Search
Search
Reddit AMA: How does the gut microbiome relate to healthy aging?
Drs. Greg Gloor, Gregor Reid, Jeremy Burton and Jean Macklaim participated in a Science AMA (Ask Me Anything) Series following the publication of their “The Gut Microbiota of Healthy Aged Chinese Is Similar to That of the Healthy Young” study.
Their study, one of the largest microbiota studies conducted in humans, has shown a potential link between healthy aging and a healthy gut.
During the AMA, the team of researchers answered over 30 questions relating to the study as well as other questions relating to probiotics and the human microbiome. Diet, environment, and fecal transplants were some of the topics reddit users wanted to discuss.
Each of the researchers also weighed in on the medical breakthroughs in microbiome and probiotic research in the future:
Dr. Greg Gloor: My prediction is that we will begin to understand the inter-relationships between the microbiota and the host. Right now the microbiome community and the human genetic community are not well connected. For example, the particular strains from a single donor that engraft following a fecal transplant differ between different recipients. We don’t understand how or why this happens, but the that the host genetic makeup and immunological response affects engraftment is an obvious starting point. We really can’t start to think about true precision medicine until we understand all the moving parts in play, we can’t just look at the host genetics, nor can we look only at the microbiota, or the broader environment - we need to synthesize all this information in order to truly deliver person-specific advice.
Dr. Gregor Reid: Sample a person’s microbiota and metabolomic read-out, know what drugs they are taking and what toxins they are being exposed to (mercury, pesticides, aflatoxins etc) and ‘design’ a probiotic that gets closer to being ‘personalized’ for whatever purpose is believed to be important to improve their health status. That would require having many probiotic strains available as options, and foods that could promote their influence in the host. Another challenge will be ethically doing this in early life; and another is to apply the intervention to impact distant sites like the brain. Furthermore, we need to know to what extent the intervention helps the person. For example, probiotics can reduce cholesterol, and this might reduce by 12.5% the risk of a cardiac event in the next ten years, while statins may reduce the risk by 25%. Depending on the actual risk of disease, the probiotic approach may not be sufficient. So, we should not promote something that endangers the life of the recipient in any way. Having said that, the side effects of high statin levels are extremely concerning, and we need to be looking at alternatives. If probiotics could reduce the need for high levels of statins, that might be a win-win.
Dr. Jeremy Burton: The gut microbiome composition has been shown to be predictive of certain conditions (T2 diabetes, some kidney stones etc), so the hospital of the future will likely analyse your microbiome, as well as your own genetics. Once a condition has been diagnosed and if there is a microbial link, some kind of microbial therapeutics will be administered in different ways. In a less severe microbial disruption, patients may only receive a dietary intervention, but where a more dramatic shift in the microbiome is required, a faecal transplant may be administered from the hospital “bank” or the person’s own microbiome maybe taken out and put in a gut model to grow and restore their bacterial populations in the laboratory before putting the “restored” microbiome back in the patient as an “auto” transplant.
Dr. Jean Macklaim: One of the things I hope we’ll be better able to understand in the future is how our early exposure to microbes sets the course of our immune response for the rest of our lives. There is a lot of evidence that the bacteria you are exposed to at birth and early in your childhood affects allergies, susceptibility to the common cold, chronic immune disorders, etc. Additionally, it’s very difficult to change your established microbiome and immune function in adulthood. If we are better able to prime our early microbiome, it could affect a lot of these disorders that change the quality of our lives during aging.
More information about the study and the full AMA can be found on Reddit.
Reduce the swelling: Why does chronic inflammation matter?
Inflammation is becoming increasingly popular as a “buzzword” for health claims and advice. It has been implicated in a number of chronic and age-related conditions, including diabetes, rheumatoid arthritis, cardiovascular disease, neurodegenerative diseases, and even depression and cancer. On the other hand, inflammation is part of the body’s natural response to infection and tissue damage, and it is crucial to the healing process.
You are invited to the Lawson’s Café Scientifique, a free community event providing an informal opportunity to get involved with science. Hear a panel of expert researchers explore how inflammation affects our health and how this knowledge can be applied to improve health care. Guests are then encouraged to ask questions as part of an open-forum discussion to gain insights from the speakers, and from one another.
Presented Talks
- “Molecular signatures: How do we listen to the music of inflammation?”
Dr. Chris McIntyre - “The effects of chronic inflammation on cancer”
Dr. Samuel Asfaha - “Coming to grips with curling fingers: A cause and potential treatment for fibrosis of the hand”
Dr. David O’Gorman - MODERATOR – Dr. David Hill
Registration
Free community event hosted by Lawson Health Research Institute.
PLEASE NOTE: Registration for this event is now full.
Email @email to be added to the event wait list. Please include the names of all individuals who wish to be added to the wait list. We apperciate your interest in Café Scientifique.
Event Information
Date: Wednesday, October 12, 2016
Time: 7 to 9 p.m.
Location: Windermere Manor (The Grand Hall), 200 Collip Circle, London, ON N6G 4X8
Speaker Biographies

In 1999 he was appointed as Consultant Nephrologist at the Royal Derby Hospital and subsequently as Reader in Vascular Medicine and then Professor of Nephrology at Nottingham University, becoming Head of the Division of Graduate Entry Medicine and Medical Sciences. Dr McIntyre led a team of multidisciplinary researchers focused largely on the pathophysiology of the widespread abnormalities of cardiovascular function and body composition in CKD patients. These studies included basic clinical science, natural history studies and the development and application of novel therapeutic strategies. These studies have increasingly focussed on the adverse consequences resulting from dialysis therapy itself and the improvement in outcomes by the reduction of preventable harm.
He has recently moved to his new role in Canada as Professor of Medicine and was awarded the inaugural Robert Lindsay Chair of Dialysis Research and Innovation at Western University, London Ontario. He also serves as Director of the Lilibeth Caberto Kidney Clinical Research Unit at London Health Sciences Centre, as Assistant Director of the Lawson Health Research Institute and is cross appointed as full Professor in the Department of Medical Biophysics at Western.

His research focuses on the intestinal stem cells of the gut and aims to identify the cellular origin of colorectal cancer.
See Dr. Asfaha’s full scientist profile.

See Dr. O’Gorman’s full scientist profile.
Moderator Biography

Reducing social isolation with new community resource
Researchers in London are sharing a new resource that can help municipalities and other organizations better understand social isolation and implement solutions proven to be effective. With input from over 35 community partners and people with lived experience, the research team hopes this tool can be used to support community-based initiatives that counteract poverty and homelessness while promoting mental health and social inclusion.
“The pandemic has highlighted the issues of isolation and homelessness, and we know there is a connection between mental health and poverty. Unfortunately, right now, many people don’t see solutions in sight,” explains Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson Health Research Institute.
“Our new resource offers an expanded understanding of isolation and homelessness based on a very broad view and many different perspectives. We have taken it a step further and given examples of solutions that are working.” She is the lead researcher for CURA (Community-University Research Alliance): Poverty, Mental Health and Social Inclusion.
Today during a virtual book launch, the team from the CURA discussed details of a new publication from Canadian Scholars: Poverty, Mental Health, and Social Inclusion, edited by Drs. Forchuk and Rick Csiernik. Community partners from Connect for Mental Health (peer support), Impact Junk Solutions from CMHA Elgin-Middlesex, and Goodwill Industries shared more about their successful programs.
The book brings together research, real stories and information about programs from the London and area community that are working to address these issues. Most of the chapters includes a wide range of co-authors, including psychiatric consumer-survivors, academics, students, front-line service providers and leadership from community partners.
“In order to find real solutions, the voices of people using the services must be at the centre. Their stories and experiences have been a very important part of producing this book,” says Betty Edwards, Executive Director at Can-Voice, a consumer-survivor group, and Community Director for CURA. "For us to move the needle, we need collaboration across different sectors, for example health, income support, housing and social services. No one sector can solve these issues on their own.”
The book summarizes the foundational work by the CURA to better understand the inter-relationships between poverty and social inclusion for psychiatric survivors. Social inclusion involves the full participation of marginalized groups in the social and economic benefits of society which can be difficult to achieve for people with the “double jeopardy” of poverty and mental illness.
“After five years of funding and several published research papers, we wanted to pull the findings together as a whole so that it would be more easily accessed and implemented by a wide range of people and organizations,” adds Dr. Forchuk. “Our hope is that other cities and service providers can pick up this book to see what we’re doing in London, and consider ways that they may reach out to their citizens to address social exclusion. It is also an academic tool to prepare the next generation as they continue to tackle the wicked problem of homelessness.”
“I reflect back on the past 15 months of the pandemic and know how isolated I have felt at times. Imagine the feelings of isolation or being forgotten that would come with experiencing homelessness? And for some, it’s been most of their adult lives,” shares Dr. Csiernik, Professor at King’s University College at Western University. “We know that many people during the pandemic have lost homes, jobs and food security. Some may have new or worsening mental health disorders. The learnings and solutions like the ones presented in the book are needed now more than ever.”
Social Inclusion Art
Incorporating an arts-based approach, the book also features photographs taken by photographer Justin Langille who would spend about a month with each of the programs offering solutions and partnered with consumer survivors to capture accurate depictions of what they considered important messages.

Impact Junk Solutions employee Allan is reflected in a mirror attached to a dresser being taken away from the home of an individual who recently passed away in the northwest end of London, Ontario in March 2014. (Photo credit: Justin Langille Photography)

A supported housing unit rendered uninhabitable by an individual suffering from mental illness, which was a challenge for Impact Junk Solutions to de-clutter. (Photo credit: Justin Langille Photography)

Diane assembles parts on the floor of the Goodwill’s RMHC Social Enterprise program in St.Thomas in April 2014. (Photo credit: Justin Langille Photography)

A participant pauses for a moment during a Connect group sharing session in October 2014. Connect facilitates peer sessions where individuals experiencing mental illness can learn and share strategies to help their recovery. (Photo credit: Justin Langille Photography)

Steve helps a co-worker navigate a couch out from a basement in the Blackfriars neighbourhood in London, Ontario in April 2014. Returning to work has been essential for Steve’s successful recovery from mental illness and substance abuse. (Photo credit: Justin Langille Photography)

Connect member Tammy makes breakfast at home in her kitchen. If there is one thing she can do habitually to set herself up for success in her mental health recovery, Tammy says it’s having a good breakfast. (Photo credit: Justin Langille Photography)

Goodwill RMHC Social Enterprise program employee Donald applies reflective tape to a stack of pylons in March 2014. (Photo credit: Justin Langille Photography)

The Goodwill Social Enterprise program includes a successful toy-recycling component that bags and re-sells used toys at a low-cost for low-income families. (Photo credit: Justin Langille Photography)
Reducing social isolation with new community resource
LONDON, ON – Researchers in London are sharing a new resource that can help municipalities and other organizations better understand social isolation and implement solutions proven to be effective. With input from over 35 community partners and people with lived experience, the research team hopes this tool can be used to support community-based initiatives that counteract poverty and homelessness while promoting mental health and social inclusion.
“The pandemic has highlighted the issues of isolation and homelessness, and we know there is a connection between mental health and poverty. Unfortunately, right now, many people don’t see solutions in sight,” explains Dr. Cheryl Forchuk, Assistant Scientific Director at Lawson Health Research Institute. “Our new resource offers an expanded understanding of isolation and homelessness based on a very broad view and many different perspectives. We have taken it a step further and given examples of solutions that are working.” She is the lead researcher for CURA (Community-University Research Alliance): Poverty, Mental Health and Social Inclusion.
Today during a virtual book launch, the team from the CURA discussed details of a new publication from Canadian Scholars: Poverty, Mental Health, and Social Inclusion, edited by Drs. Forchuk and Rick Csiernik. Community partners from Connect for Mental Health (peer support), Impact Junk Solutions from CMHA Elgin-Middlesex, and Goodwill Industries shared more about their successful programs.
The book brings together research, real stories and information about programs from the London and area community that are working to address these issues. Most of the chapters includes a wide range of co-authors, including psychiatric consumer-survivors, academics, students, front-line service providers and leadership from community partners.
“In order to find real solutions, the voices of people using the services must be at the centre. Their stories and experiences have been a very important part of producing this book,” says Betty Edwards, Executive Director at Can-Voice, a consumer-survivor group, and Community Director for CURA. “For us to move the needle, we need collaboration across different sectors, for example health, income support, housing and social services. No one sector can solve these issues on their own.”
The book summarizes the foundational work by the CURA to better understand the inter-relationships between poverty and social inclusion for psychiatric survivors. Social inclusion involves the full participation of marginalized groups in the social and economic benefits of society which can be difficult to achieve for people with the “double jeopardy” of poverty and mental illness.
“After five years of funding and several published research papers, we wanted to pull the findings together as a whole so that it would be more easily accessed and implemented by a wide range of people and organizations,” adds Dr. Forchuk. “Our hope is that other cities and service providers can pick up this book to see what we’re doing in London, and consider ways that they may reach out to their citizens to address social exclusion. It is also an academic tool to prepare the next generation as they continue to tackle the wicked problem of homelessness.”
Incorporating an arts-based approach, the book also features photographs taken by photographer Justin Langille who would spend about a month with each of the programs offering solutions and partnered with consumer survivors to capture accurate depictions of what they considered important messages.
“I reflect back on the past 15 months of the pandemic and know how isolated I have felt at times. Imagine the feelings of isolation or being forgotten that would come with experiencing homelessness? And for some, it’s been most of their adult lives,” shares Dr. Csiernik, Professor at King’s University College at Western University. “We know that many people during the pandemic have lost homes, jobs and food security. Some may have new or worsening mental health disorders. The learnings and solutions like the ones presented in the book are needed now more than ever.”
A central focus of the CURA team has been understanding homelessness – what lead someone to experience homelessness and how do we as a society respond? By bringing together different perspectives, the CURA team uncovered the issue of hospital discharge to homelessness, leading to research projects at London Health Sciences Centre and St. Joseph’s Health Care London that integrates the City of London’s housing and homeless approach. They have been better able to tailor youth specific homeless interventions after more awareness of the unique challenges of homeless youth. Driven by an information gap identified by the CURA, Dr. Forchuk’s team recently announced a research project testing data algorithms to track and identify who is homeless and where they are located.
-30-
DOWNLOADABLE MEDIA
Photo credit for all images: Justin Langille Photography

A supported housing unit rendered uninhabitable by an individual suffering from mental illness, which was a challenge for Impact Junk Solutions to de-clutter. (Photo credit: Justin Langille Photography)

Diane assembles parts on the floor of the Goodwill’s RMHC Social Enterprise program in St.Thomas in April 2014. (Photo credit: Justin Langille Photography)

Steve helps a co-worker navigate a couch out from a basement in the Blackfriars neighbourhood in London, Ontario in April 2014. Returning to work has been essential for Steve’s successful recovery from mental illness and substance abuse. (Photo credit: Justin Langille Photography)

Goodwill RMHC Social Enterprise program employee Donald applies reflective tape to a stack of pylons in March 2014. (Photo credit: Justin Langille Photography)
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Relieving the pain: Current research on pain and its management
There has been an explosion of scientific knowledge that is helping us to uncover the changes that happen when an individual develops pain, giving millions of people the hope that they will be better able to manage their own pain.
Pain is one of the most common reasons people seek medical attention. In Canada, 25 per cent of adults are affected by chronic pain and that statistic moves up to 50 per cent in the elderly.
Acute and ongoing pain have traditionally been hard to understand and there has isn’t always a clear answer for tackling these issues. We do know that ongoing pain can have significant impacts on one’s wellbeing.
Join Lawson Health Research Institute for our next Café Scientifique to hear a panel of experts share more about local research in the areas of:
- The role of opioid and cannabis analgesics in the management of pain.
- The impact of pain for individuals and families, including children experiencing pain, and some of the barriers to its management.
- The growing understanding of the mechanisms of pain to create the best long-term results for patients.
- Educational tools for patients and caregivers.
Speakers

- Dr. Dwight Moulin, Clinical Neurological Sciences and Oncology
- Dr. Naveen Poonai, Paediatric Emergency Medicine
- Dr. Dave Walton, School of Physical Therapy
- MODERATOR – Dr. Kathy Speechley, Epidemiology & Biostatistics
Event Details
Date: Tuesday, November 20, 2018
Time: 7-9 pm (doors open at 6:30 pm)
Location: Best Western Plus Lamplighter Inn & Conference Centre, 591 Wellington Rd, London, ON N6C 4R3
Map and directions
Parking: Ample free parking on-site
This is a free community event and online registration is REQUIRED.
Click here to register.
Lawson is the research institute of London Health Sciences Centre and St. Joseph’s Health Care London.
Researchers investigate a new method of sedation for paediatric patients
Scientists at Children’s Health Research Institute (a program of Lawson Health Research Institute), Sunnybrook Research Institute and The Hospital for Sick Children (SickKids) are working together to study the potential benefits of inhaled sedation as an alternative to keep critically ill children sedated and comfortable.
“Many sick children need support from a ventilator and other life-saving treatments, and may require intravenous (IV) sedatives to tolerate these uncomfortable therapies,” says Dr. Rishi Ganesan, Lawson Associate Scientist and Paediatric Neurocritical Care Physician at Children’s Hospital at London Health Sciences Centre (LHSC). “However, our current sedation options may contribute to a complication called delirium. We are interested in evaluating if delirium and long-term neurological complications are lower in children receiving inhaled sedation compared to those receiving IV sedation, which is the current standard of care.”
Delirium is an acute change in mental state that children in critical care can sometimes develop as a result of their critical illness and the medications and therapies they receive during their hospital stay. Delirium presents as confusion, disorientation, agitation, excessive drowsiness or poor attention. Dr. Marat Slessarev, Lawson Scientist and Critical Care Physician at LHSC, has been researching and comparing inhaled sedation to IV sedation in adults since the pandemic hit in 2020 in a collaborative trial called SAVE-ICU with Dr. Angela Jerath, Anesthesiologist and Scientist at Sunnybrook.
“One of the challenges with IV sedation is that we do not have a way to measure the level of sedatives in the blood,” explains Dr. Slessarev. “Critically ill patients that are sedated can sometimes develop issues with the kidney and liver, which are both important in eliminating the sedatives from the blood stream.”
Through this novel collaborative research, the team is now looking at the potential benefits of inhaled sedation in paediatric patients.
“Inhaled sedatives are an alternative to currently used IV sedatives, and they may reduce delirium and accelerate brain recovery. Inhaled sedatives are used safely every day in operating rooms, widely available and inexpensive,” explains Dr. Jerath. “In contrast to IV sedatives, they do not accumulate in the body, are rapidly eliminated via the lungs, promote faster awakening and discharge from a ventilator, and reduce inflammation – which may be a contributing factor to delirium.”
Enrollment for the ABOVE trial is beginning at Children’s Hospital at LHSC and SickKids. The pilot study will enroll 60 critically ill paediatric patients who will be randomized into two groups; one group will receive inhaled sedation while the other will get standard IV sedation. Once the pilot phase of the trial is complete, the team hopes to expand this trial across the country with more paediatric intensive care units (ICUs) joining the larger trial.
“The field of critical care has made significant strides in life-saving technologies and therapies in recent years, but now we are focused on finding ways to ensure our patients continue to do well after leaving the hospital,” says Dr. Nicole McKinnon, Critical Care Physician and lead investigator at SickKids and a Scientist Track Investigator at SickKids Research Insitute. “This trial is a first step in better understanding the effects of sedative and pain medications on children’s longer-term neurocognitive development. Our research will be key to providing critically ill children with the greatest chance to flourish at home.”
“This has the potential to change how critically ill children are cared for in paediatric ICUs across Canada and the world,” adds Dr. Ganesan. “We hope that inhaled sedation makes a difference in children’s long-term functional outcomes, so they can thrive and achieve their full potential.”
The ABOVE Trial recently received funding through a Canadian Institute for Health Research (CIHR) grant.
About Sunnybrook Research Institute: Sunnybrook Research Institute (SRI) is the research arm of Sunnybrook Health Sciences Centre, an internationally recognized academic health sciences centre fully affiliated with the University of Toronto. With well-established programs in basic and applied sciences which span across three scientific platforms and ten clinical programs, SRI is developing innovations in care for the more than 1.3 million patients the hospital cares for annually. To learn more, visit www.sunnybrook.ca/research
About The Hospital for Sick Children: The Hospital for Sick Children (SickKids) is recognized as one of the world’s foremost paediatric health-care institutions and is Canada’s leading centre dedicated to advancing children’s health through the integration of patient care, research and education. Founded in 1875 and affiliated with the University of Toronto, SickKids is one of Canada’s most research-intensive hospitals and has generated discoveries that have helped children globally. Its mission is to provide the best in complex and specialized family-centred care; pioneer scientific and clinical advancements; share expertise; foster an academic environment that nurtures health-care professionals; and champion an accessible, comprehensive and sustainable child health system. SickKids is a founding member of Kids Health Alliance, a network of partners working to create a high quality, consistent and coordinated approach to paediatric health care that is centred around children, youth and their families. SickKids is proud of its vision for Healthier Children. A Better World.
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Communications Consultant & External Relations
Lawson Health Research Institute
T: 519-685-8500 ext. ext. 64059
C: 226-919-4748
@email
Researchers looking to better personalize treatment for PTSD
Post-traumatic stress disorder (PTSD) is a condition that often develops in those who have experienced a traumatic event. PTSD affects close to 10 per cent of Canadians, and in some cases, can be difficult to treat.
In a new study through Lawson Health Research Institute and Western University’s Schulich School of Medicine & Dentistry, scientists are looking at a form of treatment called deep brain reorienting (DBR) for those suffering from PTSD.
“In our study we are looking at ways of trauma processing at the foundation of the stress response,” explains Dr. Ruth Lanius, Associate Scientist at Lawson and Professor at Western’s Schulich School of Medicine & Dentistry. “When you are faced with a stressor the first thing you do is turn your attention to it, and when you do that you engage your head and neck muscles.”

DBR was developed by Scottish psychiatrist Dr. Frank Corrigan and focuses on the muscles of the shoulders, neck, head and face of patients when recalling a traumatic event. This form of trauma processing starts right at the moment the stressor is noticed by the individual, which is often quickly followed by a moment of shock. By addressing the stressor at this level, doctors can target the foundation of where the stress response begins.
“When patients bring up a trigger in their mind, we look at what happens in terms of the tension in their head and neck. We process that gently by asking the patient to notice and stay with that tension without trying to release it, and over time the tension usually decreases,” explains Dr. Lanius, who is also a Psychiatrist at London Health Sciences Centre. “The second part involves addressing the shock response. You turn your attention to the stressor and then notice any moments of shock that follows, which is often associated with tension behind the eyes and in the shoulders. Finally, you address the visceral sensations associated with feelings and emotions associated with the stressor.”
Dr. Lanius believes that by using DBR and focusing on muscle and visceral responses, it will help patients suffering from PTSD to process the visceral feelings associated with the trauma and its triggers.
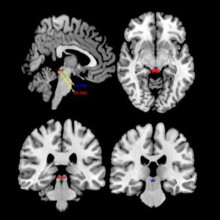
“After this form of treatment, patients often say they feel safer and don’t see themselves negatively, like they did in the past,” says Dr. Lanius. “This is because we change those intense visceral feelings and it allows the person to reevaluate who they are and how they interact with the world.”
The research team is hoping to recruit approximately 60 people to take part in the DBR study. Participants will undergo a psychological interview and an MRI, then eight sessions of treatments. Following those sessions, participants will have another interview and MRI to assess if any positive changes were made within the neurological networks and/or in psychological systems.
“Our hopes are to really personalize treatment for those living with PTSD,” says Dr. Lanius. “Some people have difficulty tolerating some forms of trauma processing and in my experience this treatment is a gentler approach for those individuals.”
Interested participants who have been diagnosed with PTSD can contact Suzy Southwell, Research Coordinator, at 519-685-8500 ext. 35186 or @email.
Researchers receive over $40,000 to study role of personality and resiliency in Veteran mental health
LONDON, ON – The unique and challenging experiences faced by Canadian Armed Forces (CAF) Veterans puts this group at high risk for developing symptoms of mental health disorders, such as Post traumatic stress disorder (PTSD), depression, and anxiety. Researchers at Lawson Health Research Institute (Lawson) have been awarded over $40,000 from Veterans Affairs Canada to study various risk and protective factors associated with mental health disorders in CAF Veterans.
The study aims to learn whether an individual’s personality traits serve as risk or protective factors for Veterans developing mental health problems. The traits that will be examined include openness, agreeableness, emotionality, honesty-humility, conscientiousness, extraversion, and resiliency. For example, someone who is high in openness and resiliency may have a lower risk of developing mental health symptoms.
“Veterans and military members experience uniquely challenging events when compared to the general population,” explains Dr. Rachel Plouffe, study co-lead and Postdoctoral Associate at Lawson. “Past research has identified some risk factors, including history of childhood trauma, age, gender, and education. However, no one to date has investigated the role that personality traits might play in Veterans’ symptoms of mental health conditions.”
The research team will look at the relationship between these personality traits, exposure to stressful experiences during military operations, and mental health outcomes through survey data provided by 500 treatment-seeking and non-treatment seeking Veterans. This information will be used to assess whether the individual’s expression of these personality traits can predict levels of depression, anxiety and PTSD.
They also hope to determine whether the association between combat exposure and PTSD is stronger for those higher in traits such as emotionality, which reflects those who tend to be anxious and fearful. On the other hand, this association will likely be weaker for those higher in more “positive” traits, such as agreeableness, as these individuals tend to be cooperative and forgiving toward others.
Plouffe notes that personalities are not completely stagnant. Certain traits can often change over time, and individuals can work to increase their levels of resiliency.
“Ultimately, our hope is to help improve the ability of CAF members and Veterans to thrive even in the face of great adversity. With the findings from our research, military organizations and mental health treatment centres could use the information from this study to predict which patients may be at greater risk of developing mental health disorders, and provide tailored treatment for these individuals,” she explains.
“This research is needed for military organizations to improve and implement strategies that enhance the well-being of Veterans and active service members,” says Dr. Don Richardson, study co-lead and Director of the MacDonald Franklin OSI Research Centre at Lawson. “Our Veterans give a lot to serve and protect, so it is our duty as researchers and clinicians to find ways that we can better serve them.”
-30-
Lawson Health Research Institute is one of Canada’s top hospital-based research institutes, tackling the most pressing challenges in health care. As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, our innovation happens where care is delivered. Lawson research teams are at the leading-edge of science with the goal of improving health and the delivery of care for patients. Working in partnership with Western University, our researchers are encouraged to pursue their curiosity, collaborate often and share their discoveries widely. Research conducted through Lawson makes a difference in the lives of patients, families and communities around the world. To learn more, visit www.lawsonresearch.ca.
Senior Media Relations Consultant
Communications & Public Engagement
T: 519-685-8500 ext. 73502
Celine.zadorsky@lhsc.on.ca
Researchers receive over $40,000 to study role of personality and resiliency in Veteran mental health
The unique and challenging experiences faced by Canadian Armed Forces (CAF) Veterans puts this group at high risk for developing symptoms of mental health disorders, such as Post traumatic stress disorder (PTSD), depression, and anxiety. Researchers at Lawson Health Research Institute (Lawson) have been awarded over $40,000 from Veterans Affairs Canada to study various risk and protective factors associated with mental health disorders in CAF Veterans.
The study aims to learn whether an individual’s personality traits serve as risk or protective factors for Veterans developing mental health problems. The traits that will be examined include openness, agreeableness, emotionality, honesty-humility, conscientiousness, extraversion, and resiliency. For example, someone who is high in openness and resiliency may have a lower risk of developing mental health symptoms.
“Veterans and military members experience uniquely challenging events when compared to the general population,” explains Dr. Rachel Plouffe, study co-lead and Postdoctoral Associate at Lawson. “Past research has identified some risk factors, including history of childhood trauma, age, gender, and education. However, no one to date has investigated the role that personality traits might play in Veterans’ symptoms of mental health conditions.”
The research team will look at the relationship between these personality traits, exposure to stressful experiences during military operations, and mental health outcomes through survey data provided by 500 treatment-seeking and non-treatment seeking Veterans. This information will be used to assess whether the individual’s expression of these personality traits can predict levels of depression, anxiety and PTSD.
They also hope to determine whether the association between combat exposure and PTSD is stronger for those higher in traits such as emotionality, which reflects those who tend to be anxious and fearful. On the other hand, this association will likely be weaker for those higher in more “positive” traits, such as agreeableness, as these individuals tend to be cooperative and forgiving toward others.
Plouffe notes that personalities are not completely stagnant. Certain traits can often change over time, and individuals can work to increase their levels of resiliency.
“Ultimately, our hope is to help improve the ability of CAF members and Veterans to thrive even in the face of great adversity. With the findings from our research, military organizations and mental health treatment centres could use the information from this study to predict which patients may be at greater risk of developing mental health disorders, and provide tailored treatment for these individuals,” she explains.
“This research is needed for military organizations to improve and implement strategies that enhance the well-being of Veterans and active service members,” says Dr. Don Richardson, study co-lead and Director of the MacDonald Franklin OSI Research Centre at Lawson. “Our Veterans give a lot to serve and protect, so it is our duty as researchers and clinicians to find ways that we can better serve them.”
Researchers testing triple intervention to combat dementia
Researchers at Lawson Health Research Institute are the first in the world conducting a clinical trial to test a triple intervention aimed at treating Mild Cognitive Impairment (MCI) and delaying the onset of dementia. The Mobility, Exercise and Cognition (MEC) team will be incorporating physical exercises, cognitive training and vitamin D supplementation to determine the best treatment for improving mobility and cognition.
“We have learned the brain processes involved in motor-control - for example how a person walks - and cognition - for example how that person solves a problem - share similar locations and networks in the brain,” explains Dr. Manuel Montero Odasso, Lawson Scientist and Geriatrician at St. Joseph’s Health Care London. “Problems with mobility are connected to lowering function in the mind, and so can be a good indicator of future progression into dementia.”
Dr. Montero Odasso is also an Associate Professor in the departments of Medicine and Epidemiology and Biostatistics at the Schulich School of Medicine & Dentistry, Western University.

Gait assessment looks at the way in which we move our whole body from one point to another, helping to analyze mobility and the brain processes involved.
MCI is an intermediate stage between the expected cognitive decline of normal aging and the more serious decline of dementia. It can involve problems with memory, language, thinking and judgment. While many older individuals experience decline in both mobility and cognition, each are assessed and treated separately with no specific recommendations available for physicians.
The SYNERGIC Trial will combine physical exercises, cognitive training and vitamin D to test how these interventions work together to improve cognition in older adults at risk for dementia. The trial is targeting cognitive decline at the earliest stage, individuals with MCI, where interventions are more likely to have an effect and can be monitored.

Dr. Manuel Montero Odasso, Lawson Scientist and lead for the SYNERGIC Trial.
Dr. Montero Odasso explains that both physical and cognitive exercises have shown promising effects for maintaining cognition, while vitamin D deficiency is associated with cognitive decline. A key feature of this trial is that participants will receive individualized and progressive training.
“By delaying declines in cognition, we can improve a person’s quality of life. This research will help to support a more comprehensive preventative treatment with clinical guidelines for physicians whose patients are at risk of developing dementia,” states Dr. Montero Odasso. “Even more, each one year delay of progression to dementia in older individuals at risk has the opportunity to save billions of dollars for the Canadian health care system.”
Individuals over 60 years old with mild cognitive impairment without dementia are eligible for this clinical trial. Those interested in participating are encouraged to contact Research Coordinator Alanna Black at 519.685.4292 ext. 42179.
Participants will be asked to complete a routine of exercises and cognitive training three times a week for six months, with one final assessment at 12 months. The main site for the study is Parkwood Institute with physical exercises taking place at the Labatt Health Sciences Building at Western University, in Dr. Kevin Shoemaker’s Laboratory for Brain and Heart Health.
This study has been funded by the Canadian Consortium on Neurodegenerative in Aging (CCNA) which represents Canada-wide research aimed at enhancing the quality of life and services for individuals diagnosed with a neurodegenerative disease. The MEC team in London, led by Dr. Montero Odasso, includes expert researchers in the field of mobility who aim to develop common assessments for the interaction of cognition and mobility for older people to aid as a diagnostic tool for detecting dementia.

Members of the study’s research team, from left to right: Korbin Blue, Research Assistant (Co-op Student); Yanina Sarquis-Adamson, Lab Research Assistant; Frederico Faria, Post-Doctoral Fellow; Dr. Montero Odasso, Director, Gait and Brain Lab; research participant; Alanna Black, Lab Research Coordinator; Stephanie Cullen, Research Assistant (Undergraduate Student); and, Navena Lingum, Research Assistant (Master Student).