of each award winner, visit the Lawson YouTube page. To see more photos from the event, visit Lawson’s Facebook page.
Funding for unique strategy to prevent homelessness after hospital discharge
In Canada, about 235,000 people experience homelessness each year. The number of homeless people, and the length of time they spend homeless, continues to rise. Homelessness is not a choice and anyone can become homeless.
Although the root cause is poverty, some underlying issues are poor physical or mental health; violence or abuse in the home; lack of employment or income; and, a shortage of affordable housing.
A group of researchers at Lawson Health Research Institute (Lawson), working at both London Health Sciences (LHSC) and St. Joseph’s Health Care London (St. Joseph’s), are committed to tackling the issue of homelessness from within hospital walls, where some patients face the risk of being discharged into homelessness.
“Many of our patients with lived experience of homelessness were saying that their journey started with a hospital discharge,” says Lawson clinician researcher Dr. Cheryl Forchuk. “Often, they were experiencing major transitions in their lives and then experienced a hospital stay. Normally a relatively short visit, they aren’t able to gather the information and make a plan to be able to leave the hospital with somewhere to stay.”
On September 10, Adam Vaughan, Canadian MP and Parliamentary Secretary (Housing and Urban Affairs), on behalf of the Honourable Jean-Yves Duclos, Minister of Families, Children and Social Development, announced that Lawson will receive $223,572 from the Homelessness Partnering Strategy’s (HPS) Innovative Solutions to Homelessness funding stream to support the project “No Fixed Address Version 2 Expansion” research project.

“This is a brilliant approach. It supports an augmented duty of care where hospitals have the means to transfer people into stable settings where they can continue to heal and move towards self-sufficiency,” says Parliamentary Secretary Vaughan.
Taking place at London Health Sciences Centre, this research will further refine the No Fixed Address strategy for reaching and supporting patients during the crucial transitional period when they are being discharged from the hospital and re-integrated into the community.
“Lawson’s expanded No Fixed Address research project is the first evaluation anywhere of a strategy to reduce the number of patients being discharged into homelessness. There is almost no literature on any aspect of this troublesome issue,” explains Dr. Forchuk who is the study’s Principal Investigator. Dr. Forchuk is also the Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery and Assistant Director at Lawson.

This project is an extension of three previous studies conducted by Dr. Forchuk’s research team, which developed and tested this novel approach. They demonstrated the efficacy, feasibility and cost-effectiveness of using the No Fixed Address strategy in acute and tertiary psychiatric care in the London region, at both LHSC and St. Joseph’s. In the first phase, they found that the interventions used prevented homelessness in 95 per cent of cases.
The researchers are now taking a solution proven to have worked in the mental health units and applying it in selected medical departments at LHSC. Through the study, the services will be available to all patients in those units who are at risk of homelessness. There have already been 17 patients who have accessed this support since the project got underway this summer.
Three community partners from London are supporting implementation of the strategy - Canadian Mental Health Association Middlesex, Ontario Works in the City of London and the Salvation Army’s Housing Stability Bank. They will provide assistance in areas like securing appropriate private-sector housing, provision of income and employment supports, and financial assistance.
“In many ways London, Ontario is the high water mark of solving and tackling homelessness. This community has a lot of be proud of given the way that the municipality is stepping up to the plate and how many different organizations are working together towards a common goal,” says Parliamentary Secretary Vaughan.
This kind of collaboration showcases the important partnership between the Canadian Government, research-intensive hospitals and community organizations to translate innovative solutions from the research stage to the front line of care.
“The hope is that the findings will be even more robust, leading to the development of a best-practice model of hospital discharge that can be adopted throughout Canada. This will reinforce the need for a systemic change in the way hospital discharges occur and ensuring the person is transitioning to a secure housing arrangement,” says Dr. Forchuk.
Learn more about the Government of Canada’s Homelessness Partnering Strategy.
News Coverage
- CBC London - Helping medical patients in London avoid homelessness when they leave hospital
- CTV London - Expanded research hopes to break the cycle of homelessness that psychiatric patients sometimes face when discharged
- Global News, AM 980 - Program that finds housing for homeless patients in hospital gets $223K in federal funding
- London Free Press - 'Brilliant approach' to homelessness gets federal grant
Gut microbiome may influence how cancer patients respond to oral therapies, study suggests
A new study from Lawson Health Research Institute and Western University illustrates how the gut microbiome interacts with an oral medication in prostate cancer patients, suggesting bacteria in the gut play a role in treatment outcomes. The findings, published in Nature Communications, highlight how the drug abiraterone acetate is metabolized by bacteria in the gut to reduce harmful organisms while promoting those that fight cancer. The team suspects this is one of many examples of how the microbiome influences our response to medications.
“Research is beginning to uncover the ways in which the human microbiome influences cancer development, progression and treatment,” explains Brendan Daisley, a PhD candidate at Western’s Schulich School of Medicine & Dentistry who is conducting research at Lawson. “Our study highlights a key interaction between a cancer drug and the gut microbiome that results in beneficial organisms with anti-cancer properties.”
Traditional prostate cancer therapies are designed to deprive the body of hormones called androgens, which are responsible for prostate cancer growth.
“Unfortunately, traditional androgen deprivation therapies are not always effective,” explains Dr. Joseph Chin, Lawson Associate Scientist, Professor at Schulich Medicine & Dentistry and Urologist at London Health Sciences Centre (LHSC). "In those cases, alternative therapies are explored.”
Abiraterone acetate is a highly effective therapy used in the treatment of prostate cancer that has been resistant to other treatments. While abiraterone acetate also works to reduce androgens in the body, it does so through a different mechanism and, unlike traditional therapies, it is taken orally.
“When drugs are taken orally, they make their way through the intestinal tract where they come into contact with billions of microorganisms,” says Dr. Jeremy Burton, Lawson Scientist, Associate Professor at Schulich Medicine & Dentistry and lead researcher on the study. “While it’s long been a mystery why abiraterone acetate is so effective, our team wondered if the gut microbiome plays a role.”
Dr. Jeremy Burton (left) and Brendan Daisley (right)
The team’s study included 68 prostate cancer patients from LHSC, including those being treated with abiraterone acetate and those being treated with traditional androgen deprivation therapies. The research team collected and analyzed patient stool samples, and conducted further experiments in their laboratory at St. Joseph’s Health Care London.
They discovered that patients’ gut microbiomes changed drastically after taking abiraterone acetate. Bacteria in the gut metabolized the drug leading to a significant increase in a bacterium called Akkermansia muciniphila. Referred to as a ‘next-generation probiotic,’ this bacterium’s relevance has recently been explored in several large cancer studies. It’s been shown to facilitate a better response to cancer immunotherapy drugs and it can elicit a wide range of other positive health benefits as well. The increase in Akkermansia muciniphila also led to an increased production of vitamin K2 which is known for anti-cancer properties that can inhibit tumour growth.
The team also observed the impact of androgen depletion on the microbiome. Both abiraterone acetate and traditional androgen deprivation therapies led to a decrease in organisms that utilize androgen.
“These findings clearly demonstrate that the gut microbiome is playing a role in treatment response,” notes Dr. Burton.
The team hopes to further explore drug-microbiome interactions with a goal of harnessing the microbiome to improve treatment outcomes for a variety of diseases. In another study, they are exploring whether fecal microbiota transplants from a healthy donor can change the microbiome of melanoma patients to increase organisms like Akkermansia muciniphila and improve response to immunotherapy. They also plan to study whether analysis of a patient’s microbiome can be used to predict their response to specific therapies.
“While more research is needed, we may one day be able to analyze a patient’s microbiome to determine the best course of treatment or even influence the microbiome to improve outcomes,” says Dr. Burton. “This could lead to a new frontier in personalized medicine.”
The study was made possible through the generous support of The W. Garfield Weston Foundation, St. Joseph’s Health Care Foundation and the Canadian Urologic Oncology Group.
Health research in London receives millions in funding from federal government
Lawson Health Research Institute was awarded over $1.2 million in the Canadian Institutes of Health Research’s Fall 2019 Project Grant competition, for three projects including one Priority Announcement.
“This is a great accomplishment for the successful researchers at Lawson and those working across the city,” says Dr. David Hill, Lawson Scientific Director. “At Lawson, our scientists target rapid response research that can be quickly incorporated into improved care for patients and families. Our research happens within hospital walls, where care is delivered, with innovations that improve lives every day.”
Western University received more than $11.9 million in research funding through the project grant competition for 17 projects. A special congratulation to Lawson researchers Drs. Samuel Asfaha, Thomas Appleton, Neil Duggal, David Spence and Zhu-Xu Zhang, as well as Dr. Subrata Chakrabarti, recipient of the CIHR Priority Announcement for “Novel mechanisms in diabetic cardiomyopathy.”
Selective Brain Hypothermia via Intranasal Cooling to Limit Brain Injury Post Cardiac Arrest
Dr. Ting-Yim Lee
There are 40,000 cardiac arrests per year in Canada. Within the body, it triggers a complex cascade of dysfunction resulting in cell death, even after successful cardiopulmonary resuscitation, with only three to seven per cent of survivors returning to normal function.
To reduce the high incidence of brain damage and the burden on families, the American Heart Association has recommended hypothermia for neuroprotection in post cardiac arrest care.
However, current clinical hyperthermia cools the whole body instead of just the brain. Simple, effective and non-invasive methods to selectively cool the brain that can be readily used in and out of hospitals are not available.

“The grant is allowing us to collect validative data on the protective effect of brain cooling in limiting brain injury from cardiac arrest,” explains Dr. Lee. “The device is very convenient to use. It is compact and can be set up right by the bedside of patients in intensive care units.”
Dr. Lee sees the device as having the potential to be used widely to limit brain injury following stroke, head trauma and sepsis.
“This kind of investment in hospital-based research allows us to identify important clinical problems and find ways to solve them, working closely with research patients along the way.”
Multi-centre diagnostic performance of dynamic CT perfusion for functional assessment of multi-vessel coronary artery disease with dense coronary calcification
Dr. Aaron So
Coronary artery disease (CAD) occurs when plaque forms in one or more coronary arteries of the heart. It is one of the leading causes of mortality and morbidity in the world.
Patients with CAD can go to a cardiac catheterization laboratory where the narrowed coronary artery can be reopened using a catheter-based technique. However, this approach is invasive for the patient and costly for the system. Studies have shown that for various reasons not all patients benefit from this treatment.

With the funding, they are testing the technique at several hospitals and national cardiovascular centres in Canada, China, Germany and Japan. With larger clinical studies in the future, they could determine the optimal diagnostic strategy for patient triage and reduce unnecessary procedures.
“Health research has been and will continue to be very important, with the commitment of patients and clinicians playing a crucial role in the success of medical research and advancement,” says Dr. So. “It’s important for the Canadian government to continue to support research in academic hospitals.”
He adds that the success of the CIHR grant application shows that Canadian researchers can be leaders in health research that benefits people around the world.
Filling Knowledge Gaps for the Success of Ontario Renal Plan 3
Dr. Matthew Weir
The Ontario Renal Network (ORN) is the agency responsible for distribution of funding for kidney care in Ontario. They have released three policy statements outlining strategic objectives for kidney care, with the most recent being the recently released Ontario Renal Plan 3 (ORP3).
“Within the strategic objective, gaps in our understanding of kidney disease have been identified as barriers to successful implementation,” explains Dr. Weir. “We have proposed a suite of 32 related retrospective cohort analyses designed using integrated knowledge translation to address those gaps.”
The Priority funding will help get the first projects underway and build momentum. “The ORP3 had extensive consultation with patients, families and other stakeholders. By supporting its successful implementation, our findings will have a direct and immediate effect on patients in areas that are a priority to them.”

ICES launches call for applications to its next faculty training cycle
The ICES Faculty Scholars Program has officially launched the call for applications to its fourth training cycle (2019-2021).
This two-year, part-time learning opportunity is open to Ontario-based academic researchers who are passionate about population health and health services research, and wish to obtain an appointment as an ICES Scientist,
The program was established at ICES Western in 2013 as part of its strong focus on supporting trainees and new investigators. By leveraging partnerships with other ICES sites and in conjunction with an interactive e-learning environment, faculty from different regions are able to fully participate in the ICES Faculty Scholars program.
Scholars will have access to:
- Training in the use of Ontario’s health administrative databases for research.
- Seminars on advanced methods relevant to population health research.
- Opportunities for collaboration with experts across the ICES network.
- Individual project mentorship and data analytic support to develop and complete one or more research studies using Ontario’s health administrative databases.
Hear from successful ICES Faculty Scholars:
“The methods of planning and completing an ICES project are unique. This program is the best possible way to demystify the process and produce high quality work from the outset. The amount of support is outstanding, so you have confidence that your work will be successful.”
Dr. Andrew Appleton, Assistant Professor, General Internal Medicine, Western University
“The Faculty Scholars Program is extremely well structured and run. The Program provides a positive and open learning environment for Scholars to ask questions and learn about the administrative and practical aspects pertaining to conducting research at ICES.”
Dr. James Crispo, Researcher, Health Sciences North Research Institute
Applications for the 2019–2021 program will be accepted until January 18, 2019. Any questions regarding the program, applications or eligibility can be directed to @email.
Go to the ICES website for more information on the ICES Faculty Scholars Program.
ICES is a not-for-profit research institute encompassing a community of research, data and clinical experts. With its growing network across the province, ICES researchers are able to access a vast and secure array of health-related data to evaluate health care delivery and outcomes. Learn more about ICES Western.
Imaging “hidden” regions of the heart
After suffering a heart attack, some patients develop a microvascular obstruction, an area of the injured heart with extremely poor blood flow. These patients are at an increased risk of developing heart failure in the future.
Medical imaging technologies such as magnetic resonance imaging (MRI) and positron emission tomography (PET) can be used to study the remodeling process after a heart attack that can lead to a microvascular obstruction. However, poor blood flow makes it difficult to get contrast agents into the obstruction. Contrast agents are used in medical imaging to show contrast between different types of tissue, such as damaged and healthy tissue.
Benjamin Wilk, a PhD candidate at Lawson Health Research Institute and Western University’s Schulich School of Medicine & Dentistry, will investigate whether a hybrid PET/MRI system and a new method of administering contrast agents can allow researchers to image microvascular obstructions and study these “hidden” regions in the heart.
Contrast agents are usually injected as a bolus, meaning the entire injection is administered immediately. In this study, participants will instead receive a constant infusion of an MRI contrast agent and PET tracer, which means the injection will be delivered over the course of an hour. The MRI contrast agent they are using is sensitive to blood flow and scar tissue, and the PET tracer is sensitive to inflammatory cells.
This will allow researchers to study the anatomy, blood flow and inflammatory processes in microvascular obstructions a week after heart attack. Participants will then be imaged again after six weeks to study the long-term effects on heart function.
“Studying the heart after a heart attack using novel contrast agent injection strategies with simultaneous PET/MRI could provide crucial information for treatment planning, helping us reduce the number of people affected by heart failure in the future,” says Wilk. “This project could also lead to further research into finding better ways to administer PET tracers and MRI contrast agents. These methods could be applied to different diseases as well.”
Wilk received a Lawson Internal Research Fund (IRF) Studentship to conduct the study, which will be supervised by Dr. Frank Prato, Assistant Director, Lawson and leader of the Lawson Imaging research program at St. Joseph’s Health Care London.
“Lawson's IRF is valuable for students for many reasons. It not only allows us to conduct further research, it also enriches our experience by giving us opportunities to write grants and attend conferences,” adds Wilk.
The IRF is designed to provide Lawson scientists the opportunity to obtain start-up funds for new projects with the potential to obtain larger funding, be published in a high-impact journal, or provide a clinical benefit to patients. Funding is provided by the clinical departments of London Health Sciences Centre and St. Joseph’s Health Care London, as well as the hospital foundations (London Health Sciences Foundation and St. Joseph’s Health Care Foundation).
Improved imaging for prostate cancer
Prostate cancer is the most commonly diagnosed cancer among Canadian men. However, with improved testing and better treatment options, the number of deaths from the disease has been declining over the last several years.
Scientists at Lawson Health Research Institute are working to continue this trend by testing improved prostate cancer imaging using a new molecule. Known as a Prostate Specific Membrane Antigen (PSMA) probe, the new molecule is used in Positron Emissions Tomography (PET) scans. The probe targets PSMA, a unique molecule on prostate cancer cells, to provide highly specific images for better diagnosis and management of patient disease.
PET probes are used in imaging to correctly diagnose cancer. The probes are injected into a patient where they spread to identify sites of disease. The most common PET probes are suitable for many types of cancer, but are not as sensitive in identifying prostate cancer. PSMA probes provide higher accuracy by targeting PSMA molecules, which are highly over-expressed on prostate cancer cells.
PSMA probes are gaining popularity across the globe. This specific probe is a molecule called 18F-DCFPyL and was developed by Dr. Martin Pomper at the John Hopkins Hospital in Baltimore. Dr. Pomper, also a Scientific Advisor to Lawson’s prostate imaging team, worked in collaboration with Canada’s Centre for Probe Development and Commercialization (CPDC) to bring the probe to our nation.
Lawson’s Canadian Institutes of Health Research (CIHR) Team in Image Guidance for Prostate Cancer gained early access to the PSMA probe due to a history of close collaboration with Dr. Pomper and the CPDC. Marking the first time a PSMA probe has been used in Canada, the team captured PET/MRI and PET/CT images from a 64-year-old prostate cancer patient on March 18, 2016 at St. Joseph’s Hospital.
“This is a tremendous step forward in the management of prostate cancer,” said Dr. Glenn Bauman, a Lawson scientist and Radiation Oncologist at London Health Sciences Centre. “PSMA probes have the potential to provide increased accuracy and detection which leads to better, personalized treatment.”
Lawson plans to study the probe with an additional 20 men over the next two years as part of an ongoing clinical trial funded by the Ontario Institute for Cancer Research (OICR). Lawson scientists are working with researchers across Ontario to develop other clinical trial protocols that will use 18F-DCFPyL to measure responses to drug treatments and to evaluate men with suspected recurrence of prostate cancer after radiotherapy.
“The goal of these studies it to establish the value of PSMA probes, particularly18F-DCFPyL, and provide evidence to support the use of these probes in routine clinical care,” said Dr. Bauman.
Donor funding through London Health Sciences Foundation was one catalyst in this research, providing initial funding to hire Research Associate, Catherine Hildebrand, who set up citywide cancer imaging workshops and helped the team prepare successful grant applications to secure key funding from CIHR and OICR.
Interdisciplinary team explores London’s unique approach to addressing homelessness
In London, Ont. more than 1,700 people are experiencing homelessness.
Recognizing the growing crisis, more than 200 individuals from 70 organizations across the city came together and developed the Health & Homelessness Whole of Community System Response – a strategic roadmap for supporting unhoused people who have the most complex health and social support challenges, and helping them access permanent housing that meets their needs. Now a team of researchers has been tasked with assessing how well the roadmap is working.
To understand if the program is meeting its ambitious goals and explore areas for improvement, the Centre for Research on Health Equity and Social Inclusion (CRHESI), a community-university partnership based at Western’s Faculty of Health Sciences, was asked by the Whole of Community Response leaders to support and coordinate research and evaluation of the program.
CRHESI works with and reports to the System Foundation Table, a team of volunteer community partners from diverse sectors with a mandate to evaluate new activities and embed continuous improvement to ensure sustainability of the program.
“London’s Whole of Community Response is a novel approach to addressing the needs of the most vulnerable individuals experiencing complex housing and health challenges within our community,” said Mick Kunze, chair of the System Foundation Table. “While our approaches and interventions are rooted in evidence-based practices, we also understand that local context matters.”
This research and evaluation work is funded jointly by Western, London Health Sciences Centre and through a generous donation from local businessman Ryan Finch to St. Joseph’s Health Care Foundation. The three groups came together recognizing there is a need to create meaningful and measurable change in our community.
Their support has allowed CRHESI to recruit two research managers, Eleanor Gebrou and Kelly Barnes, who oversee the work of more than 100 researchers and community partners from organizations across the city participating in the evaluation project.
"Community-led initiatives not only reflect the real needs of individuals facing homelessness, but they also empower frontline workers by fostering an environment of collaboration and understanding. Together, we can create solutions that prioritize well-being for all—those we serve and those who serve," said Gebrou.
This work is split into four main research areas:
- Exploring the outcomes and experiences of people who are precariously housed, unhoused or at risk of homelessness, as well as the perspectives of the broader residents of London, Ont. and especially the business community.
- Evaluating the experiences and well-being of those working in jobs that provide care and housing support.
- Answering questions related to systems, structures, processes and costs of care.
- Evaluating the processes that enabled this large and complex “whole of community” response, and how it unfolds from here.
“I really believe in evidence-based decision making and having as much information as we can to go into program and policy design,” said Barnes. “It's so important to understand what parts of our homelessness response are working well and what can be improved. Research and evaluation are some of the best ways to do that.”
The importance of voices and stories
Research teams will collect quantitative data, including statistics on how many people get housed, how this housing affects the number of hospital and police contacts and the cost-benefit of these new activities. They’ll also collect qualitative data, which involves hearing the experiences of those without homes, those accessing care and support and those providing and leading services.
This evaluation framework will be presented to city council, sitting as the Strategic Priorities and Policies Committee, on October 8, 2024.
“It is really important to us that this not just be numbers,” said Barnes. “We know how important people’s voices and stories are. When we take the numbers and combine them with people’s descriptions of their experiences, and the discussion of their journey, that gives us really solid information to bring back to the policy-makers and program developers to show what’s working and what isn’t.”
This research and evaluation work will span the next two years, with results shared annually with city council starting in July 2025. In addition to annual reporting, research project teams will share data as it emerges.
“The research and evaluation efforts led by the backbone team of this movement, including the System Foundations Table and our CHRESI research and evaluation managers, will be instrumental in guiding our present and future work, by illustrating the real impact our interventions are having on the health and well-being of those we’re aiming to support, as well as by responding to the questions and concerns voiced by all members of our community,” said Kunze.
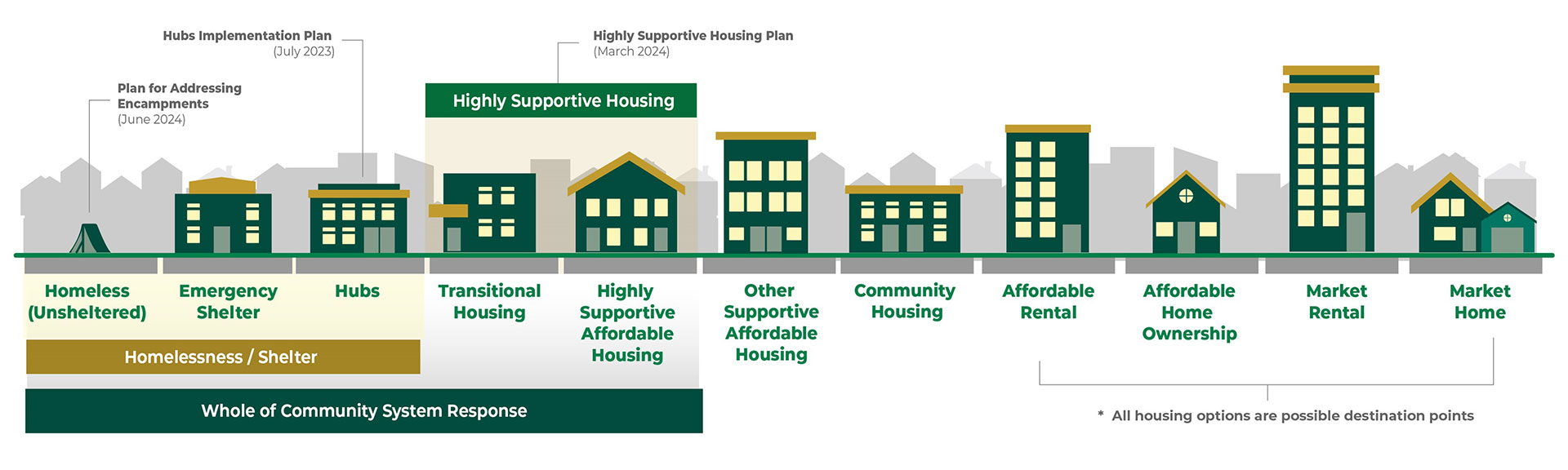
Health & Homelessness Whole of Community System Response
The Whole of Community Response is about developing wrap-around health care and housing supports for those who need them most, ensuring basic human needs are met and building trusting relationships with people so they’re set up to succeed. It includes three main pillars: establishing hubs to meet immediate needs for safe shelter, nutrition and hygiene, and allowing care providers to start the process of stabilizing people’s mental and physical health. Alongside establishing hubs, the broader plan includes bringing more highly supportive housing units to London and implementing a human rights-based approach to support people wherever they are on the housing spectrum.
City council endorsed the Whole of Community Response approach in March 2023. Since then, two hubs have been established, as well as 93 highly supportive housing units, with 50 more units in development, toward a goal of 600 highly supportive housing units within three years.
The Whole of Community Response is being facilitated through the City of London and implemented by lead agencies, with ongoing collaboration among several sectors, including police and emergency services, hospitals, front-line community service organizations, educational institutions and government.
The Health and Homelessness Fund for Change, fuelled by a transformative $25-million donation from a London, Ont. family who wishes to remain anonymous, primarily provides capital funding to help fast-track the creation of hubs and highly supportive housing units. The Fund for Change is administered by London Community Foundation in partnership with the donor family.