Search
Search
“Cook your Wash” campaign reduces risk of HIV transmission
In June 2016, a public health emergency was declared in London, Ontario when HIV rates amongst injection drug users more than doubled.
What was abnormal about the emergency in London? The outbreak occurred despite London having Canada’s largest per capita sterile needle and syringe distribution program, a strong opiate substitution therapy program and a multidisciplinary HIV clinic. Many locations with outbreaks in HIV among persons who inject drugs implement these interventions to lower rates of transmission, but they already existed in London.
Researchers at Lawson Health Research Institute and Western University recognized there must have been a novel method of HIV transmission and looked to find a solution.
In two new studies published in the Journal of Acquired Immune Deficiency Syndrome (JAIDS), the research team found for the first time that HIV can be transmitted through sharing of equipment used to prepare drugs before injection and that a simple intervention - heating the equipment with a cigarette lighter for 10 seconds – can destroy the HIV virus, preventing the transmission.
From August 2016 to June 2017, the research team interviewed 119 injection drug users to understand their injection behaviours and risk for HIV. They discovered that those who shared equipment used to prepare drugs for injection were 22 times more likely to contract HIV than those who did not, despite not sharing needles or syringes.
The equipment includes a metal ‘cooker’ used to dissolve drugs in water and a filter used to draw the mixture, known as ‘the wash,’ into the syringe. Injection drug users reported reusing the equipment when consuming controlled-release hydromorphone, one of the most commonly injected opioids.
“Controlled-release hydromorphone is expensive and difficult to dissolve. After the first wash, large amounts of the drug remain in the equipment which is then saved, shared or sold for future use,” explains Dr. Sharon Koivu, Associate Scientist at Lawson and Associate Professor at Schulich Medicine & Dentistry. “While people know not to share needles, some use their own needle multiple times allowing for contamination of the equipment.”
The team took their findings back to the research laboratory. They confirmed that, on average, 45 per cent of the drug remains in the equipment after the first wash. They not only confirmed the HIV virus can be transmitted between needles, cookers and filters, but also discovered that controlled-release hydromorphone has properties that promote survival of the virus.
“The slow release properties in the drug can unfortunately stabilize the HIV virus,” says Eric Arts, PhD, Chair of the Department of Microbiology and Immunology at Schulich Medicine & Dentistry. “For the first time, we were able to demonstrate that sharing equipment could lead to the type of HIV outbreak we observed in the community.”
The team discovered that when the cooker is heated with a cigarette lighter for approximately 10 seconds, or until the wash bubbles, the virus is destroyed. They termed the technique ‘cook your wash.’
The team also confirmed that heating the cooker did not impact drug concentration.
“We had to make sure that cooking your wash would not change the amount of drug being drawn into the syringe,” notes Dr. Michael Silverman, Lawson Associate Scientist and Chair/Chief of Infectious Diseases at the Schulich School of Medicine & Dentistry, Western University, London Health Sciences Centre and St. Joseph’s Health Care London. “If too much drug was released, it could lead to overdoses. If any drug was burnt off or lost, the intervention would not be accepted by persons who inject drugs.”
Partnering with local community organizations like the Middlesex-London Health Unit and Regional HIV/AIDS Connection, ‘Cook Your Wash’ was launched as a public health campaign.
“The ‘Cook Your Wash’ campaign is one of the most exciting things to happen in our community,” says Dr. Koivu. “We learned from persons who inject drugs, took that information to the lab to develop a solution and then brought that solution back to the community in record time.”
Dr. Silverman adds that local rates of new HIV cases fell dramatically after the introduction of the campaign. “It wasn’t the sole reason for the reduction in HIV rates as other interventions were also introduced, but the timing suggests it was part of the solution.”
The team hopes this research can be used to inform understanding and interventions in other centres facing HIV epidemics amongst persons who inject drugs.
“We hope our findings can be used to reduce the incidence of HIV transmissions even further and that, one day, society will be HIV free,” says Dr. Silverman.
The two studies, “Heating Injection Drug Preparation Equipment Used for Opioid Injection May Reduce HIV Transmission Associated with Sharing Equipment” and “Sharing of Injection Drug Preparation Equipment is Associated with HIV Infection: A Cross Sectional Study,” are published in the Journal of Acquired Immune Deficiency Syndrome (JAIDS).
2018 Scientist of the Year Award: Dr. Robert Teasell
Lawson scientist Dr. Robert Teasell is considered a global leader in neurorehabilitation research and has been instrumental in transforming clinical care in this area across Canada by ensuring that clinical practices are informed by the best available and up-to-date research evidence. In recognition of his accomplishments, he received the Scientist of the Year Award at the 2018 Lawson Impact Awards event this past spring.
Dr. Teasell leads the Collaboration of Rehabilitation Research Evidence (CORRE) research team at St. Joseph’s Health Care London’s Parkwood Institute. He is also the Medical Director of the Stroke Rehabilitation Unit at Parkwood Institute and has an active outpatient chronic pain practice.
He has led the development of three internationally renowned evidence-based reviews for stroke rehabilitation, brain injury and spinal cord injury, which are regarded as the three most comprehensive research syntheses in neurorehabilitation in the world. Dr. Teasell has advised and helped plan stroke care for all of Ontario’s 14 Local Health Integration Networks (LHINs) and six provincial healthcare systems. This is in addition to the many clinical guidelines and models of care he has helped develop and update.
Dr. Teasell also bridges the gap between research and clinical practice through collaborations between his research and clinical teams. His multidisciplinary Rehabilitation Knowledge to Action Project (REKAP) team received the 2014 Sandra Letton Quality Award for their quality improvement project designed to make Parkwood Institute a leader in stroke rehabilitation by improving care through implementation of best practices.
In addition to his neurorehabilitation research, Dr. Teasell has published extensively on chronic pain with a recent focus on the role of obsessive personality traits in determining chronic pain disability and coping abilities.
Drawing on his clinical and research expertise, Dr. Teasell has supervised many students and has been committed to developing the next generation of medical researchers.
“Dr. Teasell has been successful in a number of areas. Certainly in terms of publications and mentorship of students who have gone on and had very successful careers of their own. Despite a busy clinical schedule, he always makes a point of engaging with his research team every day. His staff and students really appreciate the opportunity to work with him,” says Dr. Cheryl Forchuk, Beryl and Richard Ivey Research Chair in Aging, Mental Health, Rehabilitation and Recovery, and Assistant Director, Lawson Health Research Institute.
Dr. Teasell has authored 335 peer-reviewed articles, as well as many other collaborative group peer-reviewed articles, book chapters, published abstracts, posters, presentations and monographs. He has also been the editor for 14 special journal editions and is on the editorial boards for Topics in Stroke Rehabilitation, Journal of Rehabilitation, and Pain Research and Management.
In 2016, he was invited to present the Ramon J. Hnatyshyn Lecture, the leading annual national stroke lecture at the Canadian Stroke Congress in Quebec City. In 2010, he received the Canadian Association of Physical Medicine and Rehabilitation Merit award for his many contributions to the field of physiatry. He was also awarded the Royal College of Physicians and Surgeons of Canada McLaughlin-Gallie Visiting Professor in 2012. This year he will be awarded the Post-Acute Stroke Award of Excellence from the American Congress of Rehabilitation Medicine and the National Stroke Association in the United States.
“I’ve received a lot of national and international awards but there’s nothing better than being recognized by your peers and particularly your peers in the city where you work. It’s been a nice acknowledgement of not just my work, but also the work by the whole research team and all the people who have supported me over the years,” says Dr. Teasell.
2018 Staff Award of Excellence: Sheila Fleming
Sheila Fleming, executive assistant to Dr. David Hill, scientific director of Lawson Health Research Institute, was the recipient of a Staff Award of Excellence at the 2018 Lawson Impact Awards event this past spring.
In addition to carrying out her administrative support functions for Dr. Hill – in itself a significant responsibility – Fleming goes above and beyond to provide support in a variety of ways to the entire Lawson administration team and research community.
Just one of the many examples of this is the key role she plays in the planning of Lawson’s annual signature events: London Health Research Day (LHRD), Lawson Impact Awards and Café Scientifiques.
Fleming has built strong relationships across Lawson and its hospital and academic partners. She often acts as a liaison connecting administrative team members to key senior leaders and researchers, and vice versa, so they are able to do their jobs more effectively.
“Sheila is the ‘hub’ of Lawson. Almost all of us on the administration team, and I’m sure many members of our research community, view Sheila as their go-to person. She has a wealth of knowledge that has guided many of us,” says Stacey Larizza, Chief Operating Officer, Lawson. “She always considers the needs of scientists, staff and trainees, and she is a passionate advocate for them. She does whatever she can to help ensure they succeed.”
Her relationship-building skills have also strengthened Dr. Hill’s advocacy efforts as Lawson continues to join research institutes across the country campaigning for increased funding, diversity in science and support for young researchers from the Canadian government.
“As a scientist it’s not just doing the research, it’s leading people; it’s really knowing how to run a business. So anyway I can help them jump those hurdles, I’m happy to do that,” says Fleming. “In my view, relationships drive everything and that’s how we get work done. If you’re fair and helpful and collaborative, people will respond in kind and then it’s easy to move things forward.”
Fleming also participates in a number of volunteer initiatives. For example, she is President of the Ingersoll District Nature Club, a group that stewards the 36 acre Lawson Nature Reserve south of Ingersoll; helps lead local advocacy efforts in opposing a proposed mega landfill adjacent to Ingersoll aquifers; and provides administrative support to the Diabetic Pregnancy Study Group, a European not-for-profit organization that fosters research and education in diabetic pregnancy.
A “safety net of relationships” to bridge the gap between hospital and community at discharge
A beneficial and cost-effective approach to mental health care that supports people as they go from hospital and back into the community is outlined in a new resource and has been recognized internationally by the World Health Organization (WHO).
"The immediate period after discharge from hospital, usually the first month, can be one of the most vulnerable times in the life of someone experiencing a mental illness. It can be when they are most at risk of committing suicide,” explains Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson Health Research Institute. “However, what we’ve seen is that there’s often a gap between when someone says ‘goodbye’ to the hospital inpatient unit and ‘hello’ to the community care provider.”
During a virtual book launch, a research team from Lawson and several community organizations discussed details of a new publication from Routledge, From Therapeutic Relationships to Transitional Care: A Theoretical and Practical Roadmap, edited by Dr. Forchuk. The book combines theory, research and best practices into a “roadmap” for organizations and others worldwide coordinating services or studying mental health care systems. It includes a practical toolkit for implementing the Transitional Discharge Model (TDM), developed and tested in communities across Ontario.
Purchase your copy of the book HERE and enter promo code SMAO3 at checkout for a 20% discount.

How Transitional Discharge works
TDM was born from a participatory action project with consumers of mental health services. They identified two factors that were most important to them when they were going from hospital to the community: consistency in therapeutic relationships and a supportive peer friendship.
It became known as a “safety net of relationships” that would bridge the gap between hospital and community services.
As a person-centred, evidence-based model, transitional discharge supports a smooth adjustment from hospital to community in two main ways:
- The inpatient staff continue to care for discharged clients until therapeutic relationships are established with community care providers.
- A friendship model of support with trained peer support workers who have lived experience of mental illness as they have made the same journey.

Perspective of a TDM client and peer support coach
Lance Dingman was a TDM client during the early phases of the project. “It makes a big difference when you’re able to get back to living in the community and in your own dwelling. You get to make more of your own decisions and learn about what you want to do. You grow with your experience and the guidance of others who are there to support you.”
Later becoming a peer support coach, Dingman feels implementing TDM for mental health care is important because people can learn from each other and get healthier in the process. “As a peer support worker, I sit with people and they tell me their story. It takes me back and I know what they are going through – I was where they are. I can share my own story and tell them what I did to get better.”
Cost-analysis and savings for the system
Dr. Forchuk’s team analyzed the cost of TDM after being tested in nine hospitals across Ontario, including London Health Sciences Centre and St. Joseph’s Health Care London.
- On average, the length of stay in hospital was reduced by almost 10 (9.8) days per admission.
- Each site saved approximately $3.3 million per year.
“People can return home sooner because a higher level of care and support is in place when they leave hospital. If all hospitals in Ontario with mental health services were able to implement our transitional discharge model, we would save $60 million per year in hospital stay costs alone while providing enhanced mental health care.”
International implementation
In Scotland, the parliament has already declared TDM as a best practice after demonstrating a significant reduction in readmission rates.
The TDM approach is now considered a “good practice” by WHO and was recently the only Canadian example included in its Guidance on community mental health services: Promoting person-centered and rights-based approaches. This set of publications provides information and support to all stakeholders who wish to develop or transform their mental health system and services to align with international human rights standards including the UN Convention on the Rights of Persons with Disabilities.
Café Scientifique: The invisible world inside us
The human microbiome is a wonder of nature, with trillions of microbes calling our body home. They live in our gut and many other places throughout our body. They are involved in virtually every aspect of how we function and we are learning that they are essential to staying healthy. An unhealthy microbiome has been linked to many diseases from allergies to cancer and even mental health.
Most people out there have heard about probiotics and fermented foods, and chances are you’re trying to get more of them in your diet. Drinking kombucha or eating yogurt, anyone?
On November 27, 2019, Lawson Health Research Institute held the latest in its Café Scientifique event series, "The invisible world inside us: Exploring the human microbiome.”
The panel of researchers helped to unravel the mysteries about the micirobiome and how we are using that knowledge to improve health and health care. They also busted some myths and shared the important facts when it comes to probiotics, prebiotics and the microbiome.
Watch their talks:
Researchers:
Probiotics and Prebiotics - Look beyond the fake news
Dr. Gregor Reid, Lawson Scientist and Professor of Microbiology & Immunology and Surgery at Western University.
Time stamp: 10:02
Fecal Transplants: What does this crap have to do with me?
Dr. Michael Silverman, Lawson Associate Scientist, Chair of Infectious Diseases, Schulich School of Medicine & Dentistry at Western University and Chief of Infectious Diseases for St. Joseph’s Health Care London and London Health Sciences Centre.
Time stamp: 31:48
Does eating bacteria make sense?
Dr. Jeremy Burton, Lawson Scientist and Assistant Professor of Surgery (Urology) and Microbiology & Immunology at Western University.
Time stamp: 55:02
See the event photos on Facebook.
Celebrating International Day of Women and Girls in Science
To mark International Day of Women and Girls in Science, Dr. Michelle Barton-Forbes, Associate Scientist at Lawson Health Research Institute and Division Head of Infectious Diseases at Children’s Hospital at London Health Sciences Centre (LHSC), shares her journey and advice for young women who are considering a career in science, technology, engineering and math (STEM).
“As a child I had a curious mind and I was always asking questions, wanting to figure out how things worked. As I got older, I also wanted to know how we could make things better,” she says. “I found a love for math and that had me wanting to solve puzzles and understand statistics from an early age.”
Dr. Barton-Forbes also loved chemistry and considered engineering, but says she was a people person. After spending some time in hospital interacting with doctors and nurses, she decided medicine would be the best way to combine her love of science and helping people.
Today she is using her love of math and science in her work at LHSC.
Growing up in Jamaica she saw first-hand the impact of infectious diseases on children in the developing world, where immunizations like those to prevent bacterial meningitis had not yet been introduced. Now her research focus is on infections in vulnerable patients such as neonates, including congenital and perinatal infections like cytomegalovirus and herpes, preventable diseases like COVID-19 in children, and studies in the Black community that address natural and vaccine immune responses to COVID-19. In her role as Chair of the Canadian Paediatric Society’s Infectious Disease and Immunization Committee, she also contributes to the development of national guidelines addressing treatment and prevention of infections in children.
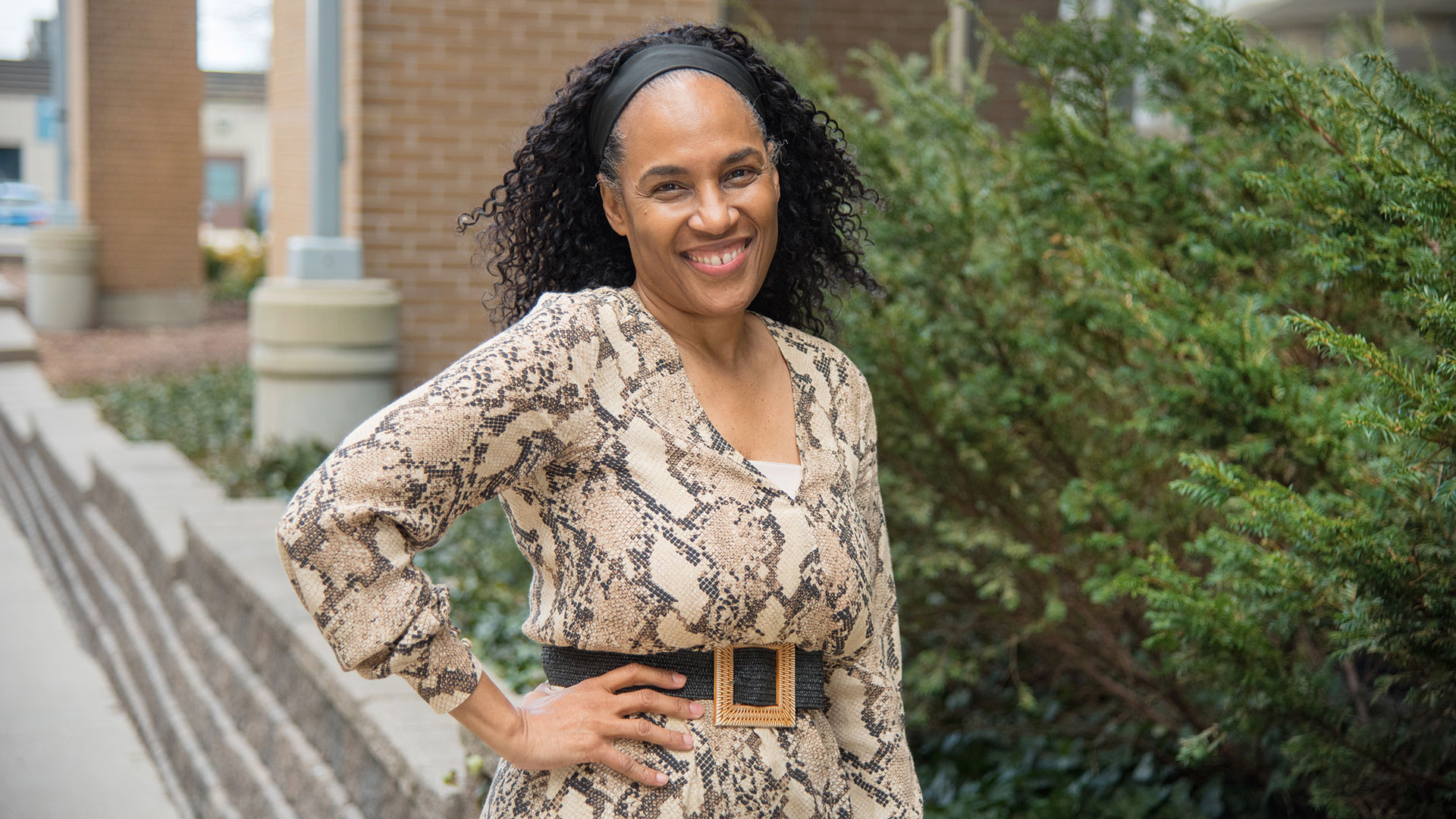
Having women in science is about equity, but also about efficiency says Dr. Barton-Forbes.
“There should be more interest in advancing more women in STEM, otherwise we aren’t maximizing on the talents and capabilities of a significant proportion of our population,” she notes.
Dr. Barton-Forbes points out that women bring unique perspectives to research. While she believes that women already in STEM are crucial in encouraging the younger generation by sharing their energy and passion, more needs to be done.
“I think the approach has to be not just at an individual level, but also at the institutional, national and global level to try to promote interest in STEM,” Dr. Barton-Forbes says.
More STEM programs, starting at the elementary school level, as well as targeted prizes, awards and scholarships are essential, she says, as well as removing additional barriers for equity-deserving populations.
“When we speak about women in science, I think there has to be a greater intentional effort to ensure that ethnic minorities are included and supported.”
And young women need to see representation at the highest levels of leadership as well, she says.
“We need more role models that can encourage at all levels, and we need programs that are deliberate in creating opportunities that improve access and ensure mentorship.”
When asked about advice for women starting a career in science, Dr. Barton-Forbes offers the following:
- Connect to a community of mentors to share ideas and find a sponsor or coach.
- Believe in yourself. Don’t second guess your ability.
- Capitalize on conferences and networks to keep up-to-date on new opportunities.
- Don’t be afraid to stand out and ask questions.
Reflecting on her own journey as a woman in science, Dr. Barton-Forbes is proud of her work.
“The research I do explores risk factors and outcomes, allowing us to identify those most likely to get a disease and predict those likely to do poorly. This helps us target our treatment and prevention to those most in need and therefore make a bigger difference. I get to see the impact of my research on children’s lives. This brings me the greatest joy because it means I am changing their trajectory and improving outcomes. Not only that, I can identify who is at risk and help prevent it from happening.”
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Controlled-release opioid may be leading to heart infections in persons who inject drugs
A new study from ICES, Lawson Health Research Institute and Western University suggests that injection drug users prescribed controlled-release hydromorphone are three times more likely to develop endocarditis, a serious bacterial heart infection, when compared to those prescribed other opioids. The findings build on growing evidence that some controlled-release opioids may lead to higher risk of infectious disease among persons who inject drugs.
The researchers looked at de-identified Ontario health data for hospital admissions related to injection drug use between 2006 and 2015. Of 60,529 admissions, 733 patients had infective endocarditis. The team found that regions with high hydromorphone prescription rates had more than double the cases of infective endocarditis (254 cases) when compared to regions with low prescription rates (113 cases).
The study also analyzed individual prescription records and found that among persons who inject drugs, those prescribed controlled-release hydromorphone were three times more likely to develop infective endocarditis when compared to those prescribed any other opioid. There was no increased risk for those prescribed the immediate-release form of hydromorphone.

“Added to the existing data, these findings make a compelling argument for the role of controlled-release hydromorphone in the growing risk of infective endocarditis among persons who inject drugs,” says Dr. Matthew Weir, Adjunct Scientist at ICES, Associate Scientist at Lawson and Assistant Professor at Western’s Schulich School of Medicine & Dentistry.
Opioids are often manufactured as controlled-release or ‘slow-release’ capsules to prevent rapid absorption of the drug. Properties in the capsules help to spread pain relief over a longer period of time.
This is the latest in a series of studies from the research team that suggest some controlled-release opioids may be leading to increased risk of infectious disease among persons who inject drugs.
In one study, they demonstrated that polymer-coated beads used to provide the slow-release property make controlled-release hydromorphone difficult to dissolve. They found equipment used to dissolve the drug retains up to 45 per cent of the initial dose, leading injection drugs users to save and reuse equipment.
With frequent re-handling of equipment, there are multiple opportunities for bacterial and viral contamination. The team found that HIV and a dangerous bacterium called Staphylococcus aureus are more likely to survive in equipment used to prepare controlled-release hydromorphone since added chemicals that make the drug slow-release promote survival of bacteria and viruses.

“There’s been a global increase in infectious diseases among persons who inject drugs and our research suggests that controlled-release prescription opioids may be a major culprit,” says Dr. Michael Silverman, Associate Scientist at Lawson and Associate Professor at Schulich Medicine & Dentistry. “We now have evidence that suggests the injection of controlled-release hydromorphone is increasing the spread of HIV, hepatitis C and endocarditis in Canada.”
The team believes these findings could also explain the increase in infectious complications in the USA and other countries where controlled-release hydromorphone is not on the market. There are other controlled-release opioids, such as controlled-release morphine, that use a similar slow-release mechanism and may carry similar risks.
“It’s important that people are aware of the infectious risks of injecting opioids and, if necessary, practice harm reduction techniques,” says Dr. Silverman. “We’ve found you can use a cigarette lighter to destroy bacteria and viruses by heating the cooker used to prepare the drug for about 10 seconds or until the mixture bubbles. We’ve termed the technique ‘cook your wash.’”
The study, "Hydromorphone and the risk of infective endocarditis among people who inject drugs: a population-based, retrospective cohort study," was published in The Lancet Infectious Diseases.
Dr. Manuel Montero-Odasso named as one of most influential Hispanic Canadians
Dr. Manuel Montero-Odasso, Clinician Scientist at Lawson Health Research Institute and Director of the Gait and Brain Lab, has been named as one of the 10 most influential Hispanic Canadians for 2019. Presented by TD Bank, those on the list were honoured at an awards ceremony in Toronto, Ontario in November.
A geriatrician at St. Joseph’s Health Care London, Dr. Montero-Odasso is recognized as a world expert in dementia and gait disorders. The main focus of his research is on the interaction of mobility and cognitive decline in aging. He is the team leader for the Canadian Consortium on Neurodegeneration in Aging (CCNA), a collaborative research program advancing dementia research, and leads the Mobility, Exercise and Cognition (MEC) Team in London, comprised of top researchers in the area of mobility, exercise and brain health.
Dr. Montero-Odasso says that one aspect of his career that he is most proud of is being able to collaborate with other researchers in his field and “contribute to new approaches to combat mobility and cognitive decline in aging.” This is evident through the clinical trials he pioneered by implementing an approach of “improving cognition to improve mobility.”
TD Bank’s “10 Most Influential Hispanic Canadians” is awarded to individuals from the Hispanic community across Canada to recognize their outstanding achievements. Dr. Montero-Odasso’s influence is displayed on a global scale as he has received over 100 invitations to give international lectures and has published over 200 manuscripts and book chapters. He has a close relationship with the Spanish-speaking community and has hosted visiting scientists from Argentina and Spain.
“I feel honoured and privileged, particularly this kind of award where you are nominated by your peers. I am also glad my work is reflecting the role that my Hispanic background plays,” says Dr. Montero-Odasso, who is also a professor of Medicine, Epidemiology, and Biostatistics at Western University. “Additionally when you look at the other nominees, and those who have received the award in the past, it really gives you a sense of the amazing things Hispanics who live and work in this country are contributing to Canadian society.”
Dr. Montero-Odasso emphasizes the value of diversity and learning from different backgrounds when seeking solutions. As he continues working in this important field as a physician and researcher, Dr. Montero-Odasso’s goal is to, “find effective ways to treat and delay aging disability in order to add, as they say, life to the years, and not only years to the life.”
Expanding transitional support for young adults with diabetes
In 2012, researchers from across Ontario, led by a team at Lawson Health Research Institute, started the first multicenter randomized controlled trial to evaluate implementation of a transition coordinator for young adults with type 1 diabetes as they transferred from paediatric to adult care.
“There is a huge difference between the kind of care that they receive as children compared to adults, and that is consistent across Canada and most other countries,” explains Dr. Cheril Clarson, associate scientist at Children’s Health Research Institute, a program of Lawson, and a paediatric endocrinologist at Children’s Hospital, London Health Sciences Centre.
With children, patient visits involve a variety of specialists from different areas, such as the physician, nurse educator, dietitian and social worker. “The naturally build up a long-term relationship with the team, as some children might start the program when they are 2 or 3 years old as an example.” Dr. Clarson adds that the child’s caregivers are an integral part of the process and the care team also gets to know them very well.
Moving into the adult program means that the patient now has more responsibility and autonomy over their own care. They have to remember to go to appointments, fill prescriptions and maintain their daily diabetes care.
“During the emerging adulthood period, your attention is taken up by many other things – leaving home, starting post-secondary education, figuring out your identity and independence,” says Dr. Tamara Spaic, Lawson associate scientist and adult endocrinologist at St. Joseph’s Health Care London. “And on top of that they need to manage their diabetes every day. They are in a completely new system with a new care team – it’s a major transition. For many, they stop coming to appointments regularly and they don’t keep up with all of their own care.”
As young adults struggle to find their footing in a new system, there are significant short and long-term consequences when it comes to their health. Some will experience acute complications like high sugars leading to diabetic ketoacidosis and hospital admission or severe low blood sugars where they can lose consciousness and have a seizure.
“Different studies show between 30 to 60 per cent increased risk of complications like retinopathy, myocardial infraction, stroke and kidney disease in those who do not follow their care plan,” notes Dr. Spaic. “We see a bump in this young adult period where levels spike and their diabetes isn’t being controlled – this has impacts for both the individual and the system.”
The study enrolled 205 young adults with type 1 diabetes between the ages of 17 and 20. Patients were recruited from three paediatric centres and their care was transitioned to three adult centres. The multi-centre partnership included Children’s Hospital; St. Joseph’s; Children’s Hospital of Eastern Ontario; The Ottawa Hospital; and, Trillium Health Partners in Mississauga.
Participants were randomly assigned to two groups, with 104 patients in the structured transition program and 101 patients receiving standard care. Patients were seen in the paediatric care setting for six months and then transferred to adult care, where they continued with either the transition program or standard care for one year.
The core component of the program was a transition coordinator, a nurse who is a certified diabetes educator. The coordinator followed the young adults throughout the transition, interacting with the paediatric health care team to establish a base of support as they moved into adult care. They attended visits, established appropriate contacts for the patient, provided support for diabetic care, problem solved and helped navigate the system. In addition to face-to-face meetings, they were available via text messages, emails and phones calls.
“We had a high recruitment rate for the population and type of study, and a high number of participants followed the full program,” says Dr. Clarson. “Our results at the end of the intervention showed that the program worked very well. By providing additional support through a transitional coordinator, the results showed better outcomes all around.”
Compared to the baseline, study participants attended more care visits, were more satisfied with their care, suffered much less distress associated with diabetes, had better management on a daily basis and reported less emotional burden of diabetes.
The team then took it a step further and spent another year following the participants to see if they were able to sustain the behaviour and positive outcomes. They did not find a difference between the control and intervention groups.
“Unfortunately, we found no difference in the number of visits they attended, their satisfaction with care and management of their diabetes,” explains Dr. Spaic. “When they didn’t have the intervention, they essentially went back to baseline. Out hope is to see the program extended.”
Dr. Clarson adds that they developed the program so that it can be integrated in different ways, and also in difference areas of health care beyond diabetes. For example, they found that the preferred method of communication with the coordinator was text. This is an easy way to provide the fundamental support of a coordinator for longer, and it is cost-effective.
“Our patients really loved the intervention. By the end of the study, they felt more comfortable being able to navigate the adult health care system. They felt empowered and responded well. They wanted to continue the program.” The next step for the researchers is to evaluate support through a virtual transition coordinator.
“Closing the Gap: Results of the Multicenter Canadian Randomized Controlled Trial of Structured Transition in Young Adults With Type 1 Diabetes” was recently published in the journal Diabetes Care by the American Diabetes Association.
Learn more about the study and read about Nicole Pelcz, study participant, who found out at 13 years old that she had type 1 diabetes.
In the media:
Diabetic teens fall back to old habits after transition care, study says – London Free Press
Fecal transplants show promise as treatment for non-alcoholic fatty liver disease
A new study from Lawson Health Research Institute and Western University suggests that fecal transplants could be used as a treatment for non-alcoholic fatty liver disease (NAFLD). The randomized controlled trial published in The American Journal of Gastroenterology found that fecal transplants in patients with NAFLD result in a reduction in how easily pathogens and other unwanted molecules pass through the human gut and into circulation, known as intestinal permeability. The results could have implications for the treatment of numerous conditions including metabolic syndrome and autoimmune diseases.
“Intestinal permeability plays a role in the development of metabolic syndrome which is a major cause of coronary and cerebrovascular disease. It has also been associated with autoimmune diseases like multiple sclerosis (MS), rheumatoid arthritis, systemic lupus and type 1 diabetes,” explains Dr. Michael Silverman, Associate Scientist at Lawson and Professor at Western’s Schulich School of Medicine & Dentistry.
Many NAFLD patients have increased intestinal permeability which triggers inflammation, increased fat in the liver, insulin resistance and elevated levels of triglycerides in the blood. The human microbiome – the diverse collection of microbes in our body – is thought to play a role. Previous studies have shown differences between the gut microbiome of NAFLD patients compared to healthy individuals.

“Our team wondered whether we could change the gut microbiome of NAFLD patients to reduce intestinal permeability,” says Dr. Jeremy Burton, Lawson Scientist and Associate Professor at Schulich Medicine & Dentistry.
The trial included 21 NAFLD patients from London Health Sciences Centre (LHSC) and St. Joseph’s Health Care London. Patients were randomized to receive a fecal transplant using stool from a healthy donor or a placebo (the patient’s own stool). Fecal material was delivered to the small intestine using endoscopy. Patients were followed for six months to assess changes to their gut microbiome, intestinal permeability, percentage of liver fat and insulin resistance.
While the researchers found no changes in percentage of liver fat or insulin resistance, they observed significant reduction in intestinal permeability in those patients who had elevated intestinal permeability at the study’s start (seven patients in total). They also observed changes to the gut microbiome in all patients who received a fecal transplant from a healthy donor.
“Our study demonstrates that intestinal permeability can be improved through fecal transplant from a healthy donor,” says Dr. Laura Craven, a recent PhD graduate from Schulich Medicine & Dentistry and first author on the published study. “This suggests that fecal transplant could be used as an early intervention in the treatment of NAFLD to reduce intestinal permeability and prevent inflammation”

Dr. Laura Craven
“Our findings have implications for other conditions too,” adds Dr. Silverman, who is also Chair/Chief of Infectious Diseases at Western, LHSC and St. Joseph’s. “Changing the gut microbiome could hold promise in preventing and treating metabolic syndrome and autoimmune diseases associated with increased gut permeability.”
The team hopes to next conduct a large multi-centre trial to further investigate FMT as an intervention for NAFLD and as a therapy to reduce intestinal permeability.
NAFLD is an obesity-related disorder and is the second-leading cause of liver transplant in North America. While reversible if treated early, its progression can lead to liver failure or cancer. Current therapies are not overly effective and the prevalence of NAFLD is increasing.
Dr. Silverman is a pioneer in the field of fecal transplants, including their use as a treatment for Clostridioides difficile (C. diff). He is involved in multiple studies examining the potential of fecal transplants as treatments or supportive therapies for numerous conditions including multiple sclerosis (MS) and different types of cancer.
“In order to conduct this research, we need stool donors,” notes Dr. Silverman. “By donating your poop, you can help us assess the value of fecal transplants to treat a variety of diseases.”
The team is in need of young, healthy stool donors for fecal transplants. All donors are required to go through a screening process. Those interested in becoming a stool donor can contact Dr. Seema Nair Parvathy, Research Coordinator, Fecal Transplant Program, at 519-646-6100 ext. 61726.

Drs. Michael Silverman (left) and Jeremy Burton (right)
First clinical guidelines in Canada for pain following spinal cord injury
Researchers at Lawson Health Research Institute are the first in Canada to develop clinical practice guidelines for managing neuropathic pain with patients who have experienced a spinal cord injury (SCI).
Neuropathic pain is complex and chronic, and is the most common complication reported by people following SCI. The research team worked with care providers at Parkwood Institute, part of the St. Joseph’s Health Care London family, and an international panel to address the complex and unique challenges for managing pain during recovery and rehabilitation.
In 2003, Dan Harvey sustained a spinal injury after falling off a trampoline. Using his personal experience, as well as his experiences meeting with newly injured people, Harvey contributed to the development of the new guidelines.
“Neuropathic pain – and pain in general – affects every person with a spinal cord injury very differently. Some people have it, some people don’t. But for those who do have it, it can make rehabilitation and recovery much more difficult,” explains Harvey.
“On top of just learning how to use your body again, you also have to deal with various forms of physical pains, which can make it challenging to mentally adapt to an injury.”
For those with chronic pain, it may be hard to just get out of bed in the morning, feel well enough to leave the house, or even fall asleep. “I have fairly extensive neuropathic pain, so I’m well aware of how difficult it can be to get a full night’s sleep, or show attentiveness at work or at school when it literally feels like your legs are on fire,” says Harvey.

Dan Harvey with Lawson researchers Stacey Guy, Swati Mehta and Dr. Eldon Loh.
Dr. Eldon Loh, Lawson Researcher and Physical Medicine and Rehabilitation Specialist at St. Joseph’s, and his team recognized that pain can be an overlooked part of a spinal cord injury and plays a major factor in the success of rehabilitation. It’s difficult for someone in pain to participate fully in their own recovery, and so long-term disability becomes more likely. Pain is difficult to manage and it often takes multiple approaches to find something that works for each person.
“This is a starting point for us to standardize how we approach pain in the clinic. We have identified gaps and offered recommendations to not only manage the pain, but also ensure that our patients can fully benefit from rehabilitation,” says Dr. Loh.
The results of the three-year process led to recommendations for screening and diagnosis, treatment and models of care. Important clinical considerations accompany each recommendation.
“For those in hospital following an injury, it’s about making sure they can be as independent as possible before discharge. Over time, we want to keep pain levels under control so that they are able to live life to the fullest,” adds Dr. Loh.
The research will inform new tools and resources for care providers and patients.
Harvey believes the guidelines will have a tremendous impact for patients whose pain may have been overlooked. “Pain can be created through many different avenues and the effects can snowball after a person is discharged and sent home. If you don’t check all of the boxes, you might be missing a very important item.”
The new guidelines have been published in the international journal Spinal Cord. The Ontario Neurotrauma Foundation and Rick Hansen Institute provided funding for the research study.
A special thanks to individuals from St. Joseph's who were involved in the project: Steve Orenczuk, Patrick Potter, Keith Sequiera, Lindsey Guilbault, Robert Teasell, Anna Kras-Dupuis, Dalton Wolfe, Alba Casalino and Dwight Moulin.

Additional members of the panel that developed the new clinical practice guidelines.
Happy Holidays from Lawson Health Research Institute
As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, Lawson Health Research Institute excels in rapid response research. We are uniquely positioned to tackle health challenges from within hospital walls.
With the COVID-19 pandemic proving to be one of the most pressing health challenges of our time, 2020 has shone a light on the critical importance of hospital-based research.
We would like to acknowledge the tremendous efforts of Lawson staff, researchers, learners and volunteers during a difficult year. Their remarkable knowledge, creativity and dedication never fails to astound. We also thank those who support health research in many different ways, including donations, study funding, and participation in clinical research.
This year, Lawson has again ranked eighth in the country according to the 2020 edition of “Canada’s Top 40 Research Hospitals List” by Re$earch Infosource, keeping us within the top five in Ontario. We have maintained this position for the past seven years. Here you will find a compilation of Lawson’s top 12 research stories from the past year. We encourage you to share this with your friends and families as there is still much to celebrate in our community.
We wish you all the very best this holiday season.
ICES launches call for applications to its next faculty training cycle
The ICES Faculty Scholars Program has officially launched the call for applications to its fourth training cycle (2019-2021).
This two-year, part-time learning opportunity is open to Ontario-based academic researchers who are passionate about population health and health services research, and wish to obtain an appointment as an ICES Scientist,
The program was established at ICES Western in 2013 as part of its strong focus on supporting trainees and new investigators. By leveraging partnerships with other ICES sites and in conjunction with an interactive e-learning environment, faculty from different regions are able to fully participate in the ICES Faculty Scholars program.
Scholars will have access to:
- Training in the use of Ontario’s health administrative databases for research.
- Seminars on advanced methods relevant to population health research.
- Opportunities for collaboration with experts across the ICES network.
- Individual project mentorship and data analytic support to develop and complete one or more research studies using Ontario’s health administrative databases.
Hear from successful ICES Faculty Scholars:
“The methods of planning and completing an ICES project are unique. This program is the best possible way to demystify the process and produce high quality work from the outset. The amount of support is outstanding, so you have confidence that your work will be successful.”
Dr. Andrew Appleton, Assistant Professor, General Internal Medicine, Western University
“The Faculty Scholars Program is extremely well structured and run. The Program provides a positive and open learning environment for Scholars to ask questions and learn about the administrative and practical aspects pertaining to conducting research at ICES.”
Dr. James Crispo, Researcher, Health Sciences North Research Institute
Applications for the 2019–2021 program will be accepted until January 18, 2019. Any questions regarding the program, applications or eligibility can be directed to @email.
Go to the ICES website for more information on the ICES Faculty Scholars Program.
ICES is a not-for-profit research institute encompassing a community of research, data and clinical experts. With its growing network across the province, ICES researchers are able to access a vast and secure array of health-related data to evaluate health care delivery and outcomes. Learn more about ICES Western.
Lawson celebrates Canada 150
Canada’s 150th anniversary of Confederation is an opportunity to celebrate the impact of health research over the last 150 years. In recognition, Lawson has launched a Canada 150 website (www.lawsonresearch.ca/canada150) to celebrate our past, our present and to look forward to how Lawson research can shape the future of health care.
Lawson’s Canada 150 website will be updated through the rest of the year with new content, including your feedback and ideas about the future of health research. We’re asking “What does the next 150 years hold for health research and innovation in Canada?” You can provide your input here or send us your ideas by tweeting us. We’ll be sharing your feedback on the Canada 150 website and social media throughout the year.
On July 1, Lawson will also be appearing alongside our hospital and foundation partners in a special insert of the London Free Press. Additionally, if you are celebrating Canada 150 at London’s Sesquifest you can view Lawson’s Canada 150 banner in the Explore Tent on Talbot Street.
Lawson Impact Awards honours research excellence and innovation
On April 11, in a full room at the London Convention Centre, almost 350 guests celebrated the sixth annual Lawson Impact Awards. The event honours research that is making a difference both locally and globally, and recognizes the remarkable accomplishments of Lawson scientists, staff, trainees and partners.
“This event gives us the opportunity to reflect on the importance of the work we do here at Lawson, and how everyone’s contributions ultimately improve patient care,” says David Hill, Scientific Director, Lawson Health Research Institute. “Throughout the organization, individuals regularly go above and beyond to drive innovative new discoveries.”
This year’s Lawson Impact Award winners are:
• Dr. Guido Filler – Scientist of the Year Award
• Dr. Don Richardson – Innovation Award
• Dr. Sarah Morrow – Dr. Joseph Gilbert Research Contribution of the Year Award
• Saagar Walia – Staff Award of Excellence
• Laura Craven – Leadership Award for Fellows and Students
• Lawrence Yip – Leadership Award for Fellows and Students
• GE Healthcare – Industry Partner of the Year
• Breast Cancer Society of Canada – Community Partner of the Year Award (LHSF)
• Legate Personal Injury Lawyers – Community Partner of the Year Award (CHF)
• 3M Canada – Community Partner of the Year Award (SJHCF)
Two Children’s Health Research Institute (CHRI) award recipients were also recognized at the event. As a program of Lawson, CHRI awards a Scientist and Trainee of the Year annually, sponsored by the Children’s Health Foundation. CHRI’s 2019 award recipients are: Dr. Craig Campbell (CHRI Scientist of the Year), and Dr. Mohamed Gatie (CHRI Deb Comuzzi Trainee of the Year).
An engaging keynote was delivered by Dr. Dorin Comaniciu, Senior Vice President for Artificial Intelligence and Digital Innovation at Siemens Healthineers, titled “Artificial Intelligence for Health Care: The Road Ahead.” Dr. Comaniciu spoke about the wide application for artificial intelligence in health care, focusing on the fields of diagnostic imaging, image-guided therapy and personalized medicine. Sharing his own digital avatar, guests were treated to a glimpse of what the future of care will look like with the advancement of this technology.
If you attended the event, you are encouraged to complete this short survey. Your feedback is important in helping make improvements for next year’s event.
Visit the Lawson YouTube channel to watch videos highlighting each of the award recipients. To see photos from the event, visit Lawson’s Facebook album.
Major Ronald Miller's story
“I just wasn’t myself,” says Major Ronald Miller when reflecting on his experience with post-traumatic stress disorder (PTSD). “I could see a significant change in my personality that just wasn’t me.”
Major Miller first joined the Canadian Armed Forces in 1971 as a young infantry private in the 1st Battalion, The Royal Canadian Regiment and later became an Officer in the Royal Canadian Artillery, which included a tour in Germany during the Cold War.
After the Cold War, he reoriented his career towards peacekeeping which saw him deployed to seven different conflict zones. “It was during the Civil War in El Salvador in 1991 that I experienced a number of incidents that first triggered my PTSD,” explains Major Miller. “From that time forward the PTSD was always there but I suppressed it.”
It wasn’t until 2016 that Major Miller’s PTSD resurfaced. After retiring from the Canadian Armed Forces in 2008, he started working a number of contracts in support of the military.
“Over the years, I was exposed to the kind of death and destruction that can be rather difficult from a psychological standpoint. The older I got, the less I was able to suppress those experiences. In fall 2016, I was supporting a NATO military exercise in the UK when I began experiencing horrible nightmares every night. I knew I needed to seek help.”
He reached out to Veteran Affairs Canada and was referred to the Operational Stress Injury (OSI) Clinic at Parkwood Institute, a part of St. Joseph’s Health Care London, where he was diagnosed with PTSD. It was there that he learned about PTSD research being conducted by Dr. Ruth Lanius, Scientist at Lawson Health Research Institute and Psychiatrist at London Health Sciences Centre.

“I saw the need to help by participating in research, not only for myself but for my friends who have succumbed to the illness.”
Major Miller participated in Dr. Lanius’ neuroimaging research which uses advanced imaging technologies like PET/MRI to study differences in brain activity and neural connections between healthy individuals and those with different subtypes of PTSD. Dr. Lanius hopes that patterns of brain activity can one day be used as an objective biomarker to accurately diagnosis different subtypes of PTSD and uncover new targets for therapy.
“The research experience was interesting. I was interviewed while in the MRI and had to talk about incidents that trigger my PTSD to study my brain waves,” explains Major Miller.
In one study, Dr. Lanius is studying patterns of brain activity for those with ‘moral injury,’ an intense feeling of shame or guilt that can sometimes affect veterans with PTSD.
“Sometimes you’re involved in situations that you don’t have control over but that you feel responsible for,” says Major Miller. “You wonder, ‘Could I have done something differently?’”
Major Miller was happy to participate in any study that might help. Today, he is managing his PTSD through a combination of therapies that work for him.
“My biggest fear was giving up the things I love. I’ve been a soldier since day one and I’m sure I will be until the day I die. It’s important we come up with solutions to ensure our veterans receive proper care. Through research, we can tailor treatment to the individual rather than looking for a broad brush solution that might not suit everyone.”
This story is also featured on Research Canada’s Patient Stories website.
Mark your calendars for London Health Research Day 2019
Mark your calendars for London Health Research Day, taking place on April 30, 2019.
London Health Research Day provides a forum for learners to showcase their innovative work and engage in networking opportunities with peers, faculty and industry leaders. A special keynote lecture presented by a world-class scientist will also take place as part of The Lucille & Norton Wolf Health Research Lecture Series.
Date: Tuesday, April 30, 2019
Location: London Convention Centre
More information will be available in the coming months. We look forward to seeing you at London Health Research Day 2019.
London Health Research Day is presented in partnership by Lawson Health Research Institute and the Schulich School of Medicine & Dentistry.
Reddit AMA: How does the gut microbiome relate to healthy aging?
Drs. Greg Gloor, Gregor Reid, Jeremy Burton and Jean Macklaim participated in a Science AMA (Ask Me Anything) Series following the publication of their “The Gut Microbiota of Healthy Aged Chinese Is Similar to That of the Healthy Young” study.
Their study, one of the largest microbiota studies conducted in humans, has shown a potential link between healthy aging and a healthy gut.
During the AMA, the team of researchers answered over 30 questions relating to the study as well as other questions relating to probiotics and the human microbiome. Diet, environment, and fecal transplants were some of the topics reddit users wanted to discuss.
Each of the researchers also weighed in on the medical breakthroughs in microbiome and probiotic research in the future:
Dr. Greg Gloor: My prediction is that we will begin to understand the inter-relationships between the microbiota and the host. Right now the microbiome community and the human genetic community are not well connected. For example, the particular strains from a single donor that engraft following a fecal transplant differ between different recipients. We don’t understand how or why this happens, but the that the host genetic makeup and immunological response affects engraftment is an obvious starting point. We really can’t start to think about true precision medicine until we understand all the moving parts in play, we can’t just look at the host genetics, nor can we look only at the microbiota, or the broader environment - we need to synthesize all this information in order to truly deliver person-specific advice.
Dr. Gregor Reid: Sample a person’s microbiota and metabolomic read-out, know what drugs they are taking and what toxins they are being exposed to (mercury, pesticides, aflatoxins etc) and ‘design’ a probiotic that gets closer to being ‘personalized’ for whatever purpose is believed to be important to improve their health status. That would require having many probiotic strains available as options, and foods that could promote their influence in the host. Another challenge will be ethically doing this in early life; and another is to apply the intervention to impact distant sites like the brain. Furthermore, we need to know to what extent the intervention helps the person. For example, probiotics can reduce cholesterol, and this might reduce by 12.5% the risk of a cardiac event in the next ten years, while statins may reduce the risk by 25%. Depending on the actual risk of disease, the probiotic approach may not be sufficient. So, we should not promote something that endangers the life of the recipient in any way. Having said that, the side effects of high statin levels are extremely concerning, and we need to be looking at alternatives. If probiotics could reduce the need for high levels of statins, that might be a win-win.
Dr. Jeremy Burton: The gut microbiome composition has been shown to be predictive of certain conditions (T2 diabetes, some kidney stones etc), so the hospital of the future will likely analyse your microbiome, as well as your own genetics. Once a condition has been diagnosed and if there is a microbial link, some kind of microbial therapeutics will be administered in different ways. In a less severe microbial disruption, patients may only receive a dietary intervention, but where a more dramatic shift in the microbiome is required, a faecal transplant may be administered from the hospital “bank” or the person’s own microbiome maybe taken out and put in a gut model to grow and restore their bacterial populations in the laboratory before putting the “restored” microbiome back in the patient as an “auto” transplant.
Dr. Jean Macklaim: One of the things I hope we’ll be better able to understand in the future is how our early exposure to microbes sets the course of our immune response for the rest of our lives. There is a lot of evidence that the bacteria you are exposed to at birth and early in your childhood affects allergies, susceptibility to the common cold, chronic immune disorders, etc. Additionally, it’s very difficult to change your established microbiome and immune function in adulthood. If we are better able to prime our early microbiome, it could affect a lot of these disorders that change the quality of our lives during aging.
More information about the study and the full AMA can be found on Reddit.
Researchers looking to better personalize treatment for PTSD
Post-traumatic stress disorder (PTSD) is a condition that often develops in those who have experienced a traumatic event. PTSD affects close to 10 per cent of Canadians, and in some cases, can be difficult to treat.
In a new study through Lawson Health Research Institute and Western University’s Schulich School of Medicine & Dentistry, scientists are looking at a form of treatment called deep brain reorienting (DBR) for those suffering from PTSD.
“In our study we are looking at ways of trauma processing at the foundation of the stress response,” explains Dr. Ruth Lanius, Associate Scientist at Lawson and Professor at Western’s Schulich School of Medicine & Dentistry. “When you are faced with a stressor the first thing you do is turn your attention to it, and when you do that you engage your head and neck muscles.”

DBR was developed by Scottish psychiatrist Dr. Frank Corrigan and focuses on the muscles of the shoulders, neck, head and face of patients when recalling a traumatic event. This form of trauma processing starts right at the moment the stressor is noticed by the individual, which is often quickly followed by a moment of shock. By addressing the stressor at this level, doctors can target the foundation of where the stress response begins.
“When patients bring up a trigger in their mind, we look at what happens in terms of the tension in their head and neck. We process that gently by asking the patient to notice and stay with that tension without trying to release it, and over time the tension usually decreases,” explains Dr. Lanius, who is also a Psychiatrist at London Health Sciences Centre. “The second part involves addressing the shock response. You turn your attention to the stressor and then notice any moments of shock that follows, which is often associated with tension behind the eyes and in the shoulders. Finally, you address the visceral sensations associated with feelings and emotions associated with the stressor.”
Dr. Lanius believes that by using DBR and focusing on muscle and visceral responses, it will help patients suffering from PTSD to process the visceral feelings associated with the trauma and its triggers.
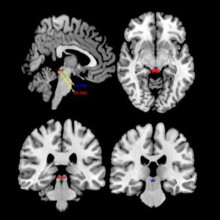
“After this form of treatment, patients often say they feel safer and don’t see themselves negatively, like they did in the past,” says Dr. Lanius. “This is because we change those intense visceral feelings and it allows the person to reevaluate who they are and how they interact with the world.”
The research team is hoping to recruit approximately 60 people to take part in the DBR study. Participants will undergo a psychological interview and an MRI, then eight sessions of treatments. Following those sessions, participants will have another interview and MRI to assess if any positive changes were made within the neurological networks and/or in psychological systems.
“Our hopes are to really personalize treatment for those living with PTSD,” says Dr. Lanius. “Some people have difficulty tolerating some forms of trauma processing and in my experience this treatment is a gentler approach for those individuals.”
Interested participants who have been diagnosed with PTSD can contact Suzy Southwell, Research Coordinator, at 519-685-8500 ext. 35186 or @email.
Understanding the vaginal microbiome essential to human health
There are trillions of microorganisms inhabiting your body. The majority of these are positive and essential to your health. They include those microorganisms found in the female reproductive system – a highly diverse environment that is crucial to human survival.
Understanding the microorganisms that inhabit the vagina, also known as the vaginal microbiome, is extremely important for women, their offspring and sexual partners. Dr. Gregor Reid recognizes this importance through his research into lactobacilli, the dominant organisms present in the healthy vagina of most women.
Dr. Reid is a Lawson microbiome and probiotics scientist and director of the Canadian Research and Development Centre for Probiotics. His interest in the vaginal microbiome began over 33 years ago.
“In the human gut, the microbiome differs with diet. But there is a global similarity to the vaginal microbiome,” said Dr. Reid. “From early in my career, I suspected a connection between this uniformity and the female’s critical role in reproduction.”
Harmful bacteria, also known as pathogens, can invade the vaginal microbiome to produce a more highly diverse state. This leads to the displacement of lactobacilli. It can also lead to bacterial vaginosis (BV) and the easier contraction of urinary tract infections (UTIs). These two ailments account for numerous physician visits each year and a reduction in a woman’s quality of life.
Mediating pregnancy and infant development
Research suggests that lactobacilli mediate complex changes that occur during pregnancy. If harmful pathogens invade and persist, inflammation and premature delivery can occur during pregnancy.
“The mechanisms behind the displacement of lactobacilli are not clear,” says Dr. Reid. “However, a number of factors can increase risk of BV. These include douching, sexual intercourse, lower estrogen levels and aging. It’s crucial that we conduct further research into these processes.”
Studies also suggest that the human fetus is exposed to the mother’s lactobacilli prior to birth, in addition to exposure during vaginal birthing. Again, understanding of this process and its significance is limited but warrants further investigation, says Reid. We need to further understand how exposure affects an infant’s immunity, metabolism and behavior in both early and later life.
“We’re seeing a dramatic rise in C-sections and a drop in breastfeeding,” says Reid. “If a developing child is not fully exposed to the mother’s lactobacilli, does this provide an opportunity for harmful bacteria to proliferate? This may cause repercussions to the offspring’s own future reproductive health.”
The role of probiotics
As research begins to focus on restoring a lactobacilli-dominant state, probiotics have been explored. However, attempts have presented challenges. “When probiotics are administered vaginally in a dried form, the lactobacilli fail to colonize long-term,” says Dr. Reid. “A study introducing lactobacilli in more natural form may lead to successful colonization. This has been the case in other areas like fecal transplantation.”
Challenges and opportunities
There are a number of other challenges when it comes to the study of the vaginal microbiome. This includes the lack of suitable animal models. While there have been recent developments that may lead to better recreations of a female microbiome, Dr. Reid explains that it will be difficult to mimic the many complexities of the female reproduction system. These include the menstrual cycle, immune responses, the use of douches, sexual intercourse and more.
“To fully understand female health, reproduction and infant development, we need to better understand lactobacilli,” said Dr. Reid. “We know that lactobacilli may help to combat herpes and environmental toxins, improve sperm motility, and even self-cure episodes of UTI and/or BV. What we are slowly uncovering is an understanding of the processes behind these interactions.”
Dr. Reid recently published a paper on this subject, "Cervicovaginal Microbiomes–Threats and Possibilities", in the publication Trends in Endocrinology & Metabolism. Dr. Reid’s own research is currently focused on compounds with the capacity to expand the proportion of lactobacilli at the expense of pathogens. The goal of this research is to improve the health of women across Canada and around the world.