Search
Search
Perceptions of confidentiality for Canadian Veterans discussing moral injuries
LONDON, ON – A new study from Lawson Health Research Institute will be the first to explore Canadian Veterans’ beliefs about confidentiality in mental health care and whether those beliefs act as a barrier to seeking treatment for a type of trauma known as moral injury.
Moral injury describes psychological distress following events where a person performs, witnesses or fails to prevent acts that conflict with deeply held moral standards. Evidence suggests that moral injuries are on the rise among deployed members of the Canadian Armed Forces (CAF), and that those exposed to such events are at a higher risk of developing post-traumatic stress disorder (PTSD) and depression.
Through the study, researchers aim to understand barriers that might prevent military personnel from disclosing details of moral injury.
“A commonly reported barrier when seeking mental health treatment is a perceived lack of confidentiality,” explains Dr. Anthony Nazarov, Post-Doctoral Associate at Lawson. “Since some events that induce moral injuries are ethically ambiguous, it’s possible that military personnel may withhold details of their trauma or even avoid seeking help due to worries about confidentiality.”
The two-year study will engage Canadian Armed Forces Veterans to investigate their perceptions around the confidentiality of disclosing moral injuries in the mental health care and research settings. This will be accomplished not only by interviewing Veterans receiving care at St. Joseph’s Health Care London’s Operational Stress Injury Clinic, but also through online surveys made available to military personnel and Veterans across Canada. The research team will also interview mental health professionals to understand their perspectives on this topic.
“Many Veterans seek help for mental health, and that’s great to see. We’ve come a long way in reducing stigma and barriers, but there’s more work to be done,” says Dr. Don Richardson, Lawson Associate Scientist, Director of the MacDonald/Franklin OSI Research Centre and Physician Lead at St. Joseph’s OSI Clinic. “It’s our duty as mental health researchers and clinicians to ensure that everyone who needs help seeks it. If Veterans do not feel comfortable disclosing certain details because of perceived mistrust related to privacy, we need to know why that is and what we can do to address this issue.“
“Through appropriate messages, it may be possible to dispel any false beliefs, increase trust in mental health professionals and, in turn, increase the number of veterans who choose to seek help,” notes Dr. Nazarov.
The study is being funded by Veterans Affairs Canada and St. Joseph’s Health Care Foundation’s Robert S. & Mary Gay, Donald, James, and Helen (Taylor) Gay Endowed Research Fellowship in Veterans Care.
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Poop in a pill helping advance cancer care
Lawson Research Institute scientists have perfected the delivery of fecal transplants via patient-friendly capsules now central in ground-breaking cancer treatment studies.
It’s one of the most exciting areas of research in cancer care.
Making waves in scientific and health care circles worldwide, it holds the potent potential to “jazz up” cells that attack cancer and boost the body’s response to treatment.
So what is this powerful ally? It’s poop in a pill – home-grown right here at St. Joseph’s Health Care London and Lawson Research Institute.
In fact, Lawson scientists Dr. Michael Silverman, Seema Nair Parvathy, PhD and their team are considered poop pill pioneers, having perfected the delivery of fecal transplantation by way of patient-friendly capsules that can be easily swallowed. These capsules contain healthy gut microbes that have become pivotal in many landmark cancer treatment studies.
Triggering an immune response
Understanding the role of poop in cancer treatment requires grasping the wonders of the human microbiome and its key role in influencing health and well-being.
The human microbiome consists of trillions of microorganisms that live inside and outside of the body, including bacteria, viruses and yeasts. While some bacteria are associated with disease, others are vital to the human immune system – the body’s main protective and disease-fighting tool – and many other aspects of health. Over the past decade, microbiome research has led to a revolution in medicine as scientists unravel just how an imbalance of these microorganisms interferes with many aspects of good health.
"(Fecal microbial transplants) allows us to harness the immune system to mount a stronger defence." Dr. Michael Silverman
The goal of fecal microbiota transplants (FMT) is to transfer healthy gut microbes from donors into patients with cancer and other diseases so that healthy bacteria will colonize in the patient’s gut and improve the microbiome, explains Silverman, Medical Director of St. Joseph’s Infectious Diseases Care Program and citywide Chief of Infectious Diseases for London’s hospitals.
To do so, stools are collected from carefully screened healthy donors, prepared in a lab into capsule format, and introduced into a patient’s gastrointestinal tract.
“What is so exciting when it comes to cancer treatment is the evidence we now have showing how a healthy microbiome activates the immune response to tumours to make the treatment more effective,” Silverman adds. “It allows us to harness the immune system to mount a stronger defense.”
St. Joseph’s capsules are central to several significant studies currently underway aimed at improving treatment for lung, kidney, breast, renal, pancreatic and other cancers.
Among the most notable is the London team’s lead role in a ground-breaking national study – one of the world’s largest randomized controlled clinical trials using FMT to improve the effectiveness of the standard of care for advanced melanoma, a type of skin cancer.
Improving melanoma survival rates
About 11,300 Canadians will be diagnosed with melanoma in 2024 and, even with standard treatment, about half that number will experience disease progression and die.
The 16-site Canadian trial builds off the work of Silverman, Parvathy and their team, in partnership with Saman Maleki, PhD, and Dr. John Lenehan at London Health Sciences Centre. Together, they were the first to demonstrate the safety and therapeutic potential of using the capsules produced at St Joseph’s to influence a patient’s gut microbiota to enhance immunotherapy and increase the odds of surviving advanced melanoma.
“London is seen as having the most expertise in use of FMT in cancer care in the world and is a driving force in moving this forward,” says Silverman. “Immunotherapy is rapidly expanding the number of treatable cancers and our FMT therapy is helping to accelerate this progress.”
Poor sleep linked to multiple chronic conditions
When clinicians are focusing on lifestyle changes for the management and prevention of multiple chronic conditions, they will often ask patients about their alcohol consumption, smoking habits, exercise regime and diet. But what about the quality and duration of their sleep?
Researchers at Lawson Health Research Institute and Western University’s Schulich School of Medicine & Dentistry have shown that how well you sleep and for how long is linked to increased odds of living with multiple chronic conditions, and argue that promotion of good sleep habits should be given greater focus in clinical practice and public health.
The study, “Sleep behaviours and multimorbidity occurrence in middle-aged and older adults,” was recently published in the journal Sleep Medicine. Funded through Lawson’s Internal Research Fund, it used data from more than 30,000 adults over the age of 45 who were part of the Canadian Longitudinal Study on Aging (CLSA).
“Sleep is still a neglected clinical and public health issue, and this study provides additional evidence of the potential role of sleep for the prevention and management of several chronic conditions,” said Dr. Saverio Stranges, principal investigator on the study, Professor and Chair of the Department of Epidemiology and Biostatistics at Schulich Medicine & Dentistry, and Lawson Associate Scientist.
The team looked specifically at the occurrence of multimorbidity, which is defined as having multiple chronic conditions (two or more) that have been diagnosed in a single individual. The conditions can include relatively common chronic disease such as diabetes and hypertension, to depression and cancer, among others.
The study found that there was a consistent relationship between the odds of multimorbidity and self-reported poor sleep quality and altered sleep duration, which includes both too much and too little sleep.
Specifically, male participants who were dissatisfied or very dissatisfied with their sleep had a 20 per cent increase in the odds of multimorbidity. And participants aged 65 to 74 years of age who self-reported dissatisfaction with their sleep quality had a 43 per cent increase in the odds of multimorbidity.
When looking at sleep duration, while the study found a link between multimorbidity and getting too little sleep, the researchers actually found that too much sleep had a much stronger link.
Female participants who self-reported short sleep duration (less than 6 hours a night) had a 16 per cent increase in the odds of multimorbidity and those who self-reported long sleep duration (more than 8 hours a night) had a 44 per cent increase in the odds of multimorbidity. Male participants who self-reported long sleep duration had a 45 per cent increase in the odds of multimorbidity.
Previous international research has shown an association between sleep and a range of chronic conditions, but this is the first Canadian study to look specifically at the relationship between sleep and multimorbidity among middle-aged and older adults.
“This study highlighted an important relationship between self-reported sleep patterns, both duration and satisfaction, and the odds of multimorbidity among older female and male adults in Canada,” said Dr. Kathryn Nicholson, Adjunct Assistant Professor at Schulich Medicine & Dentistry, who was the lead author on the study. “Although it is important to acknowledge that this relationship was cross-sectional and causation cannot be determined from this study, we were fortunate to utilize a comprehensive data source like the CLSA, which allowed us to examine both the self-reported patterns of sleep and the occurrence of multimorbidity.”
The authors point out in the paper that there is already established evidence showing that lack of sleep has negative effects on the cardio-metabolic, endocrine, immune and inflammatory systems, and that over the past several decades the population has been experiencing poorer quality of sleep.
“This is concerning because if poor quality of sleep can increase the risk of a range of chronic conditions, then we should be concerned about sleep hygiene and put that at the centre of our focus both as clinicians and as public health scientists,” said Dr. Stranges.
The researchers will be continuing their research by using the first set of follow-up data from the CLSA to begin to explore longitudinal patterns between multimorbidity and other health indicators.
“High-quality sleep can be very beneficial, but achieving this high-quality sleep can sometimes be a challenge. We hope that this study will continue to emphasize the importance of focusing on sleep as a key health indicator and ideally, this assessment of sleep will include a focus on sleep quality and sleep duration and be a point of conversation during a clinical encounter for all patients living with multimorbidity,” said Nicholson.
Additional study authors are Rebecca Rodrigues, Dr. Kelly K. Anderson, Dr. Piotr Wilk and Dr. Giuseppe Guaiana.
Precise, high-dose radiation safe and effective for inoperable kidney cancer, study suggests
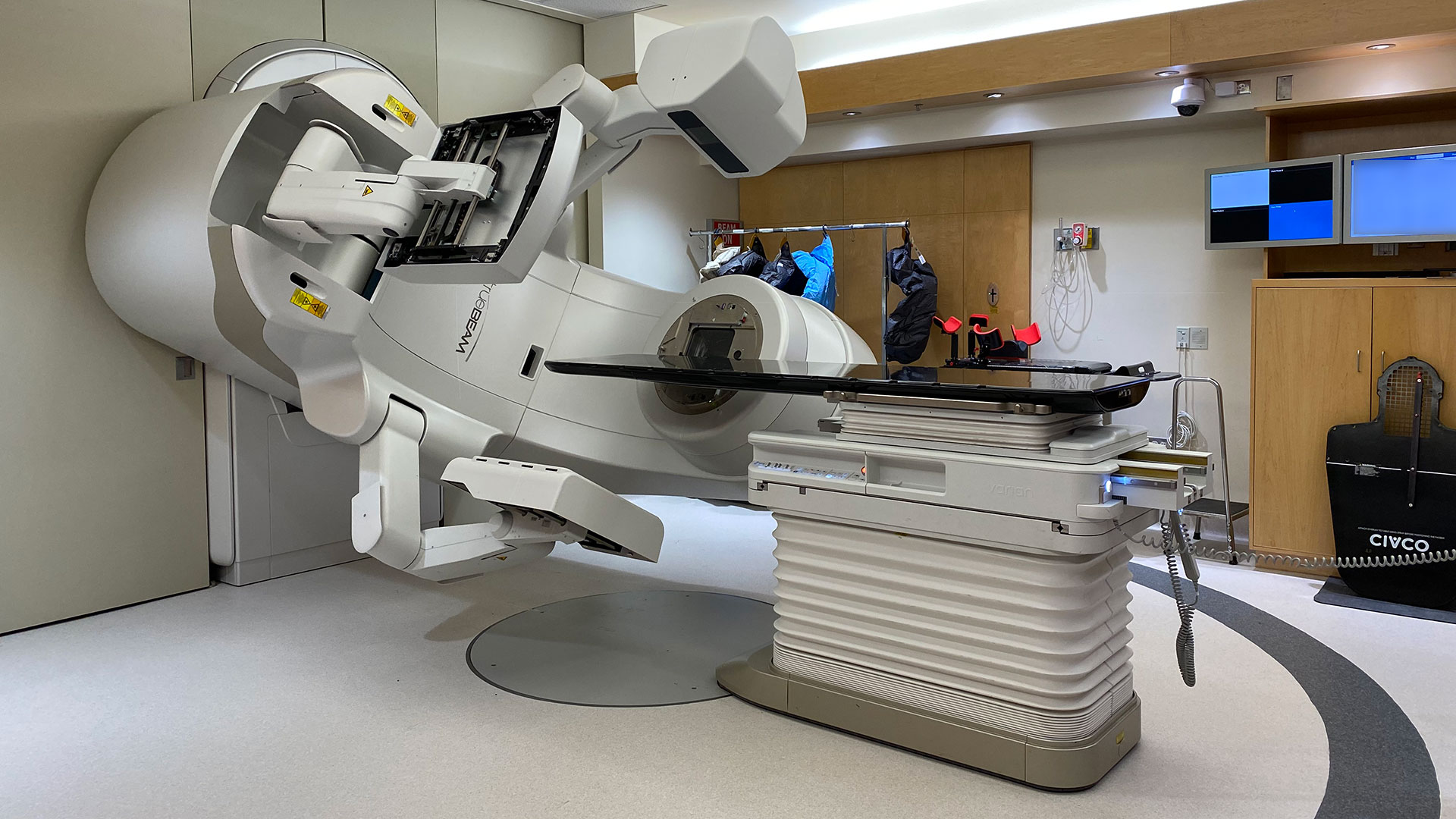
LONDON, ON – A new study published in The Lancet Oncology suggests that a very precise, high-dose form of radiotherapy called stereotactic ablative radiotherapy (SABR) may be a new treatment option for patients with inoperable kidney cancer. Lawson Health Research Institute was one of 12 participating centres from around the world with patients recruited from London Health Sciences Centre’s (LHSC) London Regional Cancer Program (LRCP).
The analysis, among the first to look at the long-term impact across multiple centres, included 190 patients with primary renal cell carcinoma, the most common type of kidney cancer. It found SABR to be effective and safe with a low rate of cancer recurrence and acceptable impact on renal function. Five years after treatment, kidney function was largely maintained and only 5.5 per cent saw their cancer return in the treated kidney.
SABR directs highly accurate and intense radiation to eradicate tumours while limiting the impact on surrounding tissues. The treatment is offered to patients who are unable or unwilling for various reasons to have surgical treatment.
Previous studies on the use of SABR for primary renal cell carcinoma have been encouraging, but this publication represents the first report of long-term follow-up from a large, international group of patients.

“This study suggests that the positive outcomes seen in our prior studies are long-lasting,” says Dr. Rohann Correa. “It shows that this non-invasive treatment is worthy of further clinical study in patients with kidney cancer.”
Dr. Correa, a Lawson Scientist and Radiation Oncologist at LHSC, says this study was the result of many years of international collaboration.
“The International Radiosurgery Consortium of the Kidney (IROCK) brought together global experience with this completely non-invasive, pioneering way to treat localized kidney cancer,” Dr. Correa explains. “Our study has shown that at five years, this technique appears to be safe and effective, giving us confidence to launch clinical trials that provide patients access to this promising treatment.”
The study was led by Dr. Shankar Siva, a Radiation Oncologist at the Peter MacCallum Cancer Centre in Australia. Dr. Siva and Dr. Correa’s teams are part of the collaborative IROCK group whose members include Surgical Oncologists and Radiation Oncologists from around the world. The team at Lawson and LHSC was a key contributor to this high-profile study, with local patients participating in the study and all international data housed and analyzed through Lawson.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Preventing infertility in men who undergo lymph node removal surgery for testicular cancer
When patients with testicular cancer undergo lymph node removal surgery there is a risk that their fertility will be affected if proper nerve sparing techniques are not used. Up to 75 per cent of men will not be able to father children if they receive the surgery without these techniques.
Lawson’s Internal Research Fund (IRF) has awarded a grant to Dr. Nicholas Power, a researcher at Lawson and urologic oncologist at London Health Sciences Centre (LHSC), who is leading a study to identify the nerves involved in fertility that are affected in lymph node removal surgery for testicular cancer.
“Sometimes patients go through a lot to be cured of testicular cancer only to be left dealing with long-term survivorship issues such as fertility. We hope to gain new insights into how fertility can be preserved after these men receive lymph node removal surgery,” says Dr. Power, who is also an assistant professor at Western University’s Schulich School of Medicine & Dentistry.
In collaboration with Schulich assistant professors Dr. Marjorie Johnson and Dr. Brian Allman, and PhD candidate Tyler Beveridge, Dr. Power published initial results in The Journal of Urology announcing their discovery of a brand new anatomic structure, the pre-hypogastric ganglion, which needs to be spared in surgery to maintain fertility. They were also able to describe the first roadmap of retroperitoneal neuroanatomy – the anatomy of nerves in the space where surgeons locate lymph nodes most commonly affected by testicular cancer that has spread.
“There has never been a definitive anatomic study of the nerves of the retroperitoneum so it was our goal to provide the first comprehensive study of the nerves as they relate directly to patients who have testicular cancer,” explains Dr. Power. “After we published the initial results we were approached by textbook authors to use our data in upcoming editions of anatomy and surgical atlases. This will help to provide insight into nerve sparing techniques for surgeons who have not been trained at high-volume centers and ultimately improve the quality of care in testicular cancer patients overall.”
Already Dr. Power has found that using this knowledge when he performs lymph node removal surgery for testicular cancer has led to a 95 per cent success rate of preserving fertility.
The IRF will go towards their research to further investigate the actual function and physiology of the retroperitoneal neuroanatomy using a pig model.
“Lawson’s IRF provides incredible support for a field of study such as ours that is not yet at the stage of applying for a large grant. Receiving the funding gives us the independence to test out novel yet important hypotheses that will then lead us to further grants,” says Dr. Power.

Above: Dr. Nicholas Power
The IRF is designed to provide Lawson scientists and students the opportunity to obtain start-up funds for new projects with the potential to obtain larger funding, be published in a high-impact journal, or provide a clinical benefit to patients. Funding is provided by the clinical departments of London Health Sciences Centre and St. Joseph’s Health Care London, as well as the hospital foundations (London Health Sciences Foundation and St. Joseph's Health Care Foundation).
Prime Minister announces support for health research
Health researchers in London and across Canada welcomed news that the federal government will provide urgently-needed financial support for research teams whose work has been largely shut down by the COVID-19 pandemic.
Prime Minister Justin Trudeau has announced $450 million in new funding to help Canada’s academic research community during the COVID-19 pandemic.
“Research staff in Canada are the source of new innovations and ideas that help keep us healthy, protect our environment, and drive our economy. We are fortunate to have some of the world’s brightest minds. We are making sure Canadian universities and health research institutes have the support they need to sustain their research capacity through this difficult situation, and continue to attract and retain talent, for the benefit of all Canadians,” says The Rt. Hon. Justin Trudeau, Prime Minister of Canada.
The investment will:
- Provide wage supports to universities and health research institutes, so they can retain their research staff who are funded from industry or philanthropic sources and are unable to access some of the government’s existing COVID-19 support measures. This would apply even if their work has been temporarily suspended. The government will provide up to 75 per cent per individual, with a maximum of $847 per week.
- Support universities and health research institutes to maintain essential research-related activities during the crisis, and to ramp back up to full research operations once physical distancing measures are lifted. This will cover up to 75 per cent of total eligible costs, and will support activities such as the safe storage of dangerous substances and restarting data sets that were interrupted during the pandemic.
“Research personnel in our universities and health research institutes are significant drivers of science, discovery, and innovation in Canada. By providing these institutions with immediate support, we continue to nurture Canada’s talent pipeline and sustain our innovation capacity, while helping to mitigate the negative impacts of COVID-19 on the research community,” says The Hon. Navdeep Bains, Minister of Innovation, Science and Industry.
This announcement follows a tremendous effort by organizations and individuals across Canada over the course of this pandemic to secure support for hospital-based research. From outreach and meetings to letters and media interviews, many advocacy-based initiatives were undertaken to bring this important issue to the attention of key decision-makers. HealthCareCAN spearheaded these efforts, working tirelessly on behalf of the national health research community.
Lawson is extremely thankful to the federal government for recognizing the critical importance of protecting Canada’s research enterprise and providing urgently-needed financial support. “While we know financial pressure remains, this will help to keep research teams intact while research has been interrupted and provide assistance for when research activities gradually resume,” says Dr. David Hill, Lawson Scientific Director.
A special thank you to local MP Peter Fragiskatos for London North Centre who took up this issue in Ottawa. His strong leadership and representation made the key difference in successfully securing this new funding.
“Tackling the COVID-19 crisis in Canada has required an all-hands on deck approach and Canada’s health researchers have answered the call by suspending all other crucial hospital-based research to meet the challenge,” adds Dr. David Hill. “With this federal support we can now work to ensure that we can maintain other critically needed research on other diseases even as we pursue what promises to be a lengthy battle against COVID-19.”
Background:
- Canadian healthcare-based research is a $3 billion annual sector of the economy and employs 50,000 highly skilled researchers and other staff across the country.
- Health research is one of Canada’s great national achievements and biomedical research conducted in Canada is at the forefront of current essential research and clinical trials around COVID-19.
- This work is fundamental to life in a society and a key driver for progress, innovation and the economy. Canada’s health researchers are global leaders in driving improvements in disease prevention, diagnosis, treatment and care.
- Ontario’s research hospitals have long been the engines of health invention and discovery in provincial and national innovation. From Ottawa, London, Toronto, Kingston, Sudbury and Thunder bay, the more than 20,000 researchers and staff at these hospitals are driven by their passion to improve health.
See also:
- Prime Minister announces support for research staff in Canada – Government news release
- Canada’s health research enterprise welcomes federal support – HealthCareCAN media release
- OHA Media Statement re: Federal Government Supporting Ontario’s Hospital-Based Research Enterprise
Probiotics could improve survival rates in honey bees exposed to pesticide
In a new study from Lawson Health Research Institute (Lawson) and Western University, researchers have shown that probiotics can potentially protect honey bees from the toxic effects of pesticides.
Honey bees are critical to agriculture as they pollinate approximately 35 per cent of the global food crop, contributing an estimated $4.39 billion per year to the Canadian economy. Pesticides are currently used to maximize crop yields, but the most common pesticides, neonicotinoid insecticides, are a major factor in colony collapse disorder which is killing honey bee populations.
“The demise of honey bees would be disastrous for humankind. A current dilemma in agriculture is how to prevent bee decline while mitigating crop losses,” says Dr. Gregor Reid, Director for the Canadian Centre for Human Microbiome and Probiotic Research at Lawson, and Professor at Western’s Schulich School of Medicine & Dentistry. “We wanted to see whether probiotics could counter the toxic effects of pesticides and improve honey bee survival.”
The study was performed by trainees Brendan Daisley and Mark Trinder in Dr. Reid’s lab at St. Joseph’s Hospital in London, Ontario. The researchers utilized fruit flies as a well-known model for studying pesticide toxicity in honey bees. Both insects are affected similarly by neonicotinoids, have very similar immune systems, and share many common microbes present in their microbiota – the collection of microorganisms found in each insect.
The researchers found that fruit flies exposed to one of the world’s most commonly used pesticides, imidacloprid (IMI), experienced changes to their microbiota and were more susceptible to infections. The flies were exposed to a comparable amount of pesticide as honey bees in the field.
By administering a specific strain of probiotic lactobacilli, survival among fruit flies exposed to the pesticide improved significantly. The mechanism involved stimulating the immune system through a pathway that insects use to adapt to infection, heat and other stresses.
“Our study showed that probiotic lactobacilli can improve immunity and potentially help honey bees to live longer after exposure to pesticides,” says Daisley, an MSc candidate. He notes that probiotic lactobacilli could be easily administered through pollen patties, which are used by beekeepers to provide nutritional support and anti-pesticide effects to honey bees.

Above: Brendan Daisley, an MSc candidate at Western's Schulich School of Medicine & Dentistry, working in Dr. Gregor Reid's lab at St. Joseph's Hospital
Over the winter months, honey bee mortality has been steadily increasing with ranges of 38 to 58 per cent in recent years, two to three times higher than the sustainable level. In Ontario alone, 340 bee keepers reported an abnormally high number of bee deaths, with over 70 per cent of dead bees testing positive for neonicotinoid residues (Government of Ontario).
“While cessation of pesticide use would be ideal, farmers currently have little alternative to obtain the yields that keep their businesses viable,” says Dr. Reid. “Until we can cease using pesticides, we need to find ways to protect humans and wildlife against their side effects. Probiotics may prove as an effective protective intervention against colony collapse disorder.”
The researchers hope to further study the mechanisms involved in this process and perform field tests on honey bee populations in Ontario.
The study, “Neonicotinoid-induced pathogen susceptibility is mitigated by Lactobacillus plantarum immune stimulation in a Drosophila melanogaster model”, is published in Nature’s Scientific Reports. The research was funded by the Natural Sciences and Engineering Research Council of Canada (NSERC).

Above: Dr. Gregor Reid, Director for the Canadian Centre for Human Microbiome and Probiotic Research at Lawson, and Professor at Western’s Schulich School of Medicine & Dentistry
Probiotics to the rescue
As the world’s most important single species of pollinators, honey bees perform many ecosystem functions. They are critical to the global food supply.
Honey bee populations are declining at alarmingly high rates here in Ontario and around the world.
“If the bees disappear, humanity is in big trouble” states Dr. Gregor Reid, Lawson researcher and professor at Western. He is also the leading scientist for the study. “Imagine walking into the grocery store and a third of the food wasn’t there. That is what would happen.”
Pesticide exposure, infection and habitat loss are the main factors suspected to be causing the decline in honey bee populations. Pesticides in particular make infections more severe and exacerbate the consequences of nutritional deficiencies in habitat loss – making those problems even worse.

Since current industrialized agricultural practice rely on pesticides to maintain high crop volume, their complete removal from the equation is not currently feasible.
“We need an alternative solution that interferes with this process where high level of pesticides cause issues like infections and habitat loss to have more severe consequences for the honey bees,” says Dr. Reid. “Supplementing honey bees with probiotic bacteria is that solution, we believe.”
“It may sound overly dramatic to state the research will ‘save the world’s honey bees’, but that is the goal, and other groups around the world are trying to follow this lead.”
The group of researchers from Lawson Health Research Institute and Western University are supplementing honey bees with a nutritional food item containing three carefully chosen strains of beneficial or probiotic bacteria to improve the overall health of the hive and specifically address infection and nutritional needs.

From left: Graduate students Anna Chernyshova, John Antonio Chmiel and Brendan Daisley are working on the honey bee probiotics project with Drs. Gregor Reid and Graham Thompson.
“We are creating what we call a BioPatty. In addition to normal nutrient substances, we infuse it with a select recipe of probiotics,” explains Dr. Graham Thompson, the regional bee expert and professor at Western University who helped set up the field-testing site and manages of the honey bee hives. “Our goal is to make the bees healthier and their immune system more vigorous. This helps them stay efficient and do their important jobs, and not be so vulnerable to the stressors of living in an urban and industrial world.”
The team’s previous scientific findings in a fly model, showed that these bacterial strains could reduce the toxic effects of pesticides and increase resistance towards infection. In May 2018, they moved their research from the lab and into the field thanks to OMAFRA funding, and started to test their BioPatties in a local apiary.
American Foulbrood caused by the pathogen Paenibacillus larvae, attacked the hives. This is one of the most serious honey bee diseases. Infection outbreaks nearly always lead to complete colony collapse and loss of the hive. “But the hives that were given the probiotics were the only ones not to be destroyed, so that was an encouraging early result,” says Brendan Daisley, a PhD student with Dr. Reid who was involved with the development of the research and coordinates sample processing and data collection.
“These results have far-reaching implications as American Foulbrood, despite its geographically-suggestive name, infects honey bees worldwide. It causes a tremendous financial burden to apiary owners and famers alike, who rely on honey bees directly or indirectly as a means of livelihood,” explains Daisley.
The probiotic approach might reduce the need for antibiotics that are so commonly used in many apiaries.
This work is taking place in London, Ontario and the study will continue over the next three years. Going forward, the researchers are planning to work with collaborators in a number of other countries around the world to determine the feasibility of large-scale implementation of probiotics for honey bees.

