Search
Search
Diagnosing COVID-19 using artificial intelligence
LONDON, ON – A team of researchers at Lawson Health Research Institute is investigating whether an artificial neural network could be used to diagnose COVID-19. The AI system is being trained to learn and recognize patterns in ultrasound lung scans of patients with confirmed COVID-19 at London Health Sciences Centre (LHSC) by comparing them to ultrasound scans of patients with other types of lung infections.
“Machines are able to find patterns that humans cannot see or even imagine. Lung ultrasound scans of patients with COVID-19 pneumonia produce a highly abnormal imaging pattern. This pattern isn’t unique to COVID-19, and can be seen in other causes of pneumonia. It is plausible, however, that there are details that distinguish COVID-19 at the pixel level that cannot be perceived by the human eye,” explains Dr. Robert Arntfield, Lawson Researcher and Medical Director of the Critical Care Trauma Centre at LHSC. “If we can train a neural network to learn and identify these unique characteristics among different scans, we can apply this AI to enhance the diagnostic power of portable ultrasound.”
Point-of-care ultrasound has become increasingly important for the care of critically ill patients and LHSC is a global leader in the use of this technology at the bedside. Lung ultrasound has proven to be effective in diagnosing different types of lung infections and illnesses, such as pneumonia, with a high degree of accuracy. The convenience, portability and low cost of using these machines has helped them become a standard bedside tool in emergency departments and intensive care units worldwide.
This research project is part of a grassroots effort by a small group of local clinicians to innovate and create technology to solve sophisticated problems with AI. With many of Dr. Arntfield’s team having a background in computer programming, they were able to code the neural network being tested. Minimal funding was required, with the project being driven largely by the urgency of COVID-19 coinciding with the recent creation of this clinical AI working group.
“Our research team has used AI to help improve diagnostics related to other parts of the body. This project is a great example of the unique ability we have here in London to be agile: that is, to identify a gap and move quickly towards finding a solution,” says Dr. Arntfield. “I am thrilled that we were able to move through the approval process quickly, and get our ideas working in such a short amount of time.”
-30-
Downloadable Media
Dr. Robert Arntfield
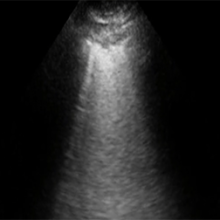
COVID-19 pneumonia ultrasound
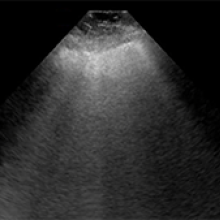
NON COVID-19 pneumonia ultrasound
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Differences in walking patterns could predict type of cognitive decline in older adults
Canadian researchers are the first to study how patterns in the way older adults walk could more accurately diagnose different types of dementia and identify Alzheimer’s disease.
A new study by a Canadian research team, led by London researchers from Lawson Health Research Institute and Western University, evaluated the walking patterns and brain function of 500 participants currently enrolled in clinical trials. Their findings are published in Alzheimer's & Dementia: The Journal of the Alzheimer's Association.

Dr. Montero-Odasso is world renowned for his research on the relationship between mobility and cognitive decline in aging. Leading the Mobility, Exercise and Cognition (MEC) team in London, he is pioneering novel diagnostic approaches and treatments to prevent and combat early dementia. Dr. Montero-Odasso is also co-lead of the Mobility, Exercise and Cognition Team at CCNA, a team composed of 22 researchers and 6 trainees.
This study compared gait impairments across the cognitive spectrum, including people with Subjective Cognitive Impairment, Parkinson’s Disease, Mild Cognitive Impairment, Alzheimer’s disease, Lewy body dementia and Frontotemporal dementia, as well as cognitively healthy controls. The study used data from the COMPASS-ND Cohort and the Gait and Brain Study Cohort.

Gait assessment looks at the way in which we move our whole body from one point to another, helping to analyze mobility and the brain processes involved.
Four independent gait patterns were identified: rhythm, pace, variability and postural control. Only high gait variability was associated with lower cognitive performance and it identified Alzheimer’s disease with 70 per cent accuracy. Gait variability means the stride-to-stride fluctuations in distance and timing that happen when we walk.
“This is the first strong evidence showing that gait variability is an important marker for processes happening in areas of the brain that are linked to both cognitive impairment and motor control,” notes Dr. Frederico Perruccini-Faria, Research Assistant at Lawson and Postdoctoral Associate at Western’s Schulich School of Medicine & Dentistry, who is first author on the paper.
“We’ve shown that high gait variability as a marker of this cognitive-cortical dysfunction can reliably identify Alzheimer’s disease compared to other neurodegenerative disorders.”
When cognitive-cortical dysfunction is happening, the person’s ability to perform multiple tasks at the same time is impacted, such as talking while walking or chopping vegetables while chatting with family.
“Having gait variability as a motor marker for cognitive decline and different types of conditions could allow for gait assessment to be used as a clinical test, for example having patients use wearable technology,” says Dr. Richard Camicioli, Professor at the University of Alberta and co-senior author on the paper.
The London team collaborated with researchers at the University of Toronto, University of Calgary and University of Alberta. They are part of the Canadian Consortium on Neurodegeneration of Aging (CCNA), a collaborative research program tackling the challenge of dementia and other neurodegenerative illnesses.
Dr. Montero-Odasso adds that this gait variability could be perceived as similar to an arrhythmia. Health care providers could potentially measure it in clinical settings, like how heart rhythm is assessed with electrocardiograms.
This study was primarily funded by CCNA, supported by a grant from the Canadian Institutes of Health Research.
Discovery shows promise for treatment of glaucoma
In a new study from Lawson Health Research Institute (Lawson), scientists have discovered that a specific protein has the potential to be used to treat some patients with primary open-angle glaucoma.
Primary open-angle glaucoma is the most common type of glaucoma, which is a group of diseases that affect nearly 70 million people worldwide. Glaucoma is characterized by progressive damage to the optic nerve which ultimately leads to blindness. In this new study, led by Dr. Sunil Parapuram, researchers examined the role of a protein called “phosphatase and tensin homolog” (PTEN) in the trabecular meshwork. The trabecular meshwork is a porous tissue in the eye through which the clear fluid that fills the eye drains out.
In some primary open-angle glaucoma patients, the structure of the trabecular meshwork is damaged by fibrosis. Fibrosis is a thickening or scarring of tissue which is caused by an excess amount of matrix molecules such as collagen. Fibrosis of the trabecular meshwork prevents the fluid in the eye from draining out normally, which leads to increased pressure in the eye and damage to the optic nerve.
Dr. Parapuram’s team found that the inactivation of the protein PTEN can cause too many matrix molecules to be deposited in the trabecular meshwork, leading to fibrosis. On the other hand, when PTEN activity was increased, it reduced the amount of matrix molecules being deposited in the trabecular meshwork. These results indicate that drugs that can activate PTEN have high potential to be used as a treatment for open-angle glaucoma.
“There’s an immediate need for a new generation of therapeutic drugs for more effective treatment of glaucoma,” says Dr. Parapuram, a Lawson scientist at St. Joseph’s Health Care London and an assistant professor in the Departments of Ophthalmology and Pathology at the Schulich School of Medicine & Dentistry, Western University. “While further research is needed, drugs that activate PTEN could be the answer.”
Dr. Parapuram’s team will continue to study the function of PTEN in the trabecular meshwork in more detail and test the role of drugs that activate the protein as a potential treatment for primary open angle glaucoma.

Dr. Michael Motolko (left), Chair/Chief, Department of Ophthalmology, and Dr. Sunil Parapuram (right).
“This study highlights the expansion of our department’s research activities into basic science application and its findings are relevant to many other fibrotic diseases,” says Dr. Michael Motolko, Chair/Chief, Department of Ophthalmology, Schulich School of Medicine & Dentistry,Western University, London Health Sciences Centre and St. Joseph’s Health Care London.
The study, “TGF-β induces phosphorylation of phosphatase and tensin homolog: implications for fibrosis of the trabecular meshwork tissue in glaucoma,” is published in Nature’s Scientific Reports.
Do It for Dads Walk Run
Location: Springbank Gardens Bandshell
Beneficiary: Prostate Cancer Research
Visit: Event website
Take the First Step and Do it for Dads. The Do It For Dads Walk Run is a fun, family friendly event, hosted on Father's Day, that raises awareness and funds for the leading cancer affecting Canadian men and the families that love them.
This run is for all of us, wherever we find our inspiration.
And whether your personal connection is through your father, your brother, your uncle, your son or a friend, we want you to remember one more thing:
Just by taking part, you are an inspiration.
5k, 2.5k, 1k and tot run
Registration Open 8:00 a.m.
Walk/Run Start 10:00 a.m.
DocTalks - Beyond Memory: How Alzheimer’s and Other Dementias Affect Mental Health

Beyond Memory: How Alzheimer’s and Other Dementias Affect Mental Health
Where: Shuttleworth Auditorium (Cheapside entrance)
Dr. Amer Burhan, associate scientist at Lawson and geriatric neuropsychiatrist at St. Joseph's Health Care London, is an expert in the field of neuropsychiatry. He will discuss how Alzheimer’s and other cognitive diseases can impact the feelings and behaviours of individuals as well as their caregivers, and how research is shaping new treatment options for hard-to-treat depression.
Online registration has reached capacity. Please consider joining the next scheduled DocTalk lecture.
DocTalks is a series of community health discussions featuring leading physicians and researchers at St. Joseph’s Health Care London. Learn from the experts how St. Joseph’s is tackling the pressing health issues of our time and why it matters to you and your family.
DocTalks is a joint initiative presented by St. Joseph’s Health Care London and St. Joseph’s Health Care Foundation.
DocTalks - Combating Food Allergies Using the Body’s Immune System

Combating Food Allergies Using the Body’s Immune System
Where: Shuttleworth Auditorium (Cheapside entrance)
Dr. Harold Kim is the Medical Director of St. Joseph’s Allergy and Immunology Program. He will explain how certain food allergies can gradually be reduced or eliminated through the process of immunotherapy.
Registration opens Open 11.
DocTalks is a series of community health discussions featuring leading physicians and researchers at St. Joseph’s Health Care London. Learn from the experts how St. Joseph’s is tackling the pressing health issues of our time and why it matters to you and your family.
DocTalks is a joint initiative presented by St. Joseph’s Health Care London and St. Joseph’s Health Care Foundation.
DocTalks - How Aging Nerves and Muscles Affect Mobility

How Aging Nerves and Muscles Affect Mobility
Where: Shuttleworth Auditorium (Cheapside entrance)
Dr. Tim Doherty is the Chair/Chief of the Department of Physical Medicine and Rehabilitation at St. Joseph’s and Western University and a researcher with Lawson Health Research Institute. He will explain how nerve and muscle function are impacted by aging and share the best ways to maintain healthy muscles and mobility as we grow older.
Registration opens August 15.
DocTalks is a series of community health discussions featuring leading physicians and researchers at St. Joseph’s Health Care London. Learn from the experts how St. Joseph’s is tackling the pressing health issues of our time and why it matters to you and your family.
DocTalks is a joint initiative presented by St. Joseph’s Health Care London and St. Joseph’s Health Care Foundation.
View more information on this DocTalks lecture.
DocTalks - Kidney Stones: From Ancient Times to Modern Practice and Prevention

Kidney Stones: From Ancient Times to Modern Practice and Prevention
Where: Shuttleworth Auditorium (Cheapside entrance)
Dr. John Denstedt is a surgeon at St. Joseph’s Hospital and professor at Western University’s Schulich School of Medicine & Dentistry. He is also the former Chair/Chief of the Department of Surgery and a world renowned leader in the field of urology. Dr. Denstedt will discuss how treatments for kidney stones have evolved over time, including current prevention strategies and how new research is unlocking new possibilities for the future.
Registration opens February 7.
DocTalks is a series of community health discussions featuring leading physicians and researchers at St. Joseph’s Health Care London. Learn from the experts how St. Joseph’s is tackling the pressing health issues of our time and why it matters to you and your family.
DocTalks is a joint initiative presented by St. Joseph’s Health Care London and St. Joseph’s Health Care Foundation.
DocTalks - Managing Persistent Dry Eyes and Why it Matters

Managing Persistent Dry Eyes and Why it Matters
Where: Shuttleworth Auditorium (Cheapside entrance)
Dr. Rookaya Mather is an ophthalmologist at St. Joseph’s Ivey Eye Institute and an associate professor at Western University’s Schulich School of Medicine & Dentistry. She will review the current understanding of Dry Eye Disease and how the condition can be managed effectively.
Registration opens October 16.
DocTalks is a series of community health discussions featuring leading physicians and researchers at St. Joseph’s Health Care London. Learn from the experts how St. Joseph’s is tackling the pressing health issues of our time and why it matters to you and your family.
DocTalks is a joint initiative presented by St. Joseph’s Health Care London and St. Joseph’s Health Care Foundation.
DocTalks - Recovery After Stroke: Retraining the Injured Brain Through Rehabilitation

Recovery After Stroke: Retraining the Injured Brain Through Rehabilitation
Where: Shuttleworth Auditorium (Cheapside entrance)
Dr. Robert Teasell is the Medical Director of St. Joseph’s Stroke Rehabilitation Program, Professor of Physical Medicine and Rehabilitation at Western University and a clinical scientist at Lawson Health Research Institute. He will discuss various rehabilitation therapies and technologies that can help an individual recover after a stroke.
Registration opens April 16.
DocTalks is a series of community health discussions featuring leading physicians and researchers at St. Joseph’s Health Care London. Learn from the experts how St. Joseph’s is tackling the pressing health issues of our time and why it matters to you and your family.
DocTalks is a joint initiative presented by St. Joseph’s Health Care London and St. Joseph’s Health Care Foundation.
Dr. Cheryl Forchuk recognized for health care innovation
Dr. Cheryl Forchuk is the recipient of the 2020 Innovation Award for her work to prevent discharges from hospital to homelessness. Throughout her career, Dr. Forchuk has been investigating potential best practice approaches to prevent homelessness in our community for a wide range of people, including those with severe mental illness, veterans, families, and youth.
Her recent project, ‘Preventing Hospital Discharge into Homelessness: No Fixed Address Version 2 (NFAv2)’ streamlines housing and income services by bringing them into the hospital, and integrating them into a coordinated system of care.
Research shows that when someone is housed, their use of medical and social services decreases. Safe and adequate housing is required for individuals to recover from illness.
Version one of this program was a great success, providing direct access to a housing advocate and Ontario Works from inpatient hospital psychiatric units in London. The No Fixed Address v2 program provides individual inpatients, at risk of becoming homeless, with housing and financial assistance while in hospital. A collaborative approach which includes the local Canadian Mental Health Association, the Salvation Army Rent Stability Bank, Ontario Works, and the City of London brings community supports to the hospital. This enables patients to recover from their illness and reduces the number who may return to the hospital. Dr. Forchuk’s use of in-depth, individual, quantitative interviews, and qualitative focus groups, allows stakeholders to voice their experiences with the program as well as capture traditional outcomes.
“This innovative program has been so successful in London’s hospitals that the City of London has integrated the NFAv2 service within its municipal housing support programs,” explains Dr. Arlene MacDougall, Lawson Scientist and Dr. Forchuk’s nominator. “It also has the potential to be integrated across the province as the best practice in reducing homelessness in communities. Her efforts have been recognized by multiple funding agencies, and it will soon be the model for the rest of the nation to follow. Dr. Forchuk’s commitment to improve the lives and of those in our community makes her truly deserving of this award.”
“The No Fixed Address research project is the first evaluation anywhere of a strategy that aims to reduce the number of hospital patients being discharged into homelessness,” says Dr. Forchuk. “I’m really proud of our collective efforts. We have been able to help a lot of people, and have also learned a lot throughout the course of this study.”
Dr. Clark Heard

Doctorate - Occupational Therapy - Temple University (Philadelphia, PA, USA)
Bachelor of Health Sciences - Occupational Therapy - McMaster University (Hamilton, ON, Canada)
- Focused on occupation, outcomes and the human experience of spirituality
Dr. Clark Heard is a staff occupational therapist at the Southwest Centre for Forensic Mental Health Care in St. Thomas, Ontario, Canada. Clark is also Adjunct Research Professor at the School of Occupational Therapy at Western University. A graduate of McMaster University (Hamilton, ON) and Temple University (Philadelphia, PA), Clark has a high volume of scholarly publication and has clinically precepted more than 125 occupational therapy students. A recipient of multiple teaching awards, Clark was nationally recognized by the Canadian Association of Occupational Therapists in 2015.Clark Has also been recognized with the Sister's of St. Joseph Award for Excellence in Care.
https://www.sjhc.london.on.ca/news-and-media/our-stories/unsung-heroes
