Search
Search
$1.2 million in federal funding to study women Veterans experiencing homelessness
A first-of-its-kind study led by Lawson Health Research Institute is receiving $1.2 million in funding from the federal government, delivered through the Veteran Homelessness Program, to better understand homelessness amongst women in Canada who are military Veterans.
“This is an important and yet often invisible problem,” says Dr. Cheryl Forchuk, Lawson Assistant Scientific Director based at St. Joseph’s Health Care London’s Parkwood Institute and the study lead. “This is the first Canadian study to focus exclusively on women Veterans’ experience of homelessness. Gender matters, especially when we’re talking about female Veterans who are homeless. If they’ve experienced sexual trauma or abuse or have children, and the only Veteran housing available is a group setting for men, that will be an issue.”
Dr. Forchuk and her team have begun travelling to cities and towns across Canada to conduct interviews with female Veterans experiencing homelessness or who have previously experienced homelessness. They will gather data such as demographics, history of housing and homelessness, and services accessed. The team will also host focus groups with homeless- and Veteran-serving agency staff. The locations have been selected in partnership with The Royal Canadian Legion and other Veteran-serving groups, focusing on areas with pockets of female Veterans experiencing homelessness.
“We will also explore the pathways and experiences of homelessness, what barriers are faced, what has been helpful and what future services should focus on,” adds Dr. Forchuk.
“This study is a vital step towards addressing the unique challenges faced by female Veterans experiencing homelessness,” says Peter Fragiskatos, Parliamentary Secretary to the Minister of Housing, Infrastructure and Communities and Member of Parliament for London North Centre on behalf of the Honourable Sean Fraser, Minister of Housing, Infrastructure and Communities. “By investing in research like this, we are making significant progress in understanding and improving the support systems for this population, contributing to the federal government's efforts to end homelessness among Veterans.”
“This significant investment reflects our dedication to addressing the issue of homelessness among female Veterans,” says Arielle Kayabaga, Member of Parliament for London West. “By supporting this pioneering study, we aim to uncover the specific barriers they face and develop targeted solutions that honour their service and ensure they receive the support they deserve.”
The goal of the four-year study is to ensure there is accurate data to inform gender-specific interventions and guidelines for policy, practice and care of female Veterans. Canadian Armed Forces Veterans make up a disproportionate percentage of those experiencing homelessness according to a 2018 report.

“It is clear that the circumstances surrounding this particular subset of our Veteran population are not well enough understood,” says Carolyn Hughes, Director of Veterans Services with The Royal Canadian Legion. “It is our hope that this project will help fill in some of those blanks and at the same time, further enlighten all of us who serve Veterans, so that we may provide even more timely and focused assistance when and where it’s needed most.”
St. Joseph’s Parkwood Institute has an embedded legacy of Veterans’ care, having originally been a Veterans’ hospital and now hosting a Veterans’ inpatient centre, the Operational Stress Injury (OSI) Clinic, as well as the MacDonald Franklin OSI Research and Innovation Centre. The research centre is recognized as Canada’s leader in mental health research dedicated to enhancing the lives and wellbeing of military personnel, Veterans and their families. The directors of the centre are co-investigators on the study.
For more information, please contact:
Debora (Flaherty) Van Brenk
Communication Consultant
St. Joseph’s Health Care London
C: 226-577-1429 or 519-318-0657
T: 519-646-6100 ext. 42534
@email
2018 Leadership Award for Fellows & Students: Amanda McIntyre
Amanda McIntyre was presented with the 2018 Leadership Award for Fellows & Students at this year’s Lawson Impact Awards, recognizing her skills as a leader, researcher, clinician and community advocate. McIntyre is a PhD candidate in nursing at Western University and a part of Lawson researcher Dr. Robert Teasell’s team at St. Joseph’s Health Care London’s Parkwood Institute.
McIntyre began her career at Lawson as a research assistant in 2011 and since then has built an impressive academic and research record, while at the same time obtaining a nursing degree from Western University. In addition to her many research obligations, she continues to take regular nursing shifts in the emergency department to build her clinical experience.
“We nominated Amanda because she’s kind of like a renaissance person. She does a lot of things and whatever she does, she does really well,” says Dr. Robert Teasell, medical director of the Stroke Rehabilitation Unit at Parkwood Institute.
McIntyre is involved in a variety of research projects in the field of neurorehabilitation and has been an author on 50 peer-reviewed publications.
She is the project coordinator and an editor of the Spinal Cord Injury Evidence-Based Review (SCIRE), an extensive and comprehensive review of the Spinal Cord Injury (SCI) Rehabilitation literature considered to be the leading research synthesis of SCI rehabilitation anywhere in the world. She also had an active role in the development of the Canadian Best Practice Recommendations for Stroke Care.
McIntyre is a two-time recipient of the Mary Elizabeth Horney Fellowship in Rehabilitation Research, which is funded through St. Joseph’s Health Care Foundation. As part of her fellowship, she is conducting research on the transition of stroke patients from inpatient to outpatient rehabilitation, and back to the community. Her doctoral research will focus on the delivery and access of care in emergency departments and the influence this has on patient outcomes.
McIntyre has assumed a supervisory and mentorship role in Dr. Teasell’s lab. She has been instrumental to the development of many research assistants, students and volunteers.
She is also currently the graduate students’ representative on the Nursing Research Advisory Committee, and a research practicum mentor for Nurse Practitioner students at Western University, allowing her to act as an advocate for current and future nursing students.
She says, “Winning this award is a huge privilege. It represents not just my successes but our entire team’s success, so I think it’s a win for all of us.”
2018 Scientist of the Year Award: Dr. Robert Teasell
Lawson scientist Dr. Robert Teasell is considered a global leader in neurorehabilitation research and has been instrumental in transforming clinical care in this area across Canada by ensuring that clinical practices are informed by the best available and up-to-date research evidence. In recognition of his accomplishments, he received the Scientist of the Year Award at the 2018 Lawson Impact Awards event this past spring.
Dr. Teasell leads the Collaboration of Rehabilitation Research Evidence (CORRE) research team at St. Joseph’s Health Care London’s Parkwood Institute. He is also the Medical Director of the Stroke Rehabilitation Unit at Parkwood Institute and has an active outpatient chronic pain practice.
He has led the development of three internationally renowned evidence-based reviews for stroke rehabilitation, brain injury and spinal cord injury, which are regarded as the three most comprehensive research syntheses in neurorehabilitation in the world. Dr. Teasell has advised and helped plan stroke care for all of Ontario’s 14 Local Health Integration Networks (LHINs) and six provincial healthcare systems. This is in addition to the many clinical guidelines and models of care he has helped develop and update.
Dr. Teasell also bridges the gap between research and clinical practice through collaborations between his research and clinical teams. His multidisciplinary Rehabilitation Knowledge to Action Project (REKAP) team received the 2014 Sandra Letton Quality Award for their quality improvement project designed to make Parkwood Institute a leader in stroke rehabilitation by improving care through implementation of best practices.
In addition to his neurorehabilitation research, Dr. Teasell has published extensively on chronic pain with a recent focus on the role of obsessive personality traits in determining chronic pain disability and coping abilities.
Drawing on his clinical and research expertise, Dr. Teasell has supervised many students and has been committed to developing the next generation of medical researchers.
“Dr. Teasell has been successful in a number of areas. Certainly in terms of publications and mentorship of students who have gone on and had very successful careers of their own. Despite a busy clinical schedule, he always makes a point of engaging with his research team every day. His staff and students really appreciate the opportunity to work with him,” says Dr. Cheryl Forchuk, Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, and Assistant Director, Lawson Health Research Institute.
Dr. Teasell has authored 335 peer-reviewed articles, as well as many other collaborative group peer-reviewed articles, book chapters, published abstracts, posters, presentations and monographs. He has also been the editor for 14 special journal editions and is on the editorial boards for Topics in Stroke Rehabilitation, Journal of Rehabilitation, and Pain Research and Management.
In 2016, he was invited to present the Ramon J. Hnatyshyn Lecture, the leading annual national stroke lecture at the Canadian Stroke Congress in Quebec City. In 2010, he received the Canadian Association of Physical Medicine and Rehabilitation Merit award for his many contributions to the field of physiatry. He was also awarded the Royal College of Physicians and Surgeons of Canada McLaughlin-Gallie Visiting Professor in 2012. This year he will be awarded the Post-Acute Stroke Award of Excellence from the American Congress of Rehabilitation Medicine and the National Stroke Association in the United States.
“I’ve received a lot of national and international awards but there’s nothing better than being recognized by your peers and particularly your peers in the city where you work. It’s been a nice acknowledgement of not just my work, but also the work by the whole research team and all the people who have supported me over the years,” says Dr. Teasell.
2018 Staff Award of Excellence: Sarah Best
Sarah Best, research manager at Lawson Health Research Institute, was a recipient of this year’s Staff Award of Excellence, presented at the 2018 Lawson Impact Awards. The award was created to honour the contributions of dynamic, hardworking staff members who help advance science at Lawson.
Best is a part of the Cognitive Clinical Research Group at St. Joseph’s Heath Care London’s Parkwood Institute. In addition to managing the research group’s staff and trainees, she has a wide range of responsibilities, including developing strategies for recruitment and retention of clinical trial participants, budgeting, assisting with grant applications, and ensuring the team has the appropriate space, hardware and training to complete their research.
“Sarah has grown a team of skilled, well-trained staff and her leadership has ultimately resulted in an increase in the volume and complexity of trials we can offer for patients with mild cognitive impairment and Alzheimer’s disease,” says Dr. Michael Borrie, Lawson researcher and medical director of the Cognitive Clinical Research Group.
Best is also the budget officer for the Consortium of Canadian Centres for Clinical Cognitive Research and a member of the platform implementation team for the Canadian Consortium on Neurodegeneration and Aging (CCNA). The CCNA was formed by more than 350 clinicians and researchers throughout Canada to accelerate progress in age-related neurodegenerative disease research.
The Comprehensive Assessment of Neurodegeneration and Dementia (COMPASS-ND) Study is a CCNA study collecting clinical, neuropsychological, and MRI imaging data as well as blood, saliva, and urine samples from participants to learn about who is at risk of developing dementia, to determine how early dementia can be detected and to find out what tests are most effective at detecting dementia. Best has helped facilitate the study start-up and patient recruitment for the more than 30 sites involved in COMPASS-ND, including Parkwood Institute.
“Working in the field of neurodegeneration is really important right now as we see the numbers of individuals that have cognitive impairment growing exponentially. Currently, we only have symptomatic treatments so we’re really looking to find that breakthrough that will lead to a disease-modifying treatment to better serve patients and actually change the course of their disease,” says Best.
She adds, “I’m really honoured to receive this award, especially knowing the previous recipients and the impact that they've had on the London research community.”
2019 Innovation Award: Dr. Don Richardson
Dr. Don Richardson was recognized at the 2019 Lawson Impact Awards for his research and innovation in working with veterans with military-related post-traumatic stress disorder (PTSD). His study titled, “Predicators of Long-Term Treatment Outcome in Combat and Peacekeeping Veterans with Military-Related PTSD,” was recently published in the Journal of Clinical Psychiatry.
Throughout Dr. Richardson’s career, he has worked diligently to develop and implement best practice assessment and treatment guidelines for Canadian Armed Forces (CAF) members and veterans. He has developed and maintained two clinical research databases ̶ a database of self-reported health status, by working with patients at the Operational Stress Injuries (OSI) clinic, and a treatment outcomes database. Through this data, he has demonstrated that military trauma populations are complex and are at greater risk of becoming resistant to treatment than most civilian trauma populations.
“Don is extremely deserving of this award,” says Dr. Cheryl Forchuk, Dr. Richardson’s nominator. “When I think of someone who does a great job of linking together research and clinical practice, Don is always someone who comes to mind.”
The treatment outcomes database gives researchers unparalleled insight into the pharmacologic interventions best suited for CAF members and veterans. With the ability to identify when individual patients are experiencing less-than-optimal outcomes, the research team can adjust their treatment plan accordingly.
Over the past 20 years, Dr. Richardson has published over 40 peer-reviewed manuscripts and book chapters on the assessment and treatment of operational stress injuries, PTSD, major depressive disorder, substance use disorders, and suicidal behaviour. He has elevated awareness for the unique mental health challenges faced by CAF members and veterans who present with operational stress injuries.
In light of Dr. Richardson’s findings, he works to assess the current treatment modalities for PTSD, their utility for treating military populations, as well as complementary therapies that may prove beneficial.
Dr. Richardson’s dedication to military mental health research is evident through his unwavering effort and has attracted the attention of many prominent figures in the field of military and veteran health. In 2017, he was granted the opportunity to build a research and innovation center for advancing military and veteran health research and clinical practice. Through a generous donation from two community peers, Dr. Richardson established and leads the Macdonald/Franklin OSI Research Centre, located at Parkwood Institute.
“It is certainly an honour to receive this award,” says Dr. Richardson. “I wish to thank all of my clients for taking the time to fill out the repeated questionnaires, as well as the research staff who support this program, and who work tirelessly to help our CAF members and veterans.”
Addressing the impacts of the COVID-19 pandemic
As the COVID-19 pandemic has continued for a year and a half, many people from all walks of life are feeling the impacts especially when it comes to their mental health and wellbeing.
Hospital researchers through Lawson Health Research Institute, along with its hospital partners, have been studying the impacts for some key groups.
Health care workers have been at the forefront of the pandemic. These heroes have worked tirelessly through every wave and continue to provide excellent care to their patients and community. Dr. Kamia Honarmand, Critical Care Physician at London Health Sciences Centre (LHSC), remembers the stress that she and her colleagues were feeling, and know that something needed to be done.
“Our team wanted to better understand the impact of the pandemic on the lives of health care workers, both personally and professionally, and understand how they were coping when it came to their mental health,” says Dr. Honarmand who is also an Associate Scientist at Lawson. “There was a lot of reasons to be stressed even before the height of the first wave in our region. There was a lot of anxiety. The hospital wanted to find ways to support health care workers and identify resources that would assist them.”

Dr. Kamia Honarmand, Critical Care Physcian at LHSC and Lawson Associate Scientist
Frontline health care workers across the region were invited to take part in an online survey about their experiences during the pandemic. “We looked at both the impacts and the preferred coping strategies, and what supportive strategies they would like to have in the hospital in the future.”
The Veterans Care Program located at Parkwood Institute, a part of St. Joseph’s Health Care London, provides complex continuing and long-term care for Canadian war Veterans. Dr. Don Richardson, Director of the MacDonald Franklin OSI Research Centre at Parkwood Institute, has been treating and studying mental health among Veterans for many years. He believed this was a group was likely to be affected by the pandemic in unique ways.
“We know that Veterans in general are at a higher risk for depression, anxiety and PTSD,” explains Dr. Richardson, who is also a Scientist at Lawson. “We also knew the pandemic and forced restrictions would have significant impact on Veterans and their families who would be more isolated than they already are.”
More than 1,100 Veterans and around 250 spouses were recruited for the study, completing an online survey every three months for 18 months.
The study is still ongoing, but Dr. Richardson says the initial data has been telling. “We have been able to analyze some of the preliminary data and what we have found is that almost 50 per cent did not indicate their mental health had worsened during the pandemic but 40 to 50 per cent have had difficulty accessing care.”

Dr. Don Richardson, Director, Macdonald Franklin OSI Research Centre
The hope is that this study will lead to better preparedness in the future to safeguard the mental health of Veterans and ensure their access to care during a pandemic.
Many people have felt isolation during the pandemic, but that feeling may have even more of an impact for youth suffering from mood and anxiety disorders.
Dr. Elizabeth Osuch, Director of the First Episode Mood and Anxiety Program (FEMAP) at LHSC says the pandemic-led lockdown forced more than a hundred mental health clients out of in-person services.

Dr. Elizabeth Osuch, Director of FEMAP and Lawson Scientist
“They lost their resources for mental health services and support as soon as the quarantine was announced,” shares Dr. Osuch, who is also a Scientist at Lawson. “We were concerned that it would be devastating to people – and to some people it was. We wanted to make sure they had an avenue to connect with the program.”
Dr. Osuch and the FEMAP team created an online research platform to find out how patients were doing by having them fill out a symptoms and function questionnaire.
“We have analyzed the first wave so far and it shows that male patients were doing better and female patients were doing worse, which was a surprise. One of the risk factors for not doing well was the loss of their job.”
The pandemic added an extra layer of stress and worry for women who were having a baby.
“This has been an enormous and pivotal time for everyone in the world,” says Dr. Genevieve Eastabrook, Obstetrician-Gynecologist at LHSC. “The experiences during pregnancy and post-partum for both the birthing person and their baby can have effects later in life for children. For example, their overall cardiovascular and metabolic health, bonding experiences and the risk of mood disorders.”
Dr. Eastabrook, who is also an Associate Scientist at Lawson and Assistant Professor at Western University’s Schulich School of Medicine & Dentistry, is working with a team to examine the effects the pandemic may be having for mothers and their babies. As part of the study, the London research team is using an approach called ‘One Health’ which offers a holistic perspective to explore how various risk factors and social determinants of health interact.

Dr. Genevieve Eastabrook, OBGYN at LHSC and Lawson Associate Scientist
“The unique aspect is that we have a comparative group to see if there are differences in markers such as risk of depression, perceived stress and social supports,” adds Dr. Eastabrook.
Study participants are asked to complete a 30-minute questionnaire at around 6-12 weeks after their delivery. The research team is still recruiting patients for this study.
An online approach to care
With an aging population, neurological conditions like stroke, brain injury and multiple sclerosis (MS) are on the rise in Canada. Those living with neurological conditions face many long-term challenges that can affect both their physical and cognitive functioning. They are also at an increased risk for mental health challenges such as depression and anxiety.
“While mental health challenges are common for those with neurological conditions, they often go untreated for a number of reasons,” says Dr. Swati Mehta, Scientist at Lawson Health Research Institute. “For example, those living in remote areas often do not have access to specialized services and many patients are concerned about stigma.”
Yet seeking mental health care is critically important for patients with neurological conditions. “Research suggests that depression among these patients can impair recovery, leading to decreased quality of life and increased health care costs.”
To improve patient outcomes, Dr. Mehta and a collaborative research team are developing an internet-delivered cognitive behavioural therapy (ICBT) program.

Cognitive behavioural therapy (CBT) is a specialized type of therapy that involves patients learning strategies and skills to self-manage mental health symptoms. It’s one of the most widely used therapies for the treatment of depression and anxiety.
A panel of researchers, persons with lived experience of neurological conditions and community organizations are working collaboratively to develop an accessible ICBT program that meets the needs of persons with neurological conditions and mild cognitive impairment who are also experiencing symptoms of depression or anxiety. The program, called The Neuro Course, will be a modified version of an existing course developed in Australia by the eCentreClinic.
“Through co-development with patients and experts in the field, the ICBT program will meet the specific needs of persons with neurological conditions who are also experiencing mental health challenges,” explains Dr. Mehta. “With online delivery, it can provide personalized treatment while being flexible and easily accessible.”
The Neuro Course will be piloted with a small group of research participants, including patients from Parkwood Institute, a part of St. Joseph’s Health Care London. Eligible participants can sign up to be notified of the course’s availability at https://www.onlinetherapyuser.ca/neuro.
The free online course consists of six easy-to-understand CBT lessons and will take approximately 10 weeks to complete. In addition to the six lessons, participants will be encouraged to work through various activities during the week.

Participants will also receive regular support from a designated online guide. Guides will be health educators who are certified providers or graduate students working under the supervision of certified providers. All guides will have training in psychology or social work. The participant’s guide will review the participant’s progress and answer any questions or comments through a secure messaging system.
Participants in the study will be asked to complete brief questionnaires before they begin the course, on a weekly basis throughout the course and then again three months after treatment ends. The research team will use the questionnaires to assess patient outcomes and improve future versions of the course.
The goal of the program is to overcome barriers to face-to-face therapy, such as limited access to specialized care and concerns about stigma related to seeking care, by providing an effective online alternative. By reaching those in need, the research team hopes to improve patient outcomes and overall wellbeing.
“The long term goal would be to implement the ICBT program into clinical practice to provide increased access to mental health services among this population,” says Dr. Mehta. “The program could be used to provide care to those with mild to moderate mental health concerns or those waiting to access face-to-face programs.”
The team is being funded for this project through Lawson’s Internal Research Fund (IRF) competition. “As an early career researcher, receiving funding from Lawson’s IRF is a great honour. It’s a great opportunity to help researchers obtain funding for small feasibility studies to develop evidence for larger grants that can be used to translate knowledge across the community,” states Dr. Mehta.
Assessing neurofeedback in stroke survivors
A new study aims to assess the use of functional near-infrared spectroscopy (fNIRS), a type of imaging, to provide neurofeedback during stroke rehabilitation with a goal of eventually improving patient outcomes.
fNIRS is used to detect changes in brain oxygen levels using light. More recently it has also been used to develop brain-computer interfaces (BCIs), which allow patients with brain injuries to control devices like robotic arms with their thoughts.
Dr. Sue Peters, a Scientist at Lawson Health Research Institute and Director of the Neurorehabilitation Physiology Lab at St. Joseph Health Care London’s Parkwood Institute, was one of the recipients of the Spring 2022 Lawson Internal Research Fund (IRF) Awards.
The funds will go towards a new study to assess whether fNIRS can be used to direct neurofeedback in stroke survivors – helping them with rehabilitation.
“Currently, there's no real measure of brain activity that is used in stroke rehabilitation to help make clinical decisions,” says Dr. Peters, who is also a Professor at Western University.

Over 400,000 Canadians live with the effects of a stroke, according to the Heart and Stroke Foundation, and there’s hope that fNIRS could make a big difference by eventually improving movement and independence.
“We're going to use the device in some common tasks that people might do with their arm and determine whether we can use this device reliably and accurately in a stroke-related context,” Dr. Peters explains.
Participants in the study will imagine moving while remaining still. This activates very similar parts of the brain to when people actually move. If done correctly, patients will see a visual cue generated through measurement using fNIRS.
“We know from MRI studies that when I move my right hand, the left side of my brain is activated,” notes Dr. Peters. “We think we can use this concept in stroke rehab.”
Dr. Peters is recruiting 40 people from the community who are at least six months post stroke and 40 healthy adults of all ages. They will first participate in motor assessment with a physiotherapist and then wear an fNIRS cap while thinking about moving their wrist to measure brain activity.
Previously, there were a lack of methods to image the brain during real-life movement.
“The hope is to eventually conduct a clinical trial where we're testing motor interventions to see whether some things are more effective than others at activating the regions of the brain that were impacted by the stroke.”
Dr. Peters believes the study has the potential to have a big impact on the future of rehabilitation for stroke patients, leading to lasting changes in quality of life.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Assessing the pandemic's impact on Canadian Veterans and their spouses
Multiple studies are reporting the pandemic’s impact on the mental health of Canadians, but what effect is it having on our nation’s Veterans and their spouses?
“With concerns about COVID-19 infection and drastic changes to everyday life, the pandemic is taking a toll on the health of Canadians,” explains Dr. Don Richardson, Associate Scientist at Lawson Health Research Institute and Director of the MacDonald Franklin Operational Stress Injury (OSI) Research Centre, located at St. Joseph's Health Care London's Parkwood Institute. “And it may be particularly distressing for those vulnerable to mental illness.”
Population studies show that Veterans are at double the risk of mental illness when compared to the rest of the population. They experience higher rates of depression, anxiety and loneliness. Spouses of Canadian Veterans are also at higher risk of distress, as they may sometimes undertake significant caregiving responsibilities that that require significant emotional and time investments.
“It’s currently unknown how the pandemic will impact Veterans and their spouses, but it could result in particularly serious outcomes,” says Dr. Anthony Nazarov, Associate Scientist at Lawson and the MacDonald Franklin OSI Research Centre.
In a new project from Lawson and the Centre of Excellence on Post-Traumatic Stress Disorder (PTSD), researchers will seek answers to these questions by partnering with up to 1,000 Canadian Veterans and 250 spouses of Canadian Veterans. Through online surveys, the project will hear directly from Veterans and their spouses to assess the pandemic’s effects on their well-being over time. The team hopes results can be used by health care workers and policy-makers to support Veterans and their families during both the current pandemic and future public health emergencies.
“We want to hear from all Canadian Veterans and their spouses, whether they’re doing well or not and whether they’re seeking care or not,” explains Dr. Nazarov.

From left: Drs. Don Richardson and Anthony Nazarov
Participants will complete online surveys, available in both English and French, once every three months for a total of 18 months. They will be asked questions about their psychological, social, family-related and physical well-being, and any relevant changes to their lifestyle and health care treatment.
“Veterans who regularly access health care services could encounter significant changes, including a move to virtual care appointments. This could lead to increased caregiving responsibilities for spouses,” says Dr. Nazarov. “Given the uncertainty surrounding the pandemic, these changes may persist well into the future, mandating a thorough assessment of patient satisfaction and treatment outcomes.”
The team hopes results can be used to support the wellness of Veterans and their families during public health emergencies. This includes providing health care professionals and policy-makers with information to guide emergency preparedness policies and health care delivery models. They hope results can also be used to recognize early signs of distress in order to target with early interventions.
“We are seeking to understand the impact of COVID-19 on Veterans and their families to identify if this global pandemic is leading to psychological distress or triggering historical traumas,” says Dr. Patrick Smith, CEO of the Centre of Excellence on PTSD. “The Centre’s primary goal is to increase Canadian expertise related to military and Veteran mental health, suicide prevention and substance use disorders. This study can help us understand if the pandemic is having debilitating and life-altering effects, and help us address a potential mental health crisis.”

Dr. Patrick Smith
Celebrating remarkable women in science
Chronic pain can affect every facet of a person’s life. “When someone is in pain, they can have significant difficulty with activities we all do in our daily life, from getting out of bed to walking to the mailbox. It can also impact their mental wellness,” shares Lawson Health Research Institute Scientist Dr. Siobhan Schabrun, PhD. Dr. Schabrun, who is the first ever William and Lynne Gray Endowed Research Chair in Mobility and Activity at St. Joseph’s Health Care London, has dedicated much of her career to unravelling the complex connection between the body and the mind known as neuroscience, with a focus on persistent pain.
She is currently leading groundbreaking work in understanding, treating and preventing persistent pain, offering hope for enhanced mobility and activity in individuals with musculoskeletal and neurological conditions at St. Joseph’s Gray Centre for Mobility and Activity, located at Parkwood Institute.
Dr. Schabrun’s research program has extended beyond conventional approaches, delving into the use of non-invasive brain stimulation technologies such as repetitive transcranial magnetic stimulation, more commonly known as rTMS, a therapeutic tool used in mental health treatments for decades, to augment neuroplasticity and optimize outcomes in rehabilitation.
Bridging the gap between human pain models and clinical trials, Dr. Schabrun’s work is contributing to the understanding of clinical pain populations and bringing new treatment methods to the forefront to improve patient care and outcomes.

Clinical trial will evaluate new therapy for treatment-resistant depression as a result of bipolar disorder
Treatment-resistant depression is a severe form of illness that does not respond to traditional therapies like medication and counselling. It is particularly common in patients with depression from bipolar disorder who are left with limited treatment options.
“There are some mental illnesses that can become resistant to therapy, similar to how infections, for example, can become resistant to antibiotics,” explains Dr. Amer Burhan, researcher at Lawson Health Research Institute and neuropsychiatrist at St. Joseph’s Health Care London. “Patients with those illnesses need more options.”
Brain stimulation is a field that holds promise for this patient population.
“When people are in a state of depression, research shows their brain networks are not functioning properly,” says Dr. Burhan. “Brain stimulation aims to stimulate neurons in the brain to correct activity and improve patient outcomes.”
Through involvement in a national clinical trial, Dr. Burhan and his research team at Lawson are offering new hope with a treatment called magnetic seizure therapy (MST). The study is the first randomized controlled trial to examine the efficacy of MST for patients with treatment-resistant depression as a result of bipolar disorder.
For years electroconvulsive therapy (ECT), one form of brain stimulation, has been the gold standard for patients with treatment-resistant depression. ECT uses an electric field to induce a seizure that provides a therapeutic benefit by stimulating the brain. But while ECT is effective, many patients opt out of treatment due to stigma surrounding the therapy and its potential for cognitive side effects like disorientation and amnesia.
MST has emerged as a promising alternative. MST works in a similar way to ECT but uses a focused magnetic field as opposed to electricity. As a result, MST induces a more focused seizure to reduce the risk of cognitive side effects.
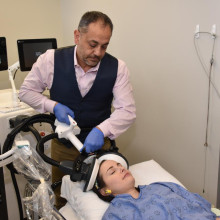
“Magnetic seizure therapy has already been shown as a promising treatment for major depressive disorder or unipolar depression,” explains Dr. Amer Burhan, local site lead for the clinical trial. “For the first time, we’re studying how effective the treatment is for depression as a result of bipolar disorder and whether it can reduce the risk of cognitive side effects associated with electroconvulsive therapy.”
The clinical trial is being led by the Centre for Addiction and Mental Health (CAMH) and will also be offered through Lawson and University of British Columbia (UBC) Hospital. Lawson researchers will invite approximately 30 eligible patients with treatment-resistant depression from bipolar disorder to participate in the trial at Parkwood Institute, a part of St. Joseph’s Health Care London.
Eligible patients will be randomized to receive either ECT or MST. Patients will be offered support throughout the study with the goal of improving patient outcomes in both groups. Patient outcomes will be compared to study the whether MST is effective and whether it is associated with reduced cognitive side effects.
MST will be delivered under anesthesia in 12 to 20 sessions. Sessions will last 10 to 15 minutes each with 60 to 90 minutes of recovery time.
“Magnetic seizure therapy holds promise of one day replacing electroconvulsive therapy as the gold standard for treatment-resistant depression, but we need to learn more about where it fits in our toolbox of potential treatments,” says Dr. Burhan.
If proven as a viable first-line treatment, MST would be very easy to implement in existing ECT clinics. MST would therefore be readily available to patients in need.
“We are on the leading edge of the field of brain stimulation for treatment-resistant depression in collaboration with CAMH and UBC,” says Dr. Burhan. “Our goal is to continue informing the care process through clinically-relevant research that serves patients, medical professionals and the public.”
Those who would like more information about the trial can email @email or @email.
Dr. Arlene MacDougall appointed Director of Research and Innovation for St. Joseph’s Mental Health Care
Dr. Arlene MacDougall has been appointed as Director of Research and Innovation for mental health care at St. Joseph’s Health Care London and Lawson Health Research Institute.
She will oversee and facilitate all mental health care research at both Parkwood Institute and Southwest Centre for Forensic Mental Health Care, working to develop strong local and global partnerships, engage patients and their caregivers in research activities, and foster trans-disciplinary approaches to research.
Her goal is to build on existing research strengths in mood disorders, suicide and smart technology. She also will look to develop research links between Mental Health and Parkwood Institute’s other major research programs, Cognitive Vitality and Brain Health, and Mobility and Activity.
Dr. MacDougall joined Lawson and the Department of Psychiatry at the Schulich School of Medicine & Dentistry, Western University in 2013 working with the Prevention and Early Intervention Program for Psychoses at London Health Sciences Centre. Last year she was cross appointed to the Department of Epidemiology and Biostatistics at Schulich.
“I come to this new role with a great deal of optimism, energy and enthusiasm. Parkwood Institute Research has a number of established strengths in the mental health care field as well as potential for new streams of research and innovation,” says Dr. MacDougall. “I look forward to working with researchers, staff, and patients and their supporters, as well as academic and community partners, to make Parkwood Institute a leading centre in Canada for mental health research.”
Parkwood Institute Research is a Lawson program that represents inter-disciplinary clinical research and focuses on the advancement of innovations and discoveries that directly improve patient care.
Dr. MacDougall will continue her own program of research, which includes recovery-oriented interventions for people with serious mental illness locally and in Africa. She is leading local studies on the use of mindfulness meditation and participatory video interventions to promote recovery among youth with early psychosis. She is also leading a project based in Kenya using social businesses and a low cost psychosocial rehabilitation toolkit to create meaningful employment, promote social inclusion and support the overall functioning and recovery of people with serious mental illness in low income settings.
Most recently she has been involved in developing and leading initiatives that use social innovation approaches to tackle complex mental health system challenges both locally and globally.
At Western, she is the Director of Global MINDS (Mental Health Incubator for Disruptive Solutions) @ Western, an educational and research initiative that supports students, faculty and community stakeholders to create solutions that will reduce the global burden of mental disorders. Global MINDS is focused on innovating for low and middle income countries and for marginalized communities in Canada. Another initiative, MINDS of London-Middlesex, is working with multiple local stakeholders to collaboratively establish a social innovation lab and use collective impact approaches that will lead to solutions that address complex challenges in the local mental health system.
Dr. MacDougall began her new role on February 1, 2017 and joins Drs. Michael Borrie and Tim Doherty as Joint/Acting Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery. She also joins Lawson’s Research Executive Committee as Assistant Director (interim) for Parkwood Institute Research, Mental Health.
Easing the pressure for patients with chronic wounds
Chronic wounds represent a significant burden in Canada. Between four and 30 per cent of patients develop a chronic wound, depending on the health care setting. Over 85 per cent of all Spinal Cord Injury (SCI) survivors will experience health complications related to pressure ulcers, injuries to the skin and underlying tissue resulting from prolonged pressure. These types of wounds can significantly reduce participation in meaningful activities and overall quality of life.
Research from around the world shows that electrical stimulation can help speed the healing of pressure ulcers. This therapy is currently done by a trained health care provider and is not readily available for people across Canada.Electrical stimulation therapy (E-Stim) is a wound treatment that involves applying low levels of electrical current to the wound bed and surrounding tissues. It stimulates several healing processes, promotes local circulation and prevents infections.
The E-Stim Collaboration: A Best Practice Implementation Project for Better Pressure Ulcer Care aims to improve the coordination of pressure ulcer care and promote the use of evidence-informed wound treatments for people living with SCI. In particular, the research project is studying how to best provide E-Stim to people with pressure ulcers, in their own communities.
“Over the years I’ve seen the serious impact pressure ulcers have on the lives of people with spinal cord injury and other health challenges. This is what drives my commitment to not only develop best practice guidelines, but also to ensure they are put into action,” says Dr. Pamela Houghton, Associate Scientist, Lawson and Professor, School of Physical Therapy at Western University. “Advances in technology make it possible for more people with care needs to live at home.”
The pilot project in the South West LHIN has a unique model that builds capacity in the community and taps into the lived experience of people with pressure ulcers and SCI. It brings together the expertise of researchers, clinicians and managers from academia, hospital centres and community care.
Partners include the Parkwood Institute Research program at Lawson Health Research Institute, Western University, Saint Elizabeth’s Health Care Research Centre, Sunnybrook Health Sciences Centre and the South West Community Care Access Centre. An interdisciplinary specialized team, called SCIPUT, has been established within the Spinal Cord Injury Rehabilitation program provided at Parkwood Institute, St. Joseph’s Health Care London.
“Our collaborative team is using the PLAN-DO-STUDY-ACT quality improvement model. This allows us to learn from each cycle and make adjustments as we go,” says Dr. Houghton. “We have just completed the first cycle and are reporting on lessons learned.” Funded by the Rick Hansen Foundation, the team hopes this will set the stage for a larger cross-country initiative.
Those interested in participating can contact phoughto@uwo.ca. The study is open to:
- Individuals with an open pressure ulcer and with a condition that causes limited mobility and/or requires a wheelchair;
- Those who are able and willing to participate in treatment plan, and communicate feedback; and,
- People who are eligible to receive services from South West CCAC.
|
Image
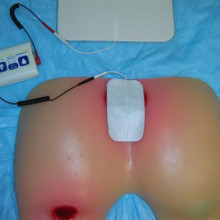
Electrical stimulation (E-Stim) directly stimulates several wound healing processes, promotes local circulation and prevents wound infections. It produces faster healing and wound closure. A trained health care provider applies low levels of electrical current to the pressure ulcer using specialized equipment. |
Embracing health research this holiday season
Community members, patients and families, and those working in the health field attended a special open house on November 28 by research groups at Lawson Health Research Institute. Together, they celebrated the holiday spirit and the gift of hope that is made possible through hospital-based research.
A part of St. Joseph’s Health Care London, Parkwood Institute represents the next era in care, recovery and rehabilitation. Across the site, clinical and research teams in different disciplines and specialties collaborate not only with each other but also with patients and families.
“Many people in the community know the high-quality and compassionate care that is supported by the various clinical teams at Parkwood Institute, but aren’t aware of the research happening at this site,” says Dr. Cheryl Forchuk, Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, and Assistant Scientific Director at Lawson.
“Lawson researchers at Parkwood are tackling important challenges with highly innovative and meaningful solutions that help improve care and quality of life.”
For the past three years, the open house gives guests a more in-depth understanding of hospital-based research and its impact. Dr. Forchuk notes that it is a great chance to talk to the researchers and their teams, and to learn about research in a really fun and interactive way. Guests may also learn about opportunities to participate in studies, as the research teams rely on people in the community getting involved.

There were 12 interactive program displays from Parkwood Institute Research, a Lawson program, in the areas of cognitive vitality and brain health, mobility and activity and mental health:
- Cognitive Clinical Trials Group (CCTG)
- Collaboration of Rehabilitation Research Evidence (CORRE)
- Gait and Brain Lab
- Geriatric Mood Disorders Lab
- MacDonald Franklin OSI Research Centre (Occupational Stress Injury)
- Mental Health Nursing Research Alliance (MHNRA)
- Mental Health INcubator for Disruptive Solutions (MINDS) of London
- Neuropsychiatry and Therapeutic Brain Stimulation Research Group
- Occupational Therapy and Spiritual Care Research Lab
- R2P (Research to Practice)
- Rehabilitation Mental Health
- Wound Care
The open house had a festive theme and many of the exhibits involved a problem solving or interactive elements to encourage learning and foster teamwork.
Karen Vecchio, federal Member of Parliament for Elgin-Middlesex-London, was among the over 200 people in attendance.

At the open house, from left: Dr. Cheryl Forchuk, MP Karen Vecchio and Roy Butler, St. Joseph's Vice President.
“London is a great community to conduct research,” explains Dr. Forchuk. “We are a mid-size city surrounded by rural areas, in many ways reflecting Canada as a whole. A lot of our projects cover the country with multiple sites and results found here by our leading experts are being implemented in health centres and national strategies in this country and around the world.”
First clinical guidelines in Canada for pain following spinal cord injury
Researchers at Lawson Health Research Institute are the first in Canada to develop clinical practice guidelines for managing neuropathic pain with patients who have experienced a spinal cord injury (SCI).
Neuropathic pain is complex and chronic, and is the most common complication reported by people following SCI. The research team worked with care providers at Parkwood Institute, part of the St. Joseph’s Health Care London family, and an international panel to address the complex and unique challenges for managing pain during recovery and rehabilitation.
In 2003, Dan Harvey sustained a spinal injury after falling off a trampoline. Using his personal experience, as well as his experiences meeting with newly injured people, Harvey contributed to the development of the new guidelines.
“Neuropathic pain – and pain in general – affects every person with a spinal cord injury very differently. Some people have it, some people don’t. But for those who do have it, it can make rehabilitation and recovery much more difficult,” explains Harvey.
“On top of just learning how to use your body again, you also have to deal with various forms of physical pains, which can make it challenging to mentally adapt to an injury.”
For those with chronic pain, it may be hard to just get out of bed in the morning, feel well enough to leave the house, or even fall asleep. “I have fairly extensive neuropathic pain, so I’m well aware of how difficult it can be to get a full night’s sleep, or show attentiveness at work or at school when it literally feels like your legs are on fire,” says Harvey.

Dan Harvey with Lawson researchers Stacey Guy, Swati Mehta and Dr. Eldon Loh.
Dr. Eldon Loh, Lawson Researcher and Physical Medicine and Rehabilitation Specialist at St. Joseph’s, and his team recognized that pain can be an overlooked part of a spinal cord injury and plays a major factor in the success of rehabilitation. It’s difficult for someone in pain to participate fully in their own recovery, and so long-term disability becomes more likely. Pain is difficult to manage and it often takes multiple approaches to find something that works for each person.
“This is a starting point for us to standardize how we approach pain in the clinic. We have identified gaps and offered recommendations to not only manage the pain, but also ensure that our patients can fully benefit from rehabilitation,” says Dr. Loh.
The results of the three-year process led to recommendations for screening and diagnosis, treatment and models of care. Important clinical considerations accompany each recommendation.
“For those in hospital following an injury, it’s about making sure they can be as independent as possible before discharge. Over time, we want to keep pain levels under control so that they are able to live life to the fullest,” adds Dr. Loh.
The research will inform new tools and resources for care providers and patients.
Harvey believes the guidelines will have a tremendous impact for patients whose pain may have been overlooked. “Pain can be created through many different avenues and the effects can snowball after a person is discharged and sent home. If you don’t check all of the boxes, you might be missing a very important item.”
The new guidelines have been published in the international journal Spinal Cord. The Ontario Neurotrauma Foundation and Rick Hansen Institute provided funding for the research study.
A special thanks to individuals from St. Joseph's who were involved in the project: Steve Orenczuk, Patrick Potter, Keith Sequiera, Lindsey Guilbault, Robert Teasell, Anna Kras-Dupuis, Dalton Wolfe, Alba Casalino and Dwight Moulin.

Additional members of the panel that developed the new clinical practice guidelines.
Global initiative aims to prevent falls in older adults
Chaired by Dr. Manuel Montero-Odasso, Scientist at Lawson Health Research Institute, a group of 96 experts from 39 countries and 36 societies and agencies in Geriatric Medicine and Aging have come together to develop the “World Guidelines for Falls Prevention and Management for Older Adults: A Global Initiative.”
Published in Age and Ageing, the official journal of the British Geriatric Society, the guidelines provide recommendations to clinicians working with older adults to identify and assess fall risks.
“The global population is aging. Thanks to social and medical advances, some chronic conditions are diminishing proportionally. This is not the case for falls,” says Dr. Montero-Odasso, who is also a Geriatrician at St. Joseph’s Health Care London’s Parkwood Institute and a Professor at Western University’s Schulich School of Medicine & Dentistry. “Unfortunately, falls and related injuries among older adults are increasing and there is no sign of future decline.”
With new evidence and studies released since previous guidelines were published more than a decade ago, experts felt it was the right time for an update and an opportunity to incorporate a worldwide perspective
“Besides the rigorous methodology that 11 international working groups followed to provide new meta-analyses, including several new Cochrane collaborations, this World Falls Guidelines are, to the best of our knowledge, the first clinical practice guidelines in fall prevention to include a panel of older adults with lived experience in falls and mobility problems,” says Dr. Montero-Odasso. “They provided feedback, comments and opinions on our recommendations, making them considerably better and with wider applicability.”
Some key themes in the recommendations include:
- Falls can be prevented, but it requires multidisciplinary management.
- Preventing falls has wider benefits for quality of life.
- Fall risk can be assessed by trained clinicians with simple resources.
- A combination of interventions, including specific exercises to improve balance and strength, when delivered correctly, can effectively reduce fall risk in older adults.
Dr. Montero-Odasso says there was enough evidence to suggest that a global approach is needed to prevent falls in older adults and that “low risk does not mean no risk.” Even active older adults who are low risk should work on preventing loss of mobility and falls.
The next steps are for the guidelines to continue obtaining formalized endorsement of all the groups involved in the initiative and then for the guidelines to be fully implemented.
You can read the full guidelines here.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
How changes in the brain affect walking while talking in older adults
Dr. Manuel Montero-Odasso’s research demonstrates that gait testing, such as walking while performing a cognitively demanding task like counting backwards (dual-task gait),can be an effective predictor of progression to dementia. In a new study, a team at Lawson Health Research Institute and Western University’s Schulich School of Medicine & Dentistry has discovered changes to the brain that correspond to these findings.
These changes identify a brain mechanism that corresponds with slow dual-task gait among older adults with mild cognitive impairment (MCI), an intermediate stage between the expected cognitive decline of normal aging and the more serious decline of dementia. Through their work Dr. Montero-Odasso and his team have found that a high dual-task gait cost, or a significant slowdown in walking speed when dual-tasking, is associated with a two- to three-fold increased risk of progression to dementia. However, the brain mechanism underlying this association was unclear.
To address this research question, Dr. Montero-Odasso partnered with Robert Bartha, PhD, an imaging scientist at Schulich Medicine & Dentistry and Robarts Research Institute at Western University. The team used magnetic resonance imaging (MRI) to examine the medial temporal areas of the brain, particularly the hippocampus, the parahippocampal gyrus, and the entorhinal cortex, which are regions particularly vulnerable to degeneration in Alzheimer’s disease. Participants were 40 older adults with MCI taking part in Dr. Montero-Odasso’s “Gait and Brain Study” at St. Joseph’s Health Care London’s Parkwood Institute.
The researchers found that participants with higher dual-task gait costs had a smaller grey matter volume in the left entorhinal cortex. Although grey matter volume loss is a common finding in people with Alzheimer’s disease, it is still unclear which areas of the brain are first affected by neurodegeneration. This finding points to the entorhinal cortex as a susceptible brain region in early stages of cognitive decline. This is in line with previous studies reporting that progression to Alzheimer’s disease is associated with volume loss in the entorhinal cortex.
The study therefore suggests that cognitive and motor dysfunction in older adults with MCI share common changes to the brain. This further supports that dual-task gait changes may be a measurable motor marker for neurological degeneration happening in Alzheimer’s disease.
“These novel results show that early brain changes common to pre-dementia states can be manifested by the way patients walk,” says Dr. Montero-Odasso, scientist at Lawson, geriatrician at St. Joseph’s Health Care London, and professor at Schulich Medicine & Dentistry. “This evidence supports walking while performing a cognitively demanding task as an important way to help predict dementia.”
The study, “Entorhinal Cortex Volume Is Associated With Dual-Task Gait Cost Among Older Adults With MCI: Results From the Gait and Brain Study,” is published in The Journals of Gerontology: Series A.
Improving mental health treatments for stroke patients is the focus of a new study
LONDON, ON- Strokes affect approximately 400,000 Canadians each year and can be debilitating. They can negatively affect a person’s cognition and mobility, and severely impact mental health and wellbeing.
A team at Lawson Health Research Institute are looking to improve mental health treatments and resources for patients who have experienced a stroke. The team will recruit 100 stroke patients to assess whether the completion of a guided therapy program can improve mental health and quality of life.
“More than sixty per cent of patients experience depression after stroke,” says Dr. Robert Teasell, Lawson Scientist and Physiatrist at St. Joseph’s Health Care London’s Parkwood Institute. “Having a stroke itself makes people more vulnerable and makes people feel their lives have changed negatively.”
During stroke rehabilitation, patients are typically offered mental health treatments, but the research team say it is post rehabilitation that stroke patients tend to experience worsening depression.
“Publicly funded allied health care services are available at inpatient and outpatient care; however, psychology is often limited across the rehabilitation continuum from acute to community care,” says Dr. Swati Mehta, Lawson Scientist. “We are looking at how we can provide a program that is cost effective to help those who have these barriers to access mental health services.”
“Patients have described to me that they feel like they have been dropped off a cliff because of the lack of resources once their programs have ended,” adds Dr. Teasell.
The study will examine the use of cognitive behavioral therapy (CBT), which is an evidence based psychological intervention that aims to provide people with increased coping ability and self-efficacy. Participants will complete a 10-week guided program with specific targeted lessons, tailored to the needs of those post stroke, delivered virtually through a trained clinician. They will then complete a questionnaire to see if there have been any improvements to self-efficacy and emotional wellbeing.
“We have found this form of therapy (CBT) has been very effective and feasible for spinal cord injury patients with mild traumatic brain injury and we want to see how a modified version could potentially help those with stroke and depression,” says Randy Upper, Clinical Research Associate at Lawson.
If CBT is proven effective through this study, Dr. Mehta hopes it will encourage similar programming that would be available to stroke patients after rehab.
“We are hoping we can connect with community organizations and work with them to implement this program in a service delivery model that would be easily accessible for stroke patients living in the community.”
Recruitment for this study is currently underway, those interested in taking part can email Dr. Swati Mehta at: @email
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Improving recovery and rehabilitation for patients with mental illness
Over 130 hospital-based clinical, administrative and research staff members, persons with lived experience of mental illness, family caregivers, peer and community supporters, and staff from local community mental health agencies attended the 18th Annual Mental Health Research & Innovation Half Day on November 1, 2017. The event provided an opportunity to learn more about mental health research at Parkwood Institute and the Southwest Centre for Forensic Mental Health Care (Southwest Centre), part of the St. Joseph’s Health Care London (St. Joseph’s) family.
“This year’s Mental Health Research and Innovation Half Day was one of the best attended in our history of hosting the event. We had a very diverse and engaged audience with great energy and a lot of enthusiasm,” says Dr. Arlene MacDougall, Director of Research and Innovation for mental health care at St. Joseph’s and Lawson Health Research Institute (Lawson).
Exciting recent projects were showcased though talks highlighting excellence in recovery and rehabilitation research, the theme of this year’s event; poster presentations; the 13th Annual Tony Cerenzia Research Lecture delivered by Dr. Sean Kidd; and interactive workshop sessions.

“We chose ‘recovery and rehabilitation’ as the theme for the event because it is so important in our clinical care and research programs to have this focus. We need to prioritize the development, implementation and evaluation of practices and interventions that foster recovery of the whole person experiencing mental illness, which includes their psychological, social and other needs that go beyond traditional notions of healthcare,” Dr. MacDougall adds.
13th Annual Tony Cerenzia Research Lecture
Guest speaker Dr. Kidd’s talk – “From clinical trials to the clinic: A story about making Cognitive Adaptation Training for schizophrenia more accessible” – focused on how to implement interventions proven in clinical trials. Dr. Kidd is a clinical psychologist, senior scientist and psychology division chief at the Centre for Addiction and Mental Health (CAMH) in Toronto. He is also an associate professor in the Department of Psychiatry at the University of Toronto.

Above: Dr. Sean Kidd's lecture focused on implementing interventions proven in clinical trials.
Workshop Sessions
Following Dr. Kidd’s lecture, attendees had the opportunity to participate in one of six workshops on a variety of topics related to recovery and rehabilitation focused mental health research:
“Implementing Interventions: A facilitated conversation attending to evidence, strategy, and recovery oriented care”
Led by Dr. Sean Kidd
Participants shared successful strategies for implementing novel approaches to care and discussed the challenges involved. They also looked at ways to leverage technology and education materials.
“Spirituality in Mental Health Care: Practically Supporting Recovery and Wellness”
Led by Stephen Yeo, Lawson allied scientist and chaplain, Southwest Centre; and Dr. Clark Heard and Jared Scott, Lawson associate scientists and occupational therapists, Southwest Centre
This workshop focused on the practical application of spirituality within the clinical setting, including the use of labyrinths, which contribute to recovery by promoting spiritual self-care, insight development and personal meaning-making reflection. Attendees had the opportunity to participate in a labyrinth walk and a related spiritual reflection. Read more about the labyrinths at Parkwood Institute and the Southwest Centre or watch the following video featuring highlights from the workshop:
“Indigenous Men’s Health and Wellbeing: Connection with Culture as a Rehabilitation and Recovery Tool”
Led by Bill Hill, social worker, Parkwood Institute and Dr. Vicki Smye, associate professor, director of nursing at Western University
Through the sharing of practitioner experience and Indigenous men’s voices, the workshop focused on understanding the powerful links between connection to culture and mental health and well-being (pictured below).

“Engaging Service Users and their Families in Research”
Led by Dr. Cheryl Forchuk, The Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, Lawson; and Deborrah Sherman, executive director, Ontario Peer Development Initiative
Participants in this workshop discussed the benefits of patient and family involvement in mental health research and identified strategies to support patient and family engagement (pictured below).

“Innovation in Mental Health Care: Moving Ideas to Impact”
Led by Kaitlin Saxton, research and innovation facilitator, Parkwood Institute; and Lisa Bitcola, centre manager of projects and operations, Ivey International Centre for Health Innovation
This workshop focused on how innovation relates to research and quality improvement initiatives within St. Joseph’s Mental Health Care facilities. Participants discussed innovative approaches that could be implemented within their own clinical practice, research and quality improvement initiatives (pictured below).

“My Professional Practice: Where's the Research?”
Led by Amanda Thibeault, director, professional practice, St. Joseph’s
In this session, participants discussed how they can incorporate research into their clinical practice (pictured below).

Latest findings on gait and dementia available to public through open access
September is World Alzheimer’s Month and Saturday, September 21 was World Alzheimer’s Day.
In recognition, the Journal of Alzheimer’s Disease has published an open access, special issue that will be available to everyone for the first two weeks of publication.
Dr. Manuel Montero-Odasso, Scientist at Lawson Health Research Institute, has edited and led the special issue focusing on gait disorders and dementia.
He is world renowned for his findings on the relationship between cognition and mobility in the elderly, and gait as a predictor of frailty and dementia. He leads the Mobility, Exercise and Cognition (MEC) Team in London, comprised of top researchers in the areas of mobility, exercise and brain health.

Dr. Montero-Odasso is also a professor at Western University’s Schulich Medicine & Dentistry, geriatrician at St. Joseph’s Health Care London and London Health Sciences Centre, and Director of the Gait and Brain Lab, a part of Lawson’s Parkwood Institute Research group.
“This Journal of Alzheimer’s Disease supplemental issue showcases studies presenting the epidemiology of gait disturbances and cognitive impairment, dissecting specific associations between cognitive domains and quantitative gait parameters, and addressing with advanced neuroimaging techniques the potential mechanisms underlying the gait-cognitive interaction seen before dementia,” explains Dr. Montero-Odasso. “Also, this issue highlights how to manage mobility impairment in the cognitive impaired by using assistive devices.”
Alzheimer’s disease is an irreversible, progressive brain disorder that slowly destroys memory and thinking skills. It is the most common cause of dementia among older adults. There are over half a million Canadians living with dementia - plus about 25,000 new cases diagnosed every year. By 2031, that number is expected to rise to 937,000, an increase of 66 per cent.
Read the Gait Disorders Special Issue with editorial from Drs. Montero-Odasso and George Perry entitled “Gait Disorders in Alzheimer’s Disease and Other Dementias: There is Something in the Way You Walk.”